Herpes of the throat, often referred to as oral herpes or cold sores on the mouth, is a common viral infection caused by the herpes simplex virus (HSV). While typically associated with the lips and surrounding facial areas, HSV can manifest within the oral cavity, including the throat. Understanding the visual presentation of throat herpes is crucial for timely identification and management. This article will delve into the characteristic appearances of oral herpes when it affects the throat, exploring its various stages and distinguishing features.
The Initial Stages: Prodromal Symptoms and Early Lesions
The onset of oral herpes in the throat often begins with prodromal symptoms, a period of warning signs that precede the appearance of visible lesions. These sensations are a vital clue to the impending outbreak and can vary in intensity and duration from person to person. While these symptoms are not directly visible, they are an integral part of the process leading to what the throat herpes “looks like.”
Tingling, Itching, and Burning Sensations
The earliest, and often invisible, signs of a developing herpes outbreak in the throat are a cluster of subjective sensations. Individuals commonly report an insidious onset of tingling, itching, or a burning feeling within the throat, sometimes localized to a specific area. This often occurs one to two days before any visible changes become apparent. The intensity of these feelings can range from a mild, almost imperceptible prickle to a more pronounced discomfort. This initial phase is a critical window where awareness can lead to proactive management. The sensation can be mistaken for a common sore throat, but its distinct tingling or burning quality often sets it apart for those familiar with herpes outbreaks.
Redness and Swelling
As the prodromal phase progresses, the affected area in the throat may begin to show subtle visual changes. The tissues might appear slightly redder than the surrounding healthy mucosa, indicating inflammation. This redness, known as erythema, is a direct response of the immune system to the viral activity. Alongside the redness, there may be a slight, localized swelling. This swelling can make the area feel slightly raised or bumpy to the touch, though this is often only detectable by the individual experiencing the symptoms. These early visual cues are still relatively mild and can be easily overlooked, especially if the individual is not specifically looking for signs of herpes.
The Formation of Blisters: The Hallmark of Herpes
The most definitive visual characteristic of oral herpes, including when it presents in the throat, is the formation of small, fluid-filled blisters, medically termed vesicles. These blisters are the direct result of the HSV replicating within the cells of the mucous membranes. Their appearance and evolution are key to identifying throat herpes.
Small, Clear, or Whitish Blisters
The hallmark of an active herpes outbreak in the throat is the eruption of small blisters. These vesicles typically appear as tiny, raised bumps, often no larger than a pinhead. Initially, they may be filled with clear fluid. As the outbreak progresses, the fluid inside can become slightly cloudy or whitish due to the presence of inflammatory cells and viral particles. These blisters are often clustered together, forming a small patch or group of lesions. The surface of these blisters is typically smooth and taut, and they may be surrounded by a slightly red halo, further indicating inflammation.
Location Within the Throat
The precise location of these blisters within the throat can influence how they are perceived and described. While less common than on the lips, herpes lesions in the throat can appear on the:
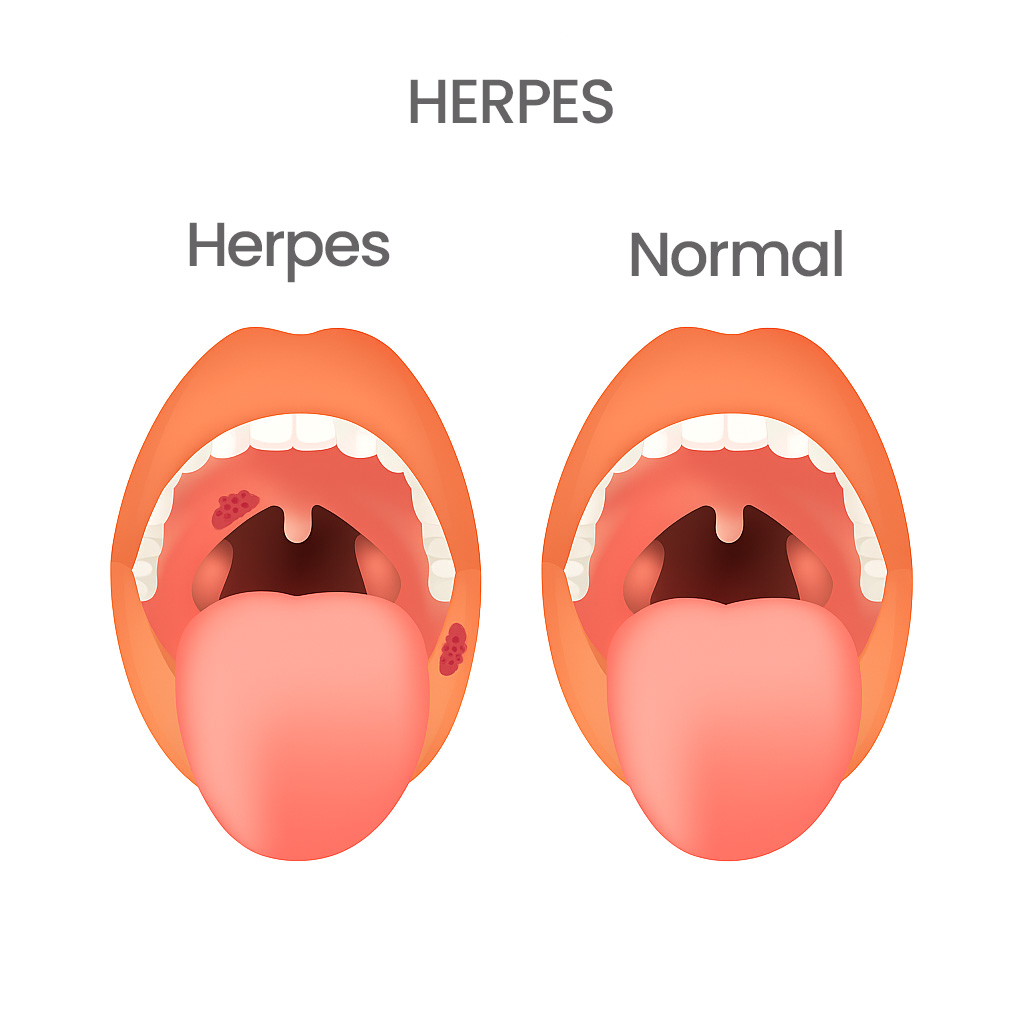
- Tonsils: This is a frequent site. Lesions on the tonsils can appear as clusters of small blisters or ulcerated sores, which may make swallowing particularly painful. They can be difficult to see without a good light source and a tongue depressor, often presenting as white or yellowish spots or ulcers on the tonsillar surface.
- Back of the Throat (Pharyngeal Wall): Lesions on the posterior pharyngeal wall can be more diffuse and may present as small red bumps that quickly ulcerate. They might be more noticeable when the individual opens their mouth wide and strains to look.
- Uvula and Soft Palate: These areas can also be affected, leading to localized pain and discomfort. Blisters here might be more visible and can cause a foreign body sensation.
- Gums and Inner Cheeks: While not strictly “throat,” these areas are part of the oral cavity and can be affected by HSV, sometimes co-occurring with throat lesions.
The appearance on these internal surfaces differs from the external presentation on the lips. Instead of a raised, crusting lesion, internal lesions are typically more mucosal and prone to ulceration.
Ulceration and Sore Formation
Following the blister stage, the vesicles typically rupture, leading to the formation of shallow, open sores or ulcers. This stage is often associated with the most significant pain and discomfort.

Open, Shallow Sores
Once the blisters break, they leave behind open, shallow ulcers. These ulcers are typically small, round or oval, and have a red base. The edges may appear slightly raised and inflamed. The surface of the ulcer might be covered with a thin, yellowish-white exudate, which is a collection of pus and dead cells. This exudate can contribute to the characteristic foul odor that sometimes accompanies active herpes outbreaks. The pain experienced at this stage is often sharp and can be exacerbated by any contact, including swallowing food or liquid.
Pain and Discomfort
The ulcerated lesions in the throat are invariably accompanied by significant pain and discomfort. This pain can interfere with essential daily functions such as eating, drinking, and speaking. Swallowing, in particular, becomes a challenging and often agonizing experience, leading to a reluctance to eat or drink, which can, in turn, lead to dehydration. The pain can be described as a raw, burning, or throbbing sensation, and it can radiate to the ears or neck.
Healing and Resolution
The final stage of a throat herpes outbreak involves the healing of the ulcers and the complete resolution of the infection. This process is marked by visual changes as the lesions gradually diminish in size and appearance.
Crusting and Scarring (Less Common Internally)
On external surfaces like the lips, ruptured blisters typically form a characteristic crust or scab. However, within the moist environment of the throat, full crusting is less common. Instead, the ulcers may gradually fill in with new tissue and gradually become less inflamed. While significant scarring from oral herpes within the throat is rare, a temporary change in the mucosal surface might be noticeable in the immediate aftermath of healing. The area may appear slightly discolored or smoother than the surrounding tissue for a short period.
Gradual Reduction in Inflammation and Pain
As the body’s immune system effectively fights off the HSV, the inflammation subsides. The redness and swelling decrease, and the pain gradually diminishes. The ulcers begin to shrink in size, and the exposed tissue starts to regenerate. This healing process typically takes about one to two weeks, though it can sometimes be longer depending on the severity of the outbreak and the individual’s immune response. By the end of this stage, the throat should return to its normal appearance, and all associated symptoms will have resolved.
Distinguishing Throat Herpes from Other Conditions
It is crucial to differentiate throat herpes from other conditions that can cause similar symptoms, such as strep throat, tonsillitis, or canker sores. While the visual presentation can offer clues, medical consultation is often necessary for a definitive diagnosis.
Comparison with Strep Throat and Tonsillitis
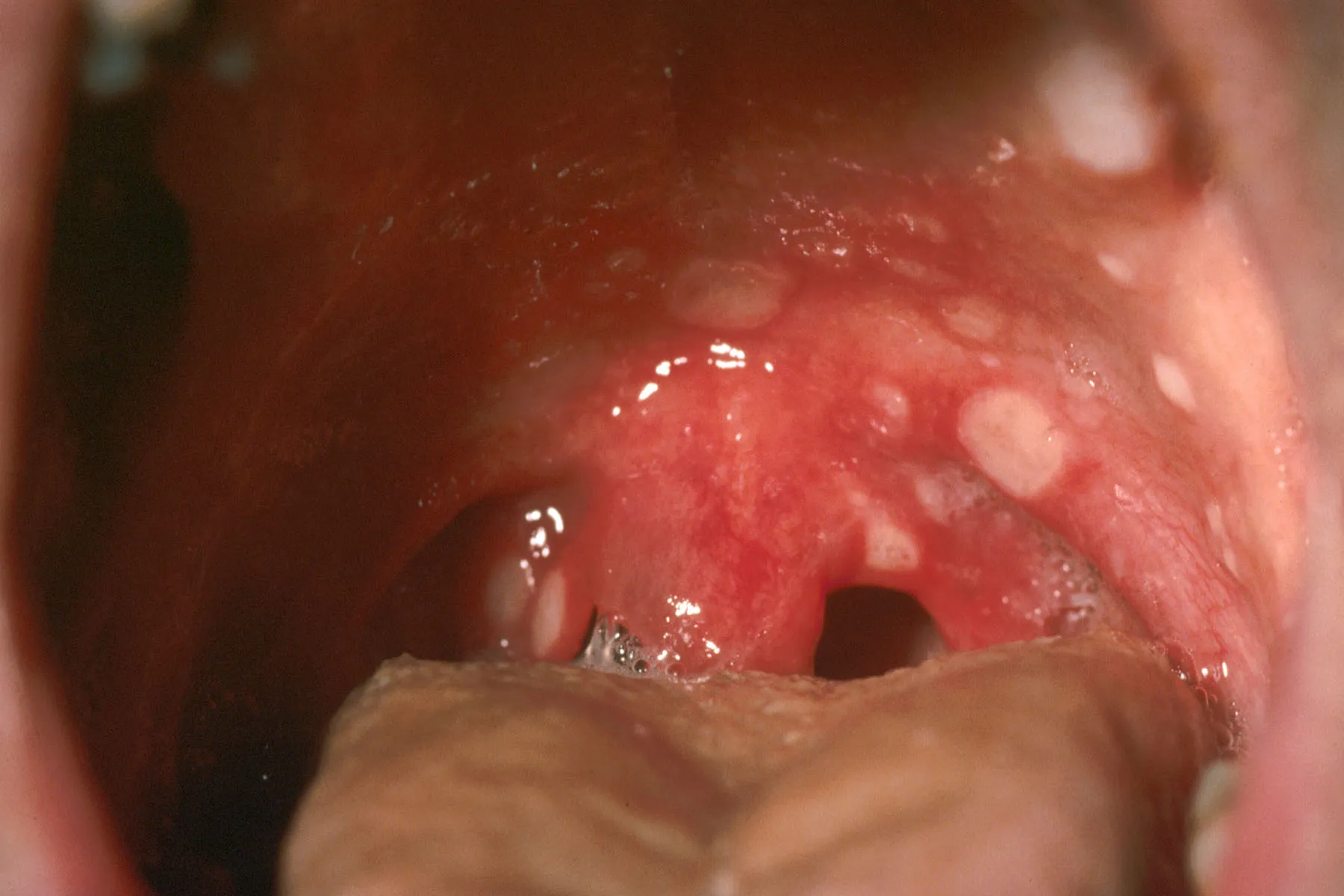
Strep throat and tonsillitis are bacterial infections that often present with a sore throat, fever, and swollen tonsils. However, the visual appearance of the lesions differs. Strep throat typically causes significant redness and swelling of the tonsils, often with white or yellow patches or streaks of pus, but rarely presents with distinct, fluid-filled blisters. Tonsillitis can also cause redness and swelling, and sometimes exudate on the tonsils, but the characteristic herpetic vesicles are absent. A key differentiator is the presence of vesicles in herpes, whereas bacterial infections are more likely to have diffuse redness and pus.
Differentiating from Canker Sores (Aphthous Ulcers)
Canker sores, or aphthous ulcers, are also common in the mouth and can cause significant pain. However, canker sores typically appear as single, round or oval ulcers with a white or yellowish center and a red border. They do not typically form clusters of blisters and are not caused by HSV. Canker sores usually occur on the movable parts of the mouth, such as the inside of the lips, cheeks, and tongue, rather than exclusively on the tonsils or back of the throat, although they can occur on the gums or palate. The presence of preceding blisters is a strong indicator of herpes, while canker sores generally appear as ulcers from the outset.
The Role of Medical Consultation
Given the potential for confusion with other conditions, and the importance of accurate diagnosis for appropriate treatment, seeking medical advice is paramount. A healthcare professional can visually inspect the throat, ask about symptoms, and, if necessary, perform diagnostic tests such as a viral culture or PCR test to confirm the presence of HSV. Early diagnosis can lead to prompt management, including antiviral medications that can shorten the duration and severity of outbreaks.
In conclusion, herpes of the throat typically begins with subtle prodromal sensations, progresses to the formation of small, fluid-filled blisters on the tonsils, pharyngeal wall, or other oral mucosal surfaces, which then rupture to form painful ulcers. Understanding these visual cues, while recognizing the importance of medical consultation for differentiation from other conditions, empowers individuals to better identify and manage this common viral infection.
