The intricate choreography of the human circulatory system relies on a precisely regulated flow of blood, a feat made possible by the remarkable efficiency of heart valves. These delicate yet robust structures act as one-way gates within the heart, ensuring that blood travels in the correct direction through the chambers and out to the rest of the body. Without their precise functioning, the heart’s ability to pump oxygenated blood to vital organs and remove deoxygenated blood would be severely compromised, leading to a cascade of physiological disruptions.
The main function of heart valves can be distilled into a singular, critical purpose: to prevent the backward flow of blood within the heart. This seemingly simple mechanism is fundamental to the heart’s role as a powerful and efficient pump. Imagine a series of one-way doors that open to allow blood to move forward and then snap shut to prevent it from returning. This prevents blood from sloshing back into the chamber it just left, thus maximizing the forward ejection of blood with each heartbeat. This unidirectional flow is essential for maintaining adequate blood pressure and ensuring that oxygenated blood reaches the body’s tissues without being diluted by deoxygenated blood, and vice-versa.
The Four Pillars of Unidirectional Flow: Anatomy and Purpose
The human heart is equipped with four primary valves, each strategically positioned to manage blood flow between its chambers and into the major arteries. These valves are not mere passive flaps; they are sophisticated biological structures composed of leaflets or cusps, supported by fibrous tissues and, in some cases, chordae tendineae and papillary muscles. Their coordinated opening and closing are governed by the pressure gradients within the heart chambers, a testament to the elegant engineering of the cardiovascular system.
The Atrioventricular (AV) Valves: Guardians of the Upper Chambers
The two valves located between the atria (the upper chambers) and the ventricles (the lower chambers) are known as the atrioventricular valves. Their primary role is to prevent blood from flowing backward from the ventricles into the atria during ventricular contraction.
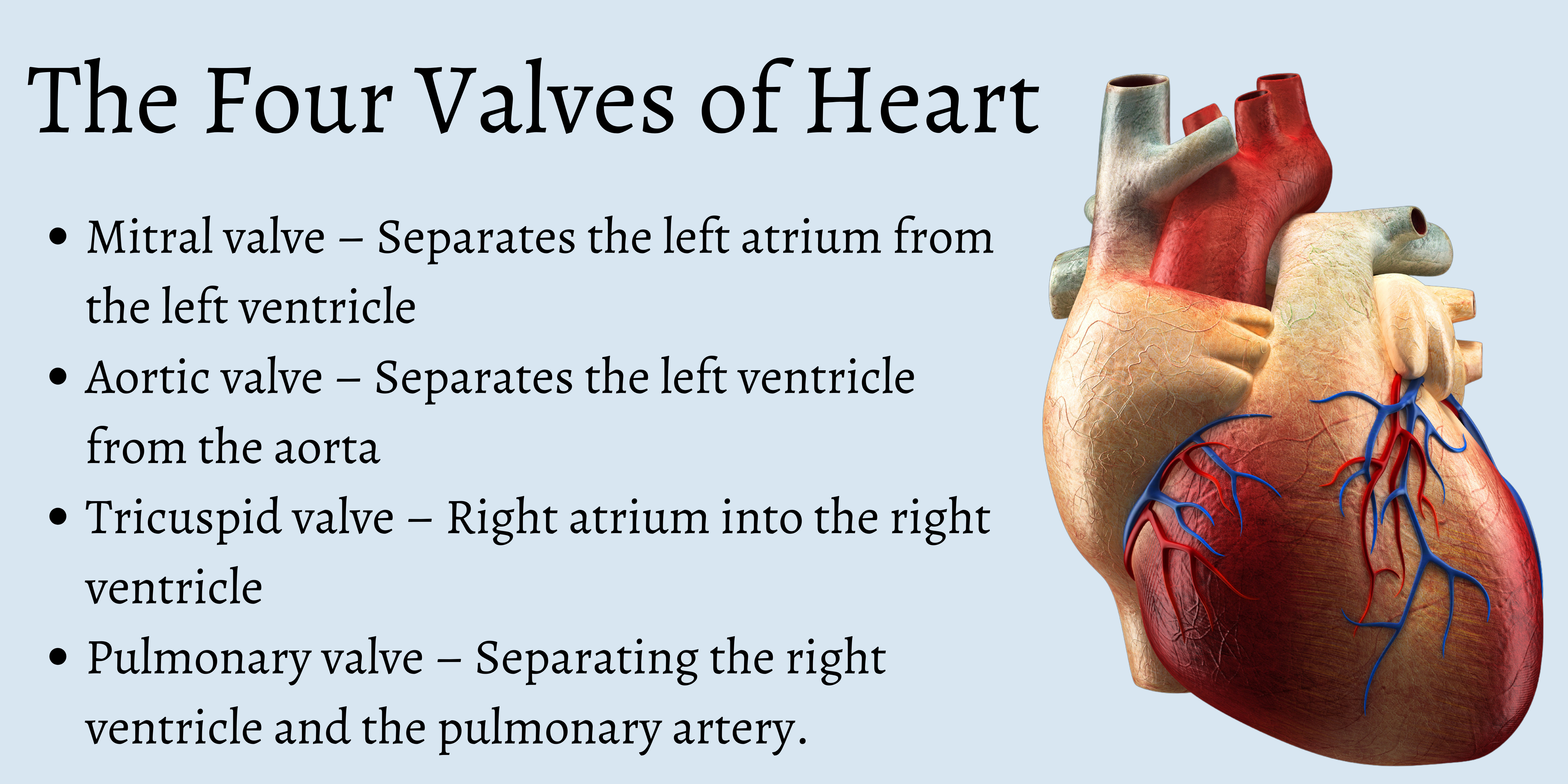
The Mitral Valve (Bicuspid Valve)
Situated between the left atrium and the left ventricle, the mitral valve is a critical component of the systemic circulation. It consists of two leaflets, hence its alternative name, the bicuspid valve. When the left atrium fills with oxygenated blood returning from the lungs, the mitral valve opens, allowing blood to flow into the left ventricle. As the left ventricle begins to contract, the pressure inside it rises sharply. This increase in pressure forces the mitral valve to snap shut, effectively sealing off the pathway back into the left atrium. This ensures that all the blood is forcefully ejected through the aortic valve into the aorta and subsequently to the rest of the body. The integrity of the mitral valve is paramount; a leaky or stenotic mitral valve can significantly impair the heart’s pumping efficiency and lead to serious health issues.
The Tricuspid Valve
Located between the right atrium and the right ventricle, the tricuspid valve serves a similar function for the pulmonary circulation. It comprises three leaflets. When the right atrium receives deoxygenated blood from the body, the tricuspid valve opens, allowing blood to enter the right ventricle. As the right ventricle contracts to pump blood to the lungs, the tricuspid valve closes firmly, preventing any backflow into the right atrium. This ensures that the deoxygenated blood is efficiently directed to the lungs for oxygenation.
The Semilunar (SL) Valves: Gatekeepers to the Arteries
The two valves located between the ventricles and the major arteries that carry blood away from the heart are called the semilunar valves. They are responsible for preventing the backflow of blood from these arteries into the ventricles after they have been emptied.
The Aortic Valve
Positioned between the left ventricle and the aorta, the largest artery in the body, the aortic valve is a vital conduit for oxygenated blood. It consists of three cusps, which resemble small pockets. When the left ventricle contracts and its pressure exceeds that of the aorta, the aortic valve opens, allowing the surge of oxygenated blood to be pumped into the aorta. Immediately after the ventricle relaxes and its pressure falls below that of the aorta, the cusps fill with blood and coapt (close together), effectively preventing blood from flowing back into the left ventricle. This rapid and efficient closure is crucial for maintaining arterial blood pressure and ensuring continuous blood supply to the body.
The Pulmonary Valve
Found between the right ventricle and the pulmonary artery, which carries deoxygenated blood to the lungs, the pulmonary valve also has three cusps. Similar to the aortic valve, it opens when the right ventricle contracts, allowing deoxygenated blood to be propelled into the pulmonary artery towards the lungs. Upon ventricular relaxation, the pulmonary valve closes to prevent blood from returning to the right ventricle, ensuring that the blood is directed solely for gas exchange in the lungs.
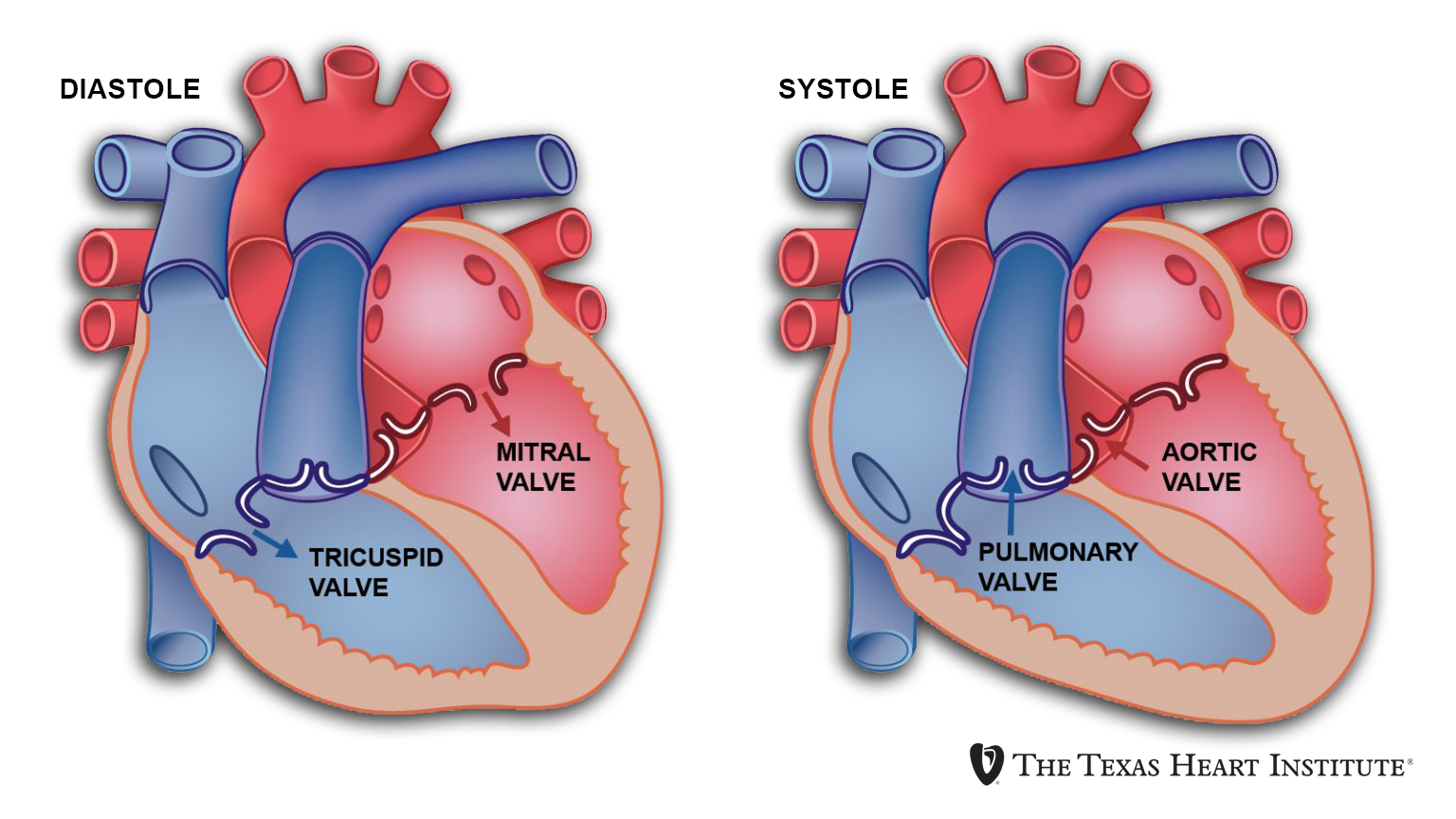
The Dynamics of Valve Function: A Symphony of Pressure and Mechanics
The opening and closing of heart valves are not voluntary actions but rather passive events dictated by the dynamic pressure changes within the heart chambers. This intricate process is a marvel of biomechanical engineering.
Pressure Gradients as the Driving Force
The fundamental principle governing valve action is the pressure gradient. When the pressure in a chamber behind a valve exceeds the pressure in the chamber or vessel in front of it, the valve opens. Conversely, when the pressure in front of the valve becomes higher than the pressure behind it, the valve closes. This simple yet elegant mechanism ensures that blood always flows from an area of higher pressure to an area of lower pressure.
For instance, during ventricular diastole (relaxation), the pressure in the atria is higher than in the ventricles, causing the AV valves to open and fill the ventricles. As the ventricles begin to contract during systole (contraction), the ventricular pressure rapidly increases, exceeding the atrial pressure and forcing the AV valves to close. Simultaneously, as the ventricular pressure rises above the pressure in the aorta and pulmonary artery, the semilunar valves open, allowing blood to be ejected. Once the ventricles begin to relax, the pressure in the aorta and pulmonary artery becomes higher than in the ventricles, causing the semilunar valves to close.
The Role of Chordae Tendineae and Papillary Muscles
In the case of the atrioventricular valves (mitral and tricuspid), the leaflets are tethered by strong, fibrous cords called chordae tendineae. These are attached to cone-shaped muscles projecting from the ventricular walls, known as papillary muscles. The primary function of these structures is to prevent the valve leaflets from prolapsing (bending backward) into the atria during ventricular contraction. When the ventricles contract, the papillary muscles also contract, creating tension on the chordae tendineae. This tension pulls on the valve leaflets, keeping them taut and preventing them from inverting, much like parachute cords prevent a parachute from collapsing. Without the support of the chordae tendineae and papillary muscles, the high pressures generated during ventricular systole would force the AV valves to bulge backward into the atria, leading to significant blood leakage.
The Consequences of Valve Malfunction: When the Gates Fail
The heart valves are designed for longevity and repeated cycles of opening and closing, but like any mechanical system, they can be subject to wear and tear or damage. When valves do not function correctly, the heart’s ability to pump blood effectively is compromised, leading to a range of cardiovascular conditions.
Regurgitation (Insufficiency or Leakage)
Valve regurgitation occurs when a valve fails to close properly, allowing blood to flow backward into the chamber it originated from. This means that a portion of the blood pumped by the heart is not propelled forward to the body or lungs, necessitating the heart to work harder to compensate. Conditions such as mitral regurgitation, aortic regurgitation, tricuspid regurgitation, and pulmonary regurgitation can arise from various causes, including damage to the valve leaflets, problems with the supporting structures (chordae tendineae, papillary muscles), or dilation of the heart chambers that stretches the valve annulus (the ring to which the valve is attached).
Stenosis (Narrowing)
Valve stenosis refers to a condition where a valve becomes narrowed or stiffened, impeding the normal flow of blood through it. This forces the heart to pump blood against increased resistance. For example, aortic stenosis means the aortic valve is narrowed, making it difficult for the left ventricle to pump blood into the aorta. This increased workload can lead to hypertrophy (thickening) of the ventricular muscle, ultimately weakening the heart over time. Stenosis can be caused by age-related calcification, rheumatic heart disease, congenital defects, or other inflammatory processes.
Prolapse
Mitral valve prolapse is a common condition where the leaflets of the mitral valve bulge backward into the left atrium during ventricular contraction. In many cases, mitral valve prolapse is a benign condition with no symptoms. However, in more severe cases, it can lead to mitral regurgitation, as the prolapsed leaflets may not coapt properly.
Conclusion: The Silent Sentinels of Cardiovascular Health
In essence, the main function of heart valves is to meticulously manage the direction and efficiency of blood flow within the heart. They are the silent sentinels that ensure the unidirectional movement of blood, a process that is absolutely critical for maintaining life. Their precise opening and closing, dictated by the subtle yet powerful shifts in blood pressure and supported by complex anatomical structures, enable the heart to perform its vital pumping role. When these valves falter, the entire cardiovascular system is affected, underscoring their profound importance in overall health and well-being. Understanding their function is key to appreciating the remarkable complexity and resilience of the human heart.
