The Foundational Role of Keratinocytes in Epidermal Structure and Function
Keratinocytes are the most abundant cell type in the epidermis, the outermost layer of the skin. These epithelial cells are the primary building blocks of the epidermis, playing a critical and multifaceted role in maintaining skin integrity, protection, and overall health. Their name derives from keratin, a tough, fibrous protein that they synthesize and accumulate, which is instrumental in forming the protective barrier of the skin. Understanding the function of keratinocytes is paramount to comprehending the complex physiology of the skin and its role in shielding the body from external environmental insults.
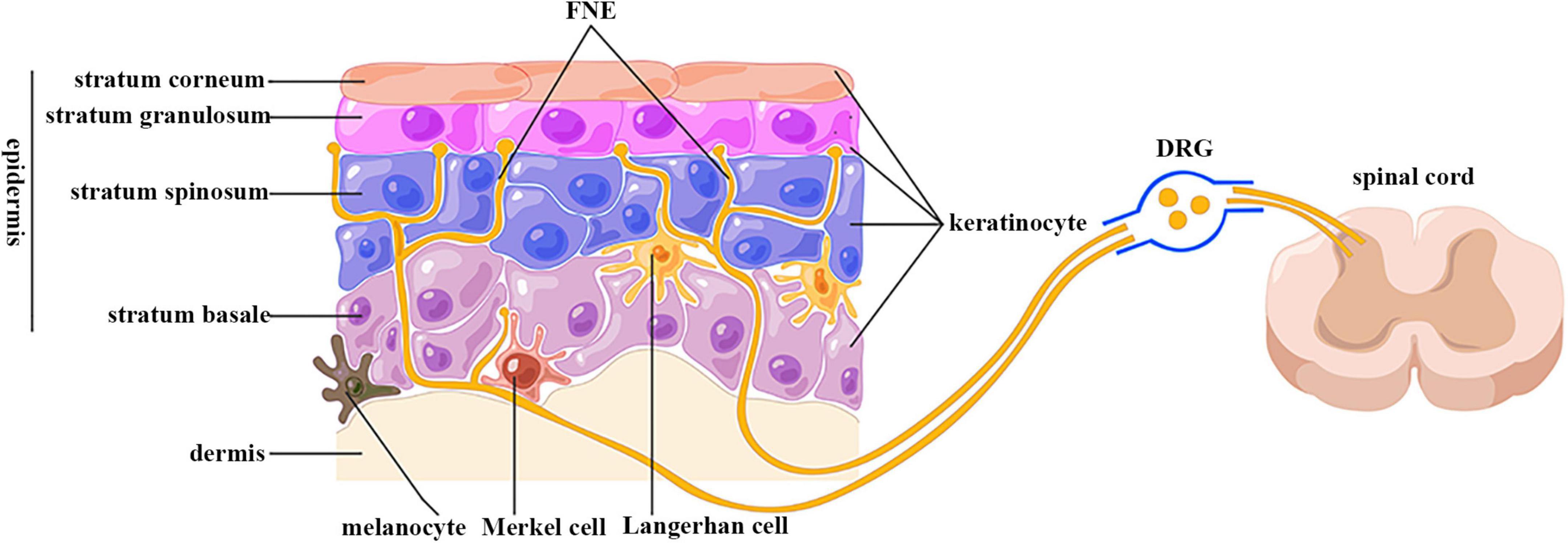
The epidermis, where keratinocytes reside, is a dynamic tissue constantly undergoing renewal. Keratinocytes originate from the basal layer, known as the stratum basale, where they are actively dividing. As these cells mature and differentiate, they migrate upwards through the epidermal layers, undergoing significant morphological and biochemical changes. This process of epidermal differentiation is a tightly regulated cascade that culminates in the formation of a robust, protective stratum corneum, the outermost layer of the skin. This journey from the basal layer to the surface is essential for the continuous renewal and maintenance of the epidermal barrier.
Epidermal Differentiation: A Journey of Transformation
The life cycle of a keratinocyte is a remarkable example of cellular differentiation. It begins in the stratum basale, a single layer of cuboidal stem cells. These basal keratinocytes are proliferative, meaning they divide through mitosis to produce new cells. Some of these daughter cells remain in the basal layer to maintain the stem cell population, while others embark on a journey of differentiation.
As cells move upwards into the stratum spinosum, they begin to flatten and develop numerous desmosomes, which are specialized cell junctions that anchor them to neighboring keratinocytes. These junctions give the stratum spinosum its characteristic spiny appearance under a microscope. During this phase, keratinocytes increase their production of keratin intermediate filaments, which begin to aggregate within the cytoplasm.
Further up, in the stratum granulosum, keratinocytes flatten even more and contain prominent keratohyalin granules. These granules are rich in proteins that play a crucial role in the formation of the cornified envelope, a specialized structure that reinforces the cell membrane of terminally differentiated keratinocytes. The cells also undergo lamellar body secretion, releasing lipid-rich substances into the extracellular space. These lipids are vital for creating a hydrophobic barrier that prevents water loss from the body and the entry of foreign substances.
The final stage of keratinocyte differentiation occurs in the stratum lucidum (present only in thick skin, like the palms and soles) and the stratum corneum. In the stratum corneum, keratinocytes are terminally differentiated, anucleated (lacking a nucleus), and devoid of most organelles. They are essentially flattened sacs filled with keratin and enclosed by a thickened, cross-linked protein envelope. These flattened, dead keratinocytes, called corneocytes, are constantly shed from the surface of the skin, a process known as desquamation, and are replaced by new cells migrating from below. This continuous renewal ensures the integrity and effectiveness of the epidermal barrier.
The Protective Barrier: Keratinocytes as the Guardians of the Skin
The primary and most vital function of keratinocytes is the establishment and maintenance of the epidermal barrier. This barrier serves as the first line of defense against a multitude of external threats, including:
Physical Protection
The dense network of keratin filaments within keratinocytes, combined with the robust desmosomal junctions between them, provides significant physical strength and resilience to the skin. This mechanical strength helps to prevent physical damage, abrasions, and trauma from external forces. The stratum corneum, composed of tightly packed corneocytes, acts as a physical shield, preventing blunt force and penetration.
Chemical Protection
Keratinocytes synthesize and secrete various substances that contribute to chemical protection. The lipid matrix secreted by lamellar bodies in the stratum granulosum creates a hydrophobic environment, effectively repelling water-soluble toxins and chemicals. Furthermore, the tightly packed structure of the stratum corneum limits the passage of many potentially harmful chemicals into the body.
Microbiological Defense
The epidermal barrier formed by keratinocytes is crucial in preventing the colonization and invasion of pathogenic microorganisms. The physical barrier itself is a significant deterrent, but keratinocytes also actively participate in innate immunity. They produce antimicrobial peptides (AMPs), such as defensins and cathelicidins, which can directly kill bacteria, fungi, and viruses. Additionally, keratinocytes can release cytokines and chemokines that recruit immune cells to the skin, further bolstering its defense against infection.
Prevention of Water Loss and Dehydration
The hydrophobic barrier formed by the lipids secreted between corneocytes in the stratum corneum is indispensable for preventing transepidermal water loss (TEWL). This function is vital for maintaining the skin’s hydration levels and preventing the systemic dehydration that would occur if the body constantly lost fluid through its surface. The tightly packed corneocytes and the lipid matrix work in synergy to create a virtually impermeable layer to water.
Beyond Structure: Keratinocytes in Immunity and Wound Healing
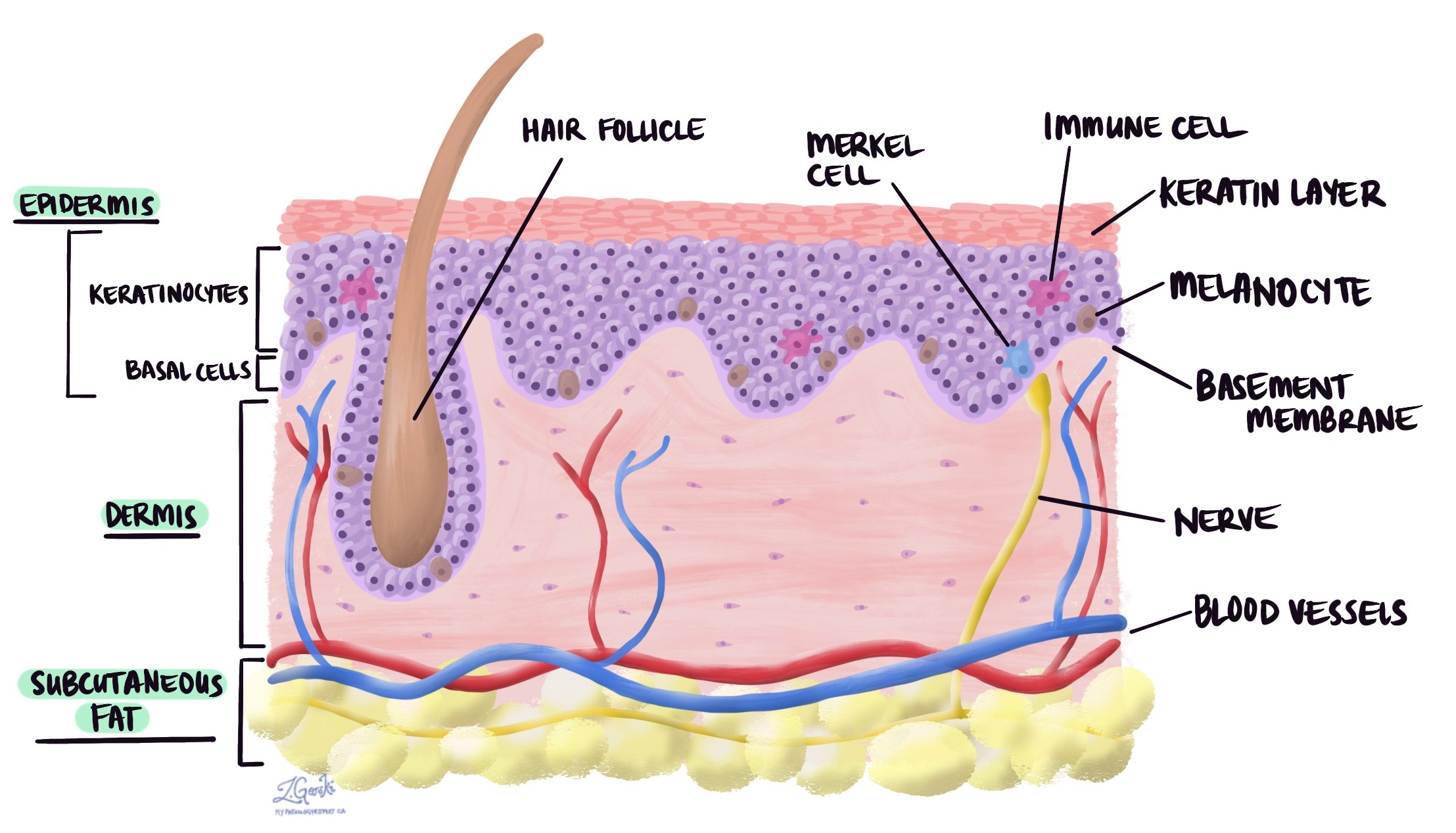
While their role in forming a physical barrier is paramount, keratinocytes are also active participants in the skin’s immune responses and the intricate process of wound healing.
Innate Immune Functions
As mentioned, keratinocytes are not passive participants in defense. They express pattern recognition receptors (PRRs) that can detect pathogen-associated molecular patterns (PAMPs) and damage-associated molecular patterns (DAMPs). Upon sensing these signals, keratinocytes can initiate inflammatory responses by releasing a variety of signaling molecules, including cytokines (e.g., IL-1, IL-6, TNF-α), chemokines (e.g., CXCL8), and growth factors. These molecules recruit immune cells like neutrophils, macrophages, and dendritic cells to the site of infection or injury, initiating a cascade of immune events.
Contribution to Adaptive Immunity
Keratinocytes also interact with antigen-presenting cells (APCs), such as Langerhans cells, which are a type of dendritic cell residing in the epidermis. Langerhans cells capture antigens and migrate to lymph nodes to present them to T cells, initiating adaptive immune responses. Keratinocytes can influence this process by releasing cytokines that modulate the function and maturation of Langerhans cells.
Role in Wound Repair and Regeneration
When the skin is injured, keratinocytes are at the forefront of the healing process. Immediately following injury, keratinocytes at the wound edge undergo changes to facilitate closure. They proliferate, migrate across the wound bed, and differentiate to restore the epidermal barrier. This process involves:
Re-epithelialization
Keratinocytes at the wound margin detach from the basement membrane, increase their motility, and migrate centripetally over the exposed dermis. This process, known as re-epithelialization, covers the wound surface and re-establishes the epidermal continuity. Growth factors released from damaged tissue and inflammatory cells stimulate this migratory and proliferative response.
Granulation Tissue Formation and Remodeling
While keratinocytes are primarily responsible for re-epithelializing the surface, they also interact with fibroblasts in the dermis. They release growth factors that promote fibroblast proliferation and collagen synthesis, contributing to the formation of granulation tissue, which fills the wound defect. As the wound matures, keratinocytes continue to differentiate, contributing to the remodeling of the newly formed tissue.
Signaling and Communication
Keratinocytes are not isolated entities; they are highly communicative cells. They receive and transmit signals from their environment and from other cells within the skin. This intercellular communication is essential for coordinated epidermal function, maintaining homeostasis, and orchestrating responses to stimuli. They communicate via:
Cell-Cell Contact
Through their extensive network of desmosomes and other cell junctions, keratinocytes directly interact with their neighbors. This physical contact allows for the transfer of small molecules and ions and is crucial for maintaining tissue integrity and coordinating cellular behavior.
Paracrine and Autocrine Signaling
Keratinocytes release a wide array of growth factors, cytokines, and chemokines that act on nearby cells (paracrine signaling) or on themselves (autocrine signaling). These signaling molecules regulate keratinocyte proliferation, differentiation, migration, and immune responses. For instance, epidermal growth factor (EGF) and transforming growth factor-alpha (TGF-α) are potent mitogens that stimulate keratinocyte proliferation during wound healing.
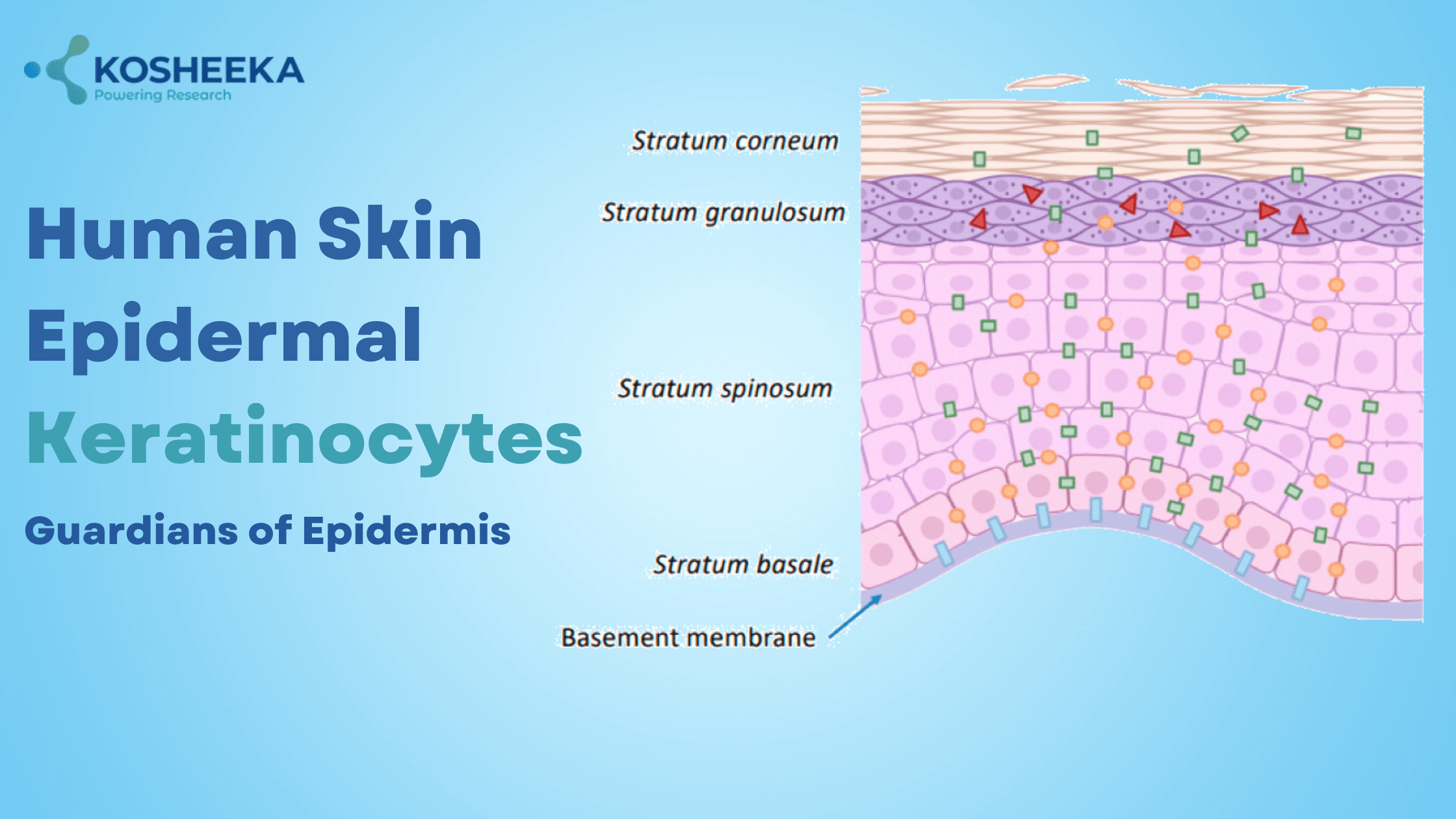
Mechanotransduction
Keratinocytes are sensitive to mechanical forces, such as stretching, pressure, and shear stress. They can convert these mechanical stimuli into biochemical signals, which influence their behavior. This ability, known as mechanotransduction, is important for adapting to physical demands and maintaining skin structure.
In conclusion, keratinocytes are fundamental to the skin’s existence and function. From their origin in the basal layer, through their elaborate differentiation process, to their final role as protective corneocytes, they form the essential barrier that shields us from the world. Their contributions extend far beyond structural support, encompassing vital roles in immunity, wound healing, and continuous communication within the complex ecosystem of the skin. Their multifaceted functions underscore their critical importance to human health and well-being.
