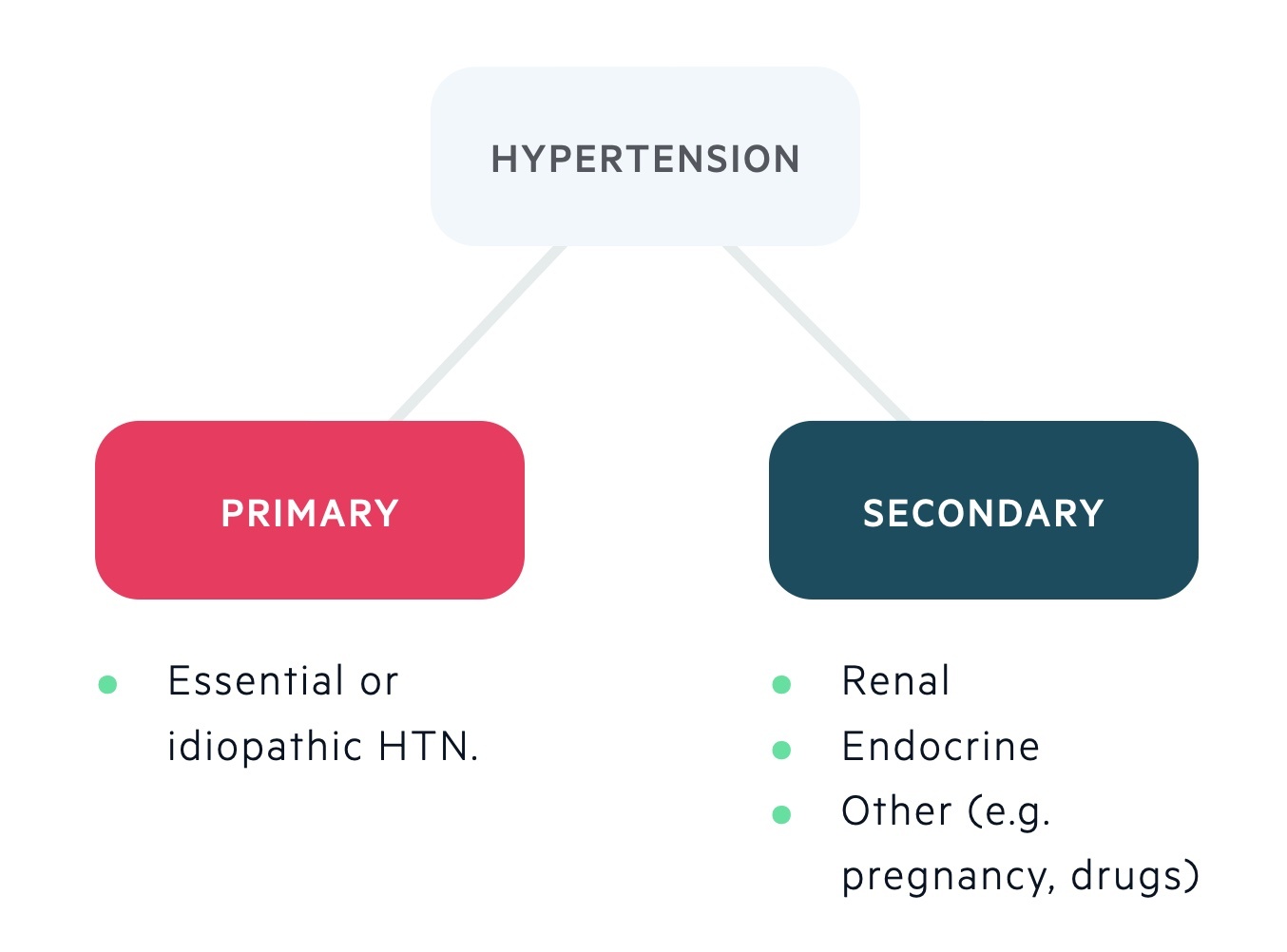
Essential primary hypertension, often simply referred to as primary hypertension or idiopathic hypertension, represents the vast majority of diagnosed hypertension cases – an estimated 90-95%. Unlike secondary hypertension, which arises as a direct consequence of an identifiable underlying medical condition (such as kidney disease, thyroid problems, or certain medications), essential hypertension has no single, clear-cut cause. It develops gradually over many years, and its origins are understood to be a complex interplay of genetic predisposition, environmental factors, and lifestyle choices. This insidious nature makes understanding and managing essential hypertension a critical public health endeavor.

Understanding the Nature of Essential Hypertension
The term “essential” in this context does not imply that the condition is unimportant or trivial. Instead, it signifies that the cause is not readily apparent or attributable to a specific external or secondary factor. This lack of a singular identifiable cause presents a significant diagnostic and therapeutic challenge.
The Silent Threat: Gradual Onset and Asymptomatic Progression
One of the most dangerous aspects of essential hypertension is its often asymptomatic nature, particularly in its early stages. Many individuals live with elevated blood pressure for years, even decades, without experiencing any noticeable symptoms. This “silent killer” characteristic allows the condition to silently inflict damage on vital organs. As blood pressure remains consistently high, it exerts excessive force on the walls of arteries, leading to a cascade of detrimental effects.
- Damage to Arteries: Over time, high blood pressure can cause arteries to thicken, stiffen, and lose their elasticity. This process, known as arteriosclerosis, narrows the blood vessels, further impeding blood flow and increasing the workload on the heart. The inner lining of the arteries can also become damaged, promoting the buildup of plaque (atherosclerosis).
- Impact on the Heart: The heart must pump harder to overcome the resistance in the narrowed arteries. This sustained extra effort can lead to left ventricular hypertrophy, where the heart muscle thickens. Eventually, this can result in heart failure, where the heart can no longer pump blood effectively.
- Strain on Other Organs: The elevated pressure can also damage blood vessels and delicate tissues in other critical organs, including the kidneys, brain, and eyes.
The Multifaceted Etiology: A Complex Web of Influences
While a single cause remains elusive, research has identified several contributing factors that, in combination, significantly increase an individual’s risk of developing essential hypertension.
- Genetic Predisposition: Family history plays a significant role. If close relatives have high blood pressure, an individual is more likely to develop it themselves. This suggests a genetic component, though the specific genes involved are complex and likely numerous. These genetic factors can influence how the body regulates blood pressure, affecting salt and water balance, hormone levels, and blood vessel tone.
- Environmental and Lifestyle Factors: These are the modifiable risk factors that individuals can often influence to mitigate their risk.
- Diet: A diet high in sodium (salt) is a well-established contributor. Sodium causes the body to retain water, increasing blood volume and thus blood pressure. Conversely, a diet rich in potassium, magnesium, and calcium can help lower blood pressure.
- Obesity: Being overweight or obese is a major risk factor. Excess body weight increases the demand on the heart and can lead to changes in hormone levels and kidney function that elevate blood pressure.
- Physical Inactivity: A sedentary lifestyle contributes to weight gain and reduces the cardiovascular benefits of exercise, which helps to keep blood vessels flexible and the heart strong.
- Alcohol Consumption: Excessive alcohol intake can raise blood pressure significantly. Moderate consumption may have some cardiovascular benefits for certain individuals, but heavy drinking is consistently linked to hypertension.
- Smoking: Nicotine in tobacco causes blood vessels to constrict, immediately increasing blood pressure. Over time, smoking damages blood vessel walls, contributing to atherosclerosis and making hypertension more likely.
- Stress: Chronic stress can lead to temporary increases in blood pressure. While the long-term impact of stress on essential hypertension is still being studied, it is believed to contribute through hormonal changes and unhealthy coping mechanisms.
- Age: The risk of developing hypertension increases with age, as arteries naturally tend to become stiffer and less elastic over time.
Diagnosis and Monitoring of Essential Hypertension
Diagnosing essential hypertension relies on consistent measurements of blood pressure over time and the exclusion of secondary causes. The process is straightforward but crucial for initiating timely management.
Accurate Blood Pressure Measurement: The Cornerstone of Diagnosis
Accurate and consistent blood pressure readings are paramount. A single elevated reading is not sufficient for diagnosis. Clinicians typically employ a series of measurements taken under standardized conditions.
- The Measurement Process: Blood pressure is measured using a sphygmomanometer and a cuff placed around the upper arm. The device measures two key pressures:
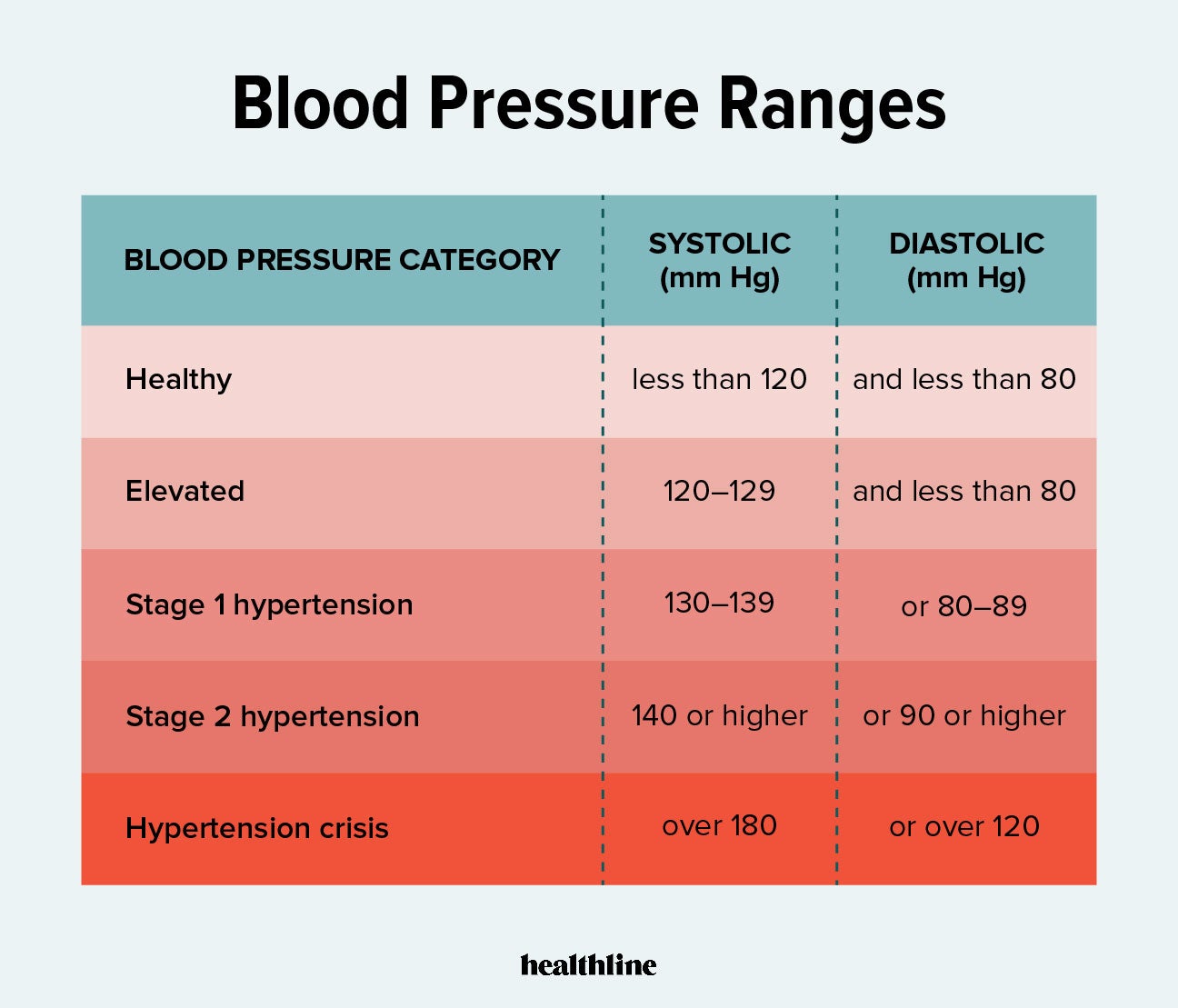
- Systolic Pressure: The pressure in the arteries when the heart beats (contracts). This is the higher number.
- Diastolic Pressure: The pressure in the arteries when the heart rests between beats (relaxes). This is the lower number.
- Blood pressure is recorded as systolic/diastolic (e.g., 120/80 mmHg).
- Diagnostic Thresholds: Current guidelines define hypertension based on consistent blood pressure readings. For example, a diagnosis of hypertension is often made when blood pressure is consistently 130/80 mmHg or higher on multiple occasions.
- Home Blood Pressure Monitoring (HBPM): Encouraging patients to monitor their blood pressure at home can provide a more comprehensive picture of their readings throughout the day and night, reducing the “white-coat hypertension” effect (elevated readings due to anxiety in a clinical setting).
Differential Diagnosis: Ruling Out Secondary Causes
Before confirming a diagnosis of essential hypertension, healthcare professionals will often conduct tests to rule out secondary causes. This is a critical step as treating the underlying condition can resolve the hypertension.
- Medical History and Physical Examination: Detailed questioning about symptoms, family history, medications, and lifestyle factors, coupled with a thorough physical exam, can provide clues to potential secondary causes.
- Laboratory Tests: Blood and urine tests can assess kidney function, electrolyte levels, thyroid hormone levels, and screen for other hormonal imbalances that could contribute to high blood pressure.
- Imaging Studies: In some cases, imaging such as ultrasounds of the kidneys or adrenal glands, or even more specialized tests like angiography, might be used to identify structural abnormalities or blockages.
The Importance of Management and Lifestyle Modifications
While essential hypertension cannot be cured, it is highly manageable. Effective management focuses on lowering blood pressure to reduce the risk of serious complications and involves a combination of lifestyle changes and, when necessary, medication.
Lifestyle Modifications: The First Line of Defense
For many individuals, particularly those with mildly elevated blood pressure or in the pre-hypertension stage, significant improvements can be achieved through sustained lifestyle changes. These modifications not only help manage blood pressure but also contribute to overall cardiovascular health.
- Dietary Adjustments:
- DASH Diet: The Dietary Approaches to Stop Hypertension (DASH) diet is a well-researched eating plan that emphasizes fruits, vegetables, whole grains, lean protein, and low-fat dairy products. It is naturally rich in potassium, magnesium, and calcium.
- Sodium Reduction: Limiting processed foods, fast food, and avoiding adding salt at the table are crucial steps in reducing sodium intake.
- Potassium Rich Foods: Increasing intake of foods like bananas, sweet potatoes, spinach, and beans can help counter the effects of sodium.
- Regular Physical Activity: Aiming for at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity activity per week, along with muscle-strengthening exercises, can significantly lower blood pressure.
- Weight Management: Achieving and maintaining a healthy weight through diet and exercise can have a profound impact on blood pressure. Even a modest weight loss of 5-10% can be beneficial.
- Moderating Alcohol Intake: Limiting alcohol consumption to no more than one drink per day for women and two drinks per day for men is recommended.
- Smoking Cessation: Quitting smoking is one of the most impactful steps an individual can take for their cardiovascular health. Resources and support are available to aid in this process.
- Stress Management Techniques: Practicing relaxation techniques such as deep breathing exercises, meditation, yoga, or engaging in enjoyable hobbies can help manage stress levels. Adequate sleep is also vital.
Pharmacological Interventions: When Lifestyle Isn’t Enough
When lifestyle modifications alone are insufficient to achieve target blood pressure levels, or for individuals with significantly elevated blood pressure at diagnosis, medication becomes a necessary component of management. A variety of classes of antihypertensive medications are available, and the choice of drug or combination of drugs is individualized based on the patient’s overall health, other medical conditions, and blood pressure readings.
- Diuretics: These medications help the kidneys remove excess sodium and water from the body, reducing blood volume.
- Beta-Blockers: They block the effects of adrenaline, slowing the heart rate and reducing the force of heart contractions.
- ACE Inhibitors (Angiotensin-Converting Enzyme Inhibitors): These drugs prevent the production of a hormone that narrows blood vessels.
- ARBs (Angiotensin II Receptor Blockers): Similar to ACE inhibitors, they block the action of a hormone that narrows blood vessels.
- Calcium Channel Blockers: They relax blood vessels by preventing calcium from entering muscle cells in the artery walls.
- Alpha-Blockers: They relax certain muscles and help small blood vessels remain open.
The management of essential hypertension is a lifelong commitment. Regular follow-up with healthcare providers is crucial to monitor blood pressure, assess the effectiveness of treatment, and adjust medications as needed. By understanding the nature of essential hypertension and actively participating in its management through lifestyle changes and medical care, individuals can significantly reduce their risk of debilitating cardiovascular events and lead healthier, longer lives.
