Hydrocolloid bandages represent a significant advancement in wound care, offering a sophisticated approach to healing that far surpasses traditional gauze and adhesive strips. Unlike conventional dressings that merely cover a wound, hydrocolloids actively participate in the healing process by creating an optimal moist environment. This innovative technology has become a cornerstone in modern medical practice, revered for its efficacy in managing a wide array of wounds, from minor cuts and blisters to more complex chronic ulcers. Understanding the unique properties and applications of hydrocolloid bandages is crucial for anyone seeking to optimize wound recovery and minimize scarring.
The Science Behind Hydrocolloids
The effectiveness of hydrocolloid bandages stems from their unique composition and the specific environment they create for wound healing. This science-backed approach differentiates them from passive wound coverings.
Composition and Mechanism
Hydrocolloid bandages are typically composed of a waterproof outer layer, often made of polyurethane film or foam, and an inner adhesive layer containing gel-forming agents. These agents are usually a mixture of hydrophilic (water-loving) colloidal particles such as carboxymethylcellulose, gelatin, and pectin. When these particles come into contact with wound exudate (the fluid that oozes from a wound), they absorb the moisture and swell, forming a soft, cohesive gel. This gel creates a moist, warm environment directly over the wound bed.
The mechanism of action is multifaceted. Firstly, the gel layer provides a barrier against external contaminants like bacteria and viruses, reducing the risk of infection. Secondly, by absorbing excess exudate, the bandage prevents maceration of the surrounding healthy skin while keeping the wound bed moist. This moist environment is critical for several reasons: it facilitates autolytic debridement (the body’s natural process of removing dead tissue), promotes angiogenesis (formation of new blood vessels), and encourages the migration and proliferation of epidermal cells, which are essential for skin regeneration. The slightly acidic pH maintained by the gel is also conducive to healing.
How They Promote Healing
The moist wound healing theory, championed by George D. Winter in the 1960s, forms the fundamental principle behind hydrocolloid bandages. Research has consistently shown that wounds kept moist heal faster and with less scarring compared to those allowed to dry out and form a scab.
- Autolytic Debridement: The gel layer traps enzymes and cells released from the wound bed that are responsible for breaking down necrotic (dead) tissue. This gentle, natural process helps to clean the wound without causing trauma, as might occur with mechanical debridement.
- Optimal Environment for Cell Growth: A moist environment prevents the wound surface from drying out and forming a hard scab. Scabs can impede the migration of new skin cells across the wound bed. In a moist environment, new epithelial cells can glide more easily over the wound surface, accelerating re-epithelialization.
- Reduced Pain: The gel layer not only protects nerve endings from exposure to air and external stimuli but also maintains a constant temperature, both of which contribute to a significant reduction in wound pain.
- Enhanced Angiogenesis: The moist, hypoxic (low oxygen) environment beneath the hydrocolloid has been shown to stimulate the growth of new blood vessels, bringing essential nutrients and oxygen to the healing tissue.
- Minimized Scarring: By promoting organized tissue regeneration and preventing scab formation, hydrocolloids contribute to a smoother healing process, often resulting in less noticeable scarring.
Benefits and Applications
Hydrocolloid bandages offer numerous advantages that make them a preferred choice for various wound types. Their versatility and patient comfort are key factors in their widespread adoption.
Advantages Over Traditional Dressings
Compared to traditional gauze dressings, hydrocolloids present several compelling benefits:
- Extended Wear Time: Hydrocolloids can typically stay on a wound for several days, sometimes up to a week, depending on the amount of exudate. This reduces the frequency of dressing changes, which saves time, decreases exposure to air (and potential contamination), and minimizes disruption to the healing wound bed.
- Waterproof and Breathable: The outer film provides a waterproof barrier, allowing patients to shower or bathe without compromising the dressing’s integrity. Yet, it remains breathable, preventing excessive moisture buildup beneath the bandage.
- Comfort and Conformability: Hydrocolloids are flexible and conform well to body contours, making them comfortable to wear even on joints or awkward areas. The adhesive is typically gentle on the skin, reducing irritation.
- Self-Adherent: Most hydrocolloid bandages are self-adhesive, eliminating the need for additional tapes or secondary dressings, simplifying application.
- Visual Indication of Exudate: As the hydrocolloid absorbs exudate, it swells and may form a visible “blister” or white gel under the bandage. This allows for a visual assessment of exudate levels and helps determine when a dressing change might be needed.
Common Uses for Hydrocolloid Bandages
The versatility of hydrocolloids allows their application across a broad spectrum of wound types:
- Blisters: They are highly effective for treating blisters, providing a protective cushion, reducing pain, and facilitating rapid healing by absorbing the fluid while keeping the underlying skin moist.
- Minor Burns: For superficial and partial-thickness burns (first- and second-degree burns without extensive blistering or open wounds), hydrocolloids can protect the damaged skin and promote healing.
- Abrasions and Minor Cuts: They offer an excellent environment for healing scraped knees, elbow abrasions, and small cuts, protecting them from infection and accelerating recovery.
- Acne Lesions: Smaller hydrocolloid patches have become popular for treating acne, particularly pustules and cystic acne. They absorb pus and oil, reduce inflammation, and protect the blemish from picking, speeding up healing.
- Pressure Ulcers (Bedsores): For stage I and II pressure ulcers, hydrocolloids provide cushioning, protect against further friction and shear, and aid in healing by maintaining a moist environment.
- Venous Leg Ulcers: In combination with compression therapy, hydrocolloids can be used to manage venous leg ulcers, assisting in debridement and granulation.
- Post-Surgical Wounds: For clean, sutured wounds, hydrocolloids can offer protection, absorb minimal exudate, and promote a favorable healing environment.
Specific Wound Types and Conditions
Beyond general applications, hydrocolloids are particularly valuable in scenarios where maintaining a sterile, moist, and protected environment is paramount. They are especially beneficial for wounds with light to moderate exudate. Their ability to gently debride necrotic tissue makes them suitable for wounds that require slough removal. However, for heavily exudating wounds, other dressings with higher absorptive capacities might be more appropriate. The choice often depends on the wound’s specific characteristics, including its depth, location, and the amount of fluid it produces.
Proper Application and Removal
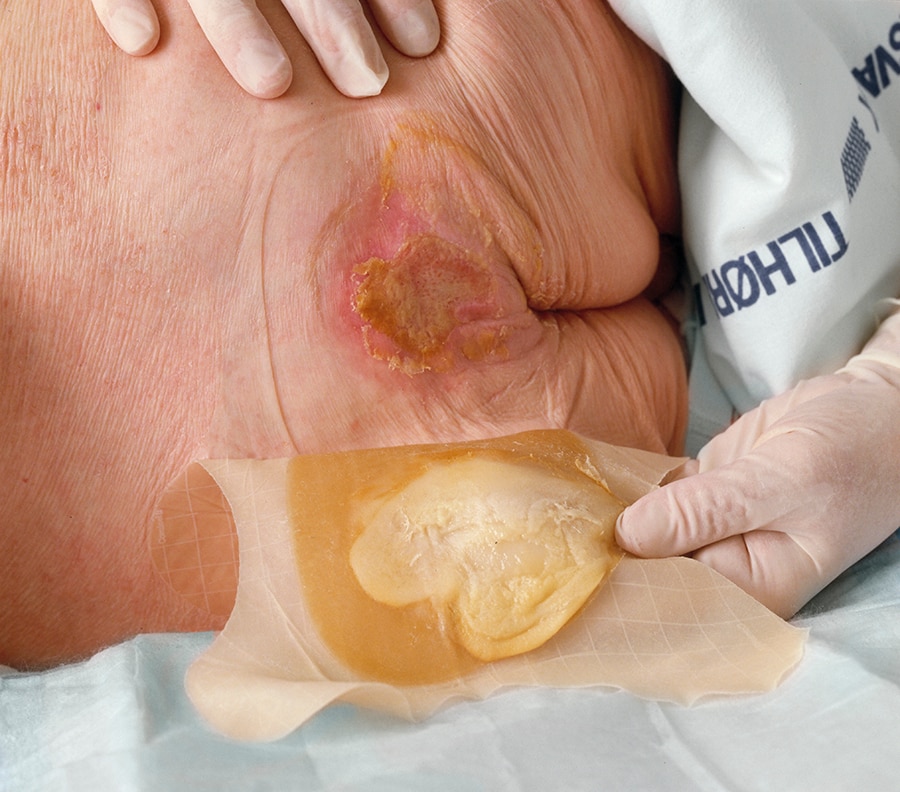
To maximize the benefits of hydrocolloid bandages, correct application and removal techniques are essential. Improper handling can lead to skin irritation, delayed healing, or increased risk of infection.
Preparing the Wound Site
Before applying any hydrocolloid bandage, meticulous wound preparation is critical.
- Cleanse the Wound: Gently clean the wound and the surrounding skin with saline solution or a mild wound cleanser. Avoid using harsh antiseptics like hydrogen peroxide or iodine, as these can damage new tissue.
- Dry the Surrounding Skin: Pat the skin around the wound completely dry. The hydrocolloid’s adhesive will not stick effectively to moist skin, which could cause the bandage to lift at the edges and compromise its protective barrier. Ensure the wound bed itself is clean but can remain slightly moist.
- Assess Wound Size: Select a bandage that is large enough to extend at least an inch beyond the edges of the wound. This ensures complete coverage and allows the adhesive to properly secure to healthy skin, preventing leakage and contamination.
Applying the Bandage
Applying a hydrocolloid bandage correctly helps ensure its longevity and effectiveness.
- Warm the Bandage (Optional): Some users find that gently warming the bandage in their hands for a few moments before peeling off the backing can improve its adhesive properties.
- Remove Backing: Carefully peel off the release paper from the adhesive side of the bandage, being careful not to touch the adhesive surface.
- Position and Apply: Center the bandage over the wound, ensuring it covers the entire wound and extends onto the surrounding healthy skin. Smooth the bandage from the center outwards to eliminate wrinkles and air bubbles, pressing down gently but firmly on the edges to ensure a secure seal.
- Avoid Stretching: Do not stretch the bandage tightly during application, as this can cause tension on the skin and lead to blistering or discomfort, especially on delicate skin.
When and How to Remove
Knowing when and how to remove a hydrocolloid bandage is just as important as proper application.
- When to Remove: Hydrocolloid bandages typically remain in place for 3 to 7 days, or until they become saturated with exudate. Signs of saturation include significant bulging, leakage, or the gel extending close to the edges of the bandage. A white, gel-like substance under the bandage is normal and indicates absorption of exudate; it is not pus.
- Gentle Removal: To remove the bandage, gently lift one edge and slowly peel it back parallel to the skin surface. Avoid pulling upwards, as this can cause trauma to the healing skin. If the adhesive is particularly strong, you can gently stretch the bandage along the skin as you peel, or use a medical adhesive remover wipe to loosen the edges.
- Clean and Reassess: After removal, gently clean the wound and reassess its condition. If healing is progressing well, apply a new hydrocolloid bandage or transition to another appropriate dressing as advised by a healthcare professional.
Potential Considerations and Misconceptions
While hydrocolloid bandages are highly beneficial, it’s important to be aware of their limitations and to address common misunderstandings to ensure safe and effective use.
Signs of Normal Healing vs. Infection
A common concern for users is distinguishing between the normal appearance of a wound healing under a hydrocolloid and signs of infection.
- Normal Healing: When a hydrocolloid absorbs wound exudate, it often forms a whitish or yellowish gel beneath the dressing. This is a normal, healthy sign and should not be confused with pus. The wound itself, when uncovered, may appear moist, pink, and healthy.
- Signs of Infection: Be vigilant for indicators of infection, which include:
- Increasing Redness or Swelling: The skin around the wound becomes noticeably redder or more swollen and the redness spreads beyond the bandage’s edge.
- Increased Pain: A significant increase in pain that is not alleviated by the bandage.
- Foul Odor: A strong, unpleasant smell emanating from the wound upon removal of the bandage.
- Green or Dark Yellow Pus: Unlike the clear or whitish gel, actual pus is typically thicker, discolored (green, dark yellow, or grey), and may have a strong odor.
- Fever or Chills: Systemic signs of infection, such as fever or chills, warrant immediate medical attention.
If any of these signs are present, remove the bandage, clean the wound, and consult a healthcare professional immediately.
Who Should Not Use Hydrocolloids
Despite their broad utility, hydrocolloid bandages are not suitable for all wound types or individuals.
- Heavily Exudating Wounds: Wounds that produce a large amount of fluid can overwhelm the absorptive capacity of hydrocolloids, leading to leakage and maceration of surrounding skin. For such wounds, super-absorbent dressings are more appropriate.
- Infected Wounds (without concurrent treatment): While hydrocolloids create a barrier against new infections, they are generally not recommended as the primary dressing for actively infected wounds unless used under strict medical supervision and in conjunction with systemic antibiotics or topical antimicrobials. The occlusive nature could trap bacteria and worsen the infection.
- Deep Cavity Wounds: Hydrocolloids are typically flat and not designed to fill deep wounds or those with tunneling. For these, specialized cavity dressings or wound fillers are needed.
- Full-Thickness Burns: For severe burns (third-degree burns), specialized burn dressings and immediate medical intervention are required.
- Wounds with Exposed Bone or Tendon: These wounds require advanced medical care and specific dressings to protect underlying structures.
- Individuals with Known Allergy: Although rare, some individuals may have an allergic reaction to components of the bandage.

Addressing Common Concerns
Many first-time users of hydrocolloid bandages might have questions or misconceptions.
- “Is the white gel pus?” As clarified, the white or yellowish gel is a normal byproduct of the bandage absorbing wound exudate and should not be mistaken for pus.
- “My wound smells bad when I remove the bandage.” A mild, slightly sweet odor can sometimes be present due to the accumulation of exudate and bacteria under the occlusive dressing. This is often normal. However, a strong, foul, or putrid odor is a sign of infection and requires medical evaluation.
- “It’s sticky and hard to remove.” Warm water or a medical adhesive remover can aid in gentle removal, especially if the bandage has been on for several days.
In conclusion, hydrocolloid bandages are a powerful tool in modern wound management, offering an effective, comfortable, and often more efficient path to healing than traditional methods. By creating an optimal moist environment, they not only protect the wound but actively facilitate the body’s natural regenerative processes. Proper selection, application, and monitoring are key to harnessing their full potential and achieving superior wound outcomes.
