The quest for effective, safe, and sustainable weight loss solutions has long been a significant area of medical research and consumer interest. In recent years, pharmaceutical innovation has yielded a new generation of weight loss medications, often referred to as “weight loss pills,” that offer promising results for individuals struggling with obesity and related health conditions. These advancements represent a significant leap forward from earlier, less effective, or more problematic weight management drugs. Understanding what constitutes these “new weight loss pills,” how they work, who they are for, and their potential benefits and risks is crucial for anyone considering them as part of a comprehensive weight management strategy.
The Evolving Landscape of Weight Loss Medications
The history of weight loss drugs is a complex tapestry of scientific discovery, market fluctuations, and regulatory oversight. Early attempts at pharmacological intervention often involved stimulants or appetite suppressants with significant side effects. Over time, research has shifted towards understanding the intricate hormonal and metabolic pathways that regulate appetite, satiety, and energy expenditure. This deeper understanding has paved the way for the development of more targeted and effective medications.
From Basic Appetite Suppression to Metabolic Regulation
Initial weight loss drugs, primarily available in the mid-to-late 20th century, focused on stimulating the central nervous system to reduce appetite. While some achieved short-term weight loss, they were frequently associated with adverse effects like increased heart rate, blood pressure, anxiety, and insomnia. Furthermore, their efficacy often waned over time, and the risk of dependence was a concern.
The scientific community then began to explore the gut-brain axis and the role of hormones in appetite regulation. Hormones like ghrelin (the “hunger hormone”) and leptin (the “satiety hormone”) became key targets. Research also delved into how the body processes and stores fat, as well as how it utilizes energy. This led to the development of drugs that aimed to influence these more complex physiological processes.
The Rise of GLP-1 Receptor Agonists
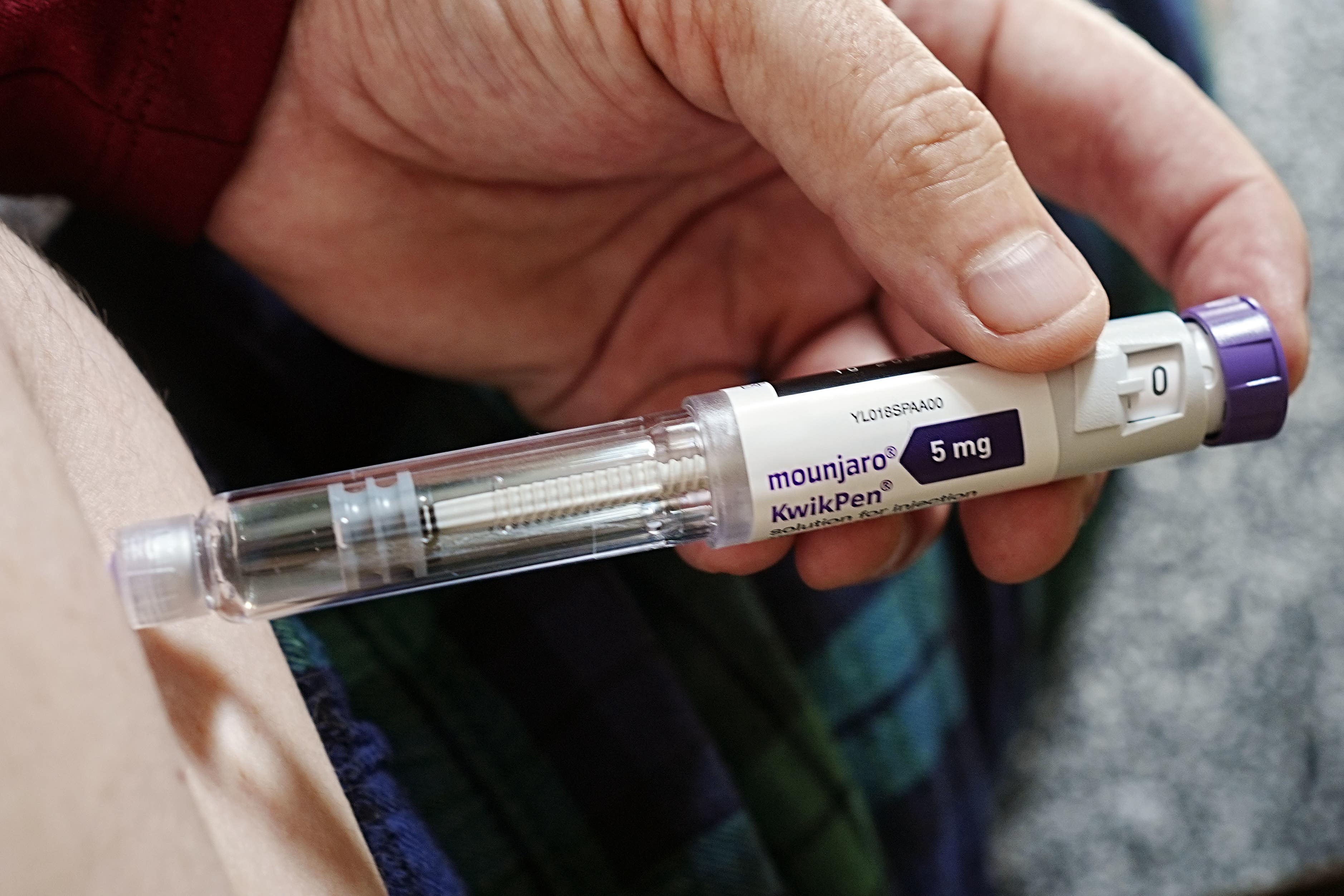
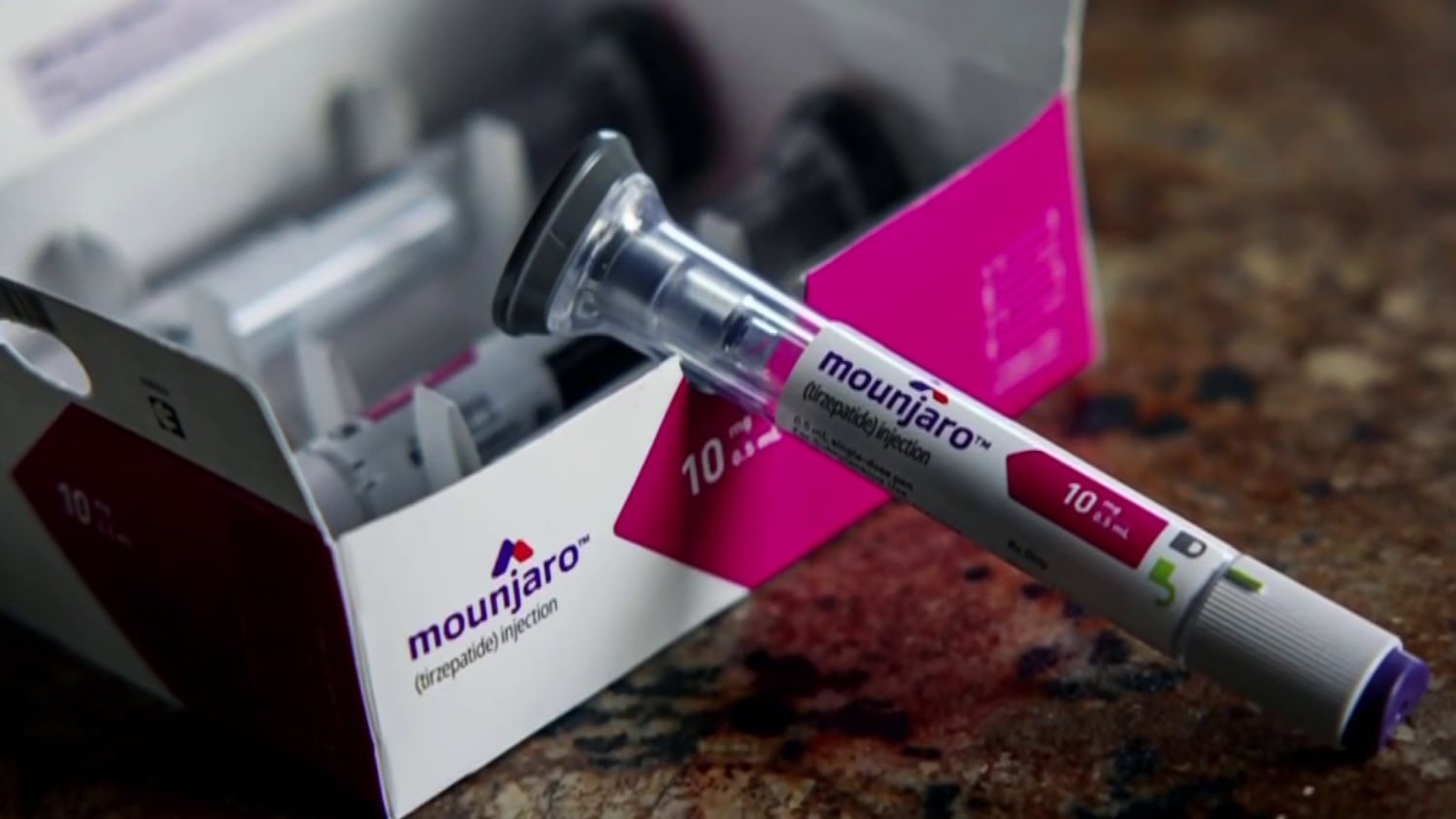
Perhaps the most significant breakthrough in recent years has been the development and widespread adoption of glucagon-like peptide-1 (GLP-1) receptor agonists. These medications were initially developed for the management of type 2 diabetes but were found to have a profound and consistent effect on weight loss. GLP-1 is a naturally occurring hormone produced in the intestines in response to food intake. It plays several crucial roles in glucose regulation and appetite control.
GLP-1 receptor agonists mimic the action of this natural hormone. They work by binding to GLP-1 receptors in various parts of the body, including the brain, stomach, and pancreas. This leads to a cascade of effects that contribute to weight loss:
- Increased Satiety: They slow down gastric emptying, meaning food stays in the stomach longer, leading to a prolonged feeling of fullness and reduced overall food intake.
- Appetite Suppression: They act on the brain’s appetite control centers, reducing cravings and hunger signals.
- Improved Glucose Control: In individuals with type 2 diabetes, they enhance insulin secretion and reduce glucagon secretion, leading to better blood sugar management.
This class of drugs, including semaglutide (marketed as Ozempic and Wegovy) and liraglutide (marketed as Victoza and Saxenda), has demonstrated significant and sustained weight loss in clinical trials, often resulting in a reduction of 5-15% or more of body weight for many individuals.
Mechanisms of Action: How the New Pills Work
The efficacy of the newer weight loss pills, particularly the GLP-1 receptor agonists, lies in their multifaceted approach to tackling the complex issue of weight management. They don’t simply suppress appetite; they influence the body’s intricate hormonal and metabolic signaling.
Targeting the Gut-Brain Axis and Appetite Regulation
The gut-brain axis is a bidirectional communication network that connects the gastrointestinal tract and the central nervous system. Hormones produced in the gut, such as GLP-1, play a vital role in signaling satiety to the brain. GLP-1 receptor agonists essentially “hijack” this natural pathway. By binding to GLP-1 receptors in the hypothalamus, the region of the brain responsible for regulating hunger and satiety, these medications effectively increase the sensation of fullness. This reduces the drive to eat, making it easier for individuals to consume fewer calories without feeling deprived or experiencing intense cravings.
Furthermore, these drugs can influence the reward pathways in the brain associated with food. By modulating these signals, they can decrease the motivation to seek out and consume high-calorie foods, further contributing to a reduced caloric intake.
Influencing Gastric Emptying and Nutrient Absorption
Another key mechanism is the slowing of gastric emptying. After eating, the stomach normally empties its contents into the small intestine at a controlled rate. GLP-1 receptor agonists slow down this process. This means that food remains in the stomach for a longer period, contributing to a sustained feeling of fullness and reducing the urge to snack between meals. This delayed emptying also has implications for nutrient absorption, potentially impacting how the body processes the food consumed. While not a primary weight loss mechanism, it plays a supporting role in overall caloric regulation.
Metabolic Effects Beyond Appetite
Beyond their direct effects on appetite and food intake, some weight loss medications, particularly those targeting GLP-1, also have beneficial effects on metabolic health. As mentioned, they improve insulin sensitivity and glucose regulation. This is particularly important for individuals who are overweight or obese, as they often have underlying metabolic dysfunction, including insulin resistance and an increased risk of developing type 2 diabetes. The improved metabolic profile can contribute to a healthier overall state, making weight loss more sustainable and reducing the risk of associated comorbidities. Some research also suggests potential effects on fat metabolism, though this is an area of ongoing investigation.
Eligibility and Considerations for Use
While the new weight loss pills offer a promising avenue for many, they are not a universal solution and require careful consideration of individual health profiles and lifestyle factors. Their use is typically reserved for specific patient populations and is best undertaken with the guidance of a healthcare professional.
Who Benefits from These Medications?
The primary candidates for these new weight loss medications are individuals who are considered obese or overweight and have at least one weight-related comorbidity. This typically includes conditions such as:
- Type 2 Diabetes: Given the dual benefit of glucose control and weight loss, GLP-1 receptor agonists are a strong option for individuals with type 2 diabetes and obesity.
- High Blood Pressure (Hypertension): Losing weight can significantly improve blood pressure readings, reducing the risk of cardiovascular events.
- High Cholesterol: Weight loss often leads to improvements in cholesterol levels.
- Sleep Apnea: Excess weight is a major contributing factor to sleep apnea, and weight reduction can alleviate symptoms.
- Cardiovascular Disease: For individuals with established cardiovascular disease, weight loss can reduce their risk of future events.
Generally, these medications are prescribed for individuals with a Body Mass Index (BMI) of 30 or higher (obesity) or a BMI of 27 or higher (overweight) who also have one or more of these comorbidities. In some cases, individuals with a lower BMI may be considered if they have a significant health risk associated with their weight.
The Importance of a Comprehensive Approach
It is critical to emphasize that these weight loss pills are not a magic bullet. They are designed to be a tool to aid weight loss within a broader, comprehensive weight management program. This program should always include:
- Dietary Changes: Sustainable, healthy eating habits that promote a caloric deficit are essential. This involves making conscious choices about food intake, portion control, and nutrient density.
- Regular Physical Activity: Incorporating regular exercise is crucial for burning calories, building muscle mass, and improving overall health. The type and intensity of exercise should be tailored to the individual’s capabilities and preferences.
- Behavioral Therapy: Addressing the psychological and behavioral aspects of eating is often necessary. This can involve working with a therapist or counselor to identify triggers for overeating, develop coping mechanisms, and build a healthier relationship with food.
Without these lifestyle modifications, the effectiveness of the medication will be limited, and weight regain is highly probable once the medication is discontinued.
Potential Benefits and Side Effects
Like all medications, the new weight loss pills offer a range of potential benefits alongside a profile of possible side effects. A thorough discussion with a healthcare provider is essential to weigh these factors for individual suitability.
Significant Health Improvements
The most compelling benefit of these medications is their ability to facilitate significant and sustainable weight loss, leading to a reduction in the burden of weight-related comorbidities. Beyond the numbers on the scale, individuals often experience:
- Improved Blood Sugar Control: Particularly beneficial for those with type 2 diabetes.
- Lowered Blood Pressure and Cholesterol: Contributing to better cardiovascular health.
- Increased Energy Levels and Reduced Fatigue: Making daily activities easier and more enjoyable.
- Enhanced Mobility and Reduced Joint Pain: Particularly for those with weight-bearing joint issues.
- Improved Self-Esteem and Quality of Life: The positive impact of achieving health goals can be profound.
- Reduced Risk of Cardiovascular Events: Studies have shown a reduction in heart attack, stroke, and cardiovascular death in certain patient populations using these medications.
Common and Serious Side Effects
The most frequently reported side effects are gastrointestinal in nature, often occurring as the body adjusts to the medication. These can include:
- Nausea: Often the most common side effect, particularly when starting the medication or increasing the dose.
- Vomiting: Can occur, especially if meals are too large or eaten too quickly.
- Diarrhea or Constipation: Bowel habits can be affected.
- Abdominal Pain: Discomfort in the stomach area.
- Heartburn: A burning sensation in the chest.
These side effects are often dose-dependent and tend to improve over time as the body adapts. Strategies like starting with a low dose and gradually increasing it, eating smaller meals, and avoiding fatty or spicy foods can help mitigate these issues.
More serious, though less common, side effects can include:
- Pancreatitis: Inflammation of the pancreas.
- Gallstones: The formation of stones in the gallbladder.
- Kidney Problems: Particularly in individuals with pre-existing kidney issues.
- Thyroid Tumors: While seen in animal studies with some GLP-1 agonists, the risk in humans is considered low and a contraindication exists for individuals with a personal or family history of medullary thyroid carcinoma or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2).
- Allergic Reactions: As with any medication, severe allergic reactions are possible.
Close monitoring by a healthcare provider is essential to identify and manage any adverse events promptly. Regular check-ups, blood tests, and open communication about any symptoms are crucial for safe and effective treatment. The decision to use these medications is a personal one, requiring careful deliberation and consultation with medical professionals to ensure it aligns with individual health goals and risk tolerance.
