Ultrasound imaging has become an indispensable tool in modern obstetrics, offering a non-invasive window into fetal development. Among its most profound applications is the detection of congenital anomalies, such as spina bifida. This neural tube defect, characterized by incomplete closure of the spinal cord, can manifest in various forms and severities. Understanding what spina bifida looks like on an ultrasound is crucial for early diagnosis, parental counseling, and timely intervention. This article delves into the visual cues that radiologists and sonographers look for when assessing the fetal spine for spina bifida, exploring both the characteristic findings and the nuances that can affect interpretation.
Visualizing the Fetal Spine: The Ultrasound Examination
The assessment of the fetal spine during an ultrasound is a systematic process, typically performed as part of routine antenatal screening or when specific concerns arise. The sonographer or radiologist meticulously examines the vertebral column from the cervical to the sacral regions, looking for any deviations from normal anatomy. This examination is often performed in multiple planes to ensure a comprehensive evaluation.
Standard Ultrasound Protocols for Spinal Assessment
During a standard obstetric ultrasound, usually conducted between 18 and 22 weeks of gestation, the fetal spine is visualized to assess its integrity. The technician will orient the probe along the long axis of the fetus to obtain sagittal views of the spine. In these sagittal planes, the characteristic three ossified centers within each vertebra (anterior and two posterior) should be clearly visible, forming a continuous, linear structure. The alignment of these ossification centers is paramount.
Transverse views are equally important. By imaging the spine in cross-section, the sonographer can assess the closure of the posterior elements of the vertebrae, specifically the laminae. In a normal spine, the posterior elements should form a closed, continuous, U-shaped or V-shaped arch in each vertebral segment. Any breaks or discontinuities in this posterior arch are highly suggestive of a spinal defect.
Key Anatomical Structures to Evaluate
- Vertebral Bodies: The bony components of the spine that support the weight of the body. Their alignment and integrity are assessed.
- Posterior Elements (Laminae and Pedicles): These form the bony arch that encloses the spinal canal. Their complete closure is critical.
- Spinal Cord: The neural tissue within the spinal canal. While difficult to visualize in detail in early scans, its position and relationship to the bony structures are important.
- Surrounding Soft Tissues: The skin and subcutaneous tissue overlying the spine. Defects can often involve an abnormal protrusion or absence of these layers.
The quality of the ultrasound images is significantly influenced by factors such as fetal position, amniotic fluid volume, maternal body habitus, and gestational age. Optimal visualization is achieved when the fetus is well-positioned, allowing clear acoustic windows.
Characteristic Ultrasound Findings of Spina Bifida
Spina bifida encompasses a spectrum of defects, ranging from the most severe, myelomeningocele, to the milder, spina bifida occulta. The ultrasound appearance will vary depending on the type and extent of the defect.
Myelomeningocele: The Most Visible Form
Myelomeningocele, the most severe and common form of spina bifida detectable by ultrasound, is characterized by the protrusion of the spinal cord and its meninges through an opening in the vertebral column. On ultrasound, this presents with several distinct findings:
- The “Lemon Sign”: In cases of myelomeningocele, the anterior and lateral aspects of the fetal skull can appear flattened, creating a characteristic concave shape that resembles a lemon. This finding is often associated with hydrocephalus, a common complication.
- The “Banana Sign”: The cerebellum, located at the back of the brain, can be displaced downwards and appear unusually curved, resembling a banana, due to the downward pressure caused by the herniated spinal contents. This is another marker of Chiari II malformation, frequently seen with myelomeningocele.
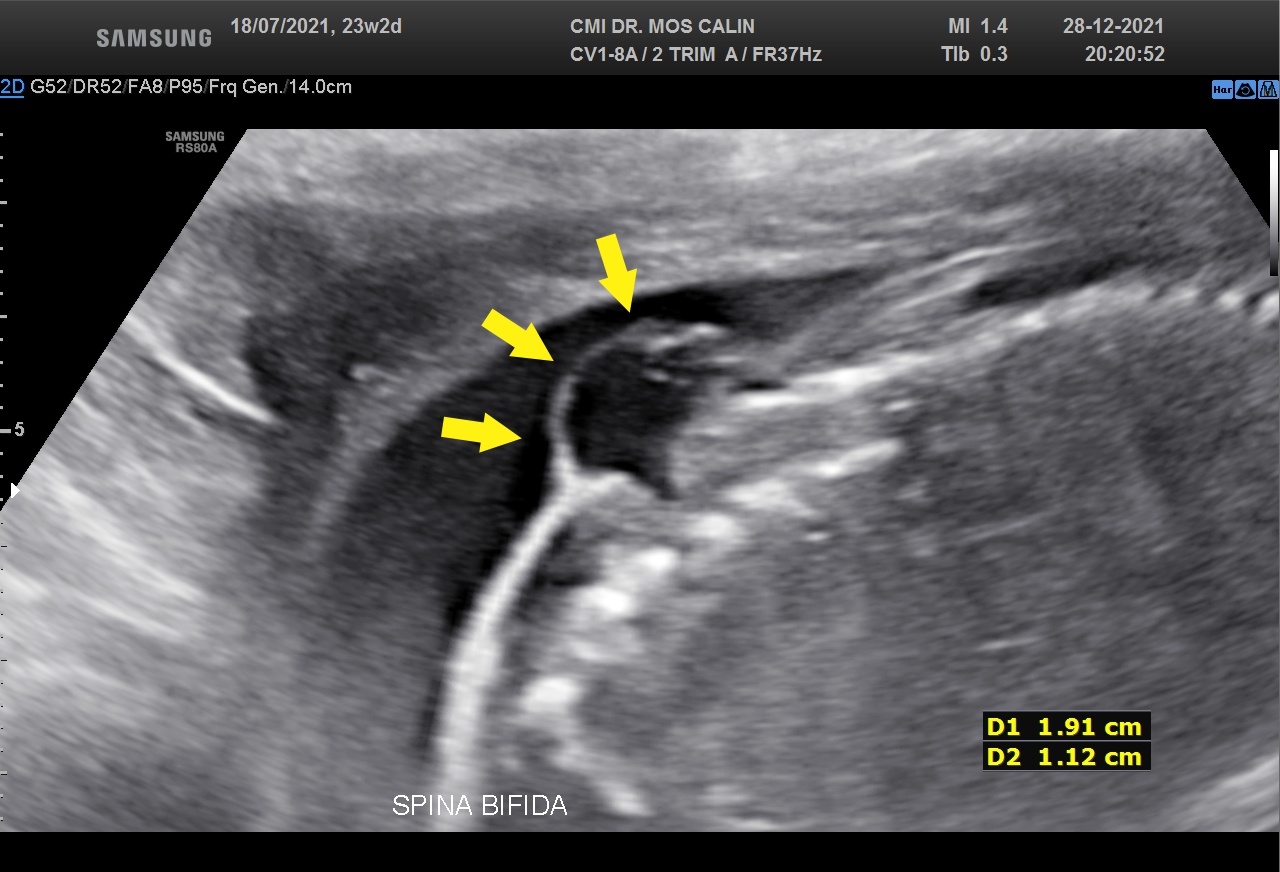
- Vertebral Arch Defect: The most direct evidence of spina bifida is the absence of the posterior ossification centers in the affected vertebral segments. Instead of a continuous U-shape, a wide gap or discontinuity is observed in the vertebral arch. This defect is typically most evident in the lumbosacral region.
- Protrusion of Sac Contents: The hallmark of myelomeningocele is the visible sac-like protrusion of meninges and spinal cord tissue through the vertebral defect. This mass may appear cystic or complex on ultrasound, often with irregular margins. Its presence is a strong indicator of an open neural tube defect.
- Abnormalities of the Spinal Cord: In some cases, the spinal cord itself may appear abnormal, showing tethering or thickening within the protruding sac.
The severity of the vertebral defect and the extent of neural tissue involvement will dictate the size and appearance of the protruding sac. In severe cases, the sac can be quite large, extending significantly from the fetal back.
Spina Bifida Occulta: The Hidden Defect
Spina bifida occulta is a milder form where the spinal cord and meninges are not exposed, and the defect is covered by skin. This form is often asymptomatic and may go unnoticed. However, certain subtle findings can sometimes be detected on ultrasound, though its diagnosis is frequently made later in life through X-rays.
- Minor Discontinuity in Posterior Elements: While not as dramatic as in myelomeningocele, a subtle break or gap in the posterior vertebral arch may be present. This might manifest as a small indentation or a slight disruption in the otherwise continuous U-shape of the lamina in the transverse view.
- Slight Sagging or Deviation: In some instances, a very slight sagging or deviation of the posterior elements might be observed in sagittal views, hinting at an underlying weakness or incomplete closure.
- Local Skin Dimple or Tuft of Hair: While not directly visualized on standard ultrasound, if a specific prenatal imaging protocol focuses on superficial fetal structures and the amniotic fluid allows for good visualization, a localized skin abnormality like a dimple or a small tuft of hair over the spine might be suggested, though this is not a definitive ultrasound finding.
It is important to note that diagnosing spina bifida occulta solely through prenatal ultrasound can be challenging due to its subtle nature. Many cases are only discovered incidentally in childhood or adulthood.
Advanced Imaging Techniques and Diagnostic Considerations
While standard 2D ultrasound remains the primary modality for detecting spina bifida, advancements in technology and specialized techniques can further refine the diagnosis and provide crucial information.
Three-Dimensional (3D) and Four-Dimensional (4D) Ultrasound

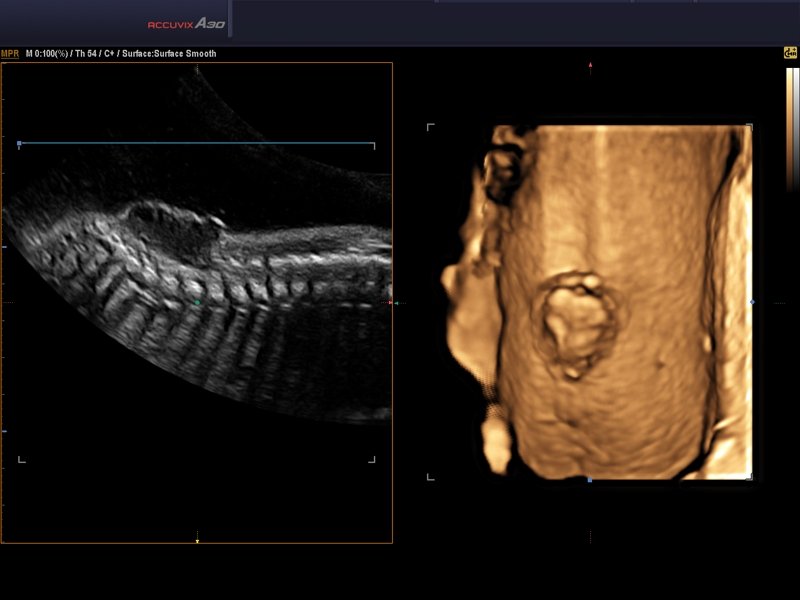
3D and 4D ultrasound offer a more intuitive and comprehensive visualization of fetal anatomy, including the spine. These techniques can provide surface renderings of the fetal back, allowing for a clearer appreciation of the extent of the vertebral defect and the overlying skin.
- Surface Rendering: 3D ultrasound can create detailed surface models of the fetal spine, highlighting any irregularities, protrusions, or gaps in the vertebral arches. This can be particularly helpful in distinguishing between a closed defect and an open one, and in assessing the size and shape of any visible sac.
- Improved Spatial Understanding: The ability to view the spine from different angles and in a more anatomically realistic representation can aid in understanding the spatial relationship of the defect to surrounding structures. This can be beneficial for surgical planning if intervention is considered.
While 3D/4D ultrasound can enhance visualization, it does not replace the diagnostic accuracy of high-quality 2D imaging. It serves as a complementary tool that can improve parental understanding and provide additional anatomical detail.
Fetal MRI for Complex Cases
In cases where the ultrasound findings are equivocal, or when more detailed information about the neural tissue and surrounding structures is required, fetal Magnetic Resonance Imaging (MRI) may be employed. Fetal MRI offers superior soft-tissue contrast and can provide high-resolution images of the spinal cord, meninges, and any associated abnormalities.
- Detailed Neural Tissue Assessment: Fetal MRI can delineate the extent of spinal cord involvement, identify tethering, and assess for other associated central nervous system anomalies that might not be fully appreciated on ultrasound.
- Evaluation of Complications: It can also be used to evaluate for complications such as hydrocephalus or other brain abnormalities.
Fetal MRI is typically reserved for specific situations due to its cost and the need for specialized expertise and equipment. It is not a routine screening tool for spina bifida.
Differential Diagnoses and Pitfalls
Interpreting ultrasound images requires careful consideration of potential differential diagnoses and awareness of common pitfalls.
- Normal Spinal Variations: In some instances, normal ossification patterns or fetal positioning can mimic a spinal defect. For example, the posterior ossification centers may not be fully mineralized in early gestation, leading to a temporarily incomplete appearance.
- Skeletal Abnormalities: Other skeletal anomalies, such as vertebral segmentation defects or vertebral body hypoplasia, could potentially be confused with spina bifida.
- Maternal Obesity or Poor Amniotic Fluid: These factors can significantly degrade image quality, making it difficult to visualize the delicate structures of the fetal spine with clarity. This can lead to either false positives or false negatives.
- Artifacts: Ultrasound artifacts, such as shadowing from maternal bone or gas, can obscure anatomical details and lead to misinterpretations.
Experienced sonographers and radiologists are trained to recognize these challenges and employ techniques to optimize image acquisition and interpretation, ensuring the most accurate diagnosis possible. The follow-up of any suspicious finding with a specialized fetal medicine unit is often recommended.
The Significance of Early Detection
The ability of ultrasound to detect spina bifida prenatally has revolutionized the management of this condition. Early diagnosis provides a multitude of benefits for families and healthcare providers.
Parental Counseling and Decision-Making
Receiving a diagnosis of spina bifida can be overwhelming for expectant parents. Ultrasound provides visual evidence of the anomaly, facilitating comprehensive counseling sessions with specialists. This allows parents to:
- Understand the Nature of the Defect: Detailed explanations can be provided regarding the type and severity of spina bifida, its potential impact on the child’s health and development, and the spectrum of possible outcomes.
- Explore Management Options: Parents can learn about the available treatment options, including surgical repair, assistive devices, and ongoing therapies.
- Prepare for Delivery and Postnatal Care: Knowing about the condition in advance enables parents to plan for specialized delivery at a center with pediatric neurosurgical capabilities and to prepare for the intensive postnatal care their child may require.
- Emotional and Psychological Support: Early diagnosis allows families to access emotional and psychological support services, helping them to cope with the diagnosis and make informed decisions.
Pre-Natal Intervention and Surgical Planning
In certain cases, prenatal surgery to repair myelomeningocele before birth is an option. Ultrasound plays a critical role in identifying suitable candidates for this complex procedure.
- Assessing Suitability for Prenatal Surgery: Detailed ultrasound assessments, often supplemented by fetal MRI, help determine if the fetus meets the criteria for prenatal repair, considering factors such as gestational age, the location and severity of the defect, and the absence of other major anomalies.
- Surgical Planning: Prenatal imaging provides vital anatomical information that guides the surgical team in planning the timing and approach of the prenatal repair.
Postnatal Management and Outcomes
A prenatal diagnosis allows for immediate postnatal management upon delivery.
- Prompt Surgical Intervention: Newborns diagnosed with spina bifida can undergo surgical closure of the defect shortly after birth, which is crucial for reducing the risk of infection and further neurological damage.
- Multidisciplinary Care Planning: The prenatal diagnosis facilitates the establishment of a multidisciplinary care team, including neurosurgeons, urologists, orthopedic surgeons, physical therapists, and developmental specialists, ensuring comprehensive and coordinated care from the outset.
- Improved Long-Term Outcomes: With timely and appropriate interventions, including early surgical repair and ongoing rehabilitation, individuals with spina bifida can achieve better functional outcomes and improved quality of life.
In conclusion, the visualization of spina bifida on ultrasound has transformed the landscape of prenatal care. By understanding the characteristic ultrasound findings, from the subtle signs of spina bifida occulta to the more dramatic presentations of myelomeningocele, healthcare professionals can provide families with vital information, enabling informed decision-making and paving the way for optimized postnatal management and improved long-term outcomes for affected children. The continuous evolution of imaging technologies promises even greater clarity and precision in the detection and characterization of this complex congenital condition.
