While the terms “food poisoning” and “gastroenteritis” are often used interchangeably in everyday conversation, especially when referring to a sudden onset of stomach upset after consuming contaminated food or water, there are distinct differences in their meaning, origin, and scope. Understanding these distinctions is crucial for accurate diagnosis, appropriate treatment, and effective public health measures. At its core, the difference lies in cause and effect, and the broader implications of each condition.
Understanding the Nuances of Gastroenteritis
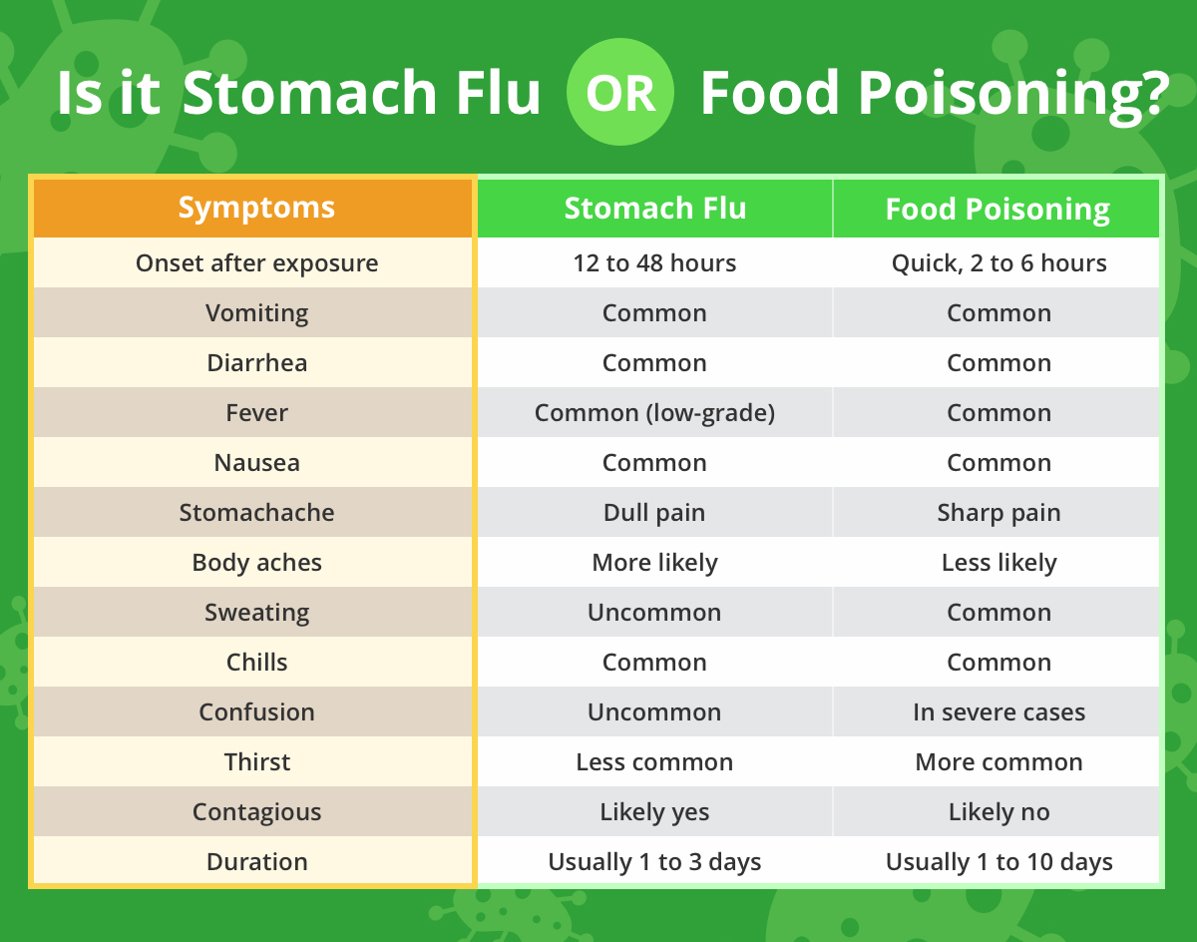
Gastroenteritis, often colloquially referred to as the “stomach flu” (though it has no relation to influenza), is a general term describing inflammation of the gastrointestinal tract, primarily the stomach and intestines. This inflammation can be caused by a variety of infectious agents, including viruses, bacteria, parasites, and even chemical irritants. Gastroenteritis is a broad umbrella term, and food poisoning is a specific subset of it.
Viral Gastroenteritis: The Most Common Culprit
Viral gastroenteritis is by far the most common cause of gastroenteritis worldwide. Several types of viruses can lead to this condition, with norovirus and rotavirus being the most prevalent. Norovirus is highly contagious and responsible for outbreaks in various settings, from cruise ships to schools. Rotavirus, while less common in adults due to vaccination, is a significant cause of severe diarrhea in infants and young children.
- Norovirus: Known for its rapid onset and highly contagious nature, norovirus infections typically manifest with sudden vomiting, diarrhea, nausea, and stomach cramps. Fever, headache, and muscle aches can also occur. Symptoms usually appear within 12 to 48 hours of exposure and last for one to three days.
- Rotavirus: This virus is a leading cause of severe diarrheal disease in infants and young children. Symptoms include watery diarrhea, vomiting, fever, and abdominal pain. Dehydration is a significant concern with rotavirus infections, particularly in young children who are more vulnerable. Vaccination programs have significantly reduced the incidence of severe rotavirus illness in many countries.
- Other Viruses: Adenoviruses and astroviruses are other viral pathogens that can cause gastroenteritis, generally leading to less severe symptoms compared to norovirus and rotavirus.
Viral gastroenteritis is typically spread through the fecal-oral route, meaning the virus is shed in the feces of an infected person and can be ingested by another person through contaminated hands, food, or water. Poor hygiene practices, such as not washing hands thoroughly after using the restroom or before preparing food, are major contributors to its spread.
Bacterial Gastroenteritis: Beyond Simple Upset
Bacterial gastroenteritis is also a significant cause of illness, often linked to contaminated food or water. While symptoms can overlap with viral gastroenteritis, bacterial infections can sometimes be more severe and may require specific medical treatment, such as antibiotics, depending on the causative agent.
- Salmonella: A common bacterial culprit, Salmonella is often associated with undercooked poultry, eggs, and contaminated produce. Symptoms include diarrhea (which can be bloody), fever, and abdominal cramps. In severe cases, Salmonella can spread beyond the intestines, leading to life-threatening infections.
- E. coli (Escherichia coli): Certain strains of E. coli, particularly Shiga toxin-producing E. coli (STEC) such as E. coli O157:H7, can cause severe illness. These strains are often linked to contaminated beef, unpasteurized milk, and contaminated water. Symptoms include severe stomach cramps, diarrhea (often bloody), and vomiting. Some individuals, especially young children and the elderly, can develop a serious complication called hemolytic uremic syndrome (HUS), which can lead to kidney failure.
- Campylobacter: This is one of the most common bacterial causes of diarrheal illness globally, frequently associated with undercooked poultry. Symptoms include diarrhea (often bloody), fever, and abdominal cramps. While most people recover without specific treatment, complications can arise in rare cases.
- Shigella: Known for causing dysentery, Shigella infections result in frequent, small stools that may contain mucus and blood, along with fever and abdominal pain. It is highly contagious and spreads easily through contaminated food and water.
Bacterial gastroenteritis is primarily contracted through the ingestion of food or water contaminated with the bacteria. This contamination can occur at various stages, from farming and processing to preparation and serving. Thorough cooking of food and proper food handling practices are essential for prevention.
Parasitic Gastroenteritis: Less Common but Potentially Persistent
Parasitic gastroenteritis is less common in developed countries but can be a significant issue in regions with poor sanitation. Parasites, such as Giardia and Cryptosporidium, can infect the intestines and cause prolonged diarrhea and other gastrointestinal symptoms.
- Giardia: Giardia lamblia is a common parasite found in contaminated water sources, including lakes, streams, and swimming pools. It can also be spread through contaminated food or person-to-person contact. Symptoms include diarrhea, gas, greasy stools, stomach cramps, nausea, and dehydration.
- Cryptosporidium: This parasite is another common cause of waterborne illness. Cryptosporidium can survive in chlorinated water, making it challenging to eradicate. Symptoms are similar to Giardia, including watery diarrhea, stomach cramps, nausea, vomiting, and fever. Individuals with weakened immune systems are particularly vulnerable to severe and prolonged cryptosporidiosis.
Parasitic gastroenteritis is often acquired by drinking contaminated water or swimming in contaminated recreational waters. It can also be transmitted through contaminated food or by direct contact with an infected person or animal.
Delving into Food Poisoning: A Specific Pathway to Illness
Food poisoning, also known as foodborne illness, is a specific type of gastroenteritis that is directly caused by consuming food or beverages contaminated with harmful bacteria, viruses, parasites, or toxins. Therefore, all food poisoning is a form of gastroenteritis, but not all gastroenteritis is food poisoning. The key differentiator is the vehicle of transmission: the contaminated food or drink.
The Role of Pathogens and Toxins in Food
The contamination of food can occur through various pathways. In the case of bacterial food poisoning, the bacteria themselves can be present in the food, or they can multiply and produce toxins within the food, particularly if it is not stored or cooked properly.
- Bacterial Contamination: As mentioned in the context of bacterial gastroenteritis, pathogens like Salmonella, E. coli, and Campylobacter can contaminate raw ingredients. If these ingredients are not cooked to a sufficient temperature, the bacteria can survive and cause illness when ingested. Improper handling, such as cross-contamination from raw meats to ready-to-eat foods, is another common route.
- Bacterial Toxins: Some bacteria, like Staphylococcus aureus and Clostridium perfringens, produce toxins in food. These toxins can cause illness even if the bacteria themselves are no longer alive. Staphylococcus aureus toxins are often produced when food is left at room temperature for extended periods, allowing the bacteria to multiply and secrete their potent toxins. Clostridium perfringens typically contaminates meat and poultry and can produce toxins if the food is not kept hot enough after cooking.
- Viral Contamination: Viruses, such as norovirus, can contaminate food through infected food handlers who do not practice proper hygiene. Raw or undercooked shellfish from contaminated waters can also be a source of viral food poisoning.
- Parasitic Contamination: Parasites can contaminate food through contaminated water used for irrigation or washing produce, or through improper handling by infected individuals. Undercooked meat can also harbor parasites.
The onset and severity of food poisoning symptoms can vary depending on the specific pathogen or toxin involved, the amount consumed, and the individual’s overall health. Symptoms typically include nausea, vomiting, diarrhea, abdominal pain, and fever.
Differentiating Causes: The Core Distinction
The fundamental difference between food poisoning and gastroenteritis lies in the direct cause and route of infection.
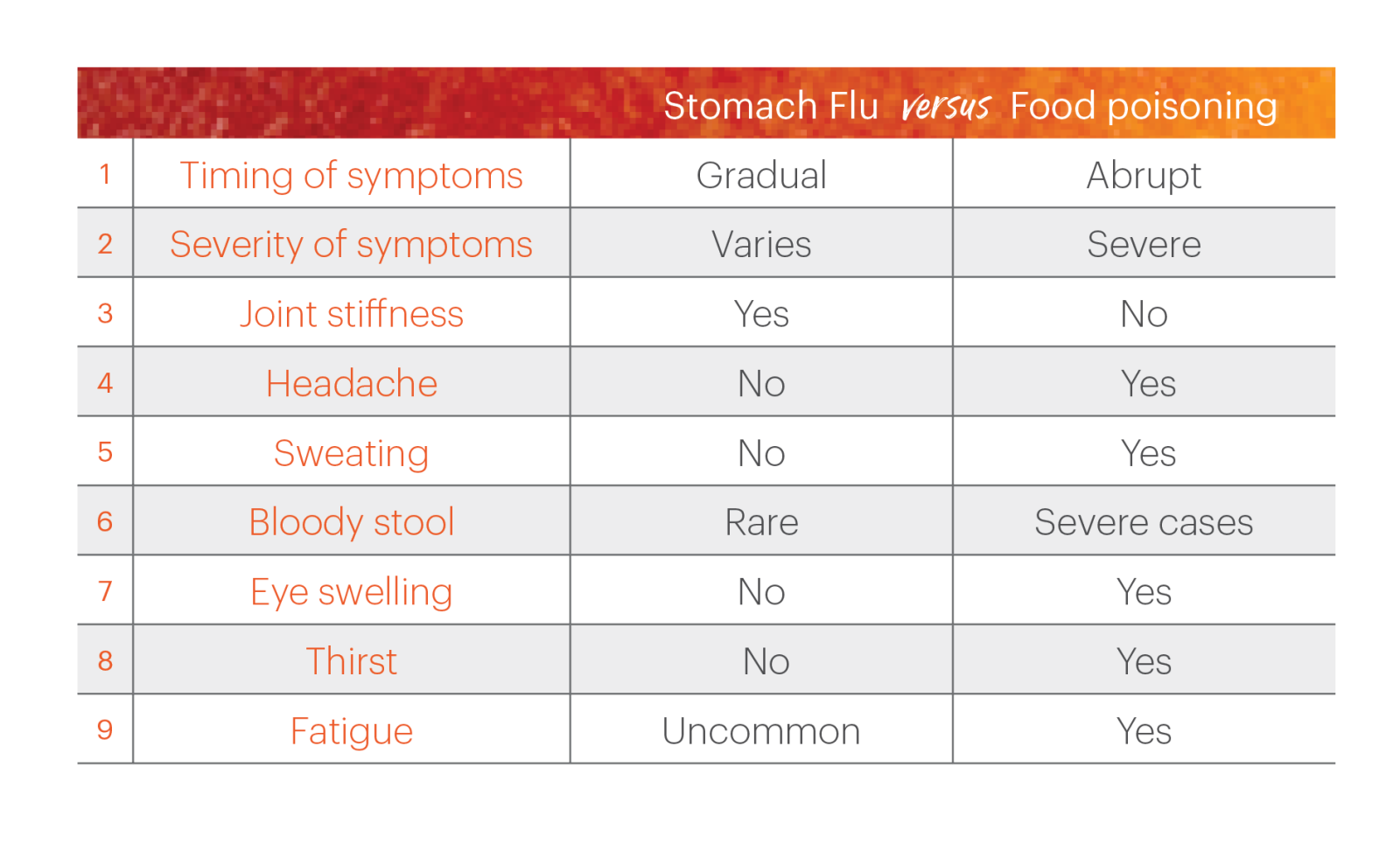
- Gastroenteritis is a broader term for inflammation of the stomach and intestines, and it can be caused by a wide array of infectious agents, including viruses, bacteria, and parasites, transmitted through various means (fecal-oral, contaminated water, person-to-person contact).
- Food Poisoning is a specific type of gastroenteritis that is caused by consuming contaminated food or beverages. The pathogen or toxin is ingested through the food item, leading to the inflammation and symptoms.
For example, if you contract norovirus from a sick family member through close contact, it is viral gastroenteritis. However, if you contract norovirus by eating contaminated oysters, it is food poisoning (and also viral gastroenteritis). Similarly, while many bacterial infections causing gastroenteritis are foodborne, some can be contracted through other means, such as contaminated water sources not directly related to food consumption.
Symptoms, Diagnosis, and Treatment: Navigating the Similarities and Differences
While the underlying causes and transmission routes differ, the symptoms of food poisoning and other forms of gastroenteritis often overlap significantly, making diagnosis challenging without medical expertise.
Overlapping Symptoms: The Common Presentation
The hallmark symptoms of both food poisoning and gastroenteritis are related to the disruption of the gastrointestinal system. These commonly include:
- Nausea: A feeling of sickness in the stomach, often preceding vomiting.
- Vomiting: The forceful expulsion of stomach contents.
- Diarrhea: Loose, watery stools, which can range from mild to severe.
- Abdominal Cramps and Pain: Discomfort and spasms in the stomach area.
- Fever: An elevated body temperature, often accompanying infections.
- Headache and Muscle Aches: General feelings of malaise.
The onset and duration of these symptoms can vary greatly. Viral gastroenteritis often has a rapid onset and is typically short-lived, resolving within a few days. Bacterial food poisoning can have a longer incubation period, with symptoms appearing hours or even days after consumption, and can sometimes be more severe and prolonged. Parasitic infections tend to have the longest incubation periods and can cause chronic or recurring symptoms.
Diagnostic Approaches: Uncovering the Cause
Diagnosing the specific cause of gastrointestinal distress often relies on a combination of patient history, physical examination, and laboratory testing.
- Medical History: A healthcare provider will inquire about the onset of symptoms, their nature, any recent travel, consumption of specific foods or water, and potential exposure to sick individuals. For suspected food poisoning, detailed questions about recent meals are crucial.
- Physical Examination: This typically involves assessing for signs of dehydration, tenderness in the abdomen, and overall well-being.
- Stool Tests: Stool samples can be sent to a laboratory to identify the presence of specific bacteria, viruses, or parasites. This is often the most definitive way to distinguish between different types of gastroenteritis and confirm food poisoning.
- Blood Tests: In some cases, blood tests may be used to check for signs of infection or dehydration.
The primary goal of diagnosis is to determine if the cause is viral, bacterial, parasitic, or toxin-mediated, as this will guide treatment decisions.
Treatment Strategies: Supportive Care and Targeted Interventions
For most cases of mild to moderate gastroenteritis, including food poisoning, the primary treatment focuses on supportive care to help the body recover and prevent dehydration.
- Hydration: This is paramount. Consuming plenty of clear fluids like water, oral rehydration solutions (ORS), broths, and diluted juices is essential to replace fluids lost through vomiting and diarrhea. Electrolyte-rich drinks can be particularly beneficial.
- Rest: Allowing the body to rest aids in recovery.
- Dietary Modifications: A bland diet is often recommended. Starting with clear liquids and gradually introducing soft, easily digestible foods like toast, crackers, rice, and bananas can help. Avoiding dairy products, fatty foods, spicy foods, and caffeine is generally advised during the initial stages.
- Medications: Over-the-counter anti-diarrheal medications may be used cautiously in adults, but it’s important to consult a healthcare provider, as they can sometimes prolong certain bacterial infections. Medications to relieve nausea and vomiting may also be prescribed.
- Antibiotics: Antibiotics are only effective against bacterial infections and are not helpful for viral gastroenteritis or toxin-mediated food poisoning. They are prescribed only when a specific bacterial pathogen requiring such treatment is identified and deemed necessary by a healthcare professional.
- Hospitalization: In severe cases, particularly with significant dehydration, hospitalization may be necessary to administer intravenous fluids and provide more intensive care.
The distinction between food poisoning and other causes of gastroenteritis becomes most critical when specific treatments are required. For instance, identifying a bacterial pathogen like E. coli O157:H7 might necessitate close monitoring for HUS, while a viral infection would be managed purely with supportive care.
Prevention: Safeguarding Against Both Threats
Preventing both food poisoning and other forms of gastroenteritis hinges on robust hygiene practices and safe food handling. Since food poisoning is a subset of gastroenteritis, many preventative measures are universally applicable.
Personal Hygiene: The First Line of Defense
Maintaining excellent personal hygiene is fundamental in preventing the spread of infectious agents.
- Handwashing: This is the single most effective way to prevent the transmission of many pathogens. Wash hands thoroughly with soap and water for at least 20 seconds, especially after using the restroom, before eating or preparing food, and after coughing or sneezing.
- Sanitation: Maintaining clean living environments and regularly disinfecting surfaces, particularly in kitchens and bathrooms, can reduce the risk of contamination.
- Safe Water Consumption: Drink clean, treated water, especially when traveling to areas where water quality may be questionable. Avoid swallowing water when swimming in lakes, rivers, or pools.

Food Safety Practices: Critical for Avoiding Food Poisoning
Given that food poisoning is directly linked to contaminated food, specific food safety practices are paramount.
- Cook Food Thoroughly: Ensure meats, poultry, eggs, and seafood are cooked to their recommended internal temperatures to kill harmful bacteria and parasites. Use a food thermometer to verify.
- Prevent Cross-Contamination: Keep raw meats, poultry, seafood, and eggs separate from ready-to-eat foods during preparation, storage, and serving. Use separate cutting boards and utensils for raw and cooked foods.
- Refrigerate Promptly: Refrigerate perishable foods within two hours of cooking or purchasing. Keep refrigerators at or below 40°F (4°C) and freezers at or below 0°F (-18°C).
- Wash Produce: Rinse fresh fruits and vegetables under running water before eating, cutting, or cooking them, even if you plan to peel them.
- Be Mindful of High-Risk Foods: Certain foods, such as raw sprouts, unpasteurized milk and juices, and raw or undercooked shellfish, carry a higher risk of contamination. Pregnant women, young children, older adults, and individuals with weakened immune systems should be particularly cautious with these items.
- Avoid Risky Food Preparation: Do not prepare food for others if you are experiencing vomiting or diarrhea.
By understanding the differences between food poisoning and the broader category of gastroenteritis, and by diligently implementing both personal and food safety practices, individuals can significantly reduce their risk of contracting these debilitating illnesses and contribute to public health.
