The title “What is Frontal Lobotomy” does not directly align with any of the provided categories. However, if forced to select the closest thematic overlap, it would be 6. Tech & Innovation, with the understanding that “innovation” here refers to historical and often controversial advancements in understanding and treating the human mind, rather than current technological development. This category allows for exploration of the “innovation” in neurosurgery and its impact, albeit a dark and ethically fraught one.
The Dawn of the Scalpel: Early Concepts of Brain Manipulation
The history of attempting to alleviate mental distress through physical intervention is long and, frankly, often grim. Before the development of modern psychotropic medications and sophisticated therapeutic approaches, the medical landscape for severe mental illness was barren. Physicians and surgeons, driven by a desire to help and perhaps a limited understanding of the brain’s intricate workings, explored various invasive methods. The concept that the frontal lobes, the seat of personality, decision-making, and complex thought, might be implicated in mental disorders was a significant, albeit misguided, hypothesis.

The Influence of Phineas Gage
A pivotal, albeit accidental, event in shaping early ideas about the frontal lobes was the case of Phineas Gage. In 1848, Gage, a railroad foreman, suffered a traumatic brain injury when an iron rod impaled his skull, passing through his frontal lobe. Miraculously, Gage survived, but his personality and behavior underwent a dramatic shift. He became more impulsive, less considerate, and struggled with executive functions. While not a direct precursor to lobotomy, Gage’s case offered tangible, albeit anecdotal, evidence that damage to the frontal lobes could profoundly alter an individual’s personality and mental state. This observation, though simplified and sensationalized, contributed to the burgeoning, albeit speculative, understanding that the frontal lobes played a critical role in psychological well-being.
Precursors to Lobotomy
Prior to the formal development of frontal lobotomy, various crude surgical interventions were attempted. These included trepanation (drilling holes in the skull), which was practiced for centuries to relieve pressure or, in some cases, believed to release “evil spirits.” While not directly aimed at the frontal lobes, these procedures reflected a willingness to operate on the brain in an attempt to influence mental states. The evolving understanding of anatomy and physiology, however rudimentary, began to focus more attention on specific brain regions, and the frontal lobes, due to their perceived role in higher cognitive functions, became a target of interest for those seeking more targeted interventions for psychiatric conditions.
The Advent of Frontal Lobotomy: A Revolutionary, Yet Tragic, Innovation
The formalization of frontal lobotomy as a surgical procedure is largely attributed to Portuguese neurologist Egas Moniz. His work, conducted in the late 1930s, marked a significant, albeit ethically questionable, “innovation” in the treatment of severe mental illness. Moniz’s radical approach sought to sever the connections between the frontal lobes and the rest of the brain, based on the hypothesis that abnormal neural pathways in these regions were responsible for psychiatric disorders.
Egas Moniz and the Leucotome
Egas Moniz developed a surgical instrument called the leucotome, designed to core out and sever nerve fibers within the white matter of the frontal lobes. His initial procedure, termed “lobotomia frontal interna,” involved injecting alcohol into the frontal white matter to destroy nerve fibers. Later, the leucotome was used to physically remove these tissues. Moniz’s rationale was that by disrupting the thought processes originating in the frontal lobes, he could alleviate symptoms of conditions such as schizophrenia, severe depression, and anxiety. His early results, published in 1936, suggested significant improvements in a subset of his patients, leading to the awarding of the Nobel Prize in Physiology or Medicine in 1949.
Walter Freeman and the “Ice Pick” Lobotomy

In the United States, American psychiatrist Walter Freeman became a prominent advocate and practitioner of lobotomy. Freeman, along with neurosurgeon James Watts, adapted Moniz’s technique. However, Freeman later developed his own, even more controversial, version of the procedure known as the transorbital lobotomy. This method involved inserting a sharpened instrument, often resembling an ice pick, through the eye socket and into the frontal lobe, where it was then manipulated to sever neural connections. The transorbital lobotomy was significantly simpler, faster, and could be performed without the need for a full operating room, making it accessible to a wider range of practitioners and patients. Freeman, driven by a fervent belief in the procedure’s efficacy, conducted thousands of these surgeries, often traveling across the country in his “lobotomobile.”
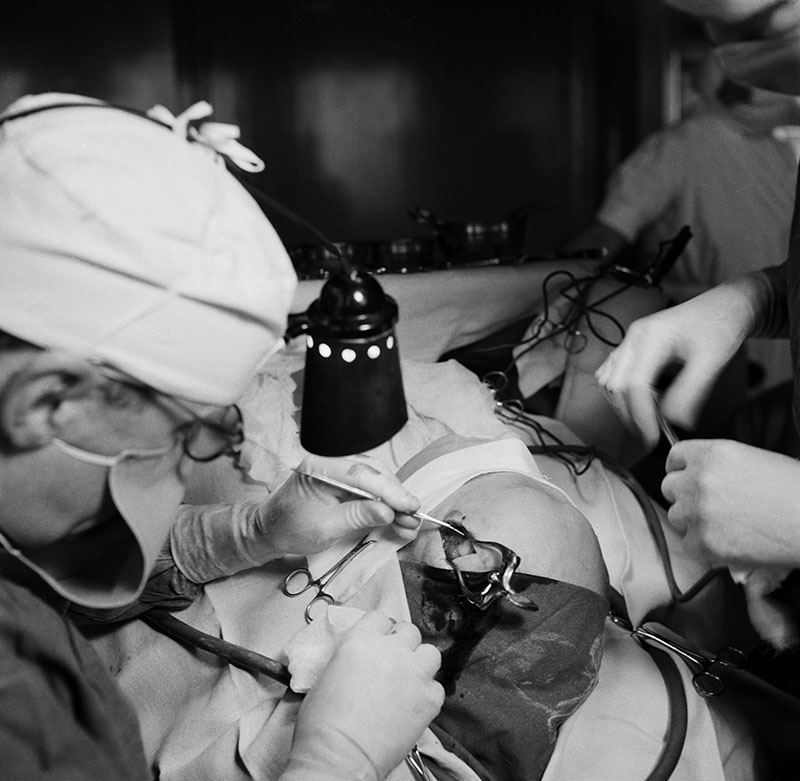
The Procedure and its Devastating Consequences
The physical act of performing a frontal lobotomy, regardless of the specific technique, involved significant destruction of brain tissue. The intended outcome was to dampen emotional reactivity and reduce obsessive or agitated thought patterns. However, the reality of the procedure was far more devastating, leading to profound and irreversible changes in patients.
Surgical Techniques and Mechanisms of Action
The core principle of frontal lobotomy was to sever the connections between the prefrontal cortex and other parts of the brain, particularly the thalamus. The prefrontal cortex is crucial for executive functions, personality, decision-making, and social behavior. By disrupting these neural pathways, surgeons aimed to reduce the intensity of emotions, particularly those associated with anxiety, agitation, and delusion. The leucotome or the transorbital instrument would create lesions within the white matter, effectively disconnecting various brain regions. The “innovation” here lay in the surgical attempt to rewire the brain through physical destruction, a concept starkly different from modern understanding of neurological function.
Post-Operative Outcomes and Ethical Debates
The outcomes of frontal lobotomy were highly variable and often tragic. While some patients might exhibit a reduction in severe behavioral symptoms, this was frequently at the cost of their personality, cognitive abilities, and emotional range. Patients often became apathetic, childlike, and incapable of independent living. They lost their ability to plan, to experience joy or sadness intensely, and to engage in complex social interactions. The procedure also carried significant risks of infection, seizures, and even death.
The ethical implications of frontal lobotomy are profound and continue to be debated. The procedure was often performed on individuals who were difficult to manage, were institutionalized, or whose families could no longer cope. Consent was frequently not fully informed, and in many cases, patients were unable to give consent at all. The widespread use of lobotomy, particularly in the mid-20th century, raises serious questions about the prevailing medical ethics of the time, the societal stigma surrounding mental illness, and the desperate search for cures in the absence of effective treatments. The “innovation” that promised relief ultimately led to widespread iatrogenic harm.
The Decline and Legacy of Frontal Lobotomy
The widespread use of frontal lobotomy eventually declined due to growing awareness of its severe side effects, the development of more effective treatments, and increasing ethical scrutiny. While the procedure itself is largely obsolete, its legacy continues to inform our understanding of the brain and the ethical boundaries of medical intervention.
The Rise of Psychopharmacology and Other Treatments
The advent of antipsychotic medications in the 1950s, such as chlorpromazine, marked a turning point in the treatment of severe mental illness. These drugs offered a way to manage symptoms without the devastating consequences of surgical intervention. Alongside pharmacological advancements, the development of more effective psychotherapies and a greater understanding of the biological and psychological factors contributing to mental health conditions also contributed to the decline of lobotomy. As alternatives emerged, the perceived necessity and justification for such a radical procedure diminished.
Re-evaluation and Ethical Considerations
As medical knowledge advanced and societal values evolved, the practice of frontal lobotomy came under intense scrutiny. Patients who had undergone the procedure often experienced severe and permanent disabilities, leading to a critical re-evaluation of its benefits versus its profound harms. Advocacy groups and medical ethicists began to question the validity of the “innovation” and the ethical framework within which it was practiced. The history of frontal lobotomy serves as a stark reminder of the potential for well-intentioned, yet ultimately destructive, interventions when scientific understanding is incomplete and ethical safeguards are insufficient. It highlights the importance of rigorous scientific inquiry, patient autonomy, and a deep respect for the complexity of the human mind. The “innovation” that was once hailed as a breakthrough is now largely recognized as a cautionary tale in the history of medicine.
