Cellulitis, a common bacterial skin infection, presents as a red, swollen, warm, and often painful area of the skin and underlying tissues. While the immediate concern for those afflicted is relief and recovery, understanding the underlying mechanisms and the evolving landscape of its treatment reveals a fascinating interplay between established medical practices and emerging technological advancements. This article delves into the various approaches to treating cellulitis, from foundational antibiotic therapies to innovative diagnostic tools and the potential future roles of technology in combating this persistent infection.
The Cornerstones of Cellulitis Treatment: Antibiotics and Supportive Care
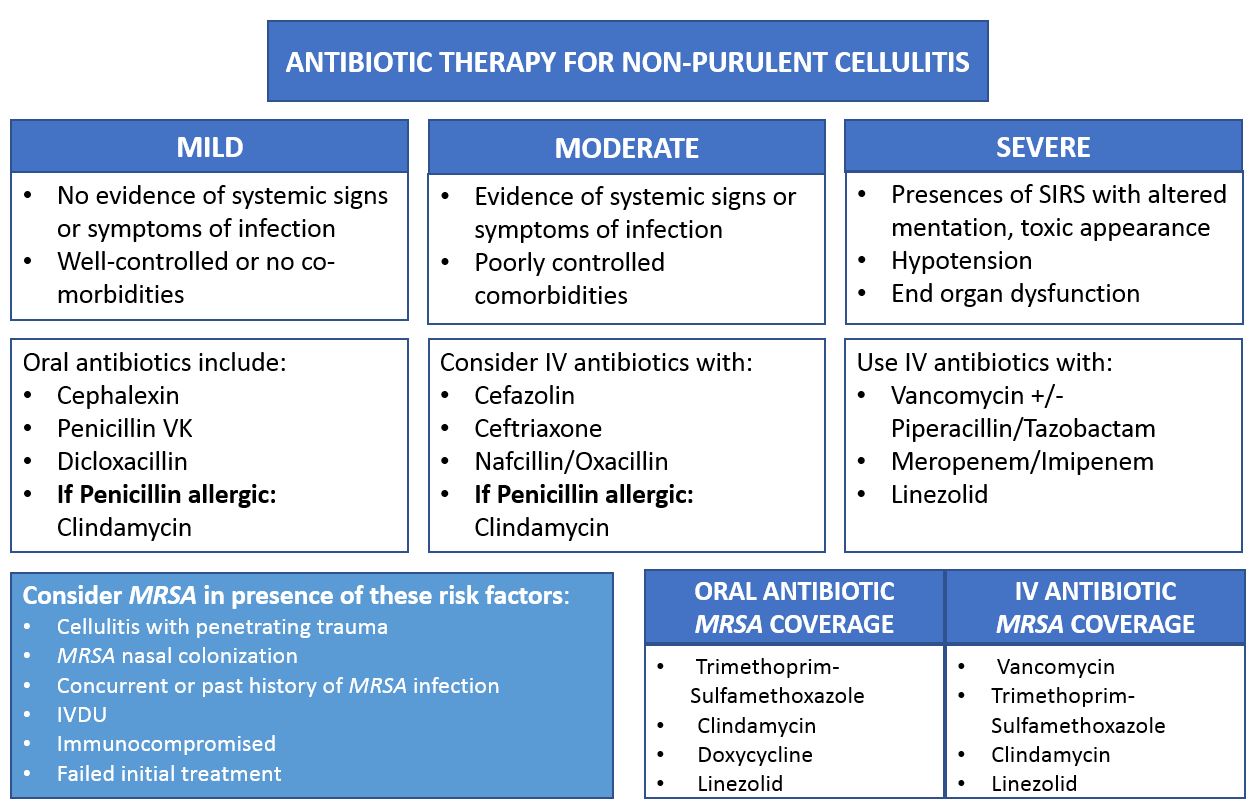
The primary weapon against cellulitis remains antibiotic therapy. The specific choice of antibiotic depends on the suspected or confirmed causative bacteria, the severity of the infection, and individual patient factors such as allergies and comorbidities. The goal is to eradicate the bacteria and prevent the spread of infection, which can, in severe cases, lead to more serious complications.
Targeting the Culprit: Antibiotic Regimens
The most common bacteria responsible for cellulitis are Streptococcus pyogenes and Staphylococcus aureus. Empiric treatment, meaning treatment initiated before definitive identification of the bacteria through cultures, often targets these pathogens.
Oral Antibiotics for Mild to Moderate Cases
For most cases of cellulitis that are not severe, oral antibiotics are the first line of treatment. These are typically prescribed for a course of 5 to 14 days. Common oral antibiotics include:
- Penicillinase-resistant penicillins: Drugs like dicloxacillin are effective against Staphylococcus aureus that produces penicillinase.
- Cephalosporins: First-generation cephalosporins, such as cephalexin, are also frequently used and offer a broad spectrum of activity against streptococci and some staphylococci.
- Clindamycin: This antibiotic is often a good choice for patients with penicillin allergies or when methicillin-resistant Staphylococcus aureus (MRSA) is suspected. Clindamycin has good tissue penetration and is effective against a wide range of bacteria.
- Macrolides: While less frequently the first choice due to increasing resistance, azithromycin or erythromycin may be considered in certain situations, particularly for patients with allergies.
The choice of oral antibiotic will be guided by local resistance patterns and the patient’s individual medical history. It is crucial for patients to complete the entire course of antibiotics as prescribed, even if symptoms improve, to ensure complete eradication of the infection and minimize the risk of recurrence or the development of antibiotic resistance.
Intravenous (IV) Antibiotics for Severe Infections and Complications
In cases of severe cellulitis, such as those with systemic signs of infection (fever, chills, rapid heart rate, low blood pressure), rapidly spreading redness, blistering, or involvement of deeper tissues, intravenous (IV) antibiotics are necessary. IV administration allows for higher drug concentrations to reach the site of infection more quickly.
- Initial IV broad-spectrum antibiotics: Initially, broad-spectrum IV antibiotics like vancomycin (for suspected MRSA), or a combination of a cephalosporin (e.g., ceftriaxone) and clindamycin might be used.
- Transition to oral therapy: Once the patient shows significant clinical improvement, typically after 24-48 hours of IV therapy and the absence of systemic symptoms, they can often be transitioned to oral antibiotics to complete the course.
The decision to hospitalize a patient for IV antibiotic treatment is based on several factors, including the severity of the infection, the patient’s ability to tolerate oral medications, the presence of underlying medical conditions that might impair healing or increase the risk of complications, and the availability of adequate home support.
Symptom Management and Supportive Measures
Beyond antibiotics, managing the symptoms of cellulitis is crucial for patient comfort and promoting healing.
Pain and Inflammation Relief
Cellulitis can be intensely painful and cause significant discomfort.
- Elevation: Elevating the affected limb above the level of the heart helps to reduce swelling and pain by improving venous return and decreasing interstitial fluid accumulation. This is a simple yet highly effective supportive measure.
- Analgesics: Over-the-counter pain relievers such as acetaminophen (Tylenol) or non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) can help manage pain and reduce inflammation. However, NSAIDs should be used with caution in individuals with certain medical conditions, such as kidney disease or gastrointestinal issues.
- Cool Compresses: Applying cool, moist compresses can provide soothing relief to the inflamed area, though care must be taken to avoid chilling the limb excessively.
Wound Care and Hygiene
Proper wound care is essential, especially if the cellulitis is associated with an open wound, ulcer, or break in the skin.
- Cleaning the affected area: Gently cleaning the area with mild soap and water is important to prevent further contamination.
- Dressing the wound: If there are open sores or blisters, appropriate sterile dressings should be applied to protect the area from further infection and promote healing. The type of dressing will depend on the nature of the wound.
- Monitoring for signs of worsening: Patients should be educated on how to monitor the affected area for signs of spreading redness, increasing pain, fever, or the development of new blisters or pus, and to seek medical attention promptly if these occur.
Identifying the Source and Preventing Recurrence
Understanding the underlying cause of cellulitis and implementing preventive measures are critical for long-term management and avoiding repeat infections. Cellulitis often occurs when bacteria gain entry through a break in the skin.
Investigating Predisposing Factors
Several factors can increase an individual’s susceptibility to cellulitis. Identifying and addressing these is a key part of treatment.
Skin Trauma and Breaks
Any break in the skin, no matter how small, can serve as an entry point for bacteria. This includes:
- Cuts, scrapes, and abrasions: From minor injuries during daily activities.
- Insect bites and stings: Which can cause localized skin damage and introduce bacteria.
- Surgical wounds: Post-operative infections can manifest as cellulitis.
- Chronic skin conditions: Such as eczema or psoriasis, which can lead to dry, cracked skin and increased vulnerability.
- Fungal infections: Athlete’s foot, for instance, can cause cracks in the skin between the toes, creating an entry point for bacteria.
Underlying Medical Conditions
Certain chronic health conditions can impair the body’s ability to fight infection and heal, making individuals more prone to cellulitis.
- Diabetes Mellitus: High blood sugar levels can damage blood vessels and nerves, impairing circulation and wound healing, and making the skin more susceptible to infection.
- Venous Insufficiency and Lymphedema: Conditions that cause swelling in the legs and feet can compromise skin integrity and lymphatic drainage, creating a favorable environment for bacterial growth.
- Obesity: Can lead to impaired circulation and increased susceptibility to skin breakdown.
- Weakened Immune System: Conditions like HIV/AIDS, or treatments such as chemotherapy or immunosuppressant medications, can significantly reduce the body’s ability to combat infections.
Strategies for Recurrence Prevention
Preventing cellulitis from returning is as important as treating the initial episode.
Maintaining Skin Integrity
Keeping the skin healthy and intact is paramount.
- Moisturizing: Regular use of emollients, especially for individuals with dry or eczematous skin, can prevent cracking.
- Prompt treatment of wounds: Minor cuts and abrasions should be cleaned and covered appropriately to prevent infection.
- Managing chronic conditions: Strict control of diabetes, proper management of venous insufficiency with compression stockings, and addressing lymphedema can significantly reduce the risk.
- Treating fungal infections: Prompt and effective treatment of conditions like athlete’s foot can prevent secondary bacterial infections.
Prophylactic Antibiotics
In individuals who experience recurrent episodes of cellulitis, particularly those with underlying predisposing factors like lymphedema or chronic venous insufficiency, a doctor may consider long-term prophylactic antibiotic therapy. This typically involves taking a low dose of an antibiotic daily or periodically to suppress bacterial growth and prevent infection. This approach is reserved for specific cases and requires careful consideration of the benefits versus the risks of long-term antibiotic use, such as the development of antibiotic resistance and potential side effects.
The Evolving Landscape: Technological Innovations in Cellulitis Management
While antibiotics remain the bedrock of cellulitis treatment, the integration of technology is beginning to play a more significant role in diagnosis, monitoring, and potentially even prevention. These advancements offer the promise of more precise and efficient patient care.
Advanced Diagnostic Tools
Accurate and early diagnosis is crucial for effective treatment. Technology is enhancing our ability to identify the infection and its extent.
Point-of-Care (POC) Diagnostics
The development of rapid diagnostic tests is a key area of innovation.
- Rapid Bacterial Identification: While still under development for widespread clinical use in cellulitis, research is ongoing into portable devices that can quickly identify the specific bacterial culprit directly from a wound swab or fluid sample. This could allow for targeted antibiotic therapy much sooner than traditional culture methods, which can take 24-72 hours.
- Biomarker Detection: Technologies are emerging to detect specific biomarkers in blood or tissue that indicate the presence and severity of infection. This could aid in differentiating cellulitis from other inflammatory conditions.
Imaging Technologies
Advanced imaging can provide valuable insights into the extent of the infection.
- Ultrasound: Portable ultrasound devices can be used at the bedside to assess the depth of the infection, identify abscesses that may require drainage, and evaluate for fluid collections. This can guide surgical intervention if necessary.
- Thermography: While not yet a standard diagnostic tool for cellulitis, infrared thermography can objectively measure skin temperature. Since inflammation in cellulitis causes increased skin temperature, thermography could potentially be used to objectively map the extent of inflammation and monitor the response to treatment over time.
Remote Monitoring and Telehealth
The increasing accessibility of telehealth and wearable devices offers new avenues for patient care and monitoring.
Telemedicine for Follow-Up and Triage
- Virtual Consultations: Patients can utilize video consultations with healthcare providers to discuss their symptoms, receive advice on home care, and have their progress monitored without the need for in-person visits, especially for follow-up appointments. This is particularly beneficial for individuals in rural areas or those with mobility issues.
- Remote Assessment of Visual Changes: Patients can share images of the affected area with their healthcare provider via secure platforms, allowing for visual assessment of changes in redness, swelling, and wound healing.
Wearable Devices and Data Integration
- Temperature Monitoring: Wearable devices that continuously monitor body temperature could alert patients and healthcare providers to potential fevers, an early sign of worsening infection or systemic involvement.
- Activity and Vital Sign Tracking: Wearables can track other vital signs like heart rate, which can also be indicators of infection. This data, when integrated into electronic health records, could provide a more comprehensive picture of a patient’s health status and aid in early detection of complications.
The Future Frontier: AI and Personalized Medicine
Artificial intelligence (AI) and the principles of personalized medicine hold significant promise for revolutionizing how cellulitis is understood and treated in the future.
AI in Diagnosis and Risk Stratification
- Image Analysis: AI algorithms are being trained to analyze medical images, including photographs of skin lesions, to aid in the diagnosis of cellulitis and differentiate it from other skin conditions with high accuracy.
- Predictive Modeling: AI can analyze vast datasets of patient information to identify individuals at high risk for developing cellulitis or experiencing recurrent infections. This could allow for targeted preventive interventions.

Personalized Treatment Strategies
- Genomic and Proteomic Analysis: In the future, understanding an individual’s genetic makeup and the specific proteins present in their body could lead to highly personalized treatment plans, optimizing antibiotic selection and dosage based on individual metabolic profiles and immune responses.
- Predicting Treatment Response: AI could potentially predict how a patient will respond to different antibiotic regimens, allowing for the selection of the most effective treatment from the outset, thereby reducing treatment failures and the risk of antibiotic resistance.
In conclusion, while the core treatment for cellulitis revolves around effective antibiotic therapy and supportive care, the medical community is continuously exploring and integrating technological advancements. From enhancing diagnostic capabilities with rapid POC tests and advanced imaging to leveraging telehealth for remote monitoring and harnessing the power of AI for predictive analytics and personalized medicine, the future of cellulitis management is poised for significant innovation, ultimately aiming for more efficient, accurate, and patient-centered care.