The healthcare landscape is undergoing a profound transformation, driven by technological advancements that promise to enhance patient care, streamline operations, and empower medical professionals. Among the emerging technologies poised to revolutionize this sector, Computerized Decision Support (CDS) systems stand out as a critical innovation. CDS encompasses a broad spectrum of software applications designed to assist healthcare providers in making better clinical decisions. These systems leverage artificial intelligence, machine learning, and extensive data analysis to offer timely, relevant, and actionable information at the point of care.
The core objective of CDS is to augment human expertise, not replace it. By integrating with electronic health records (EHRs) and other clinical data sources, CDS platforms can analyze patient information – including medical history, laboratory results, medications, and genetic data – to identify potential risks, suggest diagnoses, recommend treatments, and monitor patient progress. This proactive approach aims to prevent medical errors, improve the quality of care, and ultimately lead to better patient outcomes. The complexity of modern medicine, with its ever-expanding body of knowledge and the sheer volume of patient data, makes it increasingly challenging for individual clinicians to stay abreast of all relevant information. CDS systems serve as intelligent assistants, sifting through this complexity to highlight crucial insights that might otherwise be overlooked.
The adoption of CDS is not merely about technological sophistication; it’s about fostering a culture of evidence-based practice and continuous improvement. As healthcare systems grapple with rising costs, increasing demand, and the persistent challenge of medical errors, CDS offers a tangible pathway toward greater efficiency, safety, and effectiveness. The potential benefits extend across various healthcare settings, from large hospital networks and specialized clinics to primary care practices and even remote patient monitoring initiatives.
The Foundation of Computerized Decision Support
At its heart, Computerized Decision Support is built upon a sophisticated interplay of data, algorithms, and user-friendly interfaces. The efficacy of any CDS system is directly proportional to the quality and comprehensiveness of the data it can access and process.
Data Integration and Sources
The lifeblood of a CDS system is its ability to ingest and interpret data from a multitude of sources. This typically begins with integration into existing Electronic Health Records (EHRs). EHRs provide a longitudinal record of a patient’s health, including demographics, allergies, medications, immunizations, laboratory test results, radiology reports, problem lists, and progress notes. Seamless integration allows CDS to access the most up-to-date patient-specific information.
Beyond EHRs, CDS systems can draw from other critical data streams:
- Laboratory Information Systems (LIS): Providing detailed results from diagnostic tests.
- Radiology Information Systems (RIS) and Picture Archiving and Communication Systems (PACS): Enabling analysis of imaging reports and potentially even the images themselves.
- Pharmacy Systems: Offering insights into current and past medication regimens, dosages, and refill histories.
- Genomic Data: Increasingly, genetic information is being integrated to inform personalized medicine recommendations.
- Wearable Devices and Remote Monitoring Tools: Data from consumer wearables and medical-grade remote monitoring devices can provide real-time physiological data, such as heart rate, blood pressure, and glucose levels.
- Public Health Databases and Registries: Access to population-level data can help identify disease trends and risks within specific patient groups.
- Medical Literature and Clinical Guidelines: CDS systems are often programmed with up-to-date clinical guidelines, evidence-based research, and drug databases.
The process of data integration is complex, often requiring robust interoperability standards like HL7 (Health Level Seven) and FHIR (Fast Healthcare Interoperability Resources) to ensure that data can be exchanged and understood between different systems. Data cleansing, standardization, and validation are crucial steps to ensure that the information fed into the CDS engine is accurate and reliable.
Algorithmic Intelligence and Knowledge Representation
The “decision support” aspect of CDS is powered by sophisticated algorithms and logic engines. These systems employ various techniques to derive insights and make recommendations:
- Rule-Based Systems: These are the most traditional form of CDS. They use a set of predefined “if-then” rules, often based on established clinical guidelines and expert knowledge. For example, “IF a patient has a penicillin allergy AND is prescribed amoxicillin, THEN generate an alert for a potential allergic reaction.”
- Machine Learning (ML) and Artificial Intelligence (AI): More advanced CDS systems leverage ML algorithms to learn from vast datasets. These systems can identify subtle patterns, predict patient trajectories, and even discover new relationships between variables that might not be immediately obvious to human clinicians. Examples include predictive models for sepsis, hospital readmission risk, or the likelihood of developing a chronic condition.
- Natural Language Processing (NLP): NLP allows CDS systems to understand and interpret unstructured text data found in clinical notes, such as physician narratives, discharge summaries, and pathology reports. This enables the extraction of critical information that might not be captured in structured fields.
- Knowledge Graphs and Ontologies: These structured representations of medical concepts and their relationships help the CDS system understand the context and meaning of clinical information, leading to more nuanced and accurate recommendations.
The knowledge base that underpins these algorithms is constantly evolving, requiring regular updates to reflect the latest medical research and practice. This ensures that the CDS system remains current and relevant.
Applications of CDS in Modern Healthcare
The versatility of Computerized Decision Support systems allows them to be applied across a wide array of clinical scenarios, impacting nearly every facet of patient care. These applications are designed to proactively address potential issues, optimize treatments, and ensure adherence to best practices.
Preventing Medical Errors and Enhancing Patient Safety
One of the most critical contributions of CDS is its role in enhancing patient safety by actively preventing medical errors. These systems act as a vigilant safety net, identifying and flagging potential risks before they can lead to adverse events.
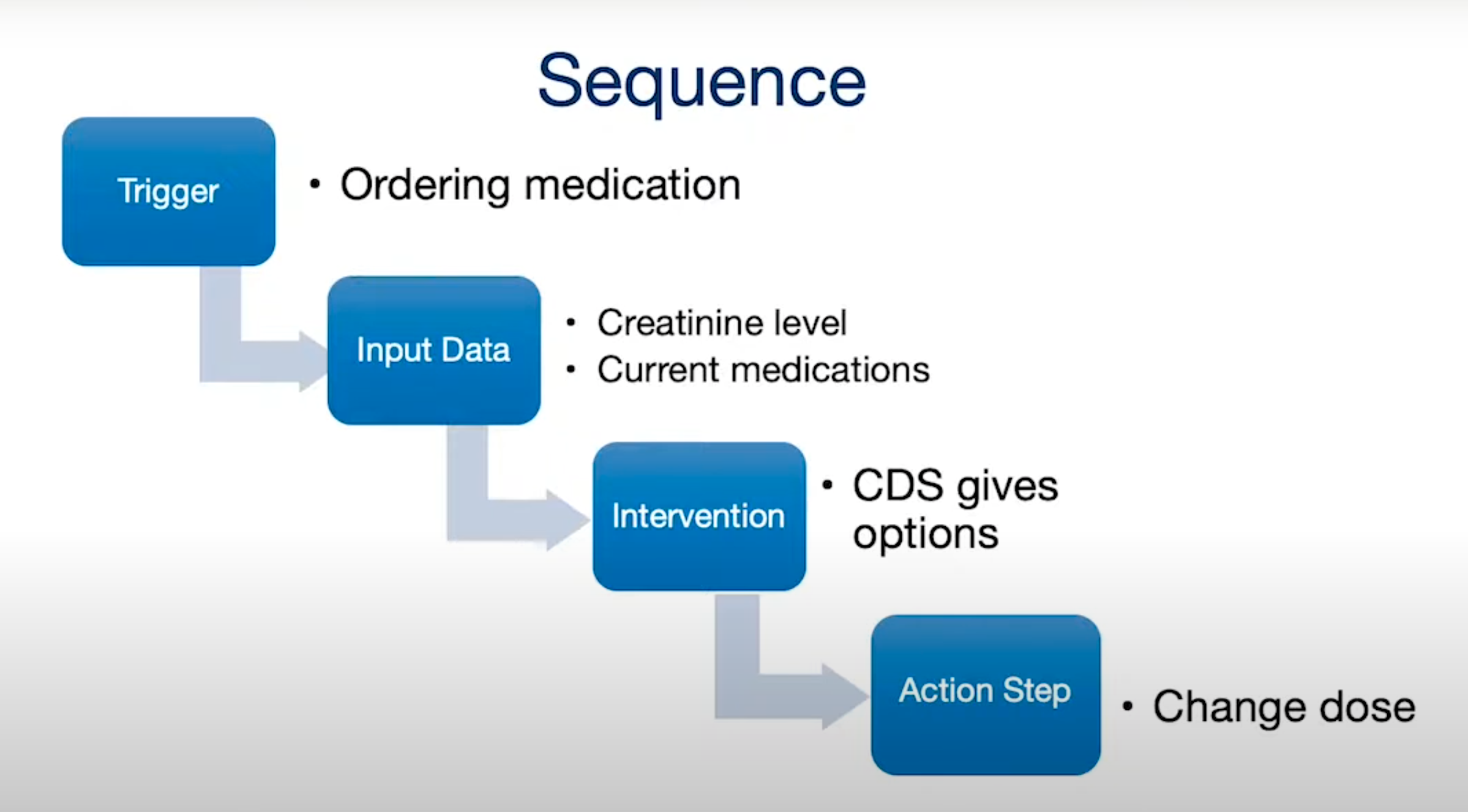
- Drug Safety Alerts: Perhaps the most widely implemented form of CDS, these alerts flag potential drug-drug interactions, drug-allergy interactions, inappropriate dosages (based on age, weight, or renal function), and contraindications. For instance, if a clinician attempts to prescribe a medication that is known to interact dangerously with a patient’s current medication, the CDS will issue an immediate alert.
- Allergy Warnings: Similar to drug interactions, CDS systems ensure that medications to which a patient has a known allergy are not prescribed.
- Preventing Diagnostic Errors: By analyzing patient symptoms, lab results, and historical data, CDS can suggest potential diagnoses that a clinician might not have considered, especially in complex or atypical presentations. It can also flag tests that are indicated but have not yet been ordered.
- Guideline Adherence: CDS can ensure that diagnostic and treatment pathways align with established clinical guidelines, reducing variability in care and promoting evidence-based practices. For example, for a patient presenting with symptoms suggestive of a specific condition, the CDS might prompt for a particular diagnostic test or a follow-up consultation based on the recommended pathway.
Optimizing Treatment and Workflow Efficiency
Beyond safety, CDS significantly contributes to optimizing treatment plans and streamlining clinical workflows, leading to more efficient and effective care delivery.
- Personalized Treatment Recommendations: By analyzing a patient’s unique genetic makeup, medical history, and lifestyle factors, advanced CDS systems can suggest personalized treatment plans, including optimal drug choices, dosages, and therapeutic approaches. This is particularly relevant in fields like oncology and pharmacogenomics.
- Order Entry and Management: CDS integrated with order entry systems can guide clinicians in selecting appropriate tests, procedures, and medications, ensuring that orders are complete and medically justified. This can reduce unnecessary testing and improve resource utilization.
- Clinical Pathway Guidance: For common conditions or procedures, CDS can guide clinicians through standardized clinical pathways, ensuring that all necessary steps are taken in the correct sequence and at the appropriate time. This can improve consistency of care and reduce variations in treatment.
- Documentation Assistance: Some CDS tools can assist with clinical documentation by suggesting relevant diagnostic codes, completing forms, or summarizing key patient information, thereby reducing the administrative burden on clinicians.
- Alert Fatigue Management: A critical challenge in CDS is “alert fatigue,” where clinicians are bombarded with too many alerts, leading them to ignore or dismiss them. Advanced CDS systems employ sophisticated algorithms to prioritize alerts based on their urgency and relevance, reducing unnecessary interruptions and improving the signal-to-noise ratio.
Monitoring and Predictive Analytics
The ability of CDS to continuously monitor patient data and identify trends opens up powerful avenues for predictive analytics, enabling proactive interventions and better resource allocation.
- Early Sepsis Detection: CDS systems can monitor vital signs, laboratory results, and other clinical data for subtle indicators of sepsis, a life-threatening condition. Early detection through CDS can trigger rapid intervention protocols, significantly improving patient survival rates.
- Predicting Readmission Risk: By analyzing factors such as the patient’s diagnosis, previous admissions, social determinants of health, and medication adherence, CDS can identify patients at high risk of hospital readmission. This allows healthcare providers to implement targeted interventions, such as enhanced discharge planning or post-discharge follow-up, to prevent unnecessary readmissions.
- Chronic Disease Management: CDS can play a crucial role in managing chronic conditions like diabetes, heart failure, and hypertension. By monitoring patient data from EHRs and remote devices, these systems can identify deviations from expected trends, alert clinicians to potential complications, and suggest adjustments to treatment plans.
- Population Health Management: On a larger scale, CDS can aggregate and analyze data from entire patient populations to identify trends, predict disease outbreaks, and allocate public health resources more effectively.
Challenges and the Future of CDS
Despite its immense potential, the widespread and effective implementation of Computerized Decision Support systems faces several challenges. Addressing these hurdles is crucial for unlocking the full transformative power of CDS in healthcare.
Implementation and Adoption Hurdles
The successful integration of CDS into clinical workflows is not without its difficulties. Several factors can impede smooth adoption.
- Interoperability and Data Silos: As mentioned earlier, achieving seamless data exchange between disparate healthcare IT systems remains a significant challenge. Data often resides in “silos,” making it difficult for CDS to access a comprehensive patient view. Lack of standardized data formats and communication protocols further exacerbates this issue.
- Workflow Integration: CDS tools must be designed to fit naturally into existing clinical workflows without causing undue disruption. If a CDS system requires significant changes to how clinicians work, adoption rates will likely suffer. The user interface must be intuitive and provide information at the right time and in the right format.
- Physician Resistance and Trust: Some clinicians may be hesitant to adopt CDS, fearing it will undermine their autonomy or expertise. Building trust in the accuracy and reliability of CDS recommendations is paramount. This requires transparent algorithm design, rigorous validation, and evidence of improved patient outcomes.
- Cost and Resource Allocation: Implementing and maintaining robust CDS systems can be expensive, requiring significant investment in software, hardware, IT support, and training. Healthcare organizations must carefully weigh the costs against the potential benefits.
- Data Quality and Completeness: The adage “garbage in, garbage out” is particularly relevant for CDS. If the underlying data is inaccurate, incomplete, or outdated, the CDS recommendations will be flawed, potentially leading to incorrect decisions and eroded trust.
Addressing Alert Fatigue and Maintaining Relevance
The issue of alert fatigue is a prominent concern that needs continuous attention.
- Sophisticated Alert Prioritization: Future CDS systems will likely employ more advanced AI and ML techniques to intelligently filter and prioritize alerts, ensuring that only the most critical and actionable information is presented to the clinician at the right moment. This might involve contextual awareness, understanding the patient’s current status and the clinician’s focus.
- Personalized Alert Thresholds: Allowing clinicians to customize alert thresholds for certain conditions or patient populations can help reduce unnecessary notifications while still maintaining vigilance for critical events.
- Feedback Mechanisms: Implementing robust feedback mechanisms where clinicians can easily provide input on the usefulness and accuracy of alerts is vital. This feedback can be used to retrain algorithms and improve the system’s performance over time.

The Future Trajectory of CDS
The evolution of CDS is inextricably linked to advancements in AI, machine learning, and data analytics.
- Proactive and Predictive Care: The trend is moving from reactive alerts to proactive and predictive insights. CDS will increasingly anticipate potential health issues before they manifest, enabling preventive interventions.
- Enhanced Personalization and Precision Medicine: As genomic and other “omic” data become more integrated, CDS will play an even more significant role in delivering truly personalized and precision medicine, tailoring treatments to an individual’s unique biological profile.
- Ambient Clinical Intelligence: Emerging technologies like ambient clinical intelligence, which uses voice and AI to automatically document patient encounters, will likely integrate with CDS to provide real-time decision support seamlessly within the patient interaction.
- Patient-Facing CDS: We may see a rise in patient-facing CDS tools that empower individuals to better understand their health conditions, treatment options, and adherence requirements, fostering greater patient engagement in their own care.
- Continuous Learning and Adaptation: Future CDS systems will be designed for continuous learning, adapting to new medical knowledge, evolving clinical practices, and the unique characteristics of the patient populations they serve.
In conclusion, Computerized Decision Support systems are no longer a futuristic concept but a present-day reality that is reshaping healthcare. By harnessing the power of data and intelligent algorithms, CDS offers a powerful means to enhance patient safety, optimize clinical decision-making, improve workflow efficiency, and drive better health outcomes. As these technologies mature and overcome current challenges, their role in delivering high-quality, efficient, and personalized healthcare will only continue to grow.
