The appearance of a wheal on the skin can be a perplexing and sometimes alarming experience. These raised, itchy welts are a common dermatological manifestation, often associated with a variety of underlying causes. Understanding what constitutes a wheal, its typical characteristics, and the potential triggers is crucial for effective management and reassurance. While the term “wheal” might sound medical, it describes a relatively straightforward physiological response that can arise from both minor irritations and more significant allergic reactions. This exploration delves into the nature of wheals, differentiating them from other skin lesions and examining the diverse array of circumstances that can lead to their formation.

Defining the Wheal: Characteristics and Distinctions
At its core, a wheal is a transient, raised, erythematous (red) and often edematous (swollen) lesion of the skin. This characteristic morphology is a direct result of localized swelling in the dermis, the layer of skin beneath the epidermis. The swelling is caused by the rapid accumulation of fluid, a process known as edema. This fluid leakage is typically triggered by the release of histamine and other inflammatory mediators from mast cells, which are immune cells abundant in the skin.
The appearance of a wheal is often described as a hive, a papule, or a plaque, depending on its size and whether it is a single lesion or part of a larger cluster. Wheals are typically well-demarcated, meaning they have distinct borders. Their color can range from pale pink to bright red, often depending on the individual’s skin tone and the severity of the inflammation. The surface of a wheal is usually smooth, although it can sometimes appear slightly bumpy.
A key feature of wheals is their transient nature. They typically appear suddenly and can last for a few minutes to several hours, but rarely persist for more than 24 hours in a single location. As the inflammatory response subsides, the fluid is reabsorbed, and the wheal flattens and disappears, often without leaving any residual marks or scars. This rapid waxing and waning is a hallmark of wheals and helps to distinguish them from other skin conditions like insect bites or eczema, which may persist for longer periods.
Differentiating Wheals from Other Skin Lesions
It is important to distinguish wheals from other common skin lesions that might superficially resemble them.
Insect Bites
Insect bites, such as those from mosquitoes, fleas, or spiders, can also cause localized redness, swelling, and itching. However, insect bites are typically initiated by the injection of venom or saliva by the insect, which contains specific irritants. While some insect bites can trigger a wheal-like reaction, the underlying mechanism is more focused on the insect’s biological material. Moreover, insect bites may sometimes have a central punctum (a small hole where the insect’s mouthparts penetrated the skin), which is generally absent in a pure wheal. The duration of insect bites can also vary, with some persisting for days.
Urticaria (Hives)
Urticaria is the medical term for a condition characterized by the widespread development of wheals. When wheals occur in multiple locations across the body, often in crops that appear and disappear in different areas, it is diagnosed as urticaria. Thus, a wheal is a singular manifestation, while urticaria is a clinical presentation of multiple wheals.
Angioedema
Angioedema is a deeper form of swelling that affects the dermis and subcutaneous tissues, often occurring alongside urticaria. While angioedema involves fluid accumulation, it typically affects areas with looser connective tissue, such as the lips, eyelids, tongue, and genitals. Unlike wheals, angioedema is usually not itchy but can cause significant discomfort and a burning sensation.
Dermatitis
Dermatitis, or eczema, is a more general term for skin inflammation. While some forms of dermatitis can involve redness, itching, and even blistering, the lesions are usually more persistent and may present with scaling, oozing, and crusting, which are not typical features of a wheal.
Causes of Wheal Formation: Triggers and Mechanisms
The formation of a wheal is a complex interplay between the skin’s immune system and external or internal stimuli. The release of histamine from mast cells is the central event, leading to vasodilation (widening of blood vessels) and increased vascular permeability, allowing fluid to leak into the surrounding tissues.
Allergic Reactions
Allergic reactions are one of the most common culprits behind wheal formation. In individuals with a heightened sensitivity to certain substances, exposure can trigger a cascade of immune responses.
Food Allergies
Ingestion of allergenic foods, such as peanuts, shellfish, milk, eggs, or certain fruits, can lead to systemic allergic reactions that manifest as urticaria (multiple wheals) and sometimes angioedema. The immune system mistakenly identifies these food proteins as harmful invaders and mounts an exaggerated response.
Drug Allergies
Many medications can elicit allergic reactions, leading to wheals. Common offenders include antibiotics (like penicillin), nonsteroidal anti-inflammatory drugs (NSAIDs), and contrast dyes used in medical imaging. The reaction can occur minutes to hours after taking the drug.
Insect Stings and Bites
As mentioned earlier, venom from stinging insects like bees, wasps, and hornets, or the saliva from biting insects like mosquitoes and ants, can trigger localized or widespread wheal reactions. Some individuals may have a more severe systemic allergic reaction to insect stings, known as anaphylaxis, which can be life-threatening.
Environmental Allergens
Exposure to airborne allergens such as pollen, mold spores, or dust mites can also cause wheals, particularly in individuals with allergic rhinitis or asthma. Contact with certain plants, like poison ivy or nettles, can cause localized wheal-like reactions and blistering due to direct skin irritation and allergic sensitization.
Non-Allergic Triggers
While allergies are a primary cause, wheals can also arise from non-allergic mechanisms, often related to direct irritation or physical stimuli.
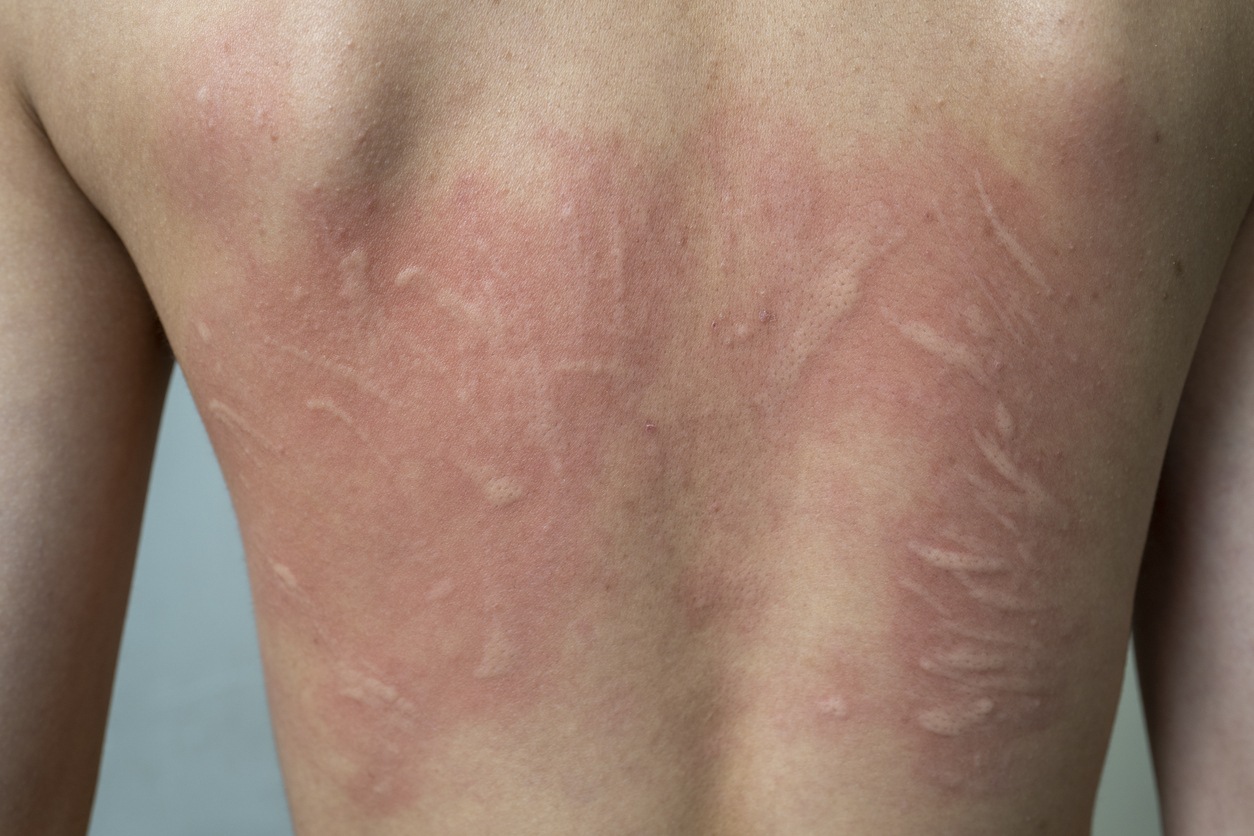
Physical Urticarias
These are a group of conditions where wheals are induced by physical agents.
- Dermatographism (Skin Writing): This is the most common form of physical urticaria. When the skin is scratched or rubbed, it develops raised, red lines that resemble writing. This is due to an exaggerated response of mast cells to mechanical pressure or friction.
- Pressure Urticaria: Prolonged or sustained pressure on the skin, such as from tight clothing, prolonged sitting, or carrying heavy objects, can lead to the development of wheals in the affected areas.
- Cold Urticaria: Exposure to cold temperatures, whether from cold air, water, or objects, can trigger wheals in susceptible individuals. The reaction typically occurs as the skin rewarms after exposure.
- Heat Urticaria: Less common than cold urticaria, this involves the development of wheals upon exposure to heat.
- Solar Urticaria: This rare condition causes wheals to appear within minutes of exposure to sunlight.
- Vibratory Urticaria: Exposure to vibration, such as from power tools or certain machinery, can induce wheals.
- Cholinergic Urticaria: This type is triggered by an increase in body temperature, often due to exercise, hot showers, emotional stress, or spicy foods. Small, intensely itchy wheals surrounded by redness are characteristic.
Infections
While not as direct a cause as allergies, certain infections can sometimes be associated with wheal formation, particularly viral infections. Some viral exanthems (rashes) can include urticarial components. Bacterial infections can occasionally lead to generalized urticaria, although this is less common.
Autoimmune Conditions
In some autoimmune diseases, the body’s immune system mistakenly attacks its own tissues. Certain autoimmune conditions, like systemic lupus erythematosus (SLE) or thyroid disease, can be associated with chronic urticaria, where wheals appear for prolonged periods without an identifiable trigger.
Idiopathic Urticaria
In a significant number of cases, particularly with chronic urticaria, the exact cause of wheal formation remains elusive. This is termed idiopathic urticaria, meaning the cause is unknown. Despite extensive investigation, no specific allergen, physical trigger, or underlying medical condition is identified.
Management and Treatment of Wheals
The approach to managing wheals depends largely on their cause, frequency, and severity. For isolated, transient wheals from a known minor irritant, no specific treatment may be necessary, as they resolve on their own. However, for recurrent, widespread, or bothersome wheals, medical intervention is often warranted.
Identification of Triggers
The cornerstone of managing recurrent wheals, especially in the context of urticaria, is the identification and avoidance of triggers. This may involve keeping a detailed diary of diet, activities, exposures, and the timing of wheal onset.
Allergy Testing
If an allergic trigger is suspected, an allergist may perform skin prick tests or blood tests (IgE tests) to identify specific food or environmental allergens. Patch testing may be used to diagnose contact dermatitis.
Elimination Diets
For suspected food allergies, an elimination diet, supervised by a healthcare professional or registered dietitian, can help pinpoint problematic foods. This involves removing suspect foods for a period and then reintroducing them systematically to observe for reactions.
Pharmacological Interventions
When triggers cannot be avoided or identified, or when symptoms are severe, medication plays a crucial role.
Antihistamines
These are the first-line treatment for most types of urticaria and wheal reactions. Antihistamines work by blocking the action of histamine, the primary mediator responsible for the itching, redness, and swelling. Second-generation antihistamines (e.g., loratadine, cetirizine, fexofenadine) are generally preferred as they are less sedating than older, first-generation antihistamines (e.g., diphenhydramine). They are typically taken daily for chronic urticaria.
Corticosteroids
For severe, acute episodes of urticaria or when wheals are accompanied by significant swelling (angioedema), a short course of oral corticosteroids (e.g., prednisone) may be prescribed. These medications reduce inflammation effectively but are generally not recommended for long-term use due to potential side effects. Topical corticosteroids are typically not effective for wheals as they affect the epidermis, while wheals are primarily a dermal phenomenon.
Other Medications
In cases of chronic urticaria that are refractory to antihistamines, other treatments may be considered, including:
- Leukotriene Receptor Antagonists: Medications like montelukast can sometimes provide additional benefit when added to antihistamines.
- Immunosuppressants: For severe, recalcitrant cases, medications that suppress the immune system, such as cyclosporine, may be used under specialist supervision.
- Biologics: Omalizumab (Xolair) is a monoclonal antibody that targets IgE and has shown significant efficacy in treating chronic spontaneous urticaria that does not respond to other therapies.
Lifestyle and Home Management
Beyond medical treatments, certain lifestyle adjustments can contribute to managing wheals.
Avoiding Irritants
Minimizing exposure to known skin irritants, such as harsh soaps, hot water, and certain fabrics, can be beneficial. Wearing loose-fitting clothing can reduce friction and pressure on the skin.
Cool Compresses
Applying cool compresses or taking cool baths can help soothe itching and reduce inflammation associated with wheals.

Stress Management
Since stress can exacerbate many inflammatory skin conditions, including urticaria, employing stress-reducing techniques such as meditation, yoga, or mindfulness can be helpful.
In conclusion, a wheal is a transient, itchy, raised lesion on the skin caused by localized fluid accumulation in the dermis, primarily mediated by histamine release. While often associated with allergic reactions, a diverse range of physical stimuli, infections, and even autoimmune conditions can precipitate their formation. Understanding the distinct characteristics of wheals and their potential triggers is the first step towards effective management and relief. With appropriate diagnosis and a tailored treatment plan, individuals experiencing wheals can significantly improve their quality of life and minimize the impact of these common, yet sometimes concerning, skin manifestations.
