Choosing the “best” contraceptive is a deeply personal and often complex decision, influenced by a myriad of factors unique to each individual’s health, lifestyle, and life stage. There isn’t a single universal answer, as what works optimally for one person may be unsuitable for another. Instead, the quest for the best contraceptive involves a comprehensive understanding of available methods, their efficacy, potential side effects, and how they align with personal priorities and health goals. This exploration delves into the diverse landscape of contraception, providing insights to empower informed choices.
Understanding the Spectrum of Contraceptive Methods
The array of contraceptive options available today is broader and more diverse than ever, each designed with different mechanisms of action, application methods, and effectiveness rates. Categorizing them helps in understanding their fundamental differences.

Hormonal Contraceptives: The Broadest Category
Hormonal methods primarily work by preventing ovulation, thickening cervical mucus to block sperm, or thinning the uterine lining to prevent implantation. They contain either estrogen and progestin (combined methods) or progestin only.
- Combined Oral Contraceptives (The Pill): One of the most common methods, taken daily. Highly effective with perfect use, offering benefits like regulating menstrual cycles and reducing acne. However, effectiveness can decrease with inconsistent use or interactions with certain medications.
- Progestogen-Only Pills (Mini-Pill): Taken daily, particularly suitable for those who cannot use estrogen, such as breastfeeding individuals or those with certain medical conditions. Requires strict adherence to timing.
- Contraceptive Patch: A thin, adhesive patch applied to the skin weekly for three weeks, followed by a patch-free week. Delivers hormones through the skin.
- Vaginal Ring: A flexible ring inserted into the vagina for three weeks, followed by a ring-free week. Releases hormones locally.
- Contraceptive Injection (Depo-Provera): Administered every 12-13 weeks. Highly effective and convenient, but can cause irregular bleeding and potential bone density changes with long-term use.
- Contraceptive Implant (Nexplanon): A small, flexible rod inserted under the skin of the upper arm, releasing progestin. Effective for up to three years, it’s one of the most reliable methods available.
Long-Acting Reversible Contraceptives (LARCs)
LARCs are highly effective, low-maintenance options that can prevent pregnancy for several years. Their “set it and forget it” nature contributes significantly to their high success rates, as they eliminate user error.
- Intrauterine Devices (IUDs):
- Hormonal IUDs (e.g., Mirena, Kyleena, Liletta, Skyla): Small, T-shaped devices inserted into the uterus that release progestin. Effective for 3-8 years, they can reduce menstrual bleeding and pain, and some may even stop periods altogether.
- Copper IUD (e.g., Paragard): A non-hormonal option effective for up to 10-12 years. It works by creating an inflammatory reaction in the uterus that is toxic to sperm and eggs. Can cause heavier or more painful periods in some individuals.
- Contraceptive Implant: As mentioned above, the implant is also considered a LARC due to its long-term effectiveness.
Barrier Methods
These methods physically block sperm from reaching the egg. They are the only contraceptive methods that also offer protection against sexually transmitted infections (STIs), particularly condoms.
- Condoms (Male and Female): Widely accessible and offer dual protection against pregnancy and STIs. Require correct and consistent use for maximum effectiveness.
- Diaphragm and Cervical Cap: Reusable devices inserted into the vagina before intercourse to cover the cervix, used with spermicide. Require fitting by a healthcare provider.
Natural Family Planning (Fertility Awareness Methods)
These methods involve tracking a woman’s menstrual cycle and fertility signs (like basal body temperature and cervical mucus) to identify fertile windows and avoid intercourse during those times. They require significant commitment, training, and consistent tracking, and are generally less effective than hormonal or LARC methods.
Permanent Contraception
For individuals who are certain they do not desire future pregnancies, permanent options offer highly effective, irreversible solutions.
- Vasectomy: A surgical procedure for men that blocks the vas deferens, preventing sperm from reaching the semen. It’s a quick, outpatient procedure with minimal recovery time.
- Tubal Ligation (for women): A surgical procedure that blocks or seals the fallopian tubes, preventing eggs from traveling to the uterus. More invasive than a vasectomy.
Key Factors in Choosing the “Best” Method
Defining the “best” contraceptive requires an individualized assessment based on several critical factors.
Efficacy: Preventing Pregnancy
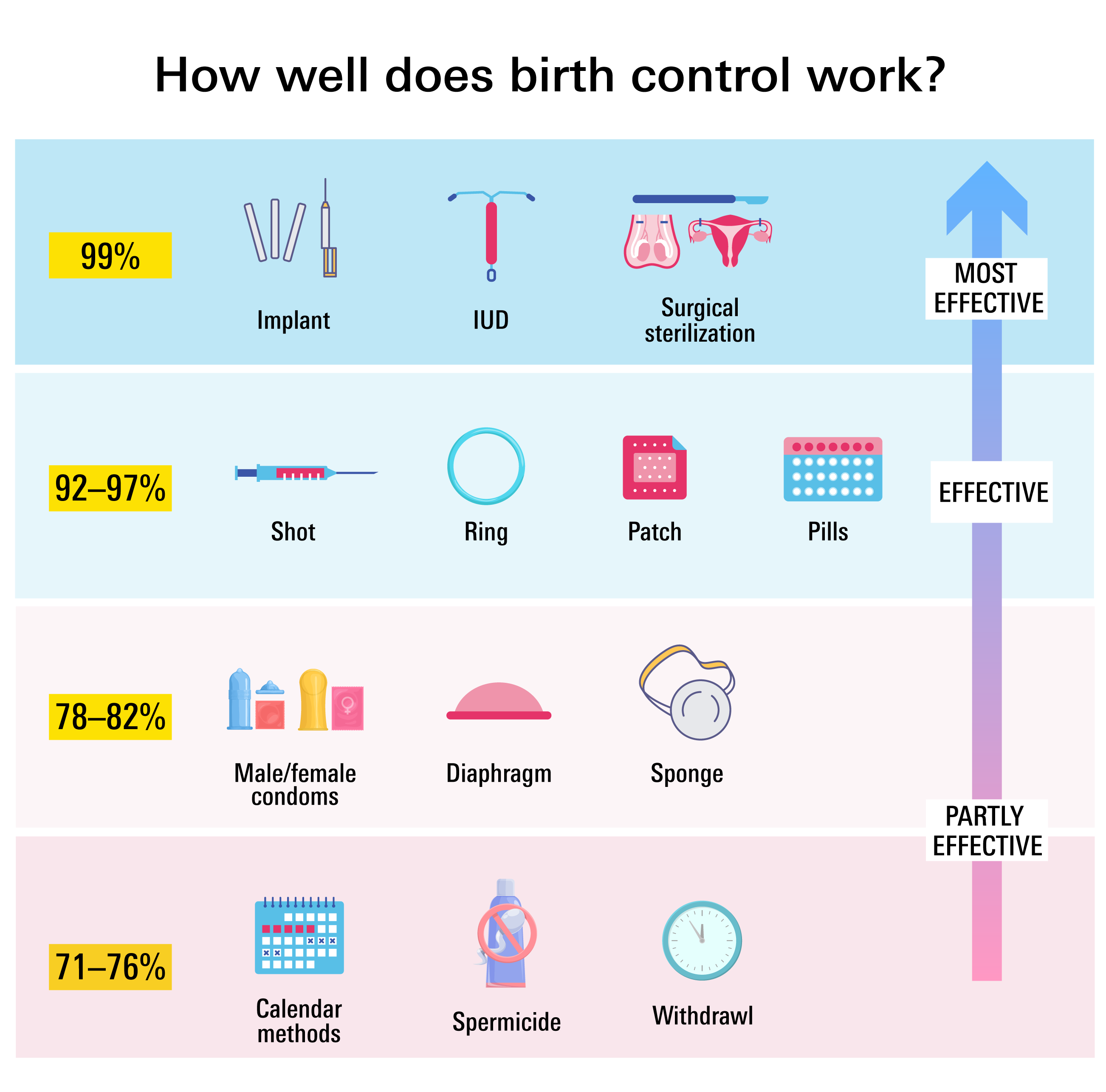
The primary goal of contraception is to prevent unintended pregnancy. Methods vary widely in their effectiveness, categorized by “perfect use” (consistent and correct application every time) and “typical use” (which accounts for human error).
- LARCs (IUDs, Implants): Boast the highest effectiveness rates (over 99%) due to their long-acting nature and independence from daily user action.
- Hormonal Pills, Patches, Rings, Injections: Highly effective with perfect use (91-99%), but typical use rates can drop due to missed doses or improper application.
- Barrier Methods (Condoms): With perfect use, male condoms are 98% effective, but typical use drops to 87%. They require diligence and correct application.
- Natural Family Planning: Can range from 76-88% effective with typical use, significantly lower than other methods.
Health Considerations and Side Effects
Each contraceptive method has its own profile of potential side effects and health implications.
- Hormonal methods can influence menstrual cycles (lighter, heavier, or absent periods), mood, weight, and sometimes increase the risk of blood clots (especially combined methods). Some individuals might experience headaches or breast tenderness.
- Non-hormonal methods like the copper IUD may lead to heavier or more painful periods, especially initially. Barrier methods generally have fewer systemic side effects but may cause irritation or allergic reactions in some.
- STI Protection: Crucially, only barrier methods like condoms protect against sexually transmitted infections. For comprehensive protection, condoms should be used in conjunction with other contraceptive methods.
Lifestyle and Personal Preferences
The practicalities of incorporating a contraceptive method into daily life are paramount.
- Ease of Use and Adherence: Daily pills require discipline. LARCs offer significant convenience.
- Frequency of Application/Administration: From daily (pills) to every few years (IUDs, implants).
- Desire for Future Fertility: LARCs offer quick return to fertility upon removal, while the injection can delay it for several months. Permanent methods are irreversible.
- Privacy and Discretion: Some methods are more discreet than others, which can be a significant factor for some individuals.
Cost and Accessibility
The financial investment and ease of obtaining a method can also influence choice. While many methods are covered by insurance or available at low cost through public health programs, the initial outlay or ongoing expense can vary.
Navigating the Decision: A Personalized Approach
Given the complexity, selecting the best contraceptive is a journey best undertaken with professional guidance.
Consulting Healthcare Professionals
An open and honest dialogue with a doctor, gynecologist, or family planning specialist is crucial. They can assess:
- Medical History and Current Health: Certain medical conditions (e.g., blood clotting disorders, migraines, breast cancer) or medications might contraindicate specific methods.
- Individual Risks and Benefits: Discussing personal risk factors and weighing the advantages and disadvantages of each option based on your unique profile.
- Family Planning Goals: Whether you plan to have children in the future, and if so, when.
Re-evaluating Choices Over Time
Life circumstances change, and so might your contraceptive needs. It’s advisable to periodically review your chosen method with your healthcare provider. Changes in relationship status, health, lifestyle, or future family planning goals might necessitate a switch to a more suitable option. Open communication with partners about contraceptive choices and sexual health is also vital.
The Role of Innovation in Contraception
The field of contraception continues to evolve, driven by ongoing research and technological advancements. Innovations aim to enhance effectiveness, reduce side effects, improve user experience, and expand options.
Advancements in Formulation and Delivery
Modern contraception has seen significant progress in refining existing methods. This includes:
- Lower Hormone Doses: Development of pills and other hormonal methods with reduced hormone levels to minimize side effects while maintaining efficacy.
- Extended Cycle Regimens: Pills designed for continuous use, reducing the frequency of periods or eliminating them altogether, offering convenience and potentially reducing menstrual-related symptoms.
- New LARC Technologies: Continuous refinement of IUDs and implants for easier insertion, better comfort, and longer effective durations. For example, smaller hormonal IUDs have been developed for nulliparous women.
- On-Demand Contraception: Research into novel methods that can be used just before or after intercourse, offering more control than daily or weekly methods.

Future Directions and Research
The future of contraception holds exciting possibilities, with significant research focused on addressing unmet needs.
- Male Contraception: A major area of innovation is the development of effective, reversible contraceptive options for men. This includes hormonal gels or pills that suppress sperm production, and non-hormonal methods like RISUG (Reversible Inhibition of Sperm Under Guidance), which involves injecting a polymer into the vas deferens to block sperm.
- Non-Hormonal Options for Women: Efforts are underway to develop more diverse non-hormonal methods for women, catering to those who experience adverse effects from hormonal contraception or prefer hormone-free solutions. This includes exploring new barrier methods and agents that affect sperm viability or egg implantation without systemic hormonal changes.
- Digital Health Tools for Fertility Awareness: Advancements in wearable technology and smartphone applications are enhancing the accuracy and ease of fertility awareness methods, providing more precise data for individuals wishing to track their cycles naturally.
- Tailored Medicine: The long-term vision involves more personalized contraceptive solutions, potentially guided by genetic profiles or individual metabolic responses to different hormone formulations, minimizing trial and error.
Ultimately, the “best” contraceptive is the one that an individual consistently uses, that meets their health requirements, aligns with their lifestyle, and effectively prevents unintended pregnancy while supporting their overall well-being. This choice should be an ongoing conversation with a trusted healthcare provider, adapting as life evolves and as innovative solutions emerge.
