A cavity, also known as tooth decay, is a common dental problem that occurs when bacteria in your mouth produce acids that erode the enamel of your teeth. This erosion can lead to the formation of a small hole, or cavity, which, if left untreated, can progress deeper into the tooth, potentially causing pain, infection, and tooth loss. Understanding the causes, recognizing the signs, and knowing the appropriate actions to take are crucial for maintaining good oral health and preventing more serious complications.
The Science Behind Tooth Decay
Tooth decay is a complex biological process that involves a dynamic interplay between tooth structure, oral bacteria, and dietary factors. The primary culprits in this process are the microorganisms residing in the oral cavity, predominantly Streptococcus mutans. These bacteria, when exposed to fermentable carbohydrates from our diet – such as sugars and starches – metabolize these substances and produce acids as a byproduct.
The Role of Bacteria and Acids
The enamel, the hard outer layer of our teeth, is primarily composed of hydroxyapatite, a mineral rich in calcium and phosphate. Acids produced by oral bacteria create an environment that favors the demineralization of this mineral structure. This process involves the dissolution of calcium and phosphate ions from the enamel. Simultaneously, saliva plays a vital role in oral homeostasis. It contains minerals that can help to remineralize the enamel, effectively reversing the early stages of demineralization. This constant battle between demineralization and remineralization determines the overall health of the tooth surface.
When the rate of demineralization exceeds the rate of remineralization, a net loss of tooth structure occurs. This is the fundamental mechanism behind cavity formation. The longer teeth are exposed to acids, and the more frequent these exposures are, the greater the potential for enamel breakdown. Factors that can exacerbate this process include poor oral hygiene, a diet high in sugars and acidic foods, and a reduced salivary flow.
Demineralization and Remineralization Cycles
The enamel’s surface is not static; it undergoes continuous cycles of demineralization and remineralization throughout the day. Following the consumption of sugary or starchy foods, bacteria rapidly begin their acid production, lowering the pH in the plaque biofilm. This acidic environment drives the dissolution of enamel minerals. Saliva, when present, buffers these acids and provides calcium and phosphate ions to the tooth surface, facilitating remineralization. Fluoride, found in toothpaste and some water sources, significantly enhances this remineralization process by making the enamel more resistant to acid attacks and promoting the formation of fluorapatite, a more acid-resistant mineral.
However, if the frequency of acid attacks, typically from frequent snacking or sipping on sugary drinks, overwhelms the buffering and remineralizing capacity of saliva, the demineralization process will prevail. Over time, this sustained net demineralization leads to the breakdown of the enamel structure, creating a microscopic void that gradually enlarges into a visible cavity. Understanding these cycles highlights the importance of not only brushing and flossing but also managing dietary habits to minimize prolonged acid exposure.
Recognizing the Signs and Symptoms of a Cavity
Early detection of cavities is key to simpler and more effective treatment. While some cavities may not present any noticeable symptoms in their initial stages, others can manifest in various ways. Being aware of these signs allows for prompt professional assessment and intervention.
Initial Stages: No Apparent Symptoms
In the earliest stages of enamel demineralization, the damage might be so superficial that it is not visually apparent and does not cause any discomfort. This is often referred to as a “white spot lesion.” At this point, with proper oral hygiene, a fluoride-rich toothpaste, and potentially a dentist’s intervention with a fluoride treatment, the demineralized area can be successfully remineralized, and the cavity formation can be reversed. This emphasizes the importance of regular dental check-ups, even when you don’t feel any pain or see any visible issues. Dentists use specialized tools and examinations to identify these early signs that might be missed by the untrained eye.
Developing Symptoms: What to Look For
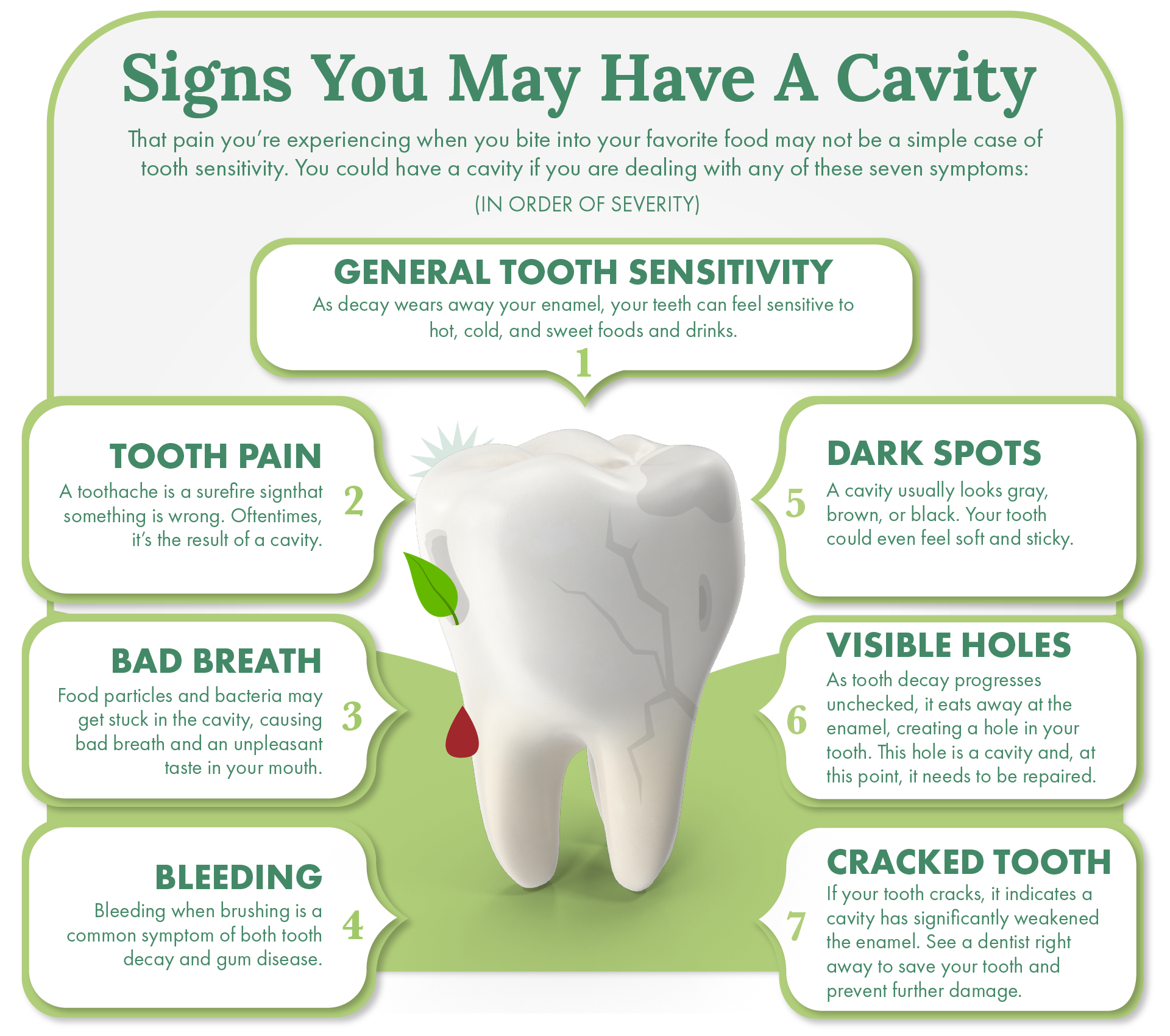
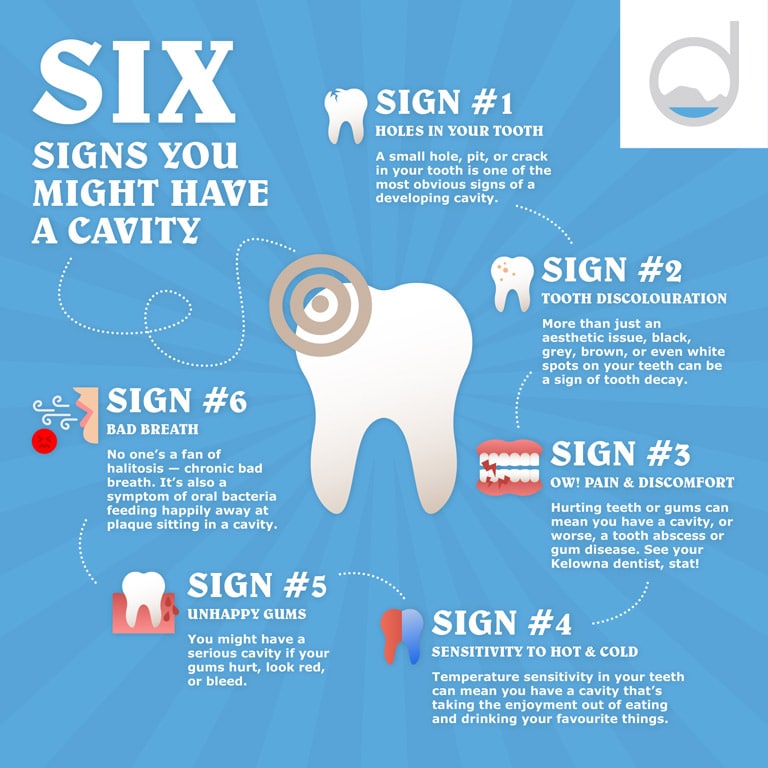
As a cavity progresses and erodes deeper into the enamel and potentially into the dentin (the layer beneath the enamel), symptoms may begin to emerge. These can include:
- Tooth Sensitivity: A common symptom is increased sensitivity to hot, cold, sweet, or even acidic foods and beverages. This sensitivity arises because the protective enamel layer has been compromised, allowing stimuli to reach the sensitive dentin and nerve endings within the tooth. The sensation is often described as a sharp, fleeting pain.
- Visible Holes or Pits: You might notice a dark spot, a visible hole, or a pit on the surface of your tooth. These can be particularly evident on the chewing surfaces of molars or between teeth.
- Pain When Biting Down: As the decay reaches deeper into the tooth, it can cause pain or discomfort when you bite down, especially if food gets lodged in the cavity.
- Toothache: A persistent or throbbing toothache can indicate that the decay has reached the pulp (the innermost part of the tooth) and may have led to inflammation or infection. This pain can range from mild to severe and may worsen at night or when lying down.
- Bad Breath or a Bad Taste: Bacteria accumulating in a cavity can produce foul-smelling gases, leading to persistent bad breath (halitosis) or an unpleasant taste in your mouth that doesn’t go away with brushing.
It is important to note that the absence of pain does not mean a cavity is not present. Regular dental examinations are the most reliable way to detect decay before it causes significant discomfort or irreversible damage.
Taking Action: When to See a Dentist
The definitive answer to “what do you do if you have a cavity” is to seek professional dental care. Self-treatment is not an option for established cavities, and delaying professional intervention can lead to more complex and costly treatments.
The Importance of Professional Diagnosis
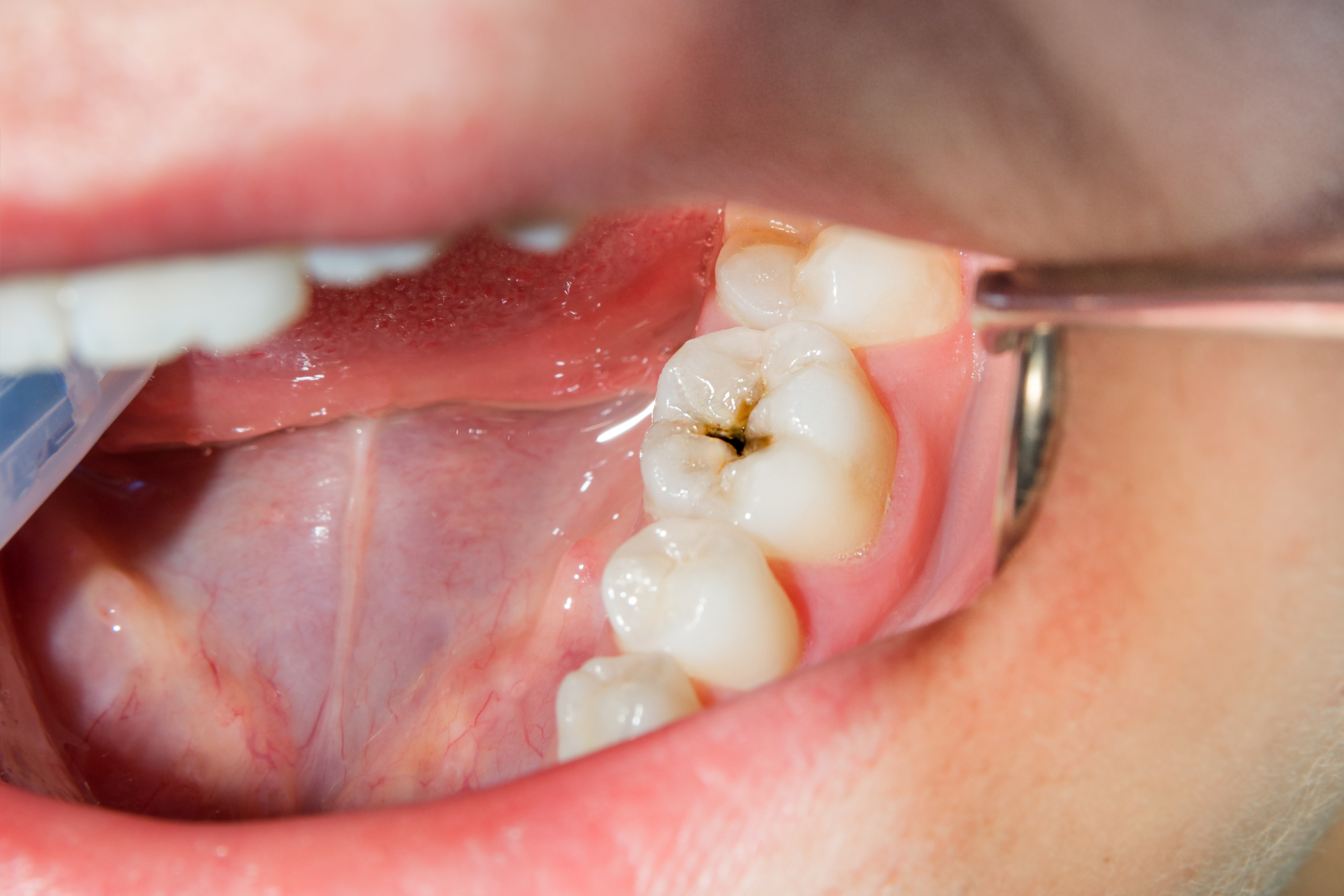
If you suspect you have a cavity, or if you experience any of the symptoms mentioned, the most crucial step is to schedule an appointment with your dentist. Dentists are equipped with the knowledge, tools, and diagnostic techniques to accurately identify the presence, extent, and location of tooth decay. This typically involves:
- Visual Examination: The dentist will carefully examine all surfaces of your teeth, looking for any signs of discoloration, pits, or holes.
- Dental Explorer: A sharp, pointed instrument called a dental explorer is used to gently probe the tooth surface. It can detect soft spots that indicate demineralization or a cavity.
- Dental X-rays: Radiographs (X-rays) are essential for detecting cavities that are not visible to the naked eye, particularly those located between teeth or beneath existing fillings. They can also reveal the depth of the decay and whether it has reached the pulp.
Based on the diagnosis, the dentist will recommend the most appropriate treatment plan.
Treatment Options for Cavities
The treatment for a cavity depends on its size and depth. Common treatment options include:
- Fillings: This is the most common treatment for cavities. After removing the decayed portion of the tooth, the dentist will fill the cavity with a dental restorative material, such as composite resin (tooth-colored) or amalgam (silver-colored). This restores the tooth’s shape and function and prevents further decay.
- Dental Crowns: For larger cavities that have significantly weakened the tooth structure, a dental crown may be necessary. A crown is a tooth-shaped cap that is cemented over the damaged tooth, providing strength, protection, and an improved appearance.
- Root Canal Therapy: If the decay has reached the pulp of the tooth, causing inflammation or infection, a root canal procedure may be required. This involves removing the infected pulp, cleaning and shaping the inside of the tooth, and then filling and sealing it. A crown is typically placed on the tooth after a root canal.
- Tooth Extraction: In severe cases where the tooth is too damaged to be saved, extraction may be the only option. This is usually a last resort, and the dentist will discuss replacement options, such as dental implants or bridges, to restore your bite and prevent surrounding teeth from shifting.
Prevention: The Best Defense Against Cavities
While treating cavities is essential, the most effective strategy is to prevent them from forming in the first place. Adopting good oral hygiene habits and making informed lifestyle choices can significantly reduce your risk of developing tooth decay.
Maintaining Excellent Oral Hygiene
Regular and proper brushing and flossing are the cornerstones of cavity prevention.
- Brushing: Brush your teeth at least twice a day for two minutes each time, using a fluoride toothpaste. Ensure you brush all surfaces of your teeth – outer, inner, and chewing surfaces. Consider using an antimicrobial mouthwash to further reduce bacteria.
- Flossing: Floss daily to remove food particles and plaque from between your teeth and under the gum line, areas that your toothbrush cannot reach. This is crucial as cavities often start between teeth.
Dietary Modifications for Oral Health
Your diet plays a pivotal role in cavity formation.
- Limit Sugary and Starchy Foods: Reduce your intake of sugary drinks (soda, fruit juices), candies, cookies, and refined carbohydrates. These foods provide a readily available food source for cavity-causing bacteria.
- Choose Tooth-Friendly Snacks: Opt for healthier snack alternatives such as fresh fruits, vegetables, cheese, and nuts.
- Hydration is Key: Drinking plenty of water, especially fluoridated water, helps to wash away food particles and neutralize acids in the mouth. It also supports saliva production, which is essential for remineralization.
The Role of Fluoride
Fluoride is a natural mineral that strengthens tooth enamel and makes it more resistant to acid attacks.
- Fluoride Toothpaste: Using a fluoride toothpaste is one of the most effective ways to incorporate fluoride into your daily oral hygiene routine.
- Fluoridated Water: Drinking tap water in communities with fluoridation programs provides a systemic source of fluoride that benefits teeth throughout their development and life.
- Professional Fluoride Treatments: Your dentist may recommend professional fluoride treatments, especially if you are at a higher risk for cavities. These treatments involve applying a concentrated fluoride solution directly to your teeth.
Regular Dental Check-ups
Routine dental check-ups are not just for treating problems; they are a crucial part of prevention. Your dentist can:
- Detect Early Signs: Identify early signs of demineralization or cavities that you might not be able to see or feel.
- Provide Professional Cleanings: Remove plaque and tartar that can lead to decay and gum disease.
- Offer Preventive Advice: Provide personalized advice on your oral hygiene routine and dietary habits to minimize your risk.
- Apply Sealants: In some cases, dental sealants can be applied to the chewing surfaces of molars to create a barrier against food particles and bacteria, further preventing cavities.
By understanding the causes, recognizing the signs, and taking proactive steps towards prevention and timely treatment, you can effectively manage and avoid the discomfort and complications associated with cavities, ensuring a healthier smile for years to come.
