A dry socket, medically known as alveolar osteitis, is a painful complication that can occur after a tooth extraction, most commonly a wisdom tooth. While the initial extraction may go smoothly, the subsequent development of a dry socket can cause significant discomfort and distress. Understanding what a dry socket looks like is crucial for timely recognition and management, enabling a quicker return to comfort and proper healing. This condition arises when the blood clot that normally forms in the empty tooth socket either dislodges prematurely or fails to form altogether. This protective blood clot is vital as it shields the underlying bone and nerve endings from the oral environment. Without it, the bone and nerves are exposed, leading to intense pain.
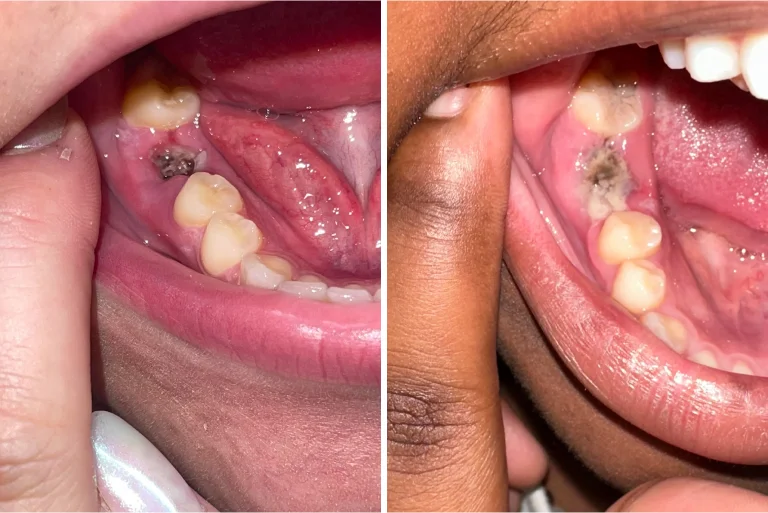
The Appearance of a Dry Socket
Distinguishing a dry socket from a normal, healing extraction site is primarily based on visual cues and the accompanying symptoms. While a dentist will make the definitive diagnosis, recognizing the characteristic signs can empower individuals to seek prompt professional care.
The Empty Socket
The most striking visual characteristic of a dry socket is the appearance of the extraction site itself. Instead of a healthy, pinkish or reddish-red clot filling the socket, a dry socket will appear largely empty or contain a degraded, greyish-brownish mass. The absence of a robust, organized blood clot is the hallmark of this condition. In a typical healing socket, you would expect to see granulation tissue beginning to form, a process that gradually fills the void. This granulation tissue is usually red and healthy-looking. In contrast, a dry socket reveals the raw bone surface of the socket wall.
Exposed Bone and Granulation Tissue
When the protective blood clot is missing, the alveolar bone lining the socket becomes directly exposed. This exposed bone can appear chalky white or a dull grey. In some cases, there might be a small amount of unhealthy-looking, yellowish or greyish granulation tissue present, but it will not be the healthy, vibrant red seen in normal healing. The edges of the socket might also appear more inflamed and irritated than in a typical healing process. It’s important to note that the appearance of exposed bone does not always indicate a dry socket; it can also be a sign of other minor irritants. However, when combined with severe pain, it strongly suggests alveolar osteitis.
Signs of Inflammation
The surrounding gum tissue around the extraction site may also show signs of inflammation. This can manifest as redness, swelling, and tenderness. While some degree of inflammation is normal after an extraction as the body initiates its healing response, excessive or persistent inflammation, particularly when coupled with the other signs of a dry socket, warrants medical attention. The gums might appear more sensitive to touch, and the area may feel warmer than the surrounding tissue.
Accompanying Symptoms of a Dry Socket
While visual inspection is important, the symptoms experienced by the patient are often the most significant indicators of a dry socket. The pain associated with alveolar osteitis is typically severe and distinct from the normal post-operative discomfort.
Severe, Throbbing Pain
The hallmark symptom of a dry socket is intense pain that usually starts two to four days after the extraction, although it can occur sooner or later. This pain is often described as a deep, throbbing ache that can radiate from the socket to other parts of the head and face, including the ear, eye, and temple on the same side. Unlike the manageable post-operative soreness, the pain from a dry socket is often excruciating and can interfere with eating, sleeping, and daily activities. Over-the-counter pain relievers are frequently insufficient to manage this level of discomfort, necessitating stronger prescription medications.
Bad Taste and Odor
Another characteristic symptom of a dry socket is a foul taste in the mouth and a persistent, unpleasant odor emanating from the extraction site. This is due to the decomposition of any lingering food debris or blood clot remnants within the exposed socket, as well as the presence of bacteria. The exposed bone and tissues become a breeding ground for bacteria, leading to the release of volatile compounds that cause the offensive smell and taste. This symptom can be particularly distressing and can contribute to a feeling of general unwellness.
Pain Relief from Nothing
A peculiar and often alarming symptom is that the pain may not be significantly relieved by any of the usual pain management strategies. While pain medication can offer some respite, the discomfort often returns with great intensity shortly after the medication wears off. This lack of sustained relief is a strong indicator that the underlying issue is more than just typical post-operative soreness. The exposed nerve endings are constantly irritated by the oral environment, leading to this persistent and severe pain.
Differentiating from Normal Healing

It is crucial to understand the normal healing process after a wisdom tooth extraction to appreciate how a dry socket deviates from this.
Normal Healing Process
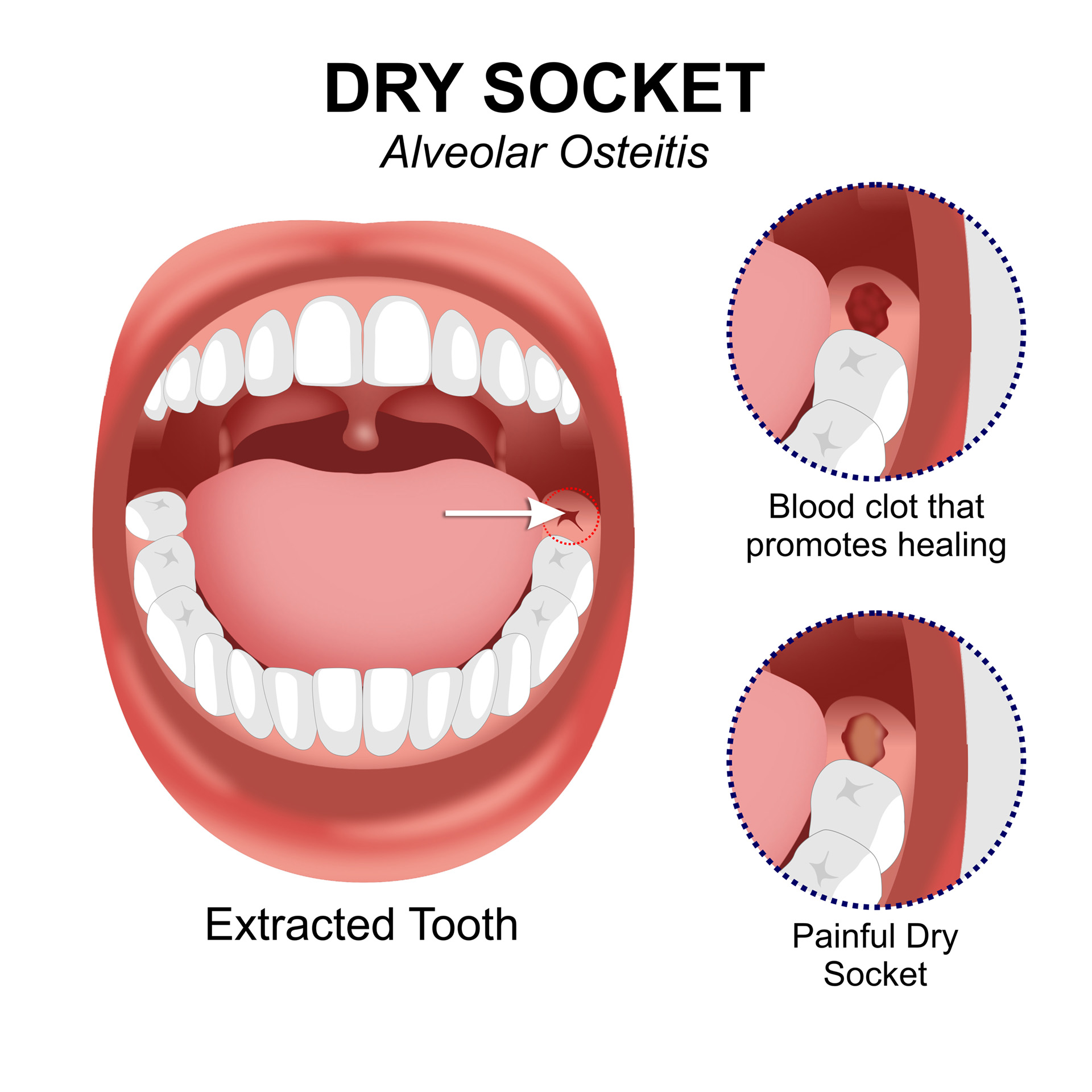
Immediately following a wisdom tooth extraction, a blood clot begins to form within the socket. This clot is dark red and appears to fill the socket. Over the next few days, this clot will gradually change color, becoming lighter red and then pinkish as healthy granulation tissue begins to grow from the bottom and sides of the socket. This tissue is vascular and actively involved in the healing process. The gum tissue around the socket may be slightly inflamed initially but will typically return to normal within a few days. The pain experienced during normal healing is usually manageable with prescribed or over-the-counter pain medication and gradually subsides over time.
Key Differences
The primary distinction lies in the presence and appearance of the blood clot. A normal socket will have a well-formed clot, gradually replaced by pink granulation tissue. A dry socket will be characterized by the absence of a healthy clot, revealing exposed bone and potentially unhealthy-looking debris. The pain is another major differentiator; normal healing involves a manageable level of discomfort that decreases over time, whereas dry socket pain is severe, persistent, and often worsens. The presence of a foul taste and odor is also a significant indicator of alveolar osteitis, as these are not typically associated with normal healing.
Risk Factors and Prevention
While understanding the appearance and symptoms is vital for diagnosis, being aware of the risk factors for dry socket can help in its prevention.
Post-Extraction Care
Adhering strictly to your dentist’s post-operative instructions is paramount in preventing dry socket. This includes:
- Avoiding Disturbing the Socket: Refrain from spitting forcefully, rinsing vigorously, or using straws for at least 24-48 hours after the extraction. These actions can dislodge the delicate blood clot.
- Maintaining Oral Hygiene: Gently brush and floss the areas of your mouth away from the extraction site. Your dentist may recommend a specific antiseptic mouthwash for use after the initial healing period.
- Dietary Considerations: Stick to soft foods for the first few days and avoid chewing directly on the extraction site. Hot liquids and hard, crunchy foods should also be avoided.
Lifestyle Factors
Certain lifestyle choices can increase the risk of developing a dry socket:
- Smoking and Tobacco Use: Nicotine constricts blood vessels, impairing blood flow and the healing process. It also encourages the dislodging of the blood clot. Avoiding smoking for as long as possible after surgery is crucial.
- Oral Contraceptives: Hormonal fluctuations associated with oral contraceptives have been linked to an increased risk of dry socket. It is advisable to discuss this with your dentist if you are taking these medications.
- Previous Dry Socket: If you have experienced a dry socket in the past, you are at a higher risk of developing it again.
Seeking Professional Help
If you suspect you have developed a dry socket, it is essential to contact your dentist or oral surgeon immediately.
Diagnosis and Treatment
A dentist will diagnose a dry socket through a visual examination of the socket and a discussion of your symptoms. Treatment typically involves:
- Cleaning the Socket: The dentist will gently irrigate the socket to remove any debris or food particles.
- Medicated Dressing: A medicated dressing, often containing a soothing agent like eugenol, will be placed into the socket. This dressing helps to protect the exposed bone and relieve pain.
- Pain Management: Prescription pain medication will likely be provided to manage the severe discomfort.
- Follow-up Care: You may need to return to the dentist for regular dressing changes and to monitor the healing process.
The primary goal of treatment is to manage pain and promote healing by protecting the exposed bone and allowing healthy granulation tissue to form. With prompt and appropriate care, the pain associated with dry socket usually subsides within a few days, and the socket will continue to heal. Recognizing what a dry socket wisdom tooth looks like, coupled with an awareness of its associated symptoms, empowers individuals to take swift action, ensuring a smoother and more comfortable recovery after oral surgery.
