Baastrup’s disease, also known as “kissing spines,” is a degenerative condition affecting the lumbar spine. It’s characterized by the spinous processes of adjacent vertebrae elongating and coming into contact with each other. This physical impingement can lead to inflammation, pain, and a range of musculoskeletal issues that can impact an individual’s mobility and quality of life. While the title itself doesn’t directly align with the provided categories, understanding conditions that affect human anatomy and movement is crucial for the development and application of various technologies, particularly those involving human-computer interaction, biomechanics, and assistive devices. For the purpose of this article, we will explore Baastrup’s disease through the lens of Tech & Innovation, focusing on how technology can be utilized in its diagnosis, management, and the potential for future innovative solutions.

Understanding the Biomechanics of Baastrup’s Disease
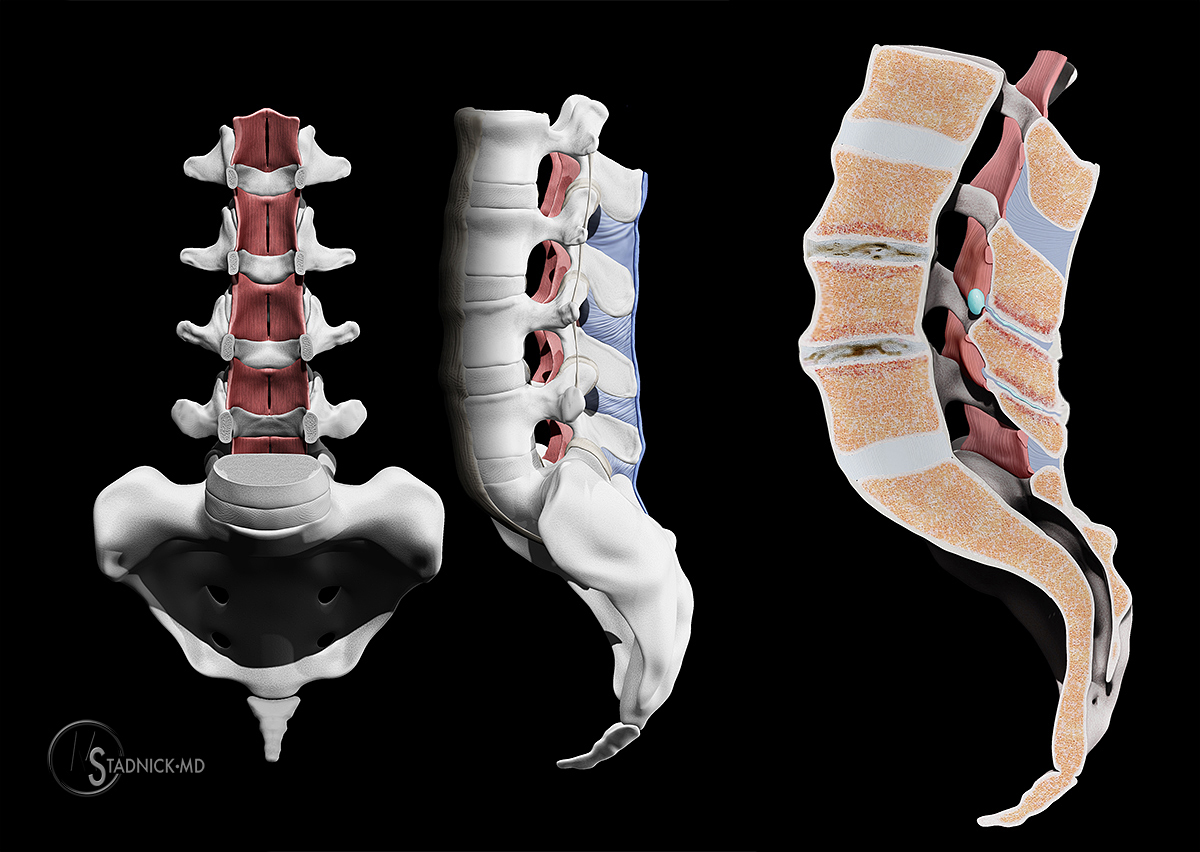
At its core, Baastrup’s disease is a biomechanical problem within the spinal column. The spine is a marvel of biological engineering, designed for both strength and flexibility. It’s composed of a series of vertebrae stacked upon one another, with intervertebral discs acting as shock absorbers and allowing for movement. Each vertebra has bony projections, including the spinous processes that extend posteriorly. In a healthy spine, these spinous processes are separated by ligaments and musculature, allowing for smooth articulation between vertebrae.
In Baastrup’s disease, a key pathological process is the abnormal elongation of these spinous processes. The exact cause of this elongation is not fully understood, but several factors are believed to contribute:
Contributing Factors and Pathological Changes
- Age-Related Degeneration: As we age, the intervertebral discs lose hydration and height, leading to a phenomenon known as disc degeneration. This can cause the vertebrae to move closer together. In response to this increased proximity and altered biomechanical forces, the spinous processes may begin to elongate as a compensatory mechanism. This is a form of adaptation, albeit one that can lead to problems.
- Poor Posture and Biomechanical Strain: Chronic poor posture, particularly excessive lumbar lordosis (the inward curve of the lower back), can place increased stress on the posterior elements of the spine, including the spinous processes. Over time, this repetitive strain can contribute to their abnormal growth and eventual contact.
- Osteoarthritis: The degenerative changes associated with osteoarthritis, which affects the joints of the body, can also impact the facet joints and surrounding bone structures of the spine. This can lead to bony spurs and changes in the shape of the spinous processes.
- Genetic Predisposition: While not definitively proven, there may be a genetic component that makes some individuals more susceptible to developing Baastrup’s disease.
When the spinous processes elongate and make contact, a cascade of inflammatory and degenerative changes can occur. This direct contact can lead to:
- Bursitis: Inflammation of the bursa, a small fluid-filled sac that reduces friction between bones and tendons. In Baastrup’s disease, a bursa can develop between the contacting spinous processes and become inflamed.
- Ligamentous Hypertrophy: The supraspinous and interspinous ligaments, which normally span between the spinous processes, can thicken and ossify in response to the chronic irritation, further exacerbating the problem.
- Facet Joint Arthropathy: The increased loading and altered biomechanics can also lead to degeneration of the facet joints, which are located on the posterior aspect of the vertebrae and allow for spinal extension and rotation.
Technological Innovations in Diagnosis and Assessment
The diagnosis of Baastrup’s disease relies heavily on imaging techniques that can visualize the bony structures of the spine. Modern diagnostic technologies have significantly improved the accuracy and early detection of this condition.
Advanced Imaging Modalities
- X-ray: Standard X-rays of the lumbar spine are often the first line of diagnostic imaging. They can reveal the elongated spinous processes, the degree of contact, and any associated degenerative changes in the vertebrae and discs. Lateral views are particularly useful for assessing the alignment and spacing of the spinous processes.
- MRI (Magnetic Resonance Imaging): MRI provides more detailed information about the soft tissues surrounding the spine, including the ligaments, muscles, and intervertebral discs. It can help identify inflammation in the bursa, thickening of the ligaments, and the extent of facet joint degeneration. MRI is also crucial for ruling out other conditions that may cause similar symptoms, such as spinal stenosis or disc herniation.
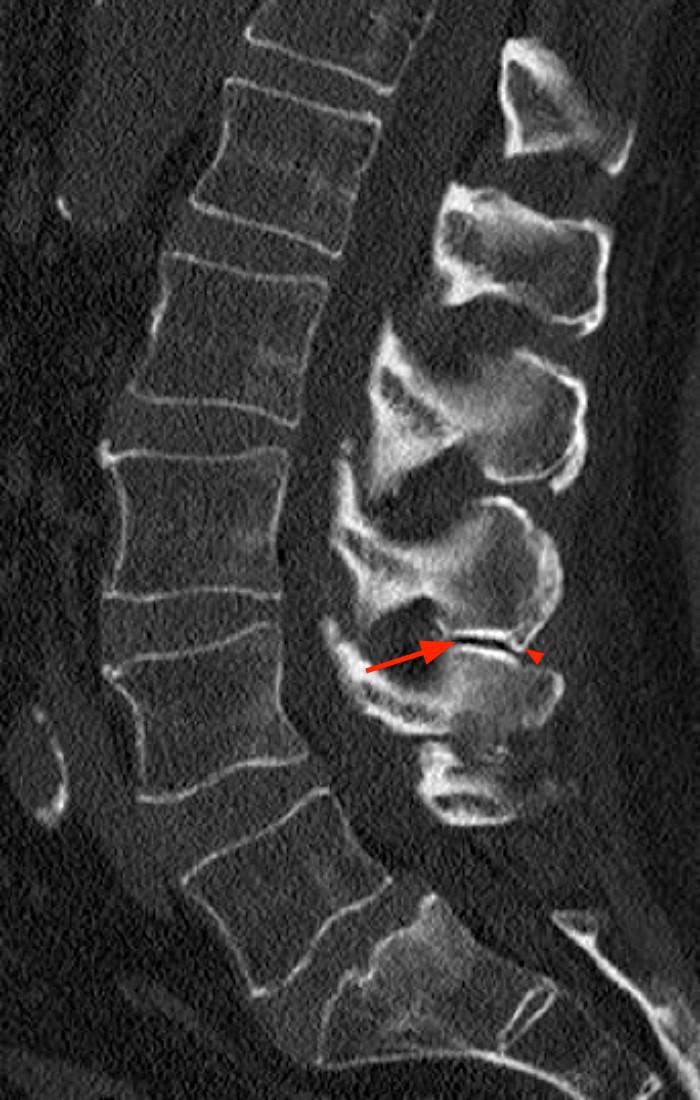
- CT (Computed Tomography) Scan: CT scans offer excellent visualization of bony structures and can provide highly detailed cross-sectional images of the spinous processes and their relationship to each other. This can be particularly useful for surgical planning if intervention is considered.
Biomechanical Assessment Technologies
Beyond static imaging, innovative technologies are emerging to assess the dynamic biomechanics of the spine and how conditions like Baastrup’s disease affect movement.
- Motion Capture Systems: Sophisticated motion capture systems, commonly used in sports science and animation, can be adapted to analyze gait and posture in individuals with spinal conditions. By tracking the movement of specific body markers, clinicians can identify abnormal compensatory movements and assess the impact of Baastrup’s disease on overall mobility and functional capacity. This data can inform personalized rehabilitation programs.
- Pressure Mapping Systems: While typically used for analyzing foot pressure, pressure mapping technology could theoretically be applied to understand weight distribution and pressure points along the spine during various activities. This could offer insights into how Baastrup’s disease alters spinal loading.
- Wearable Sensors: The development of advanced wearable sensors, such as inertial measurement units (IMUs), can provide continuous, real-world data on spinal posture and movement patterns. These sensors can detect prolonged periods of poor posture, excessive spinal loading, or abnormal ranges of motion that might exacerbate Baastrup’s disease. This objective data can be invaluable for patient monitoring and adherence to therapeutic recommendations.
Innovative Management and Treatment Strategies
While traditionally managed with conservative treatments, technological advancements are paving the way for more targeted and personalized interventions for Baastrup’s disease.
Minimally Invasive Interventions
- Image-Guided Injections: Ultrasound and fluoroscopy (real-time X-ray imaging) are routinely used to guide injections of corticosteroids and local anesthetics into the affected areas. These injections can effectively reduce inflammation and pain in the bursa or facet joints associated with Baastrup’s disease. Robotic-assisted navigation systems are further enhancing the precision of these procedures.
- Radiofrequency Ablation (RFA): For persistent pain originating from the facet joints or nerves irritated by the impingement, RFA can be an effective treatment. This technique uses heat generated by radiofrequency current to disrupt the nerve signals transmitting pain. Image guidance is essential for accurate targeting of the affected nerves.
Rehabilitation and Physical Therapy Technologies
- Virtual Reality (VR) and Augmented Reality (AR) for Rehabilitation: VR and AR technologies are transforming physical therapy. For patients with Baastrup’s disease, VR environments can provide engaging and motivating exercises designed to improve posture, core strength, and spinal mobility in a controlled setting. AR can overlay visual cues and guidance onto the real world, helping patients perform exercises with correct form.
- Robotics in Physical Therapy: Robotic exoskeletons and therapeutic robots are being developed to assist with movement and provide resistance training. These devices can offer precise and consistent support, allowing individuals with Baastrup’s disease to regain strength and improve their functional abilities safely.
- Tele-Rehabilitation Platforms: The rise of digital health platforms allows for remote monitoring and delivery of physical therapy programs. Patients can connect with their therapists via video conferencing, receive personalized exercise plans through apps, and have their progress tracked through wearable sensors, making rehabilitation more accessible and convenient.
Future Innovations: AI, Robotics, and Beyond
The integration of artificial intelligence (AI) and advanced robotics holds significant promise for the future management and understanding of Baastrup’s disease.
AI in Diagnosis and Prognosis
- AI-Powered Image Analysis: Machine learning algorithms are being trained to analyze spinal imaging with remarkable accuracy. AI can identify subtle signs of Baastrup’s disease that might be missed by the human eye, leading to earlier diagnosis. Furthermore, AI can analyze vast datasets of patient information to predict the progression of the disease and the likelihood of successful treatment outcomes.
- Predictive Modeling for Personalized Treatment: AI can analyze a patient’s unique biomechanical data, imaging results, and clinical history to create personalized treatment plans. This includes predicting which interventions are most likely to be effective and identifying individuals who might benefit from surgical consultation.
Robotics and Surgical Advancements
- Robotic-Assisted Spinal Surgery: For cases where conservative management fails and surgical intervention is necessary, robotic surgical systems offer enhanced precision and control. These systems can assist surgeons in performing complex procedures with smaller incisions, leading to reduced recovery times and improved outcomes. This could be particularly relevant for procedures aimed at decompressing the spinous processes or correcting spinal alignment.
- Exoskeletons for Mobility Assistance: Advanced exoskeletons, integrated with AI for adaptive movement, could provide significant mobility support for individuals severely impacted by chronic spinal pain. These devices could help maintain independence and improve quality of life by enabling movement that would otherwise be difficult or impossible.
Smart Devices and Continuous Monitoring
The development of “smart” implants or devices that can continuously monitor spinal alignment, pressure, and inflammatory markers could revolutionize the management of chronic spinal conditions. While currently in early stages of research for spinal applications, such technology could provide real-time feedback to patients and clinicians, allowing for proactive adjustments to treatment and lifestyle to prevent exacerbations of Baastrup’s disease.
In conclusion, while Baastrup’s disease is a physical ailment, the application of technology is profoundly impacting how we understand, diagnose, and treat it. From advanced imaging and biomechanical analysis to AI-driven insights and robotic interventions, the field of Tech & Innovation is at the forefront of developing solutions that promise to alleviate the burden of this challenging spinal condition and improve the lives of those affected.
