An early period, a menstrual cycle that arrives sooner than anticipated, can be a source of concern and curiosity for many individuals. While variations in menstrual cycle length are common and can be influenced by a myriad of factors, a consistently early period might warrant a closer look. Understanding the potential indicators behind a shortened cycle is crucial for maintaining reproductive health and addressing any underlying issues proactively. This exploration delves into the physiological and lifestyle elements that can contribute to an early period, offering insights into what these changes might signify.
Understanding the Menstrual Cycle’s Rhythm
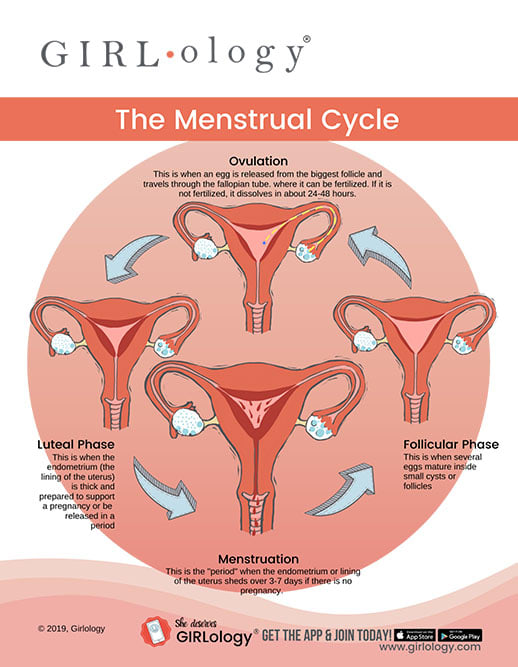
The menstrual cycle is a complex interplay of hormones that prepares the body for potential pregnancy. Typically, a cycle ranges from 21 to 35 days, with the average being around 28 days. The count begins on the first day of menstruation (Day 1) and ends on the day before the next period starts. This cycle is broadly divided into two main phases:

The Follicular Phase
This phase begins on Day 1 of the period and lasts until ovulation. During this time, the pituitary gland releases follicle-stimulating hormone (FSH), which stimulates the ovaries to develop several follicles, each containing an immature egg. As these follicles grow, they produce estrogen. The dominant follicle, which matures most effectively, will eventually release its egg.
The Luteal Phase
This phase begins after ovulation and lasts until the start of the next period. Following ovulation, the ruptured follicle transforms into the corpus luteum, which produces progesterone and estrogen. These hormones thicken the uterine lining (endometrium) in preparation for a potential fertilized egg. If fertilization does not occur, the corpus luteum degenerates, leading to a drop in progesterone and estrogen levels. This hormonal decline triggers the shedding of the uterine lining, resulting in menstruation.
A shortened menstrual cycle, meaning a period arriving earlier than expected, can occur due to alterations in either of these phases. Most commonly, a consistently early period is a result of a shortened luteal phase, also known as luteal phase defect (LPD). However, other factors affecting the follicular phase can also lead to a shorter overall cycle.
Factors Contributing to an Early Period
A variety of factors, ranging from lifestyle choices to underlying medical conditions, can influence the timing of a woman’s menstrual cycle. Identifying these potential causes is the first step in understanding what an early period might indicate.
Hormonal Fluctuations and Imbalances
The delicate balance of reproductive hormones—estrogen, progesterone, FSH, and luteinizing hormone (LH)—is fundamental to a regular menstrual cycle. Disruptions to this balance can lead to shorter cycles.
-
Polycystic Ovary Syndrome (PCOS): This common endocrine disorder is characterized by hormonal imbalances that can lead to irregular ovulation or anovulation. While PCOS is often associated with irregular or absent periods, it can also manifest as shorter cycles in some individuals due to imbalances in androgens and LH. The hormonal chaos can disrupt the normal follicular development and ovulation process.
-
Thyroid Disorders: Both an overactive thyroid (hyperthyroidism) and an underactive thyroid (hypothyroidism) can significantly impact the menstrual cycle. Thyroid hormones play a role in regulating reproductive hormones. Hyperthyroidism, in particular, can accelerate metabolic processes, potentially leading to shorter cycles by affecting ovulation timing or the duration of the luteal phase. Hypothyroidism, while often linked to longer or absent periods, can also contribute to irregularities, including shortened cycles in some cases.
-
High Prolactin Levels (Hyperprolactinemia): Prolactin is a hormone primarily responsible for milk production. Elevated levels of prolactin, for reasons other than pregnancy or breastfeeding, can interfere with the release of FSH and LH, disrupting ovulation and leading to irregular periods, including shorter cycles.
-
Perimenopause: As women approach menopause, their ovaries gradually produce less estrogen and progesterone. This hormonal decline can cause significant changes in the menstrual cycle, including periods that become shorter, lighter, heavier, or more irregular. An early period can be an early sign of perimenopause, as the body’s hormonal regulation shifts.
Lifestyle and Environmental Factors
External influences can also play a substantial role in disrupting the body’s hormonal equilibrium and consequently affecting the menstrual cycle.
- Stress: Significant emotional or physical stress can disrupt the hypothalamic-pituitary-ovarian (HPO) axis, the signaling pathway that regulates the menstrual cycle. Chronic stress can lead to the release of stress hormones like cortisol, which can interfere with the release of GnRH (gonadotropin-releasing hormone), a key hormone in the reproductive cascade. This disruption can lead to skipped periods, irregular cycles, or, in some cases, shorter cycles by affecting ovulation.
-
Extreme Weight Changes: Significant and rapid weight loss or gain can disrupt hormonal balance. Inadequate body fat can lead to the body conserving energy, potentially suppressing reproductive hormone production and affecting ovulation. Conversely, excessive body fat can also lead to hormonal imbalances, particularly in estrogen levels, which can influence cycle length.
-
Intense Exercise: Overtraining or engaging in very strenuous physical activity, especially without adequate caloric intake, can impact the HPO axis. The body may prioritize energy for physical exertion over reproductive functions, leading to menstrual irregularities, including shorter cycles.
-
Poor Nutrition: A diet lacking essential nutrients can impact overall health and hormonal balance. Deficiencies in vitamins and minerals critical for hormone production and regulation can contribute to cycle irregularities.
-
Sleep Disturbances: Disruptions to the natural sleep-wake cycle (circadian rhythm) can affect hormone production. Insufficient or poor-quality sleep can impact the HPO axis and lead to hormonal imbalances that manifest as menstrual irregularities.
Medical Conditions and Treatments
Certain medical conditions and their treatments can also influence menstrual cycle length.
-
Uterine Fibroids and Polyps: These non-cancerous growths in the uterus can cause abnormal bleeding patterns, including changes in menstrual flow and timing. While they don’t directly shorten the cycle in the typical sense of ovulation timing, they can lead to intermenstrual bleeding or a perception of a shorter cycle due to spotting.
-
Endometriosis: This condition, where uterine-like tissue grows outside the uterus, can cause irregular bleeding, pelvic pain, and infertility. Hormonal fluctuations associated with endometriosis can sometimes contribute to shorter or more frequent periods.
-
Certain Medications: Some medications can affect hormonal balance and menstrual regularity. For example, some antidepressants, antipsychotics, chemotherapy drugs, and hormonal contraceptives can influence cycle length and regularity.
-
Early Menopause: While less common, some individuals may experience early menopause (before age 40). This is characterized by a significant decline in ovarian function and can manifest with erratic periods, including consistently shorter cycles, as the ovaries produce fewer eggs and hormones.
When to Seek Medical Advice
While occasional variations in menstrual cycle length are normal, a consistently early period, especially if accompanied by other concerning symptoms, warrants medical attention. It is advisable to consult a healthcare provider if you experience:
- Consistently Short Cycles: If your period arrives every 21 days or less for several consecutive months.
- Sudden Changes: A noticeable and persistent shift in your cycle length from your usual pattern.
- Associated Symptoms: Besides an early period, if you experience any of the following, it’s important to get checked:
- Severe pelvic pain
- Abnormal vaginal bleeding (e.g., heavy bleeding, bleeding between periods)
- Unexplained weight changes
- Increased facial hair growth or acne (potential signs of PCOS)
- Fatigue, weight gain, or hair loss (potential thyroid issues)
- Difficulty conceiving
- Symptoms of perimenopause at a younger age
A healthcare professional can perform a thorough evaluation, which may include a medical history, physical examination, blood tests to check hormone levels (FSH, LH, estrogen, progesterone, thyroid hormones, prolactin), and potentially imaging tests such as an ultrasound to assess the ovaries and uterus.
The Significance of a Shortened Luteal Phase
As mentioned earlier, a shortened luteal phase is a common cause of consistently early periods. The luteal phase is crucial for supporting early pregnancy. A healthy luteal phase typically lasts between 10 to 16 days. If the luteal phase is significantly shorter than this, it can lead to:
-
Infertility: A shortened luteal phase may not provide sufficient time for a fertilized egg to implant in the uterine lining. The declining hormone levels might trigger menstruation before implantation can successfully occur.
-
Recurrent Miscarriage: Even if implantation occurs, a short luteal phase can make it difficult for the pregnancy to be sustained, potentially leading to early miscarriages.
Diagnosing a luteal phase defect often involves tracking ovulation through basal body temperature charting, ovulation predictor kits, or monitoring hormone levels throughout the cycle. Treatment for luteal phase defect may involve progesterone supplementation during the luteal phase to help support implantation and early pregnancy.

Conclusion: Proactive Health Management
An early period, while potentially alarming, is often a signal from the body that can be understood and addressed. By understanding the intricate hormonal mechanisms of the menstrual cycle and recognizing the various factors that can influence it, individuals can be more attuned to their reproductive health. Whether it’s a matter of lifestyle adjustments, stress management, or addressing an underlying medical condition, seeking professional guidance is paramount. Proactive engagement with healthcare providers ensures that any indicators of an early period are properly investigated, leading to appropriate management and the maintenance of overall well-being. The menstrual cycle is a vital indicator of a woman’s health, and paying attention to its rhythm can unlock crucial insights into her physiological state.
