Medicaid’s Modified Adjusted Gross Income (MAGI) is a pivotal concept that fundamentally reshaped how eligibility for Medicaid and the Children’s Health Insurance Program (CHIP) is determined for many individuals and families. Prior to the implementation of MAGI rules, the calculation of household income for these programs was a complex and often inconsistent process, varying significantly by state and program. The Affordable Care Act (ACA) brought about a standardized approach, aiming to simplify the application process and ensure greater fairness and predictability in who qualifies for these essential health coverage programs. Understanding MAGI is crucial for anyone navigating the landscape of public health insurance in the United States.
The Evolution of Medicaid Eligibility
Before MAGI, Medicaid eligibility was primarily determined by looking at specific categories of need, such as disability, age, or family status, and then applying a set of income and asset tests that were unique to each category. For instance, eligibility for pregnant women might have been based on a different income threshold than for a low-income parent or an elderly individual. This categorical approach, while intended to serve vulnerable populations, created a fragmented system.
Pre-MAGI Challenges
The pre-MAGI system presented several significant challenges:
- Complexity and Confusion: Applicants often struggled to understand which rules applied to them, leading to frustration and incorrect applications. The variations in state-specific rules further exacerbated this issue, making it difficult for individuals moving between states to maintain coverage.
- Inconsistent Coverage: Individuals with similar financial circumstances could receive different eligibility outcomes depending on the specific Medicaid category they applied under or the state they resided in.
- Administrative Burden: State agencies faced a substantial administrative burden in managing multiple sets of eligibility rules, processing applications, and conducting reviews. This often led to higher operational costs and longer processing times.
- Asset Tests: Many pre-MAGI Medicaid categories included asset tests, requiring applicants to deplete their savings or liquidate certain assets to qualify. This could be particularly detrimental for individuals seeking long-term care services.
The Affordable Care Act’s Impact
The ACA, enacted in 2010, sought to address these shortcomings by introducing the MAGI methodology. The primary goal was to create a more streamlined, equitable, and accessible system for determining eligibility for Medicaid and CHIP. The MAGI rules largely standardized how income is calculated, making it more consistent across different household types and for various public assistance programs.
Understanding Modified Adjusted Gross Income (MAGI)
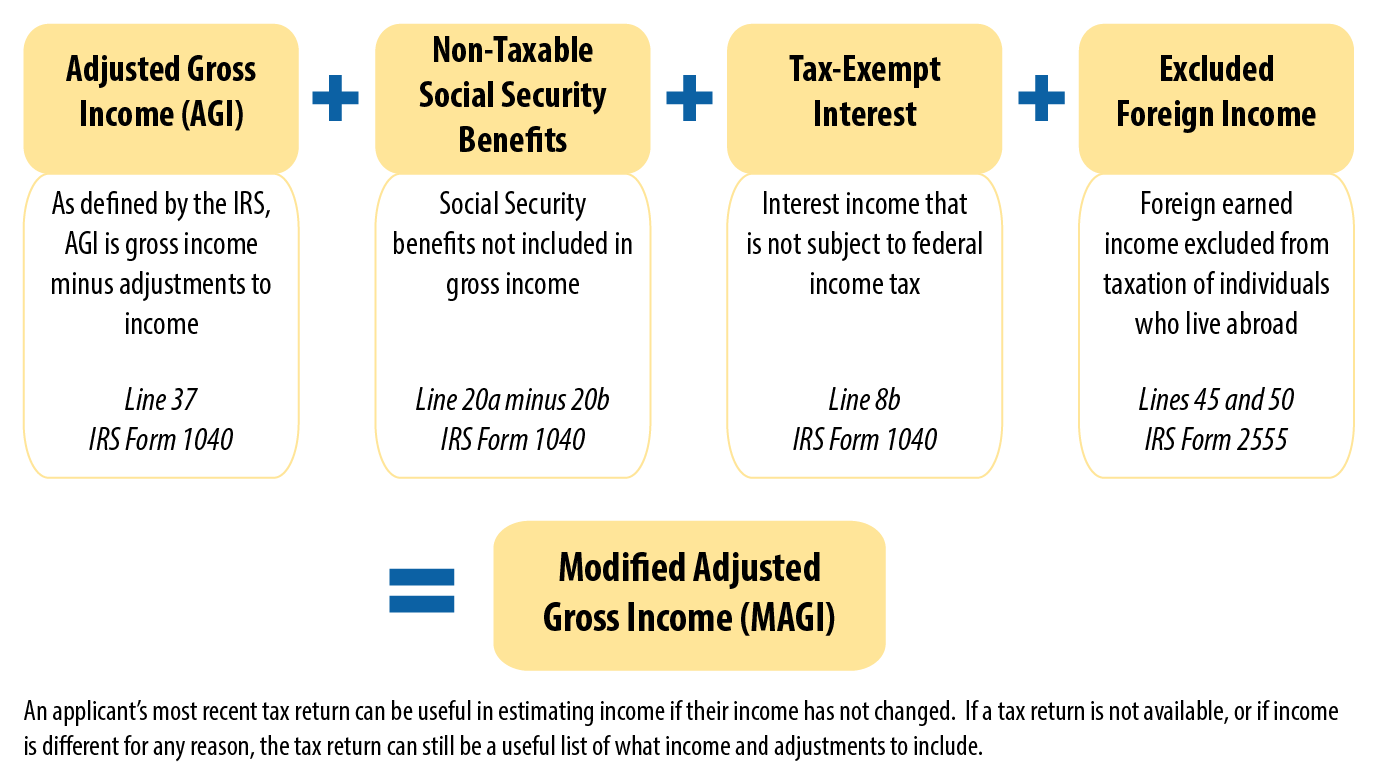
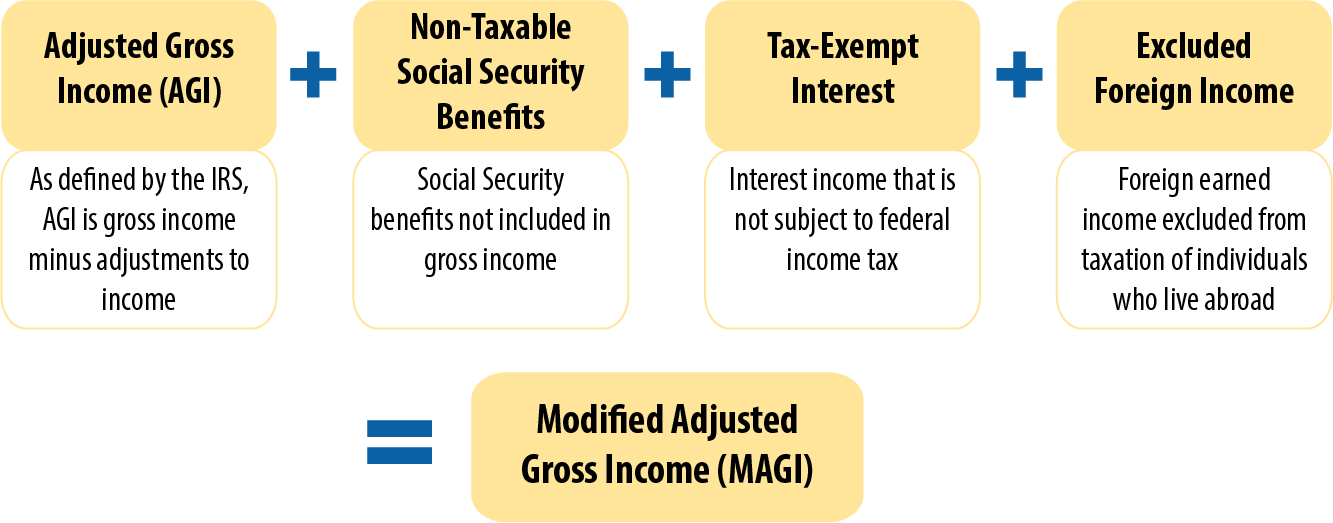
At its core, MAGI is a specific definition of income derived from the U.S. tax code. It’s not a new concept; it’s a figure that most taxpayers are already familiar with from their federal income tax returns. For Medicaid and CHIP purposes, MAGI represents a modified version of Adjusted Gross Income (AGI). The “modification” involves adding back certain deductions that are typically allowed on tax returns and excluding others that are specific to tax code benefits but not relevant to assessing a household’s ability to pay for healthcare.
Key Components of MAGI for Medicaid
The calculation of MAGI for Medicaid and CHIP purposes focuses on several key components of income:
- Wages, Salaries, and Tips: This is the most straightforward component, representing income earned from employment.
- Taxable Interest and Dividends: Income from investments is generally included.
- Business Income: Net income from self-employment or small businesses is considered.
- Retirement Income: Distributions from pensions, annuities, and individual retirement accounts (IRAs) are typically included.
- Unemployment Compensation: Benefits received from unemployment insurance are counted.
- Alimony Received: For divorces finalized after December 31, 2018, alimony received is considered income.
- Rental Property Income (Net): Income from rental properties, after deducting expenses, is included.
- Farm Income: Net income from farming operations is factored in.
What is Excluded from MAGI?
Crucially, certain types of income are not counted in the MAGI calculation for Medicaid and CHIP. These exclusions are designed to protect income that is not readily available for healthcare expenses or that is already being used for specific purposes. Common exclusions include:
- Gifts and Inheritances: Monetary gifts received and inheritances are generally excluded.
- Disability Payments (Certain Types): Some disability benefits, particularly those from workers’ compensation or veteran’s benefits, may be excluded.
- Child Support Received: Payments received for the support of a child are not counted as income for the custodial parent.
- Foster Care Payments: Payments received for caring for a foster child are typically excluded.
- Scholarships and Grants: Funds received for educational purposes that are used for tuition and fees are generally not counted.
- Lump-Sum Payments (Certain Types): Certain one-time payments, such as insurance settlements for property damage, may be excluded.
- Supplemental Security Income (SSI): SSI benefits are not counted.
- Payments from Home Care Programs: Specific payments made to individuals who provide care for family members under certain home-based care programs may be excluded.
Household Definition for MAGI
A critical aspect of MAGI is the definition of the “household” for income calculation purposes. Unlike tax filings, where household definition can be more complex, for MAGI, the household generally includes:
- The applicant.
- Their spouse.
- Their dependents, as defined for tax purposes.
- Any other individuals claimed as dependents on the applicant’s tax return.
This definition ensures that income is assessed based on the resources available to the immediate family unit that the applicant is responsible for or is financially dependent upon.
How MAGI Impacts Eligibility
The MAGI system has a profound impact on who is eligible for Medicaid and CHIP. Instead of relying on a patchwork of categorical rules, eligibility is now primarily determined by comparing a household’s MAGI to a percentage of the Federal Poverty Level (FPL).
Federal Poverty Level (FPL) and Medicaid Expansion
The FPL is a set of dollar figures established by the U.S. Department of Health and Human Services that indicates the minimum income necessary to meet basic needs. For Medicaid, eligibility is often expressed as a percentage of the FPL.
- Medicaid Expansion: The ACA provided states the option to expand Medicaid eligibility to cover nearly all adults with incomes up to 138% of the FPL. For states that have adopted this expansion, adults who were previously ineligible due to their income or lack of a specific category are now able to access coverage.
- Non-Expansion States: In states that have not expanded Medicaid, eligibility for adults remains more restricted, often limited to specific categories like pregnant women, parents with very low incomes, or individuals who are disabled or elderly.
MAGI vs. Non-MAGI Pathways
It’s important to note that MAGI rules do not apply to all Medicaid eligibility pathways. Certain groups, such as individuals who are elderly, blind, or disabled, and who are applying for benefits through programs like Supplemental Security Income (SSI) or Medicaid’s institutional long-term care programs, continue to be assessed under the older, non-MAGI rules. These rules may still involve asset tests and different income calculations. The MAGI pathway is primarily for individuals and families who are not eligible for these specific disability or age-based programs.
Simplified Application Process
One of the intended benefits of the MAGI system was to simplify the application process. By using a standardized income definition and aligning it with tax filing principles, it was hoped that applicants would find it easier to provide the necessary information. States were required to implement online portals and other streamlined application methods to facilitate this.
The Significance of MAGI for Healthcare Access
The introduction of MAGI has had a significant impact on healthcare access for millions of Americans. By expanding coverage to previously uninsured or underinsured populations, it has contributed to improved health outcomes, reduced financial burdens from medical debt, and a more stable healthcare system.
Increased Insurance Coverage
The expansion of Medicaid under the ACA, facilitated by the MAGI rules, has been a major driver of increased health insurance coverage in the United States. Millions of low-income individuals and families who previously could not afford private insurance or did not qualify for pre-MAGI Medicaid now have access to comprehensive health benefits.
Impact on Child Health
The MAGI rules are also critical for CHIP, which provides low-cost health coverage to children in families who earn too much income to qualify for Medicaid but cannot afford private insurance. The standardized income calculation ensures that families can more easily determine their eligibility for CHIP benefits, leading to greater access to essential pediatric care, vaccinations, and preventative services.
Economic and Public Health Implications
Beyond individual benefits, the widespread adoption of MAGI and Medicaid expansion has broader economic and public health implications. Reduced uninsurance rates can lead to fewer emergency room visits for primary care needs, which are often more expensive. It can also mean that individuals are more likely to seek early diagnosis and treatment for chronic conditions, leading to better long-term health and reduced healthcare costs. Furthermore, a healthier workforce is a more productive workforce, contributing to overall economic stability.
Navigating MAGI and Medicaid Applications
For individuals seeking to understand their eligibility for Medicaid or CHIP, familiarizing themselves with the MAGI rules is an essential first step. The process generally involves gathering documentation related to income and household composition.
Gathering Necessary Documentation
When applying for Medicaid or CHIP under the MAGI rules, applicants will typically need to provide proof of:
- Identity: Government-issued identification (e.g., driver’s license, passport).
- Citizenship or Immigration Status: Proof of legal residency in the U.S.
- Income: Pay stubs, W-2 forms, tax returns (if applicable), unemployment benefit statements, self-employment records, and any other documents showing sources of income.
- Household Composition: Birth certificates for dependents, tax return information showing dependents, or other proof of relationships.
The Application Process
The application process can vary by state but generally involves:
- Completing an Application: This can often be done online through the state’s Medicaid or health insurance marketplace website, by mail, or in person at a local social services office.
- Providing Information: Applicants will need to report their MAGI and household details accurately.
- Verification: State agencies will verify the information provided using various data sources, including federal tax databases.
- Eligibility Determination: Based on the reported and verified information, the state will determine eligibility for Medicaid or CHIP.

Seeking Assistance
Navigating the complexities of eligibility determination can be challenging. Many states offer resources and assistance programs to help individuals with their applications. These may include:
- Trained Navigators: Available through state health insurance marketplaces or community organizations.
- County or State Social Services Offices: Staff at these offices can provide direct assistance.
- Community Health Centers: Often have staff who can help with enrollment.
Understanding MAGI is not just about a number on a tax form; it’s about unlocking access to vital healthcare services. The standardized approach has democratized eligibility, making it more predictable and accessible for a broader segment of the population. As the healthcare landscape continues to evolve, the principles of MAGI remain a cornerstone of equitable access to health coverage for millions.
