Lipedema fat is a chronic and progressive condition characterized by the symmetrical accumulation of adipose tissue, primarily in the lower extremities. Unlike common obesity, this fat is resistant to diet and exercise, presenting a unique set of challenges for those affected. Understanding the distinct nature of lipedema fat is crucial for accurate diagnosis, effective management, and improved quality of life.
The Unique Characteristics of Lipedema Fat
The defining feature of lipedema is the nature of the fat itself. It doesn’t behave like typical subcutaneous fat, which readily mobilizes in response to caloric deficit. Instead, lipedema fat appears to be genetically predisposed to accumulate and resist metabolic breakdown. This resistance means that even significant weight loss through traditional means often fails to reduce the affected areas.
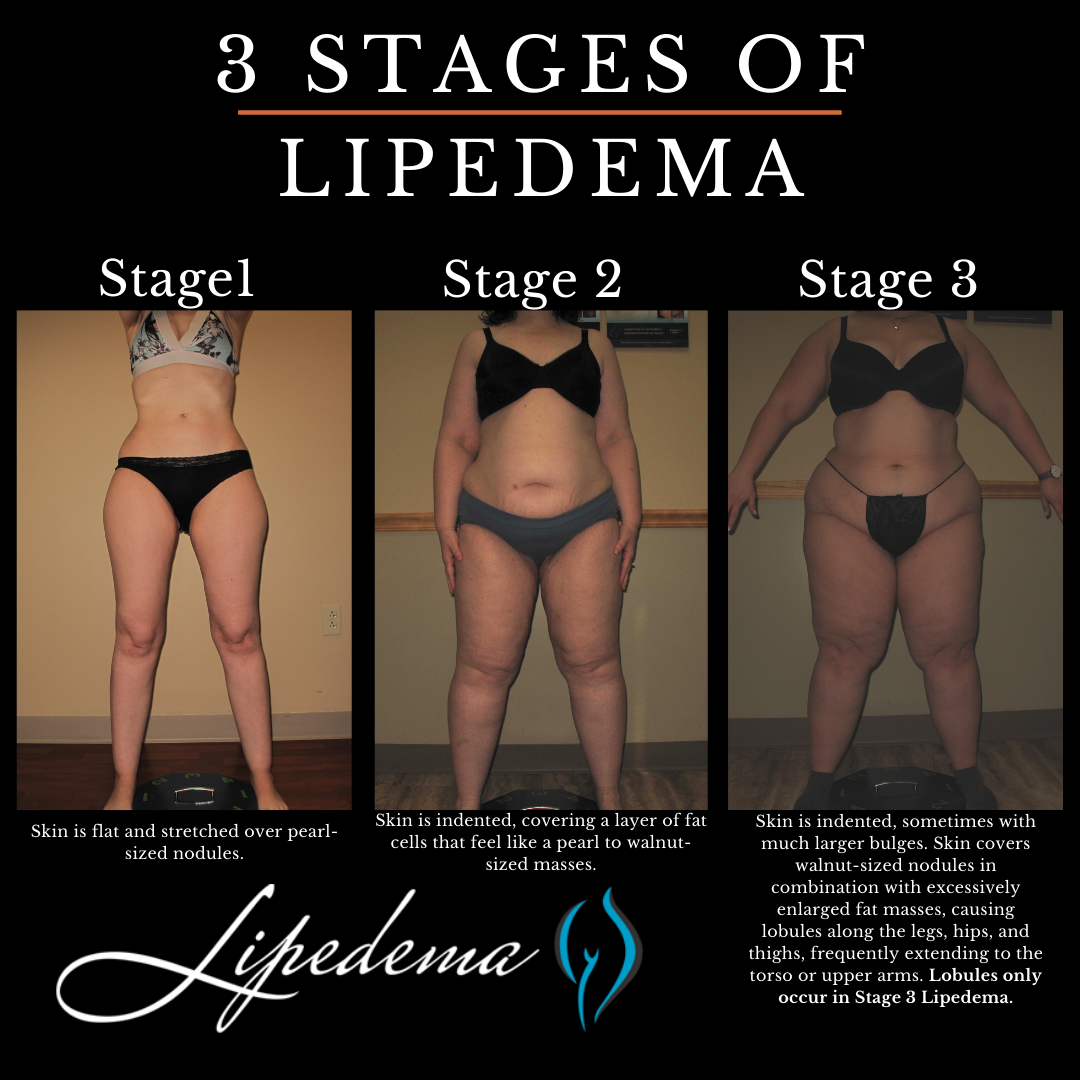
Symmetrical Distribution
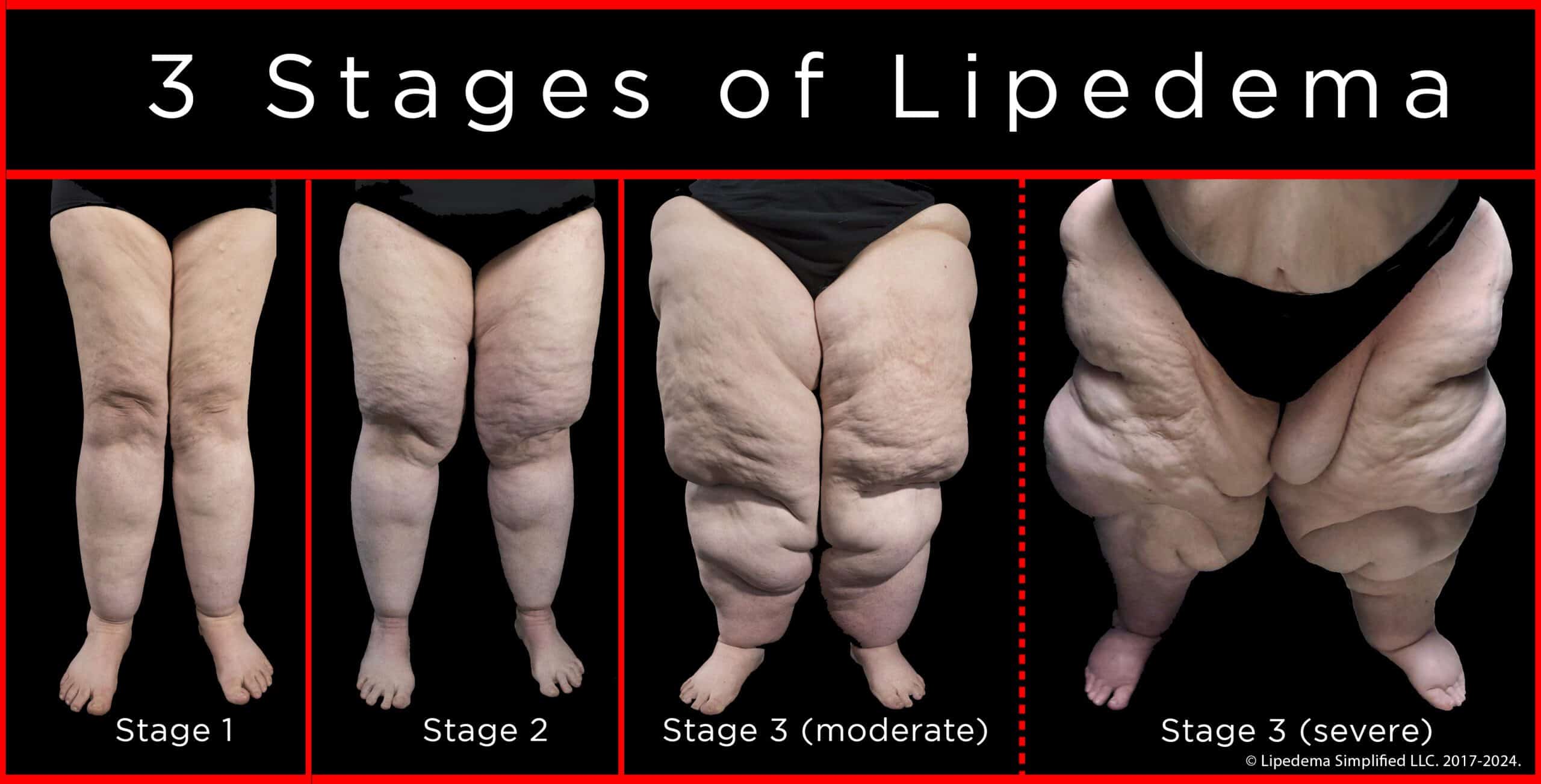
A hallmark of lipedema is the symmetrical distribution of fat. This means that both legs, or both arms, are affected to a similar degree. The accumulation typically begins at the hips and thighs, extending downwards to the ankles. The feet, however, are usually spared, a key differentiator from lymphedema. This symmetrical pattern often leads to a “column-like” appearance of the legs.
Resistance to Diet and Exercise
Perhaps the most frustrating aspect of lipedema fat is its defiance of conventional weight loss methods. While a healthy lifestyle can benefit overall health and may lead to some fat reduction in unaffected areas, the fat deposits specific to lipedema remain largely unchanged. This metabolic resistance suggests underlying biological differences in how these adipocytes (fat cells) function.
Pain and Tenderness
Lipedema fat is not merely an aesthetic concern; it is often accompanied by significant pain and tenderness. The affected limbs can feel heavy, achy, and bruise easily. This pain can range from a dull ache to sharp, stabbing sensations, and it can be exacerbated by prolonged standing, pressure, or even light touch. The tenderness contributes to a reduced quality of life and can impact daily activities.
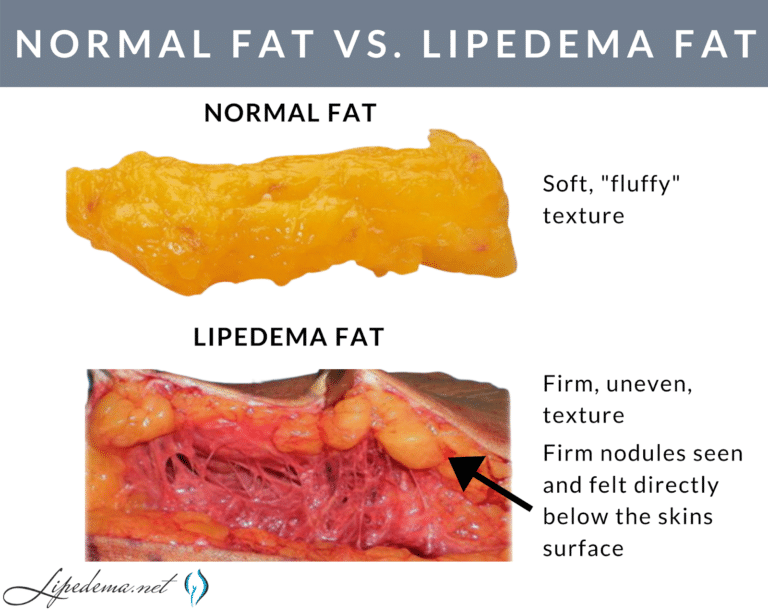
Nodular and Fibrotic Texture
As lipedema progresses, the accumulated fat can become more dense, nodular, and fibrotic. This means it can feel lumpy and less pliable than normal fat. The increased fibrosis can further impede circulation and contribute to the feeling of heaviness and stiffness in the affected limbs. In later stages, this fibrotic tissue can also impede lymphatic flow.
Distinguishing Lipedema Fat from Other Conditions
The specific characteristics of lipedema fat are vital for differentiating it from other conditions that involve fat accumulation or swelling in the limbs. Misdiagnosis can lead to ineffective treatments and a delay in appropriate care.
Lipedema vs. Obesity
The most common point of confusion is distinguishing lipedema from generalized obesity. In obesity, fat accumulation is typically generalized throughout the body and is responsive to caloric restriction. In lipedema, the fat is largely confined to the limbs, is symmetrical, and is highly resistant to diet and exercise. While a person can have both obesity and lipedema, the lipedema fat component remains distinct and unyielding to weight loss efforts.
Lipedema vs. Lymphedema
Another critical differentiation is between lipedema and lymphedema. Lymphedema is a condition where there is a blockage or impairment in the lymphatic system, leading to the accumulation of lymphatic fluid in the tissues. A key distinguishing factor is that lipedema typically spares the feet, whereas lymphedema often affects the feet and ankles, leading to swelling that extends to the toes. While lipedema can coexist with or progress to secondary lymphedema due to the increased tissue load and fibrosis, the initial fat accumulation pattern is different.
Lipedema vs. Dercum’s Disease
Dercum’s disease, also known as adiposis dolorosa, is another rare disorder characterized by painful fatty tumors. However, Dercum’s disease typically presents with lipomas (benign tumors of fat) that are often scattered and not necessarily symmetrical in distribution like lipedema. While pain is a feature of both, the pattern of fat accumulation and the presence of distinct lipomas are characteristic of Dercum’s disease.
The Underlying Mechanisms and Theories
While the exact cause of lipedema remains elusive, research points towards a complex interplay of genetic predisposition, hormonal influences, and potentially inflammatory factors. Understanding these potential mechanisms offers insight into why lipedema fat behaves as it does.
Genetic Predisposition
Evidence strongly suggests a genetic component to lipedema. The condition often runs in families, and studies are ongoing to identify specific genes that may be involved in the development and progression of lipedema fat accumulation. This genetic link helps explain why certain individuals are more susceptible to developing the condition, regardless of lifestyle factors.
Hormonal Influences
Hormonal factors are also believed to play a significant role. Lipedema often appears or worsens around puberty, during pregnancy, or during menopause, periods of significant hormonal fluctuation. Estrogen, in particular, has been implicated, and research is exploring the possibility that altered estrogen receptor sensitivity or metabolism contributes to the abnormal fat deposition. However, it is important to note that lipedema is not solely an estrogen-driven disease and occurs in pre-pubertal individuals as well.
Potential Inflammatory Pathways
Emerging research suggests that inflammatory processes may be involved in the development and perpetuation of lipedema. While not an autoimmune disease, there is evidence of low-grade chronic inflammation within the adipose tissue of individuals with lipedema. This inflammation could contribute to the fibrosis, pain, and resistance to metabolic breakdown observed in lipedema fat.
Management and Treatment of Lipedema Fat
Given the unique nature of lipedema fat, management strategies differ from those for standard obesity. The focus is on symptom management, reducing discomfort, and slowing the progression of the condition.
Conservative Management
Conservative approaches are the cornerstone of lipedema management and aim to alleviate symptoms and improve limb function. These include:
- Manual Lymphatic Drainage (MLD): This gentle massage technique helps to move lymphatic fluid and reduce swelling. While lipedema is not primarily a lymphatic fluid issue, MLD can be beneficial for managing associated edema and discomfort, especially if secondary lymphedema develops.
- Compression Therapy: Wearing specialized compression garments is crucial for managing swelling, supporting the limbs, and reducing pain. The constant, gentle pressure helps to minimize fluid accumulation and can improve the sensation of heaviness.
- Exercise: While exercise may not reduce lipedema fat itself, low-impact activities like swimming, cycling, and walking can improve circulation, muscle strength, and overall fitness. It’s important to find exercises that are pain-free and don’t exacerbate symptoms.
- Diet and Nutrition: While diet won’t eliminate lipedema fat, a healthy, anti-inflammatory diet can support overall health and manage any co-existing metabolic issues. Focusing on whole foods, reducing processed items, and ensuring adequate hydration are beneficial.
Surgical Interventions
For individuals with significant and debilitating lipedema, surgical interventions may be considered. These aim to remove the excess adipose tissue.
- Liposuction: Specialized liposuction techniques, such as tumescent liposuction or VASER liposuction, are often employed. These are typically performed by surgeons experienced in treating lipedema, as the technique requires careful consideration of the fibrous nature of the tissue and the potential for lymphatic damage. It’s important to understand that liposuction aims to debulk the affected areas and improve symptoms, not to achieve a typical cosmetic outcome. Multiple sessions are often required.
Lifestyle and Self-Care
Beyond medical interventions, self-care plays a vital role in managing lipedema.
- Skin Care: Maintaining healthy skin is important, especially in areas prone to swelling and potential breakdown. Regular moisturizing and keeping the skin clean can prevent infections.
- Activity Pacing: Understanding one’s limits and pacing activities throughout the day can help manage fatigue and pain.
- Emotional Support: Living with a chronic condition that impacts body image and physical comfort can be emotionally challenging. Connecting with support groups and seeking professional counseling can be invaluable.
The Future of Understanding Lipedema Fat
Research into lipedema is a continually evolving field. As our understanding of the genetic, hormonal, and cellular mechanisms behind lipedema fat deepens, so too will our ability to develop more targeted and effective treatments. The journey from recognizing lipedema as a distinct entity to uncovering its precise pathophysiology is ongoing, offering hope for improved diagnosis, management, and ultimately, a better quality of life for those affected. The distinct nature of lipedema fat, its resistance to conventional therapies, and its profound impact on individuals underscore the need for continued scientific inquiry and patient advocacy.
