The Endocrine System: A Symphony of Hormonal Regulation
The human body is an incredibly complex organism, a marvel of biological engineering that functions through a sophisticated network of systems. Among the most vital of these is the endocrine system, a communication network that governs a vast array of bodily processes through the secretion of hormones. These chemical messengers, produced by specialized glands, travel through the bloodstream to target cells and tissues, influencing everything from growth and metabolism to mood and reproductive function. When this delicate hormonal balance is disrupted, it can lead to a wide spectrum of health conditions, which is precisely where the expertise of an endocrinologist becomes indispensable.
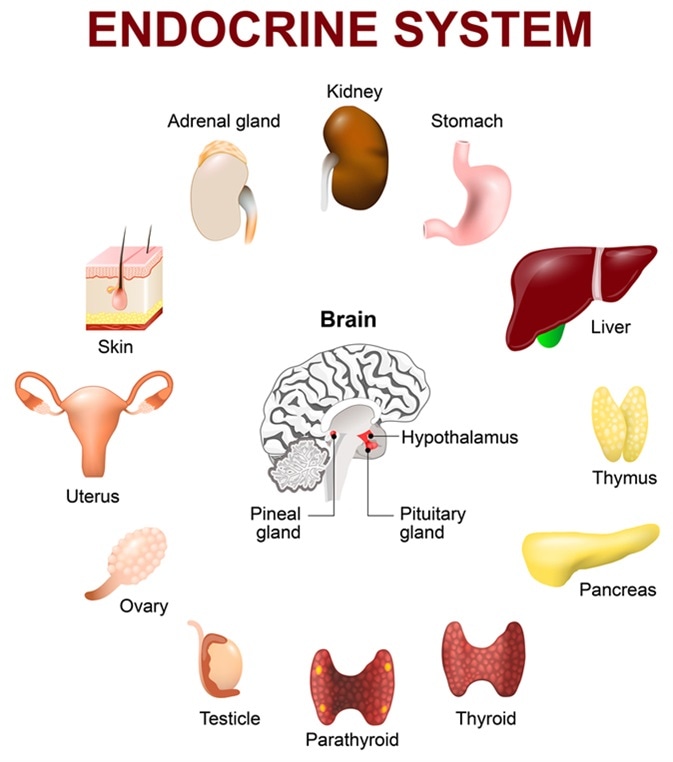
Endocrinologists are medical doctors who specialize in diagnosing and treating diseases and conditions related to the endocrine glands and their hormones. They are the custodians of this intricate hormonal symphony, working to identify the root causes of imbalances and to restore the body to its optimal state of equilibrium. Their practice involves a deep understanding of the interplay between various glands, including the pituitary, thyroid, adrenal glands, pancreas, ovaries, and testes, and how their secretions impact overall health.
The scope of conditions treated by endocrinologists is broad, encompassing both common ailments and rarer disorders. They are frequently consulted for issues related to diabetes, thyroid disorders, osteoporosis, certain reproductive issues, and challenges with growth and metabolism. Their diagnostic toolkit includes a range of laboratory tests, imaging studies, and physical examinations to accurately pinpoint the source of the endocrine dysfunction. Treatment strategies often involve medication, hormone replacement therapy, lifestyle modifications, and sometimes surgical intervention, all tailored to the individual patient’s specific needs.
The Pancreas and Diabetes: A Central Focus
One of the most prevalent conditions managed by endocrinologists is diabetes mellitus. The pancreas, a gland nestled behind the stomach, plays a critical role in regulating blood sugar levels by producing insulin and glucagon. Insulin is a hormone that helps glucose (sugar) from food get into the body’s cells for energy. Glucagon, on the other hand, raises blood glucose levels when they get too low.
Type 1 Diabetes: An Autoimmune Challenge
Type 1 diabetes is an autoimmune condition where the body’s immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. This results in little to no insulin production, leading to dangerously high blood glucose levels. Endocrinologists manage Type 1 diabetes by prescribing insulin therapy, educating patients on blood glucose monitoring, carbohydrate counting, and the importance of a healthy lifestyle. They guide patients through the complexities of managing this chronic condition, aiming to prevent long-term complications such as heart disease, kidney damage, nerve damage, and eye problems.
Type 2 Diabetes: A Multifaceted Approach
Type 2 diabetes, the most common form, develops when the body either doesn’t produce enough insulin or the body’s cells become resistant to insulin’s effects. This resistance, known as insulin resistance, means that glucose cannot easily enter the cells, leading to elevated blood sugar levels. Endocrinologists treat Type 2 diabetes with a multifaceted approach that often begins with lifestyle interventions.
Lifestyle Modifications: The Foundation of Management
Crucial to managing Type 2 diabetes are sustainable lifestyle changes. This includes adopting a balanced diet rich in fruits, vegetables, and whole grains, while limiting processed foods, sugary drinks, and unhealthy fats. Regular physical activity is equally vital, as exercise helps improve insulin sensitivity and can aid in weight management. Endocrinologists work closely with patients to develop personalized nutrition and exercise plans, often referring them to registered dietitians and exercise physiologists for specialized guidance.
Pharmacological Interventions: Beyond Lifestyle
When lifestyle modifications alone are insufficient to control blood glucose levels, endocrinologists introduce pharmacological treatments. These medications work through various mechanisms to lower blood sugar. Metformin is often the first-line drug, helping to reduce glucose production by the liver and improve insulin sensitivity. Other classes of medications include sulfonylureas, DPP-4 inhibitors, GLP-1 receptor agonists, and SGLT2 inhibitors, each with its unique mode of action. In some cases, particularly for individuals with advanced Type 2 diabetes or those who have not achieved adequate control with oral medications, insulin therapy may also be necessary. The endocrinologist meticulously monitors the patient’s response to these medications, adjusting dosages and combinations as needed to achieve target blood glucose levels and minimize the risk of complications.
Thyroid Disorders: Regulating Metabolism and More
The thyroid gland, a small, butterfly-shaped organ located in the front of the neck, produces hormones that regulate metabolism, growth, and development. These hormones, thyroxine (T4) and triiodothyronine (T3), influence nearly every cell in the body. Endocrinologists are experts in diagnosing and treating a range of thyroid conditions that arise when this gland either produces too much or too little of these critical hormones.
Hypothyroidism: An Underactive Thyroid
Hypothyroidism occurs when the thyroid gland doesn’t produce enough thyroid hormones. This can lead to a slowing down of many bodily functions, resulting in symptoms such as fatigue, weight gain, cold intolerance, constipation, dry skin, and hair loss. Common causes include autoimmune diseases like Hashimoto’s thyroiditis, where the immune system attacks the thyroid, and iodine deficiency. Endocrinologists treat hypothyroidism primarily with thyroid hormone replacement therapy, typically with synthetic levothyroxine. The goal is to restore hormone levels to normal, alleviating symptoms and preventing long-term health issues like heart problems and infertility. Regular monitoring of thyroid hormone levels through blood tests is essential to ensure the correct dosage.
Hyperthyroidism: An Overactive Thyroid
Conversely, hyperthyroidism occurs when the thyroid gland produces too much thyroid hormone. This accelerates bodily functions, leading to symptoms like weight loss despite increased appetite, rapid heartbeat, anxiety, tremors, heat intolerance, and frequent bowel movements. Graves’ disease, another autoimmune disorder, is a common cause of hyperthyroidism. Treatment options for hyperthyroidism are varied and depend on the underlying cause and severity of the condition.
Medical Management of Hyperthyroidism
Antithyroid medications, such as methimazole and propylthiouracil, are often prescribed to block the production of excess thyroid hormones. These medications can be highly effective in managing symptoms and restoring normal thyroid function. Endocrinologists carefully monitor patients on these medications for side effects and adjust dosages as needed.
Radioactive Iodine Therapy
Radioactive iodine therapy is another effective treatment for hyperthyroidism. In this procedure, the patient ingests a small dose of radioactive iodine, which is selectively absorbed by the thyroid gland, destroying overactive thyroid cells. While effective, this treatment often leads to permanent hypothyroidism, necessitating lifelong thyroid hormone replacement therapy.
Surgical Intervention
In some cases, particularly when there is a large goiter (enlarged thyroid) causing compression symptoms, or when other treatments are not suitable or effective, thyroid surgery (thyroidectomy) may be recommended. This involves surgically removing part or all of the thyroid gland. As with radioactive iodine therapy, this often results in hypothyroidism, requiring hormone replacement.
Pituitary and Adrenal Disorders: The Master Glands and Stress Response

The pituitary gland, often referred to as the “master gland,” is a small but mighty organ located at the base of the brain. It produces hormones that control many other endocrine glands, including the thyroid, adrenal glands, ovaries, and testes. The adrenal glands, situated atop the kidneys, are responsible for producing hormones like cortisol, adrenaline, and aldosterone, which regulate stress response, metabolism, blood pressure, and electrolyte balance. Endocrinologists treat a variety of conditions stemming from dysfunctions in these crucial glands.
Pituitary Gland Disorders
Disorders of the pituitary gland can manifest in numerous ways, depending on which hormones are affected.
Pituitary Tumors
Many pituitary disorders are caused by benign tumors (adenomas) that can either overproduce or underproduce certain hormones, or by pressing on surrounding tissues, affecting pituitary function. For example, a prolactinoma can lead to excessive prolactin production, causing irregular menstruation, infertility, and galactorrhea (milk production). Cushing’s disease, characterized by excessive cortisol production, is often caused by a pituitary tumor stimulating the adrenal glands. Acromegaly and gigantism, resulting from excess growth hormone, are also linked to pituitary adenomas. Endocrinologists diagnose these conditions through hormone level testing, imaging studies like MRI, and then develop treatment plans that may include medication to control hormone production, surgery to remove the tumor, or radiation therapy.
Pituitary Insufficiency
Conversely, pituitary insufficiency (hypopituitarism) occurs when the pituitary gland doesn’t produce enough of one or more hormones. This can lead to a cascade of downstream hormonal deficiencies, affecting growth, reproduction, thyroid function, and adrenal function. Treatment involves replacing the deficient hormones.
Adrenal Gland Disorders
The adrenal glands are equally critical for maintaining homeostasis, and their dysfunctions can lead to significant health challenges.
Cushing’s Syndrome
Cushing’s syndrome is a condition caused by prolonged exposure to high levels of cortisol. This can be due to the body producing too much cortisol (e.g., from an adrenal tumor or pituitary tumor like in Cushing’s disease) or taking corticosteroid medications. Symptoms include weight gain, particularly in the face and trunk, thinning skin, easy bruising, muscle weakness, high blood pressure, and mood changes. Treatment focuses on reducing cortisol levels, which may involve surgery, radiation, or medication, depending on the cause.
Addison’s Disease
Addison’s disease is a rare but serious condition where the adrenal glands produce too little cortisol and often too little aldosterone. This can lead to fatigue, muscle weakness, weight loss, low blood pressure, and skin darkening. It is typically caused by an autoimmune attack on the adrenal glands. Treatment involves lifelong hormone replacement therapy with corticosteroids and sometimes mineralocorticoids.
Pheochromocytoma
Pheochromocytomas are rare tumors of the adrenal medulla that produce excessive amounts of adrenaline and noradrenaline. This can lead to severe, episodic high blood pressure, headaches, sweating, and palpitations. Surgical removal of the tumor is the primary treatment, often preceded by medication to control blood pressure.
Other Endocrine Conditions and Specialties
Beyond diabetes, thyroid, pituitary, and adrenal disorders, endocrinologists address a variety of other hormonal imbalances and related conditions.
Reproductive Endocrinology
This subspecialty within endocrinology focuses on hormonal issues related to reproduction in both men and women.
Female Reproductive Health
Endocrinologists manage conditions such as Polycystic Ovary Syndrome (PCOS), a common hormonal disorder characterized by irregular periods, excess androgens (male hormones), and ovarian cysts. They also treat infertility when it is caused by hormonal imbalances, menopause-related symptoms, and conditions affecting the ovaries and uterus that have hormonal components.
Male Reproductive Health
In men, endocrinologists address issues like hypogonadism (low testosterone), which can lead to decreased libido, fatigue, loss of muscle mass, and infertility. They also manage conditions related to the testes and the hormones they produce.
Bone Health and Calcium Metabolism
Disorders affecting bone health, such as osteoporosis and Paget’s disease of bone, often have hormonal underpinnings. Endocrinologists manage these conditions, which involve imbalances in calcium, vitamin D, and parathyroid hormone (PTH). The parathyroid glands, four small glands located behind the thyroid, play a crucial role in regulating calcium levels in the blood. Imbalances can lead to hyperparathyroidism (overactive parathyroid glands) or hypoparathyroidism (underactive parathyroid glands), both of which impact bone health and calcium metabolism.

Growth and Development
Endocrinologists also play a vital role in diagnosing and treating disorders of growth and development in children and adults. This includes conditions like growth hormone deficiency, precocious puberty (puberty that begins too early), and delayed puberty.
In conclusion, the field of endocrinology is vast and intricately linked to the overall well-being of an individual. Endocrinologists are essential medical professionals who navigate the complex world of hormones, diagnosing and treating a wide array of conditions that can significantly impact quality of life. Their expertise ensures that the body’s intricate hormonal symphony plays in harmony, promoting health and vitality.
