The term “pneumonia” often conjures images of severe illness, requiring hospitalization and significant medical intervention. However, the reality is far more nuanced. Pneumonia is a broad term encompassing infections that inflame the air sacs (alveoli) in one or both lungs. These air sacs may fill with fluid or pus, leading to a range of symptoms. Within this spectrum, “walking pneumonia” represents a milder form of the condition, distinct from more severe presentations. Understanding these differences is crucial for accurate diagnosis, appropriate treatment, and informed health management.
Understanding the Core of Pneumonia
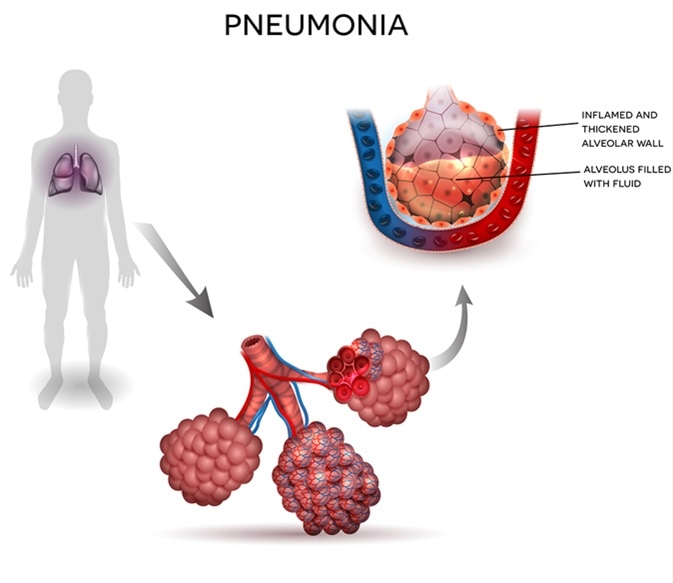
At its heart, pneumonia is an infection of the lungs. The primary culprits are typically bacteria, viruses, or fungi. These microorganisms invade the respiratory system, setting up an inflammatory response. When pathogens enter the alveoli, the body’s immune system dispatches white blood cells to combat them. This battle results in the alveoli filling with fluid and inflammatory debris, a process that impedes the lungs’ ability to transfer oxygen into the bloodstream and remove carbon dioxide.
Causes and Pathogens
The cause of pneumonia dictates much of its character, including its severity and typical progression.
Bacterial Pneumonia
Bacterial pneumonia is often characterized by a more abrupt onset of symptoms and can be quite severe. Common bacterial culprits include Streptococcus pneumoniae (pneumococcal pneumonia), Haemophilus influenzae, and Mycoplasma pneumoniae. Bacterial infections tend to respond well to antibiotic treatment, but prompt diagnosis and intervention are vital to prevent complications.
Viral Pneumonia
Viral pneumonia is frequently seen in conjunction with or following other viral illnesses, such as influenza or the common cold. Viruses like influenza, respiratory syncytial virus (RSV), and even coronaviruses can cause viral pneumonia. Viral infections are generally harder to treat directly, as antibiotics are ineffective against them. Treatment often focuses on supportive care to manage symptoms and allow the body’s immune system to fight off the infection.
Fungal Pneumonia
Less common in healthy individuals, fungal pneumonia can occur in people with weakened immune systems, such as those with HIV/AIDS or undergoing chemotherapy, or after prolonged exposure to certain environmental fungi. Examples include Pneumocystis jirovecii pneumonia (PCP), which is common in individuals with compromised immune systems, and infections from fungi like Histoplasma capsulatum or Coccidioides immitis, found in specific geographic regions.
The Alveolar Inflammatory Process
Regardless of the causative agent, the underlying pathology involves inflammation and fluid accumulation in the alveoli. This directly impacts gas exchange. In healthy lungs, alveoli are tiny, thin-walled sacs. When infected, they swell, and exudate (pus and fluid) fills the space normally occupied by air. This thickening of the alveolar walls and the presence of fluid create a barrier, hindering the efficient diffusion of oxygen from the air into the capillaries surrounding the alveoli and the removal of carbon dioxide from the capillaries into the air. This deficit in gas exchange leads to the hallmark symptoms of pneumonia, such as shortness of breath and reduced blood oxygen levels.
Defining Walking Pneumonia
Walking pneumonia, also known medically as atypical pneumonia, is a colloquial term used to describe a milder form of pneumonia. The name itself highlights its defining characteristic: individuals with walking pneumonia are typically well enough to continue their daily activities, or “walk around,” despite being infected. This stands in stark contrast to the more severe, classic presentations of pneumonia where bed rest and hospitalization are often necessary.
Key Distinguishing Features
The distinction between walking pneumonia and more severe forms lies in several key aspects:
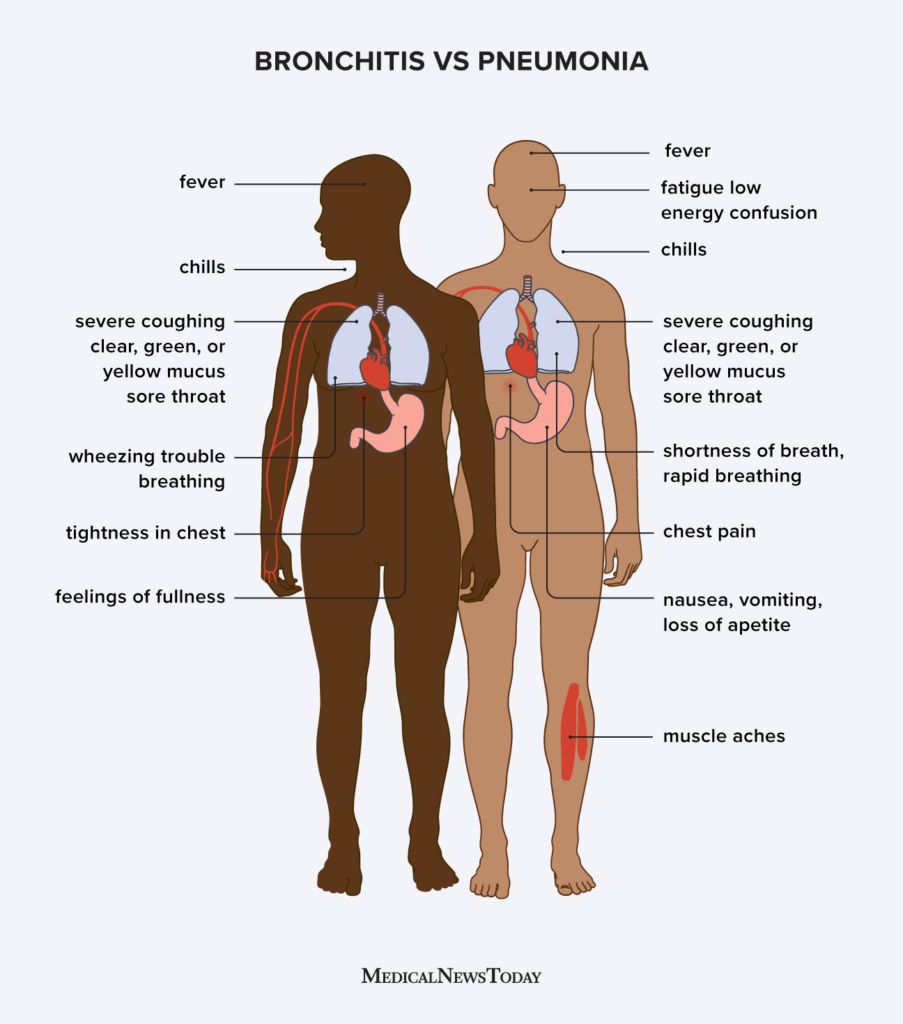
- Severity of Symptoms: This is the most significant differentiator. While symptoms are present, they are generally less debilitating. Patients may experience a persistent cough, fatigue, and a low-grade fever, but they often avoid the severe shortness of breath, high fever, chest pain, and profound weakness that can accompany typical pneumonia.
- Causative Agents: Walking pneumonia is frequently caused by certain types of bacteria, particularly Mycoplasma pneumoniae, and sometimes viruses. These pathogens tend to cause a less intense inflammatory response compared to the bacteria that typically cause severe pneumonia. Mycoplasma pneumoniae is often referred to as “the walking pneumonia germ” due to its association with this milder form.
- Radiographic Appearance: On a chest X-ray, walking pneumonia often presents with patchy infiltrates rather than the dense consolidation seen in more severe cases. This means the inflammation is more scattered and less consolidated, which can sometimes make it harder to detect on initial imaging, hence the term “atypical.”
- Onset and Progression: The onset of walking pneumonia is often more gradual than that of bacterial pneumonia. Symptoms may develop slowly over several days or even weeks.
Common Symptoms of Walking Pneumonia
While less severe, the symptoms of walking pneumonia are still indicative of a lung infection and should not be ignored.

- Persistent Cough: This is often the most prominent symptom. The cough may be dry initially but can later produce mucus.
- Fatigue and Malaise: A general feeling of tiredness and being unwell is common.
- Low-Grade Fever: A mild elevation in body temperature, typically below 102°F (38.9°C), is often present.
- Headache: General headaches can accompany the illness.
- Sore Throat and Runny Nose: These symptoms can sometimes precede or accompany the cough, mirroring a common cold.
- Mild Shortness of Breath: Some individuals may experience mild breathlessness, particularly with exertion, but it is usually not severe enough to prevent daily activities.
- Chest Discomfort: A mild ache or discomfort in the chest might be present.
It is important to note that symptoms can vary greatly from person to person, and some individuals with walking pneumonia may experience no symptoms at all, especially if it’s discovered incidentally during imaging for another reason.
Differentiating from Classic Pneumonia
The term “classic pneumonia” is generally used to refer to the more severe forms of the infection, often caused by more virulent bacteria like Streptococcus pneumoniae. The differences are pronounced and have significant implications for diagnosis and management.
Onset and Severity
Classic pneumonia typically has a more sudden and dramatic onset. Individuals often experience a rapid escalation of symptoms, including:
- High Fever: Temperatures frequently exceed 102°F (38.9°C) and can be accompanied by chills.
- Severe Cough: The cough is often productive, bringing up thick, colored mucus, and can be painful.
- Significant Shortness of Breath: Difficulty breathing, even at rest, is a hallmark symptom. This can lead to rapid breathing and a feeling of suffocation.
- Sharp Chest Pain: Pain in the chest, especially when breathing deeply or coughing, is common.
- Profound Fatigue and Weakness: Patients often feel too ill to get out of bed and require significant rest.
Diagnostic Markers
While both forms involve inflammation in the lungs, the extent and appearance on diagnostic tests can differ.
- Chest X-ray: In classic pneumonia, an X-ray typically reveals lobar pneumonia, characterized by a dense, consolidated area in one lobe of the lung. In contrast, walking pneumonia often shows patchy infiltrates, appearing as scattered cloudy areas.
- Blood Oxygen Levels: Patients with classic pneumonia are more likely to have significantly lower blood oxygen saturation (hypoxemia) compared to those with walking pneumonia, often necessitating supplemental oxygen.
- White Blood Cell Count: While both conditions can elevate white blood cell counts, the magnitude might be more pronounced in severe bacterial pneumonia.
Treatment Approaches
The differing severities dictate distinct treatment strategies.
- Antibiotics: Bacterial pneumonia, especially severe forms, requires prompt antibiotic treatment. The choice of antibiotic depends on the suspected or confirmed pathogen.
- Hospitalization: Patients with classic pneumonia are often admitted to the hospital for monitoring, intravenous antibiotics, oxygen therapy, and management of complications.
- Supportive Care: For both forms, supportive care is crucial, including rest, hydration, and fever reducers. However, the intensity of supportive care is significantly higher for classic pneumonia.
Diagnosis and When to Seek Medical Attention
Accurately diagnosing pneumonia, whether walking or classic, is essential for effective treatment. Medical professionals typically rely on a combination of patient history, physical examination, and diagnostic tests.
The Diagnostic Process
- Medical History: A doctor will ask about symptoms, their duration, onset, any underlying health conditions, and recent exposures.
- Physical Examination: This includes listening to the lungs with a stethoscope for abnormal sounds like crackles or wheezing, checking vital signs (temperature, heart rate, respiratory rate), and assessing for signs of distress.
- Chest X-ray: This is a primary tool for visualizing the lungs and identifying infiltrates or consolidation indicative of pneumonia.
- Sputum Culture: If mucus is produced, it can be sent to a lab to identify the specific bacteria or fungus causing the infection, guiding antibiotic selection.
- Blood Tests: These can help assess the level of infection and inflammation in the body, as well as blood oxygen levels.
- Pulse Oximetry: A non-invasive device that measures the oxygen saturation in the blood.
Recognizing the Need for Care
While walking pneumonia can be managed at home, it’s crucial to know when to seek professional medical help.
- Difficulty Breathing: Any significant shortness of breath, even if intermittent, warrants medical attention.
- High Fever: A fever that is persistently high or unresponsive to over-the-counter medications.
- Chest Pain: Severe or worsening chest pain.
- Confusion or Altered Mental State: This can be a sign of severe infection affecting oxygen supply to the brain.
- Worsening Symptoms: If symptoms of walking pneumonia begin to worsen or new, more severe symptoms develop.
- Underlying Health Conditions: Individuals with chronic lung diseases (like COPD or asthma), heart disease, diabetes, a weakened immune system, or those who are very young or elderly are at higher risk for complications and should seek medical advice promptly if they suspect pneumonia.
Conclusion: Navigating Lung Health
The distinction between walking pneumonia and classic pneumonia lies primarily in the severity of symptoms and the impact on an individual’s daily life. While both involve inflammation and infection in the lungs, walking pneumonia, often caused by atypical pathogens like Mycoplasma pneumoniae, allows individuals to maintain a greater level of function. This doesn’t diminish the importance of seeking medical advice, as even milder forms require proper diagnosis to ensure appropriate treatment and prevent potential complications. Understanding these differences empowers individuals to better recognize symptoms, seek timely medical care, and manage their lung health effectively. Prompt medical evaluation remains the cornerstone of recovery for any form of pneumonia, ensuring the best possible outcome and a return to full health.
