Understanding the Nuances of Fecal Consistency
The appearance and consistency of feces can offer valuable insights into an individual’s digestive health. While variations are common and often harmless, understanding what constitutes “normal” can help in identifying potential issues. This article delves into the characteristics of sticky poop, exploring its potential causes, implications, and when it might warrant medical attention.
The Spectrum of Stool Consistency
Before examining sticky stool specifically, it’s helpful to understand the broader spectrum of fecal consistency. This is often categorized using the Bristol Stool Scale, a medical aid that classifies stool into seven types. This scale was developed by researchers at the University of Bristol, UK, and is widely used by healthcare professionals to assess stool form.

The Bristol Stool Scale Explained
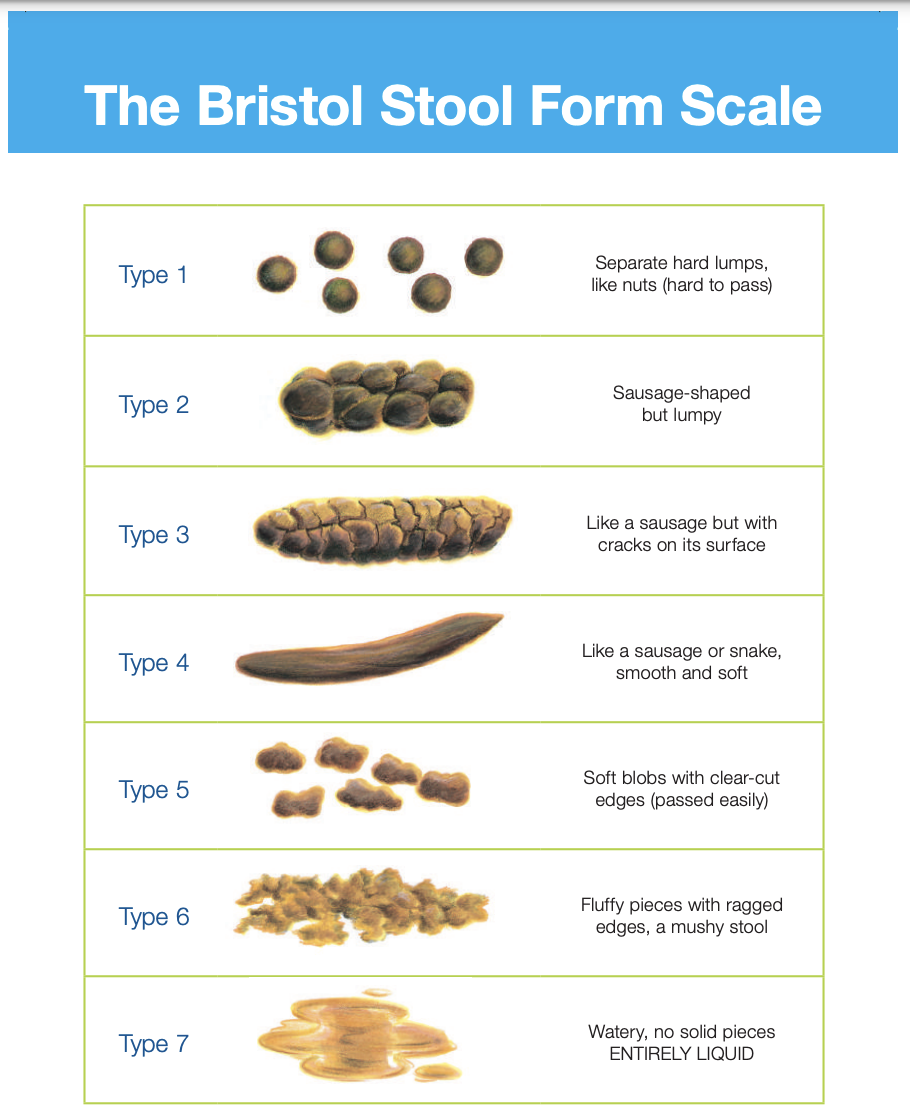
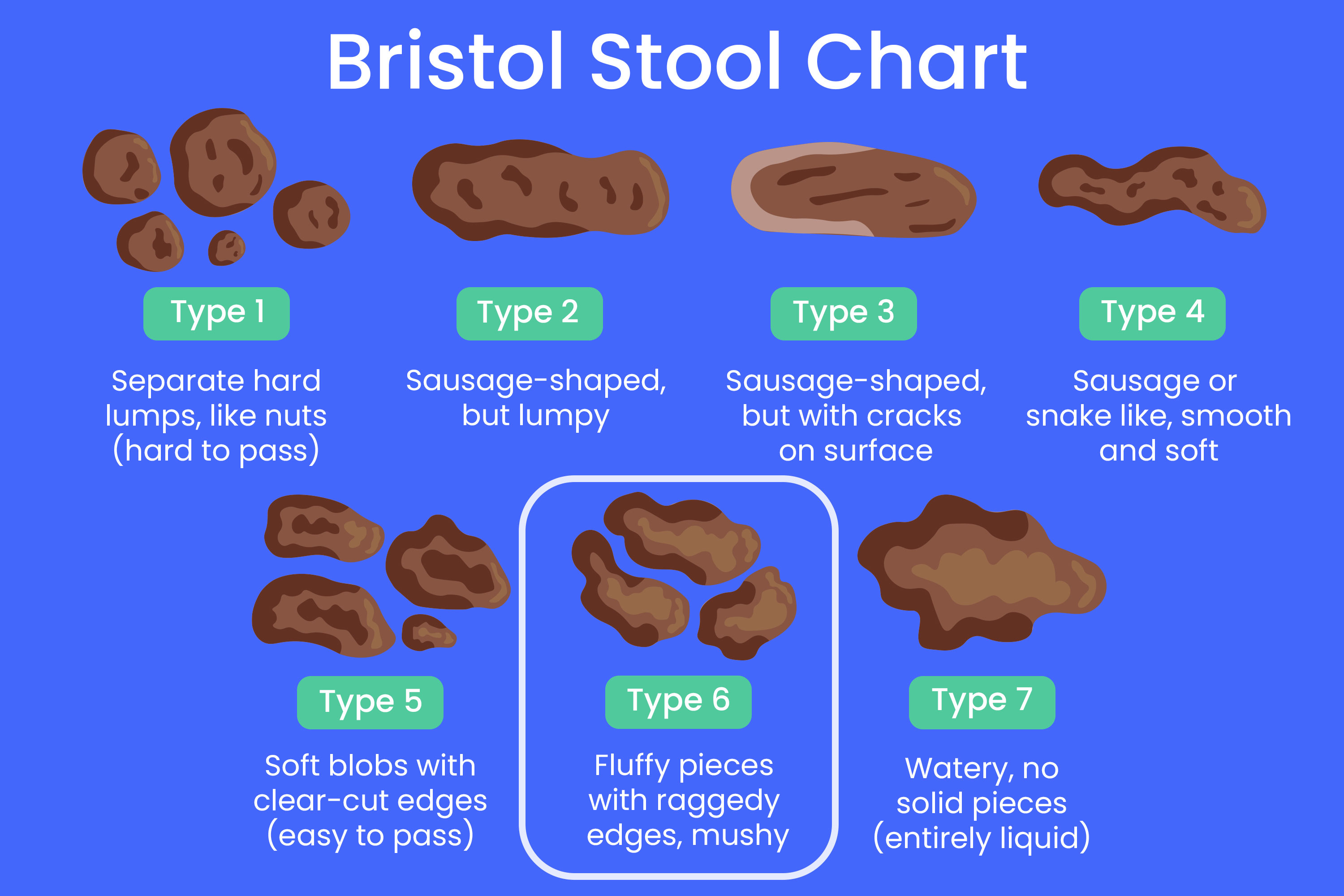
The Bristol Stool Scale provides a visual representation of different stool types, ranging from hard lumps to liquid. Each type is associated with a different transit time through the colon, which is the amount of time food takes to pass through the digestive system.
-
Type 1: Separate hard lumps, like nuts (hard to pass)
- This type indicates very slow transit time, often associated with constipation. The stool has spent a long time in the colon, allowing excessive water to be absorbed, making it hard and difficult to expel.
-
Type 2: Sausage-shaped but lumpy
- Also indicative of constipation, though slightly less severe than Type 1. The stool is still hard and takes longer than average to pass.
-
Type 3: Like a sausage but with cracks on its surface
- This type is considered normal by some standards, though it can still indicate mild constipation or a need for more fiber. The stool is passing, but its consistency suggests it could be more easily expelled.
-
Type 4: Like a sausage or snake, smooth and soft
- This is widely considered the ideal, normal stool form. It passes easily and indicates a healthy transit time and balanced hydration and fiber intake.
-
Type 5: Soft blobs with clear-cut edges (passed easily)
- This type suggests a faster transit time than Type 4. While still within a normal range for many, it can sometimes indicate the beginning of looser stools.
-
Type 6: Fluffy pieces with ragged edges, a mushy stool
- This category represents looser stools than normal. It suggests a faster transit time and potentially a need to re-evaluate diet or hydration. This is where “sticky poop” often falls on the spectrum.
-
Type 7: Entirely liquid, no solid pieces. Entirely passed as water.
- This is diarrhea, indicating a very rapid transit time. The stool has little to no water absorbed, often due to an underlying cause such as infection, food intolerance, or medication side effect.
Sticky poop typically falls into the Type 6 category on the Bristol Stool Scale. It’s characterized by its mushy consistency, often clinging to the toilet bowl and being difficult to flush. While not as severe as outright diarrhea (Type 7), it signifies a departure from the ideal, easily passed stool.
Potential Causes of Sticky Poop
Several factors can contribute to stool becoming sticky. These range from dietary choices to underlying medical conditions. Understanding these potential causes is the first step in addressing the issue.
Dietary Factors
The food we consume has a direct impact on our digestive system and the consistency of our stool.
-
High Fat Intake: A diet rich in fats, particularly saturated and unhealthy fats, can lead to the malabsorption of fat. When the body cannot efficiently break down and absorb fats, they pass through the digestive tract largely undigested. This undigested fat can coat the stool, giving it a greasy or sticky appearance and making it more difficult to flush. This condition is known as steatorrhea. Foods high in fat include fried foods, fatty cuts of meat, butter, cream, and processed snacks.
-
Low Fiber Intake: Fiber plays a crucial role in adding bulk to stool and regulating its consistency. Soluble fiber absorbs water, forming a gel-like substance that softens stool, while insoluble fiber adds bulk and helps it move through the intestines more quickly. A diet lacking in fiber can result in harder, drier stools that are more difficult to pass. However, a sudden increase in fiber without adequate hydration can also sometimes lead to looser stools initially as the digestive system adjusts. Conversely, a very low fiber diet might contribute to stool that doesn’t form well, leading to a stickier consistency. Good sources of fiber include fruits, vegetables, whole grains, legumes, nuts, and seeds.
-
Dairy Intolerance or Lactose Intolerance: For individuals who are lactose intolerant, consuming dairy products can lead to digestive distress. Undigested lactose ferments in the gut, producing gas and causing diarrhea, which can manifest as sticky or loose stools. This is because the body lacks sufficient lactase, the enzyme needed to break down lactose.
-
Artificial Sweeteners and Sugar Alcohols: Certain artificial sweeteners and sugar alcohols, such as sorbitol, mannitol, and xylitol, found in sugar-free gums, candies, and diet drinks, can have a laxative effect. They are poorly absorbed in the small intestine and can draw water into the colon, leading to looser, stickier stools.
-
Spicy Foods: While not a direct cause for everyone, for some individuals, very spicy foods can irritate the digestive lining, leading to faster transit and looser stools.
Medical Conditions and Malabsorption
Beyond diet, certain medical conditions can impair the digestive system’s ability to absorb nutrients, leading to changes in stool consistency.
- Malabsorption Syndromes: These are conditions where the body is unable to absorb essential nutrients from food. Examples include:
- Celiac Disease: An autoimmune disorder triggered by gluten, which damages the lining of the small intestine and impairs nutrient absorption. This often leads to steatorrhea (fatty stools), which are typically greasy, foul-smelling, and sticky.
- Crohn’s Disease and Ulcerative Colitis (Inflammatory Bowel Diseases – IBD): These chronic inflammatory conditions of the digestive tract can affect nutrient absorption and alter bowel motility, leading to various stool changes, including stickiness and diarrhea.
- Pancreatic Insufficiency: The pancreas produces enzymes essential for digesting fats, proteins, and carbohydrates. If the pancreas doesn’t produce enough of these enzymes, fats are not properly digested, leading to steatorrhea. This can be caused by conditions like pancreatitis or cystic fibrosis.
-
Infections: Bacterial, viral, or parasitic infections of the gastrointestinal tract can cause inflammation and rapid transit, leading to diarrhea and sticky stools. This is often accompanied by other symptoms like nausea, vomiting, abdominal cramps, and fever.
-
Irritable Bowel Syndrome (IBS): IBS is a common disorder that affects the large intestine. Symptoms can vary widely but often include abdominal pain, bloating, gas, constipation, and diarrhea. For individuals with IBS who experience diarrhea-predominant IBS (IBS-D), sticky stools can be a common occurrence.
-
Gallbladder or Liver Issues: The liver produces bile, which aids in fat digestion and is stored in the gallbladder. Problems with the gallbladder or liver can affect bile production and flow, potentially leading to impaired fat digestion and steatorrhea.
Medications
Certain medications can have side effects that affect bowel movements and stool consistency.
-
Antibiotics: Antibiotics are designed to kill bacteria, but they can also disrupt the balance of beneficial bacteria in the gut. This disruption can lead to an overgrowth of certain organisms or changes in gut function, resulting in diarrhea and sticky stools.
-
Antacids containing Magnesium: Some antacids that contain magnesium can have a laxative effect and lead to looser stools.
-
Chemotherapy Drugs: These powerful medications can significantly impact the digestive system, often causing diarrhea, nausea, and changes in stool.
-
Certain Weight-Loss Medications: Some medications designed for weight loss work by blocking fat absorption. While intended to reduce calorie intake, a common side effect is the passage of oily stools, which are characteristically sticky.
When to Seek Medical Advice
While occasional episodes of sticky poop might be attributed to a transient dietary indiscretion or a mild illness, persistent changes or accompanying symptoms warrant medical attention.
Red Flags to Consider
- Persistence: If sticky stools continue for more than a few days and are not clearly linked to a specific dietary change or a minor, resolving illness.
- Accompanying Symptoms: The presence of other concerning symptoms alongside sticky stools is a strong indicator to consult a doctor. These include:
- Unexplained weight loss
- Severe abdominal pain or cramping
- Blood or mucus in the stool
- Persistent nausea or vomiting
- Fever
- Signs of dehydration (e.g., dark urine, dry mouth, dizziness)
- Jaundice (yellowing of the skin or eyes)
- Changes in Stool Color: While sticky stools are often pale or light brown due to fat content, significant changes in color (e.g., black, tarry, or white stools) should always be investigated.
- Foul Odor: While stool typically has an odor, a significantly more foul or pungent smell, especially when coupled with other symptoms, can indicate malabsorption or infection.
The Diagnostic Process
When you consult a healthcare professional about sticky stools, they will typically:
- Take a Detailed Medical History: This will include questions about your diet, lifestyle, recent travel, medications, and any other symptoms you are experiencing.
- Perform a Physical Examination: This may include an abdominal exam to check for tenderness or distension.
- Order Stool Tests: These tests can help identify infections, check for blood, and analyze fat content (fecal fat test) to diagnose steatorrhea.
- Conduct Blood Tests: Blood tests can help assess for inflammation, nutrient deficiencies, and markers of conditions like celiac disease or IBD.
- Consider Imaging Studies: Depending on the suspected cause, an endoscopy, colonoscopy, or imaging tests like an ultrasound or CT scan might be recommended.
Managing Sticky Poop
The management of sticky poop depends entirely on its underlying cause.
Dietary Adjustments
If sticky stools are linked to diet:
- Reduce Fat Intake: Gradually decrease the consumption of high-fat foods, especially processed and fried items. Opt for leaner protein sources, healthy fats in moderation (like avocado, nuts, and olive oil), and limit butter and cream.
- Increase Fiber Gradually: If low fiber is a suspected issue, slowly incorporate more fruits, vegetables, whole grains, and legumes into your diet. Ensure adequate water intake when increasing fiber to prevent constipation.
- Identify and Avoid Trigger Foods: If lactose intolerance or sensitivity to artificial sweeteners is suspected, trial elimination diets under medical guidance.
- Stay Hydrated: Drink plenty of water throughout the day, which is crucial for overall digestive health and stool consistency.
Medical Treatments
If an underlying medical condition is diagnosed, treatment will be tailored to that specific condition:
- For Celiac Disease: A strict gluten-free diet is essential.
- For IBD: Treatment often involves anti-inflammatory medications, immunosuppressants, and lifestyle modifications.
- For Pancreatic Insufficiency: Enzyme replacement therapy is prescribed.
- For Infections: Appropriate antibiotics or antiparasitic medications will be used.
- For IBS: Management may include dietary changes, stress management techniques, and medications to manage specific symptoms.
Lifestyle Changes
- Stress Management: Chronic stress can significantly impact digestive health. Techniques like mindfulness, yoga, or regular exercise can be beneficial.
- Regular Exercise: Physical activity promotes regular bowel movements and can aid in digestion.
In conclusion, while the term “sticky poop” might sound unpleasant, understanding its potential causes and implications is vital for maintaining good health. It serves as a signal from your body, and by paying attention to such signals and seeking appropriate medical advice when necessary, you can effectively address digestive concerns and ensure overall well-being.
