The quest for the most effective and user-friendly tympanostomy system is a perpetual endeavor within the otolaryngology field. Tympanostomy tubes, commonly known as ear tubes, play a critical role in managing recurrent otitis media, otitis media with effusion, and ventilating the middle ear space. The “leading” system isn’t merely about a single product but encompasses a confluence of design innovation, material science, ease of insertion, patient comfort, and long-term efficacy. Evaluating the current market landscape reveals a dynamic environment where established players continually refine their offerings, while new technologies emerge to address specific challenges and improve outcomes.
![]()
Advancements in Tympanostomy Tube Design and Materials
The evolution of tympanostomy tubes has moved beyond simple cylindrical conduits. Modern systems are designed with a sophisticated understanding of middle ear anatomy and the body’s biological response.
Material Innovation for Enhanced Biocompatibility and Retention
The materials used in tympanostomy tubes are paramount to their success. Historically, metal and glass were employed, but the advent of plastics and polymers revolutionized the field. Today, the leading systems often feature materials that balance rigidity for insertion with flexibility to minimize patient discomfort and the risk of extrusion.
- Silicone: Medical-grade silicone remains a dominant material due to its excellent biocompatibility, flexibility, and inertness. It is less likely to cause inflammatory reactions and can be molded into various shapes. Silicone tubes are often favored for longer-term ventilation, as they tend to be softer and less prone to migration or extrusion.
- Teflon (PTFE): Polytetrafluoroethylene (PTFE), commonly known as Teflon, offers a smooth surface that reduces tissue adhesion and biofilm formation, potentially decreasing the risk of infection. Its inherent lubricity aids in insertion and removal.
- Titanium: While less common for standard tubes, titanium alloys are sometimes used for specialized applications or for patients with allergies to plastics. Their strength and biocompatibility are well-established.
The selection of material directly impacts the tube’s surface characteristics, its ability to resist biofouling, and its overall longevity within the middle ear. Leading systems are exploring novel coatings and surface treatments to further enhance these properties, aiming to reduce the incidence of otorrhea (discharge) and the need for premature replacement.
Anatomically Inspired Shapes for Improved Efficacy
Beyond material, the shape of the tympanostomy tube has seen significant refinement. The goal is to ensure proper placement and sustained ventilation while minimizing trauma to the tympanic membrane.
- “T” or “Shah” Tubes: These are perhaps the most recognizable and widely used designs. The “T” shape, with its flanges, provides excellent retention within the tympanic membrane, reducing the likelihood of accidental extrusion. Variations exist in the diameter of the lumen, the length of the arms, and the angle of the flanges to accommodate different anatomical variations.
- “Collar Button” or “Shepard” Tubes: These tubes feature a larger flange on one side and a narrower shaft, designed to rest within the external auditory canal, while the larger portion sits flush against the tympanic membrane. This design can offer good stability.
- “Short-Term” vs. “Long-Term” Tubes: The distinction is often in the design and material. Short-term tubes, often made of slightly more rigid materials, are designed for temporary ventilation (e.g., following acute otitis media), while long-term tubes, typically made of softer silicone, are intended for prolonged use in cases of chronic effusion or Eustachian tube dysfunction.
- “Grommets”: These are typically short, cylindrical tubes with no retaining flanges. They are primarily used for very short-term ventilation, often during procedures like myringotomy for drainage.
The leading systems often offer a range of these designs and sizes, allowing surgeons to select the most appropriate tube based on the patient’s age, the specific clinical indication, and the anatomy of their tympanic membrane. The subtle differences in flange size, tube diameter, and overall length can significantly impact retention and the potential for discomfort or TM perforation.
The Insertion Process: Tools and Techniques
The effectiveness of a tympanostomy system is intrinsically linked to the ease and safety of its insertion. Innovations in insertion instruments and techniques have made the procedure less invasive and more efficient.
Minimally Invasive Insertion Instruments
The traditional method of myringotomy followed by manual insertion of a tube has been augmented by specialized instruments designed for quicker and more precise placement.
- Myringotomy Knives: While sharp blades are still used, many systems incorporate integrated knives or lancets that create a precise incision in the tympanic membrane, often in a specific location to optimize tube placement and healing.
- Tube Insertion Forceps: These specialized forceps are designed to grasp the tube securely and deliver it through the myringotomy incision with minimal manipulation of the tympanic membrane. Some designs feature atraumatic tips to prevent damage.
- “Click” or “Pneumatic” Injectors: These devices offer a more automated approach. The tube is pre-loaded into the injector, and a spring-loaded mechanism or controlled air pressure is used to deploy the tube rapidly into the tympanic membrane. These can be particularly useful in pediatric cases where patient movement is a concern.
- Pre-loaded Systems: The most advanced systems often come with tubes pre-loaded onto an applicator or injector. This significantly reduces preparation time in the operating room and minimizes the risk of contamination of the tube before insertion.
The leading tympanostomy systems prioritize designs that facilitate a smooth and rapid insertion, thereby reducing operative time and the potential for patient discomfort or complications. The reliability and ease of use of the insertion tools are as critical as the design of the tube itself.
The Role of Visualization and Guidance
While not always integrated into the tube system itself, advances in visualization and guidance during the insertion process significantly contribute to the overall success.
- High-Definition Otoscopes and Microscopes: Improved magnification and illumination allow surgeons to better visualize the tympanic membrane and precisely target the incision.
- Endoscopic Approaches: In certain complex cases or for revision surgeries, endoscopic visualization provides an alternative view of the middle ear and tympanic membrane, allowing for more precise tube placement.
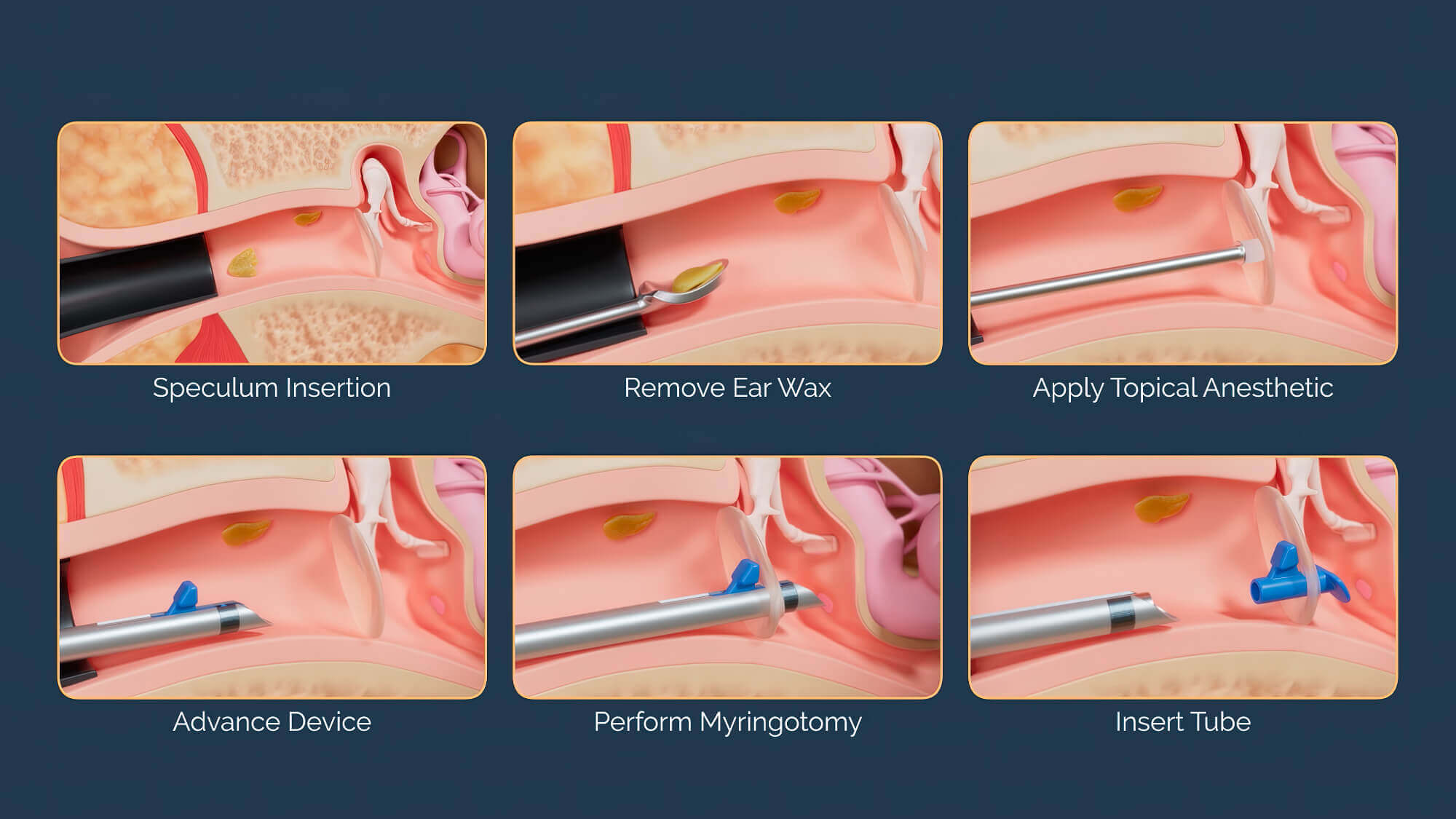
The synergy between an optimized tube design, intuitive insertion instruments, and superior visualization techniques defines the cutting edge of tympanostomy systems.
Patient Outcomes and Clinical Efficacy
Ultimately, the measure of a “leading” tympanostomy system lies in its ability to achieve positive patient outcomes. This includes effective ventilation, reduced recurrence of infections, and minimized complications.
Sustained Ventilation and Patency Rates
The primary goal of tympanostomy tube insertion is to ventilate the middle ear space. The leading systems are designed to maintain patency for the intended duration.
- Reduced Occlusion: The materials and surface properties of advanced tubes are engineered to resist mucus and tissue ingrowth, which can lead to occlusion.
- Adequate Lumen Size: The internal diameter of the tube is crucial for effective airflow. Leading systems offer a range of lumen sizes to accommodate different needs.
- Retention: A well-designed tube that remains securely in place ensures continuous ventilation. Premature extrusion or migration can compromise the treatment’s effectiveness.
Clinical studies and surgeon experience consistently highlight the importance of a system that reliably maintains its position and its open lumen.
Minimizing Complications and Promoting Healing
Beyond ventilation, the leading systems are associated with lower rates of complications.
- Otorrhea: While difficult to completely eliminate, innovative materials and surface treatments aim to reduce bacterial adherence and biofilm formation, thereby lowering the incidence of post-operative discharge.
- Tympanic Membrane Perforation: The design of the tube and the insertion technique are critical in minimizing the risk of causing or enlarging perforations.
- Granulation Tissue Formation: Some materials and designs are less likely to incite the formation of granulation tissue around the tube, which can impede ventilation or lead to bleeding.
- Tinnitus and Vertigo: While rare, certain tube designs or materials might theoretically influence these symptoms. Leading systems are generally chosen to minimize such risks.
The selection of a tympanostomy system often involves a consideration of the surgeon’s experience, the patient’s specific anatomical and pathological factors, and the reported efficacy and safety profiles of different products.
The Future of Tympanostomy Systems
The field of otolaryngology is continually seeking improvements in managing middle ear pathologies. The future of tympanostomy systems likely involves further integration of technology and novel approaches.
Smart Tubes and Drug Delivery
One exciting avenue is the development of “smart” tympanostomy tubes capable of delivering therapeutic agents directly to the middle ear.
- Antibiotic and Steroid Eluting Tubes: Impregnating tubes with antibiotics or steroids could provide targeted, sustained drug delivery to combat infection and inflammation, potentially reducing the need for systemic medications and minimizing resistance.
- Biosensors: Future iterations might incorporate biosensors to monitor middle ear pressure, pH, or the presence of inflammatory markers, providing real-time data to clinicians and potentially enabling personalized treatment adjustments.
Biodegradable and Resorbable Materials
The development of biodegradable or resorbable tympanostomy tubes could offer significant advantages.
- Elimination of Removal Procedures: For short-term ventilation needs, tubes that naturally dissolve or resorb over time would eliminate the need for a subsequent surgical procedure to remove them, reducing costs and patient burden.
- Controlled Dissolution: Research into materials that can be engineered to resorb over a predictable timeframe would be a major breakthrough.

Patient-Centric Designs
As the focus on patient experience intensifies, tympanostomy systems will likely evolve to be even more comfortable and less disruptive to daily life. This could involve novel bio-adhesives, less invasive insertion methods, and materials that are virtually imperceptible to the patient.
In conclusion, identifying the “leading” tympanostomy system is a multifaceted assessment. It requires a comprehensive understanding of the materials used, the innovative designs that ensure proper placement and efficacy, the advancements in insertion technology that prioritize safety and efficiency, and ultimately, the clinical evidence demonstrating superior patient outcomes. The ongoing innovation in this critical area of otolaryngology promises even more sophisticated and patient-friendly solutions in the years to come.
