Kidney disease, also known as chronic kidney disease (CKD), is a progressive condition characterized by a gradual loss of kidney function over time. The kidneys are vital organs responsible for filtering waste products and excess fluid from the blood, producing hormones that help control blood pressure, red blood cell production, and bone health. When kidney function declines, these essential tasks are compromised, leading to a range of health problems. Kidney disease is typically staged based on the estimated glomerular filtration rate (eGFR), which measures how effectively the kidneys are filtering waste. Stage 3a kidney disease represents a specific point in this progression, indicating a moderate but still significant reduction in kidney function. Understanding the characteristics, causes, symptoms, and management of Stage 3a CKD is crucial for individuals diagnosed with this condition and their healthcare providers.
Understanding Kidney Function and Staging
The kidneys are complex organs with millions of tiny filtering units called nephrons. Each nephron contains a glomerulus, a cluster of small blood vessels that filters blood. The Glomerular Filtration Rate (GFR) is a measure of how much blood passes through the glomeruli each minute. It is the best overall index of kidney function. An eGFR, or estimated GFR, is calculated using a blood test that measures creatinine levels, along with factors like age, sex, and race.
The stages of CKD are defined as follows:
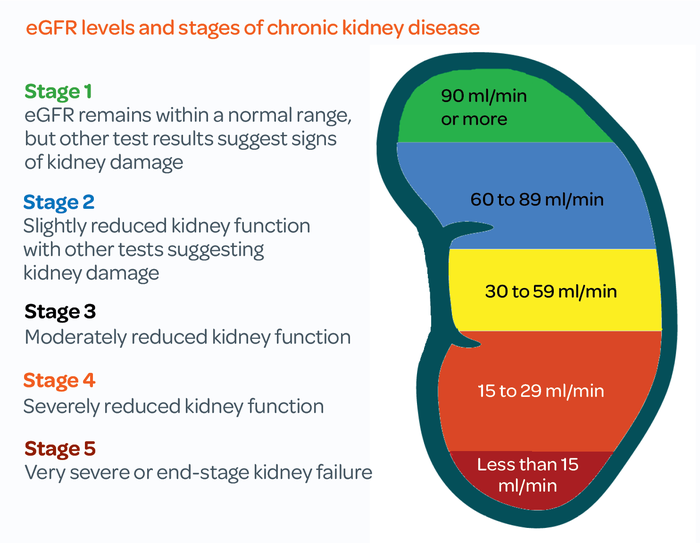
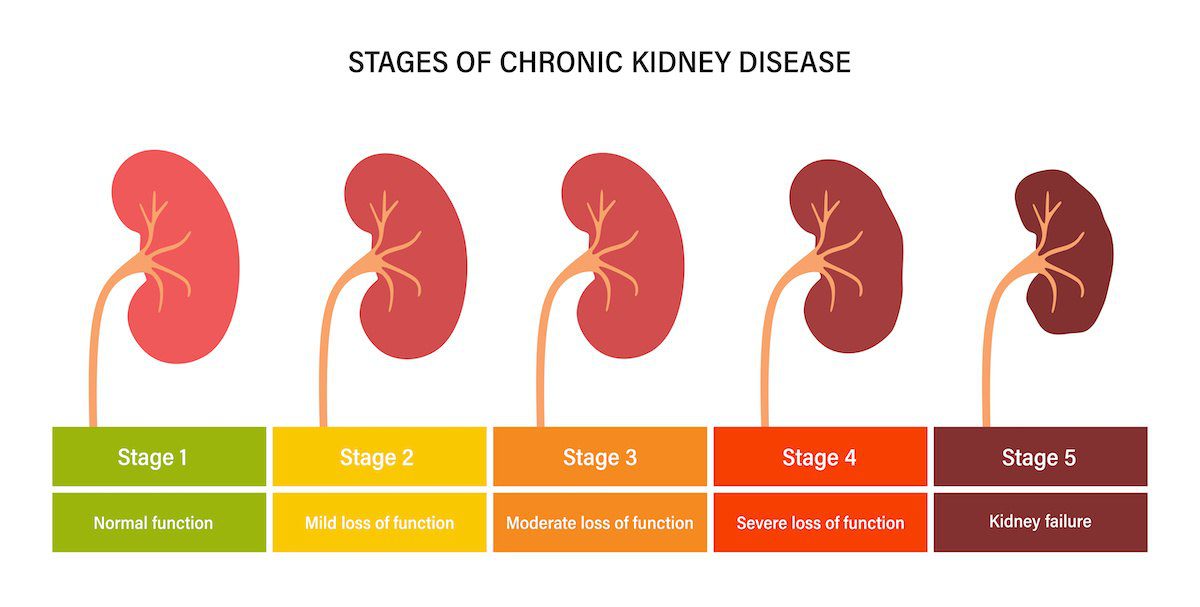
- Stage 1: GFR of 90 or higher, with evidence of kidney damage (e.g., protein in the urine). Kidney function is still normal or nearly normal.
- Stage 2: GFR between 60 and 89, with evidence of kidney damage. Kidney function is slightly reduced.
- Stage 3: GFR between 30 and 59. This stage is further divided into two sub-stages:
- Stage 3a: GFR between 45 and 59. This is the focus of our discussion.
- Stage 3b: GFR between 30 and 44.
- Stage 4: GFR between 15 and 29. Severe loss of kidney function.
- Stage 5: GFR less than 15. Kidney failure, requiring dialysis or a kidney transplant.
Therefore, Stage 3a kidney disease signifies a GFR in the range of 45-59 mL/min/1.73m². While kidney function is reduced, it is not yet considered severe. However, it represents a significant decline from normal, and proactive management is essential to slow the progression of the disease and prevent complications.
The Significance of eGFR in Staging
The eGFR is the cornerstone of CKD staging. It provides a quantitative measure of the kidneys’ ability to filter waste, making it an objective indicator of disease severity. A lower eGFR directly correlates with impaired kidney function. In Stage 3a, the kidneys are still performing a substantial portion of their filtering duties, but they are working harder and less efficiently. This reduced efficiency can lead to a buildup of waste products and fluid in the body, as well as hormonal imbalances.
Differentiating Stage 3a from Stage 3b
The distinction between Stage 3a and Stage 3b is based on the specific eGFR range. While both fall under the umbrella of moderate kidney disease, Stage 3b indicates a more advanced stage of decline than Stage 3a. This differentiation is important for guiding treatment strategies and predicting the rate of progression. Patients in Stage 3b may experience more pronounced symptoms and face a higher risk of complications compared to those in Stage 3a.
Causes and Risk Factors for Stage 3a Kidney Disease
Several underlying conditions can lead to the development and progression of kidney disease, ultimately resulting in Stage 3a CKD. Identifying and managing these risk factors is paramount for prevention and slowing disease progression.
Diabetes Mellitus
Diabetes is the leading cause of chronic kidney disease worldwide. High blood glucose levels over extended periods can damage the delicate blood vessels within the glomeruli, impairing their filtering ability. This condition is often referred to as diabetic nephropathy. Effectively managing blood sugar levels through diet, exercise, and medication is crucial for individuals with diabetes to protect their kidney health.
High Blood Pressure (Hypertension)
Hypertension is the second leading cause of CKD. High blood pressure exerts increased force on the blood vessels throughout the body, including those in the kidneys. Over time, this sustained pressure can damage the arteries supplying the kidneys, leading to reduced blood flow and impaired function. Managing blood pressure through lifestyle modifications and medication is vital for kidney protection.
Glomerulonephritis
Glomerulonephritis refers to a group of diseases that cause inflammation and damage to the glomeruli. This inflammation can stem from various causes, including infections, autoimmune diseases (like lupus), or as a primary kidney disorder. When glomeruli are inflamed, they become less efficient at filtering waste and can allow protein and blood to leak into the urine.
Polycystic Kidney Disease (PKD)
PKD is a genetic disorder characterized by the growth of numerous cysts in the kidneys. These cysts can enlarge the kidneys and impair their function over time. While PKD is a hereditary condition, its progression can be influenced by lifestyle and medical management.
Other Contributing Factors
- Obesity: Obesity is often linked to diabetes and hypertension, both major risk factors for CKD. Excess weight can also put direct strain on the kidneys.
- Family History: A family history of kidney disease increases an individual’s risk.
- Age: The risk of kidney disease increases with age, as kidney function naturally declines over time.
- Certain Medications: Prolonged use of certain medications, such as non-steroidal anti-inflammatory drugs (NSAIDs), can potentially harm the kidneys.
- Autoimmune Diseases: Conditions like lupus and rheumatoid arthritis can attack the kidneys.
- Recurrent Kidney Infections: Repeated urinary tract infections can sometimes lead to kidney damage.
Symptoms and Diagnosis of Stage 3a Kidney Disease
In the earlier stages of CKD, including Stage 3a, many individuals may experience few or no noticeable symptoms. This is often why kidney disease goes undiagnosed until it has progressed to more advanced stages. However, as kidney function continues to decline, subtle signs may begin to emerge.
Subtle or Absent Symptoms
The insidious nature of early-stage CKD means that symptoms are often vague and can be attributed to other conditions. Some individuals may report:
- Fatigue: A general feeling of tiredness or lack of energy.
- Swelling: Mild swelling in the hands, feet, or ankles due to fluid retention.
- Changes in Urination: More frequent urination, especially at night, or changes in the color or appearance of urine.
- Loss of Appetite: A reduced desire to eat.
- Itching: Persistent itching on the skin.
- Muscle Cramps: Particularly at night.
As the disease progresses into Stage 3a, these symptoms may become slightly more pronounced, but they are still often mild enough to be overlooked.
Diagnostic Process
The diagnosis of Stage 3a kidney disease relies on a combination of medical history, physical examination, and laboratory tests.
- Blood Tests: The most critical diagnostic tool is the blood test to estimate the GFR. This involves measuring serum creatinine levels and using an eGFR formula. Other blood tests may be performed to assess electrolyte balance, anemia, and calcium/phosphorus levels.
- Urine Tests: Urinalysis can detect the presence of protein (proteinuria) or blood (hematuria) in the urine, which are indicators of kidney damage. A 24-hour urine collection may be ordered to quantify the amount of protein being lost.
- Imaging Tests: Ultrasound or CT scans of the kidneys may be used to visualize the size and structure of the kidneys, detect any abnormalities, blockages, or cysts.
- Kidney Biopsy: In some cases, a kidney biopsy may be recommended to obtain a small sample of kidney tissue for microscopic examination. This can help identify the specific cause of kidney damage.
Early and regular screening, especially for individuals with risk factors like diabetes and hypertension, is essential for detecting Stage 3a CKD before significant damage occurs.
Management and Treatment of Stage 3a Kidney Disease
The primary goals of managing Stage 3a kidney disease are to slow the progression of the disease, prevent complications, and maintain the best possible quality of life. While Stage 3a CKD is not reversible, a comprehensive management plan can significantly impact its course.
Lifestyle Modifications
Significant changes in lifestyle play a crucial role in managing Stage 3a CKD.
- Dietary Adjustments:
- Sodium Restriction: Limiting sodium intake helps manage blood pressure and fluid retention.
- Protein Intake: While not always necessary in Stage 3a, a healthcare provider may advise moderation in protein intake to reduce the workload on the kidneys.
- Potassium and Phosphorus: Monitoring potassium and phosphorus levels may become important as kidney function declines.
- Fluid Intake: Maintaining adequate hydration is important, but excessive fluid intake might be discouraged if there’s a risk of fluid overload.
- Regular Exercise: Physical activity helps control blood pressure, manage weight, and improve overall cardiovascular health, all of which benefit kidney function.
- Smoking Cessation: Smoking significantly exacerbates kidney damage and should be quit immediately.
- Weight Management: Achieving and maintaining a healthy weight can reduce the strain on the kidneys.
Medical Management
Medications are often prescribed to address underlying conditions and manage symptoms.
- Blood Pressure Control: Antihypertensives are crucial for managing high blood pressure. Angiotensin-converting enzyme (ACE) inhibitors and angiotensin II receptor blockers (ARBs) are often favored as they can also help protect the kidneys from further damage.
- Blood Sugar Control: For individuals with diabetes, strict blood sugar management is paramount.
- Cholesterol-Lowering Medications: Statins may be prescribed to manage high cholesterol levels, which are common in CKD.
- Anemia Management: As CKD progresses, the kidneys may produce less erythropoietin, a hormone that stimulates red blood cell production, leading to anemia. Iron supplements and erythropoiesis-stimulating agents (ESAs) may be used.
- Medication Review: Healthcare providers will carefully review all medications, including over-the-counter drugs and supplements, to ensure they are safe for individuals with impaired kidney function and to avoid potential nephrotoxic agents.

Monitoring and Follow-Up
Regular monitoring is essential to track the progression of kidney disease and adjust treatment as needed.
- Regular eGFR and Blood Pressure Checks: Frequent monitoring of eGFR and blood pressure helps assess treatment effectiveness and detect any worsening of kidney function.
- Urine Protein Monitoring: Regular urine tests for protein can indicate ongoing kidney damage.
- Electrolyte and Mineral Monitoring: Blood tests to monitor levels of potassium, phosphorus, calcium, and other electrolytes are important.
While Stage 3a kidney disease represents a moderate decline in kidney function, proactive management through lifestyle changes, medical treatment, and consistent monitoring can significantly impact its long-term prognosis. Early diagnosis and a collaborative approach with healthcare providers are key to preserving kidney health and overall well-being.
