The health and well-being of an infant are paramount to every parent. Among the common concerns that can arise in the early months of a baby’s life, thrush is a frequent visitor. This article delves into the nature of infant thrush, its causes, symptoms, diagnosis, and, most importantly, its effective management and prevention. Understanding this common fungal infection is crucial for parents to address it promptly and ensure their baby’s comfort and health.
Understanding the Fungus: Candida Albicans
At its core, infant thrush is a yeast infection, most commonly caused by a fungus called Candida albicans. This particular yeast is a naturally occurring organism that lives in many parts of the body, including the mouth, digestive tract, and on the skin, in small, harmless amounts. For most individuals, Candida coexists peacefully with other microorganisms and poses no threat.

However, in certain circumstances, this balance can be disrupted, leading to an overgrowth of Candida. This overgrowth is what we recognize as a yeast infection. In infants, the immature immune system plays a significant role in their susceptibility. Their bodies are still developing the robust defenses needed to keep Candida in check. This makes their mouths, which are frequently exploring the environment and can harbor various microbes, particularly vulnerable to an overgrowth.
Beyond the infant’s developing immune system, other factors can contribute to the disruption of the natural balance. For instance, if a mother is breastfeeding, and she has a yeast infection on her nipples or breasts (often referred to as nipple thrush), she can transmit the Candida to her baby during feeding, and vice versa. Additionally, if an infant has recently been treated with antibiotics, these medications can kill off beneficial bacteria in the mouth that normally help to keep Candida populations under control. This leaves an opening for the yeast to proliferate.
The environment within the infant’s mouth can also play a role. A moist, warm environment, which the mouth naturally provides, is ideal for yeast to thrive. While this is a normal aspect of the oral cavity, when combined with a weakened defense system or external introduction of Candida, it can facilitate an infection.
The Role of the Immune System
The immune system is the body’s primary defense against pathogens, including fungi like Candida. In newborns and very young infants, this system is still undergoing maturation. Key components, such as the T-cells which are crucial for fighting fungal infections, are not yet as developed or experienced as they are in older children and adults. This immaturity means that the infant’s body may not be as effective at recognizing and eliminating an overgrowth of Candida on its own. Consequently, even a small initial overgrowth can quickly escalate into a noticeable infection.
Transmission Pathways
Candida albicans is highly adaptable and can be transmitted through various means. For infants, the most common route of transmission is from mother to baby during childbirth. If a mother has a vaginal yeast infection, the baby can ingest or come into contact with the yeast as it passes through the birth canal.
Another significant transmission pathway, especially for breastfeeding mothers and their infants, is through direct contact. As mentioned, if a mother has nipple thrush, the Candida can be passed to the baby during feeding. Conversely, if an infant has oral thrush, they can transmit the yeast to their mother’s nipples during feeding, leading to a cyclical infection that can be difficult to clear. This highlights the importance of treating both mother and baby concurrently if both show signs of infection.
Shared items that come into contact with the baby’s mouth can also be vectors for transmission. This includes pacifiers, bottle nipples, teething toys, and even the hands of caregivers if they are not properly washed after handling an infected individual or contaminated items.
Antibiotic Use and Disruption of Flora
Antibiotics are powerful medications designed to kill bacteria. While essential for treating bacterial infections, they can have a broad-spectrum effect, meaning they can also eliminate beneficial bacteria that reside naturally in the body. In the mouth, these good bacteria play a crucial role in maintaining a healthy microbial balance and preventing the overgrowth of opportunistic organisms like Candida.
When an infant or a breastfeeding mother takes antibiotics, the disruption of this natural bacterial flora can create an environment where Candida can multiply unchecked. This is why thrush is often observed following a course of antibiotic treatment, particularly in infants who have had a bacterial infection themselves or if the mother has been taking antibiotics while breastfeeding.
Recognizing the Signs: Symptoms of Infant Thrush
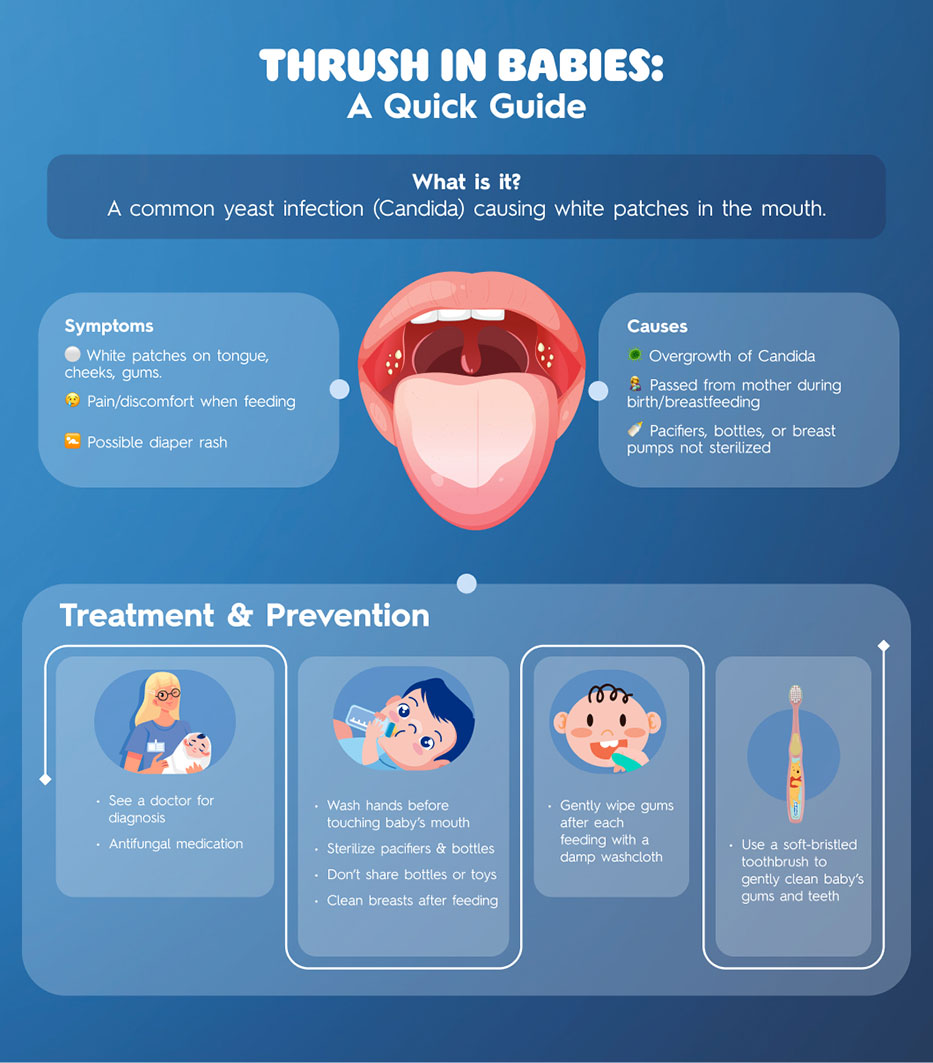
Identifying thrush in infants is often straightforward, though it can sometimes be mistaken for other conditions. The hallmark signs usually appear in the mouth, but the infection can also affect the diaper area.
Oral Manifestations
The most visible signs of oral thrush typically involve the tongue, inner cheeks, gums, and the roof of the mouth. Parents may notice creamy white, cottage cheese-like patches or lesions. These patches can be slightly raised and may appear on a red, irritated background.
- Appearance of Patches: The characteristic white patches are the primary indicator. They are distinct from the milk residue that often coats an infant’s tongue after feeding; thrush patches are more firmly adherent and cannot be easily wiped away. If an attempt is made to scrape them off, the underlying tissue may appear red, raw, and sometimes even bleed.
- Irritability and Discomfort: Infants with thrush often experience discomfort and pain in their mouths. This can manifest as increased fussiness, crying during feeding, and general irritability. They may refuse to eat or eat less than usual due to the soreness.
- Feeding Difficulties: The pain and discomfort associated with oral thrush can significantly impact feeding. Babies might latch poorly, become distressed mid-feed, or pull away from the breast or bottle. This can lead to reduced milk intake and concerns about adequate nutrition and weight gain.
- Soreness and Redness: The oral tissues beneath the white patches are often inflamed and sore. This can be observed as a distinct redness on the gums, tongue, or inner cheeks.
Diaper Area Involvement (Diaper Rash)
Infant thrush is not confined to the mouth. The Candida fungus can also cause a severe form of diaper rash. This typically occurs if the yeast is transferred from the mouth to the diaper area through drool or if the baby is directly infected through soiled diapers.
- Distinct Rash Characteristics: Unlike typical diaper rash, which may present as redness and irritation, Candida-related diaper rash is often more severe and widespread. It commonly appears as bright red patches, often with smaller satellite lesions (red spots or pustules) appearing around the main rash.
- Location: The rash typically affects the skin folds in the diaper area, including the groin, buttocks, and thighs. It can be intensely itchy and cause the baby considerable discomfort.
- Persistence: This type of diaper rash can be stubbornly resistant to standard diaper rash creams and treatments, a key indicator that a fungal infection may be present.
Diagnosis and When to Seek Medical Advice
While many cases of infant thrush can be diagnosed based on visual symptoms, seeking professional medical advice is always recommended, especially if symptoms are severe, persistent, or if there are concerns about the baby’s health.
Visual Inspection by a Healthcare Professional
A pediatrician or healthcare provider can typically diagnose oral thrush with a simple visual examination of the infant’s mouth. They will look for the characteristic white patches and assess the surrounding tissues for redness and irritation. If diaper rash is also present and suspected to be fungal, a similar visual inspection of the affected area will be performed.
Differential Diagnosis
In some instances, it may be necessary to differentiate thrush from other conditions that can cause similar symptoms. For example, milk residue in the mouth needs to be distinguished from true thrush patches. Other oral conditions or irritations might also present with redness or white spots, so a professional diagnosis is valuable.
When to Consult a Doctor
- Persistent Symptoms: If the white patches in the mouth do not improve after a few days of home care, or if they seem to be spreading, it is advisable to consult a doctor.
- Severe Discomfort or Feeding Issues: If the infant is in significant pain, crying excessively, or having trouble feeding due to oral discomfort, medical intervention may be necessary.
- Fungal Diaper Rash: A severe or persistent diaper rash that does not respond to over-the-counter treatments should be evaluated by a doctor, as it could indicate a fungal infection.
- Recurrent Infections: If an infant experiences recurrent episodes of thrush, it may be a sign of an underlying issue that needs investigation, such as a weakened immune system or a persistent source of infection.
- Concerns for the Mother: If a breastfeeding mother experiences nipple pain, redness, or burning sensations, she should also consult her doctor, as she may have nipple thrush and need treatment concurrently with her baby.
Effective Management and Treatment Strategies
Fortunately, infant thrush is treatable, and with the right approach, discomfort can be alleviated, and the infection cleared effectively. Treatment strategies focus on eliminating the fungal overgrowth and preventing its recurrence.
Antifungal Medications
The cornerstone of thrush treatment is the use of antifungal medications. These are typically prescribed by a pediatrician and come in several forms, tailored for infants.
- Oral Antifungal Gels or Liquids: For oral thrush, a common treatment involves an antifungal medication applied directly to the inside of the baby’s mouth. These are often in the form of a gel or liquid and are typically administered with a dropper or swab after feedings. The medication is gently spread over the affected areas, including the tongue, gums, and inner cheeks. It is crucial to follow the prescribed dosage and duration of treatment meticulously.
- Topical Antifungal Creams: For fungal diaper rash, a topical antifungal cream is prescribed. These creams are applied to the affected diaper area during diaper changes. It is important to ensure the area is clean and dry before application.
Home Care and Hygiene Practices
Beyond prescribed medications, diligent hygiene practices are essential for managing and preventing the spread of thrush.
- Sterilizing Feeding Equipment: All items that come into contact with the baby’s mouth should be thoroughly sterilized. This includes pacifiers, bottle nipples, teething toys, and any breast pump parts. These items should be washed with hot, soapy water and then boiled for at least five minutes or washed in a dishwasher on a hot cycle.
- Breastfeeding Mother’s Hygiene: For breastfeeding mothers, meticulous hygiene is critical. Nipples and areolas should be washed thoroughly with water after each feeding. If the mother has been diagnosed with nipple thrush, she will likely be prescribed an antifungal cream for her nipples, which should be applied as directed. It is also important to avoid using soap on the nipples as this can dry out the skin and make it more susceptible to infection.
- Hand Washing: Frequent and thorough hand washing is paramount for everyone who handles the baby or their feeding equipment. Caregivers should wash their hands before and after feeding the baby, changing diapers, and handling any items that go into the baby’s mouth.
- Diaper Changes: Frequent diaper changes are essential to keep the diaper area clean and dry, which helps to prevent the spread and exacerbation of fungal diaper rash.
Duration of Treatment and Follow-Up
It is vital to complete the full course of antifungal medication as prescribed by the doctor, even if the symptoms appear to improve sooner. Stopping treatment prematurely can lead to the recurrence of the infection. Typically, treatment for oral thrush lasts for about one to two weeks.
A follow-up appointment with the pediatrician may be recommended to ensure the infection has been completely cleared. If symptoms persist or worsen, medical attention should be sought again to reassess the situation and adjust the treatment plan if necessary.
Preventing Recurrence and Long-Term Oral Health
Once an infant has experienced thrush, taking steps to prevent its recurrence is important for maintaining their ongoing comfort and health. This involves a combination of ongoing hygiene and understanding potential triggers.
Maintaining Good Hygiene Routines
The hygiene practices mentioned for treatment are equally important for prevention.
- Consistent Sterilization: Continue to sterilize pacifiers, bottle nipples, and teething toys regularly, especially if they are used frequently.
- Regular Hand Washing: Emphasize hand hygiene among all caregivers who interact with the infant and their feeding items.
- Prompt Diaper Changes: Addressing diaper rash promptly and ensuring the diaper area remains clean and dry can help prevent the spread of yeast.
Dietary Considerations and Probiotics
While not a primary treatment, some parents explore dietary interventions and probiotics.
- Probiotics: Some research suggests that certain strains of probiotics, particularly Lactobacillus species, may help restore a healthy balance of microorganisms in the gut and mouth, potentially reducing the risk of yeast overgrowth. It’s advisable to discuss the use of probiotics for infants with a pediatrician.
- Breastfeeding Diet: For breastfeeding mothers, maintaining a balanced and healthy diet can support overall immune function, which indirectly benefits the baby. Some sources suggest reducing sugar intake, as yeast thrives on sugar, but this is not a universally proven method for preventing thrush.
Monitoring for Early Signs
Being aware of the early signs of thrush allows for prompt intervention. If a parent notices any white patches in the baby’s mouth or a developing rash in the diaper area that looks suspicious, they can consult their doctor sooner rather than later. Early detection and treatment can often prevent a more severe or prolonged infection.
Addressing Underlying Factors
In cases of recurrent thrush, it is important to work with a healthcare provider to rule out any underlying conditions that might be contributing to the problem. This could include exploring potential immune system deficiencies or ensuring that all sources of transmission (e.g., maternal nipple thrush) are fully addressed. A thorough evaluation can help identify and manage any contributing factors, thereby minimizing the likelihood of future occurrences. By understanding the nature of thrush, recognizing its symptoms, and employing effective management and prevention strategies, parents can confidently navigate this common infant health concern and ensure their baby enjoys a healthy and comfortable start to life.
