Congestion in infants is a common and often distressing experience for both baby and parents. While a stuffy nose is typically not a sign of a serious illness, it can significantly impact a baby’s ability to feed, sleep, and generally feel comfortable. Understanding the causes of infant congestion and employing safe, effective remedies is crucial for providing relief and ensuring your little one’s well-being. This guide delves into the nuances of infant congestion, offering practical strategies rooted in a gentle, supportive approach.
Understanding Infant Congestion
Infant congestion, often referred to as a “stuffy nose” or “blocked nasal passages,” occurs when the delicate tissues within a baby’s nasal cavity become inflamed and swollen, leading to an accumulation of mucus. Unlike older children or adults, babies are obligate nasal breathers, meaning they primarily breathe through their noses, especially during feeding. This makes nasal congestion particularly challenging for them, as it can interfere with their ability to suck and swallow effectively.
Common Causes of Nasal Congestion in Babies
Several factors can contribute to a congested nose in infants:
- The Common Cold: This is the most frequent culprit. Viruses that cause colds lead to inflammation of the nasal passages and increased mucus production. Babies have smaller nasal passages, making them more susceptible to blockage from even a small amount of mucus.
- Allergies: While less common in very young infants, allergies to environmental factors such as dust mites, pet dander, or pollen can cause nasal inflammation and congestion. Symptoms may also include sneezing and watery eyes.
- Irritants: Exposure to smoke (including secondhand smoke), strong perfumes, or other airborne irritants can inflame a baby’s sensitive nasal lining, leading to congestion.
- Dry Air: Particularly in arid climates or during winter months when heating systems dry out the air, dry nasal passages can become irritated and produce thicker mucus, contributing to a stuffy nose.
- Teething: Some parents report increased nasal congestion during teething periods. While not fully understood, the theory is that the body’s inflammatory response to teething may affect the nasal passages.
- Gastroesophageal Reflux (GER) or Gastroesophageal Reflux Disease (GERD): In some cases, reflux can lead to irritation in the upper airway, potentially causing congestion.
Why Infant Congestion is Different
It’s essential to recognize that infant congestion differs from that experienced by older individuals. Babies have:
- Smaller Nasal Passages: This means a small amount of swelling or mucus can cause significant blockage.
- Limited Ability to Clear Nasal Passages: They cannot blow their nose, and their natural instinct to clear their throat is less developed.
- Reliance on Nasal Breathing: As mentioned, they primarily breathe through their nose, making feeding and breathing a delicate balance that can be easily disrupted by congestion.
Safe and Effective Remedies for Infant Congestion
When your baby is congested, the primary goals are to help them breathe more easily, facilitate feeding and sleep, and provide comfort. Always prioritize safety and consult your pediatrician if you have any concerns or if symptoms are severe or prolonged.
Nasal Saline Drops and Sprays
Saline solution is a remarkably effective and safe method for thinning mucus and loosening congestion in infants. It works by hydrating the dried mucus, making it easier for your baby to expel.
- How to Use:
- Positioning: Gently lay your baby down on their back.
- Application: Tilt your baby’s head back slightly. Administer one or two drops of sterile saline solution into each nostril. For older infants who can tolerate it, a saline spray designed for infants can also be used.
- Wait: Allow the saline to work for a minute or two. You may hear or see some of the mucus loosen.
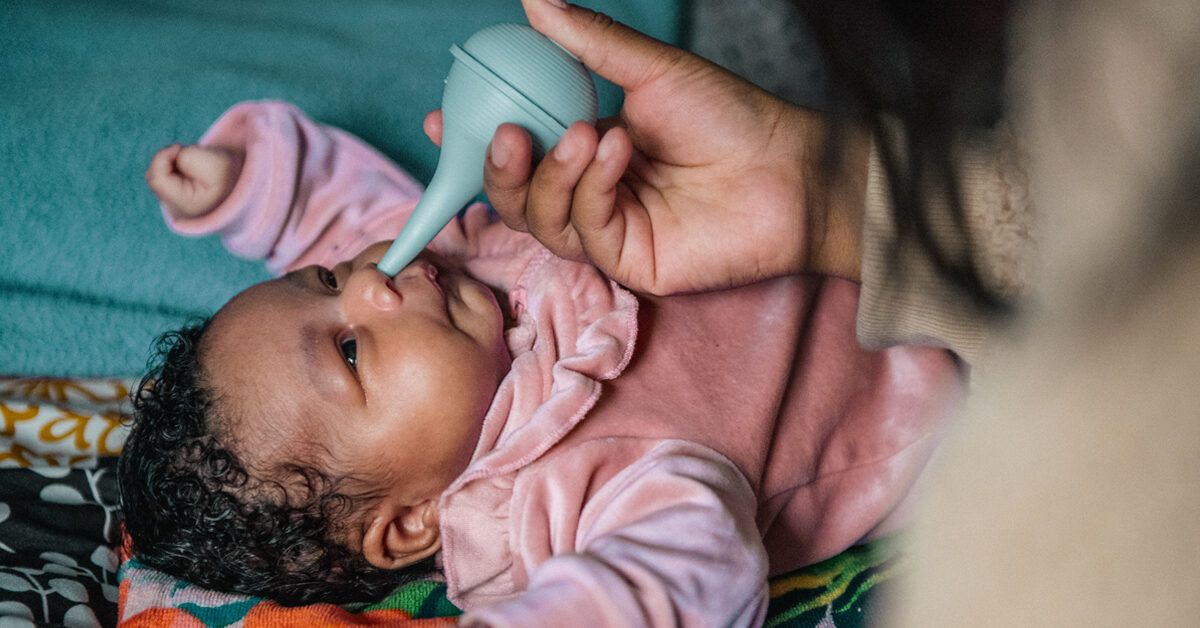
- Suction (if needed): If the mucus is thick and your baby is struggling, you can gently use a nasal aspirator (bulb syringe or a more advanced nasal suction device) to remove the loosened mucus. Squeeze the bulb syringe before inserting it gently into the nostril, then slowly release the bulb to suction out the mucus. Empty the syringe and repeat as necessary, cleaning it thoroughly after each use.
- Frequency: Saline drops can be used as often as needed, especially before feeding and sleep, to help your baby breathe and feed more comfortably.
Humidifying the Air
Increasing the humidity in your baby’s environment can help keep their nasal passages moist and prevent mucus from drying and hardening.
- Cool-Mist Humidifiers: These are generally recommended over warm-mist humidifiers for infants due to the risk of burns associated with warm mist.
- Placement: Place the humidifier in your baby’s room, but not directly next to their crib or bed. Ensure it’s out of reach of curious hands.
- Maintenance: It is crucial to clean humidifiers regularly according to the manufacturer’s instructions to prevent the growth of mold and bacteria, which can be harmful. Use distilled or demineralized water to minimize mineral buildup.
- Steam from the Bathroom: A warm, steamy bathroom can also provide temporary relief.
- Method: Run a hot shower to create steam, then sit in the bathroom with your baby for 10-15 minutes. Ensure the room is comfortably warm and not excessively hot.
![]()
Elevating the Head of the Crib (with caution)
Elevating the head of your baby’s crib can help with drainage and make breathing easier. However, it is crucial to do this safely.
- Safe Elevation: The American Academy of Pediatrics (AAP) recommends against using pillows or positioning devices in the crib due to the risk of suffocation and Sudden Infant Death Syndrome (SIDS).
- Approved Methods: If you choose to elevate, place a firm pillow or folded towel underneath the mattress at the head of the crib, creating a slight incline. Never place anything on top of the mattress. Some parents find placing a rolled towel or a wedge under the crib mattress (not inside the crib) to be effective. Always ensure the mattress remains firm and flush with the crib sides.
- Consult Your Pediatrician: Discuss any inclination strategies with your pediatrician to ensure they are appropriate and safe for your baby.
Keeping Baby Hydrated
Adequate hydration is vital for thinning mucus. For breastfed or formula-fed babies, this is typically achieved through their regular milk intake.
- Breastfeeding/Formula Feeding: Continue offering feeds as usual. If congestion makes feeding difficult, offer smaller, more frequent feeds. Some babies may need a break during feeding to clear their nasal passages.
- Older Infants (over 6 months): For babies over six months, offering small amounts of water between feeds can also aid hydration.
Positioning for Comfort
Certain sleeping and holding positions can help ease congestion.
- Upright Positioning: Holding your baby upright during feeding and for a period afterward can help prevent milk from entering the nasal passages and can aid in drainage.
- Side Sleeping (Supervised): While babies should always sleep on their backs for safety, some parents find that holding their baby on their side (while supervised and supported) can temporarily help with congestion. This should only be done when actively holding and monitoring your baby.
When to Seek Medical Advice
While infant congestion is usually minor, it’s essential to know when to consult your pediatrician.
Red Flags and Warning Signs
Contact your doctor immediately if your baby:
- Has a fever: Especially if the fever is high (consult your pediatrician for specific temperature guidelines based on age) or persistent.
- Shows signs of difficulty breathing: This includes rapid breathing, grunting, flaring nostrils, or chest retractions (skin pulling in between the ribs or at the base of the throat).
- Is refusing to feed or is feeding poorly: Significant reduction in intake can lead to dehydration.
- Appears lethargic or unusually irritable: Changes in overall demeanor can indicate a more serious issue.
- Has thick, colored nasal discharge that persists for more than a week or two: While clear mucus is common with colds, persistently thick, colored mucus could indicate a secondary bacterial infection.
- Develops a cough that worsens or is accompanied by wheezing.
- Has ear pain or tugging at their ears: This can be a sign of an ear infection, which can sometimes accompany or be exacerbated by congestion.
- Has symptoms that don’t improve after 10-14 days, or that seem to worsen.
What Not to Do
Certain remedies are unsafe or ineffective for infants:
- Over-the-counter (OTC) cold and cough medicines: These are generally not recommended for infants and young children due to the risk of serious side effects and lack of proven effectiveness. Always consult your pediatrician before giving any medication.
- Vapor Rubs with Camphor and Menthol: These can be too strong for an infant’s delicate airways and can cause respiratory distress.
- Forceful Nose Blowing: This can be painful and ineffective for babies.
- Using saline without proper suction: If the mucus is thick, simply adding saline might not be enough to clear the passages. Gentle suction is often necessary.

Conclusion
Infant congestion can be a challenging phase, but by understanding its causes and employing safe, evidence-based remedies, parents can effectively manage their baby’s discomfort. Prioritizing gentle techniques like saline irrigation, humidification, and ensuring adequate hydration, while remaining vigilant for any warning signs that require medical attention, will help your baby breathe easier and recover more comfortably. Always remember that your pediatrician is your most valuable resource for guidance and reassurance throughout your baby’s health journey.
