The uterus, a vital organ in the female reproductive system, plays a central role in menstruation, conception, and pregnancy. Understanding its normal measurements is crucial for healthcare professionals to assess reproductive health, diagnose potential abnormalities, and monitor conditions such as fibroids, endometriosis, and pregnancy progression. While “normal” can vary significantly based on factors like age, parity (number of pregnancies), and hormonal status, a general understanding of typical uterine dimensions provides a valuable baseline. This article delves into the standard measurements of the uterus, exploring how these dimensions are assessed and what variations might indicate.
Understanding Uterine Anatomy and Measurement Techniques
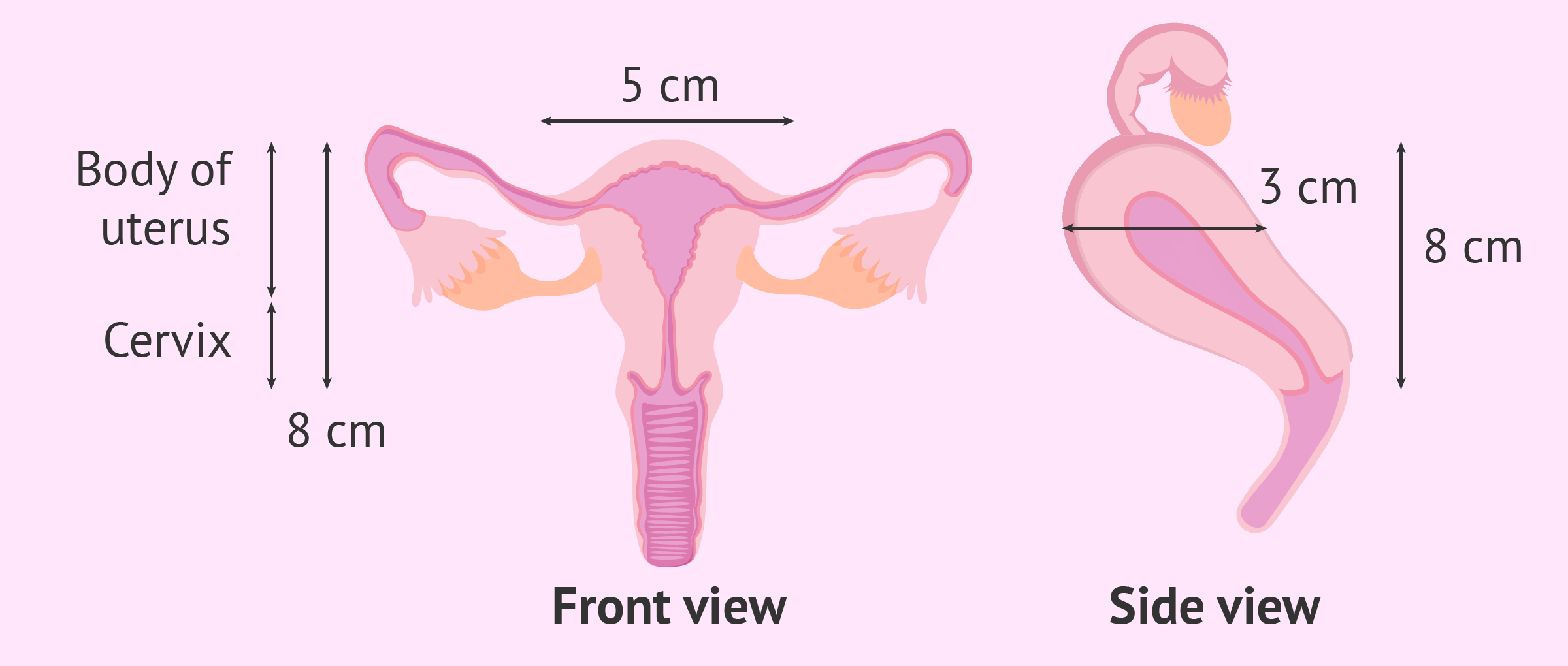
The uterus is a pear-shaped, muscular organ situated in the pelvic cavity, between the bladder and the rectum. It is comprised of several key anatomical components, each contributing to its overall size and shape: the fundus (the upper, rounded portion), the corpus (the main body), and the cervix ( the lower, narrow part that opens into the vagina).
Anatomical Landmarks for Measurement
When measuring the uterus, clinicians typically focus on three primary dimensions:
- Length (Longitudinal Measurement): This is the measurement from the superior aspect of the uterine fundus to the external os of the cervix. It represents the longest dimension of the uterus.
- Width (Transverse Measurement): This measurement is taken at the widest point of the uterine corpus, perpendicular to the length.
- Anteroposterior (AP) Diameter (Thickness): This measurement is taken from the anterior wall of the uterus to the posterior wall at its thickest point, usually in the mid-corpus region.
Imaging Modalities for Uterine Assessment
The most common and accurate methods for measuring uterine dimensions involve imaging techniques:
Transvaginal Ultrasound (TVUS)
Transvaginal ultrasound is the gold standard for assessing uterine size and morphology in non-pregnant women. A specialized transducer is inserted into the vagina, allowing for close proximity to the uterus and high-resolution imaging. This method provides clear visualization of the uterine walls, endometrial lining, and any potential masses. TVUS allows for precise measurements in sagittal and axial planes.
Transabdominal Ultrasound (TAUS)
Transabdominal ultrasound is often used as a complementary or initial assessment tool, particularly in cases where transvaginal access is difficult or uncomfortable. A transducer is placed on the lower abdomen, and ultrasound waves pass through the abdominal wall to visualize the pelvic organs. While less detailed than TVUS, it can provide general measurements and is useful for assessing larger uteri or in obese patients.
Magnetic Resonance Imaging (MRI)
MRI offers superior soft-tissue contrast and can provide detailed anatomical information, especially for complex cases or when differentiating between various pathologies. It is not typically used for routine uterine measurement but is invaluable for detailed evaluation of uterine anomalies, masses, and extent of disease.
Hysterosalpingography (HSG)
While primarily used to assess the patency of the fallopian tubes, HSG involves injecting contrast dye into the uterine cavity. The X-ray images produced during this procedure can indirectly provide information about uterine size and shape, particularly its internal dimensions and any irregularities within the cavity.
Normal Uterine Measurements in Non-Pregnant Adults
The dimensions of a non-pregnant uterus are influenced by several factors, with age and parity being the most significant.
Nulliparous Uterus (Never Given Birth)
In women who have never been pregnant or given birth (nulliparous), the uterus is generally smaller and more compact. Typical measurements are:
- Length: 6.0 to 7.0 cm
- Width: 4.0 to 5.0 cm
- AP Diameter: 2.0 to 3.0 cm
The cervix in nulliparous women is also relatively longer compared to the corpus.
Multiparous Uterus (Given Birth)
Women who have had one or more pregnancies and deliveries (multiparous) tend to have a slightly larger uterus, even outside of pregnancy. This is due to the muscular stretching and changes that occur during pregnancy. Typical measurements in multiparous women are:
- Length: 7.0 to 8.0 cm
- Width: 5.0 to 6.0 cm
- AP Diameter: 3.0 to 4.0 cm
The cervix in multiparous women is often shorter and wider, with a more capacious external os.
Hormonal Influence and Menstrual Cycle
The size of the uterus can also fluctuate slightly throughout the menstrual cycle due to hormonal influences, particularly estrogen. The endometrium (the inner lining of the uterus) thickens in preparation for potential implantation, which can subtly increase the uterine cavity’s volume and anteroposterior diameter. However, these cyclical changes are generally minor and do not significantly alter the overall dimensions of the uterine wall itself.

Pre-Pubertal and Post-Menopausal Uterus
- Pre-pubertal Uterus: Before puberty, the uterus is small, with a length of approximately 2.5 to 3.5 cm. The cervix is proportionally larger than the corpus.
- Post-menopausal Uterus: After menopause, the ovaries produce less estrogen and progesterone, leading to atrophy of the uterus. The uterine lining thins, and the overall size decreases. Typical measurements in post-menopausal women can range from:
- Length: 4.0 to 5.0 cm
- Width: 2.5 to 3.5 cm
- AP Diameter: 1.5 to 2.5 cm
However, a uterus that remains enlarged post-menopausally warrants further investigation.
Factors Causing Uterine Enlargement and Abnormalities
Deviations from these normal measurements can indicate various physiological or pathological conditions.
Pregnancy
The most significant cause of uterine enlargement is pregnancy. As the fetus grows, the uterus expands dramatically. During the first trimester, the uterus grows in size, and by the end of pregnancy, it can extend from the pelvis to the xiphoid process, reaching a length of approximately 30-35 cm and a significantly increased volume.
Uterine Fibroids (Leiomyomas)
Fibroids are benign smooth muscle tumors that grow within the uterine wall. They are very common and can vary in size from microscopic to very large. The presence of fibroids can significantly increase the overall size and alter the shape of the uterus, making measurements irregular. The uterus may appear lobulated or distorted depending on the number, size, and location of the fibroids.
Adenomyosis
Adenomyosis is a condition where the endometrial tissue grows into the muscular wall of the uterus (myometrium). This causes the uterus to enlarge and become tender. An adenomyotic uterus is often described as symmetrically enlarged, with measurements typically exceeding the normal range.
Endometrial Hyperplasia and Polyps
While these conditions primarily affect the endometrium, significant thickening or large endometrial polyps can contribute to a slightly increased anteroposterior diameter of the uterine cavity.
Uterine Anomalies
Congenital anomalies of the uterus, such as a bicornuate (heart-shaped) or septate uterus, can result in altered uterine dimensions and shape, although the overall volume might not always be significantly larger.
Malignancy
Although less common than benign conditions, uterine cancers (e.g., endometrial cancer, uterine sarcoma) can cause uterine enlargement, particularly in later stages.
Clinical Significance of Uterine Measurements
Accurate uterine measurements are fundamental in clinical practice for several reasons:
Diagnosis of Reproductive Health Issues
Enlarged or abnormally shaped uteri can be the first sign of underlying reproductive health problems. Deviations from normal measurements prompt further investigation to determine the cause.
Monitoring Pregnancy
During prenatal care, ultrasound measurements of the uterus and fetal growth are essential for monitoring the progress of a pregnancy and identifying potential complications like intrauterine growth restriction or suspected multiple gestations.
Assessment of Fertility
Uterine size and morphology can impact fertility. For example, a significantly small uterus may be associated with primary ovarian insufficiency, while fibroids or adenomyosis can interfere with implantation.
Guiding Treatment Decisions
Knowing the size and characteristics of the uterus is crucial for planning surgical interventions, such as myomectomy (fibroid removal) or hysterectomy (uterus removal), or for managing conditions like endometriosis.

Tracking Disease Progression
For conditions like fibroids or adenomyosis, regular measurement of uterine size can help monitor disease progression or the effectiveness of medical therapies.
In conclusion, while a range of dimensions constitutes a “normal” uterus, understanding these benchmarks is vital. Variations from the typical measurements—whether in length, width, or anteroposterior diameter—serve as important clinical indicators, prompting further evaluation and ensuring optimal reproductive health management for women. The advancements in imaging technologies continue to refine our ability to accurately assess and interpret these crucial uterine parameters.
