The human body is a marvel of biological engineering, capable of incredible feats of resilience and repair. When faced with injury, it mobilizes a complex cascade of cellular events to mend itself. But not all parts of the body heal at the same rate. The speed and efficacy of healing are influenced by numerous factors, including blood supply, cell turnover rate, and the presence of essential nutrients. Understanding which parts heal fastest can offer insights into our overall health and the remarkable regenerative power inherent within us.
The Mouth: A Surprisingly Rapid Healer
The oral cavity, encompassing the gums, tongue, and the lining of the cheeks, is remarkably adept at healing. This is primarily due to a rich blood supply and a high rate of cell regeneration. The cells that line the mouth are constantly shedding and being replaced, a process that significantly speeds up wound closure and tissue repair.

Gums and Soft Tissues
Injuries to the gums, such as those from accidental bites or dental procedures, typically heal within a matter of days to a couple of weeks. The rich vascularization of the gingival tissue ensures a constant flow of oxygen and nutrients to the injured site, facilitating the inflammatory and proliferative phases of healing. Fibroblasts, crucial cells for collagen production, are abundant in this region, laying down new tissue rapidly. Even minor cuts and abrasions on the inside of the cheeks or lips often close and resolve much faster than similar injuries on the skin.
The Tongue
The tongue, while highly mobile and subjected to constant friction, also possesses exceptional healing capabilities. Its extensive network of blood vessels supports rapid regeneration. Minor nicks or burns on the tongue can often feel better within hours and be fully healed within a week. The constant moisture in the mouth also contributes to a more favorable healing environment compared to drier external tissues.
Factors Influencing Oral Healing
While the mouth is a fast healer, certain factors can impede this process. Poor oral hygiene can introduce bacteria, increasing the risk of infection and delaying healing. Conditions like diabetes can also impair the body’s ability to repair tissues effectively, even in the mouth. Smoking is another significant detriment, reducing blood flow and hindering the delivery of essential healing factors. Nevertheless, in the absence of these complicating factors, the oral cavity stands out as a champion of rapid regeneration.
The Liver: A Regenerative Powerhouse
The liver is arguably the most impressive organ when it comes to regeneration. It possesses an extraordinary capacity to regrow after significant damage, a trait that has made liver transplants possible even with partial donations. This remarkable ability stems from the unique nature of its cells and their inherent capacity for replication.
Hepatocyte Replication
The primary cells of the liver, hepatocytes, are capable of dividing and multiplying even in adult mammals. When a portion of the liver is removed, either through surgery (hepatectomy) or disease, the remaining hepatocytes can increase in size and number to compensate for the loss. This regenerative process can restore the liver to its original size and function within weeks to months, depending on the extent of the damage.
The Role of the Microenvironment
The intricate structure of the liver, with its specialized connective tissue framework and unique vascular system, plays a crucial role in supporting this regenerative capacity. This microenvironment provides signals and scaffolding that guide the proliferation and organization of new hepatocytes, ensuring that the regenerated tissue is functional.
Limits to Regeneration
While the liver’s regenerative potential is vast, it is not limitless. Chronic, long-term damage, such as that caused by viral hepatitis or excessive alcohol consumption, can lead to cirrhosis. In cirrhosis, the continuous scarring and inflammation overwhelm the liver’s ability to regenerate effectively, leading to irreversible damage and loss of function. However, for acute injuries, the liver’s capacity to heal itself is unparalleled.
Fingernails and Hair: Continuous Growth and Repair

While not “healing” in the sense of repairing an injury, fingernails and hair are constantly growing and replacing themselves, showcasing a continuous form of tissue renewal. This perpetual growth cycle means that any damage to these structures is eventually shed and replaced by new, healthy material.
Fingernail Regeneration
Fingernails grow from the nail matrix, a region of actively dividing cells located at the base of the nail. This growth is relatively slow, with fingernails growing at an average rate of about 3.5 millimeters per month. If a fingernail is damaged or lost, the new nail will gradually grow out. The speed of this regrowth is influenced by factors such as age, diet, and overall health. While not a rapid “healing” event, the continuous replacement of nail tissue means that any damage is eventually resolved.
Hair Follicle Cycles
Hair, similarly, grows from follicles embedded in the skin. Each hair follicle goes through a cycle of growth (anagen), transition (catagen), and resting (telogen). This cycle allows for continuous renewal of the hair shaft. While hair loss can be concerning, the follicles themselves remain, capable of producing new hair. If a hair is broken or cut, it will eventually be replaced by new growth. The speed of hair growth is slower than that of nails, averaging about 0.5 inches per month.
Bone: A Remarkable Repair Mechanism
Bone is a dynamic tissue that, while appearing static, is constantly undergoing remodeling. When fractured, bone possesses an impressive ability to repair itself, a process that involves several distinct stages. The speed of bone healing is highly dependent on the type and severity of the fracture, as well as the individual’s age and overall health.
Stages of Bone Healing
- Hematoma Formation: Immediately after a fracture, blood vessels within the bone and surrounding tissues are torn, leading to bleeding and the formation of a hematoma (blood clot) at the fracture site. This hematoma provides a scaffold for the subsequent healing process.
- Soft Callus Formation: Within days, inflammatory cells clean up the debris, and granulation tissue, rich in new blood vessels and fibroblasts, begins to form. This develops into a soft callus, a fibrocartilaginous mass that bridges the gap between the broken bone ends.
- Hard Callus Formation: Over the next few weeks, the soft callus is gradually replaced by woven bone, forming a hard callus. This callus provides initial stability to the fracture site.
- Bone Remodeling: In the final stage, the woven bone is gradually replaced by stronger lamellar bone, and the excess callus is remodeled to restore the original shape and strength of the bone. This remodeling process can take months to years.
Factors Influencing Bone Healing Speed
The excellent blood supply to most bones is a key factor in their ability to heal. However, certain bones, such as the scaphoid in the wrist, have a more limited blood supply, leading to slower healing and a higher risk of non-union. Age is another significant factor; children’s bones heal much faster than those of adults. Proper immobilization of the fracture through casts or surgical fixation is crucial to allow the healing process to occur undisturbed. Nutritional status, particularly adequate intake of calcium, vitamin D, and protein, also plays a vital role in bone repair.
The Skin: A Constant Battleground of Repair
The skin, our largest organ, is constantly exposed to the environment and thus frequently sustains minor injuries. Its remarkable ability to heal efficiently is crucial for survival, preventing infection and maintaining bodily integrity. The skin’s healing process is a complex, multi-stage event that varies depending on the depth of the wound.
Superficial Wounds (Epidermal and Superficial Dermal)
Minor cuts, abrasions, and scrapes that involve only the epidermis (the outermost layer) or the superficial dermis heal very quickly. The epidermal cells at the wound edges proliferate and migrate across the wound bed, effectively closing the gap. This process can occur within a few days, with minimal or no scarring. The presence of a moist wound environment, often maintained by wound dressings, can significantly accelerate this type of healing by facilitating cell migration and reducing inflammation.
Deeper Wounds (Partial and Full Thickness)
Deeper wounds that extend into the dermis or involve the subcutaneous tissue require a more complex healing response. This involves inflammation, proliferation (formation of granulation tissue and new blood vessels), and remodeling (collagen deposition and maturation). While these deeper wounds take longer to heal, often weeks or months, the skin’s regenerative capacity is still impressive. Full-thickness wounds may require the formation of scar tissue, as the dermis has a limited capacity to regenerate completely.
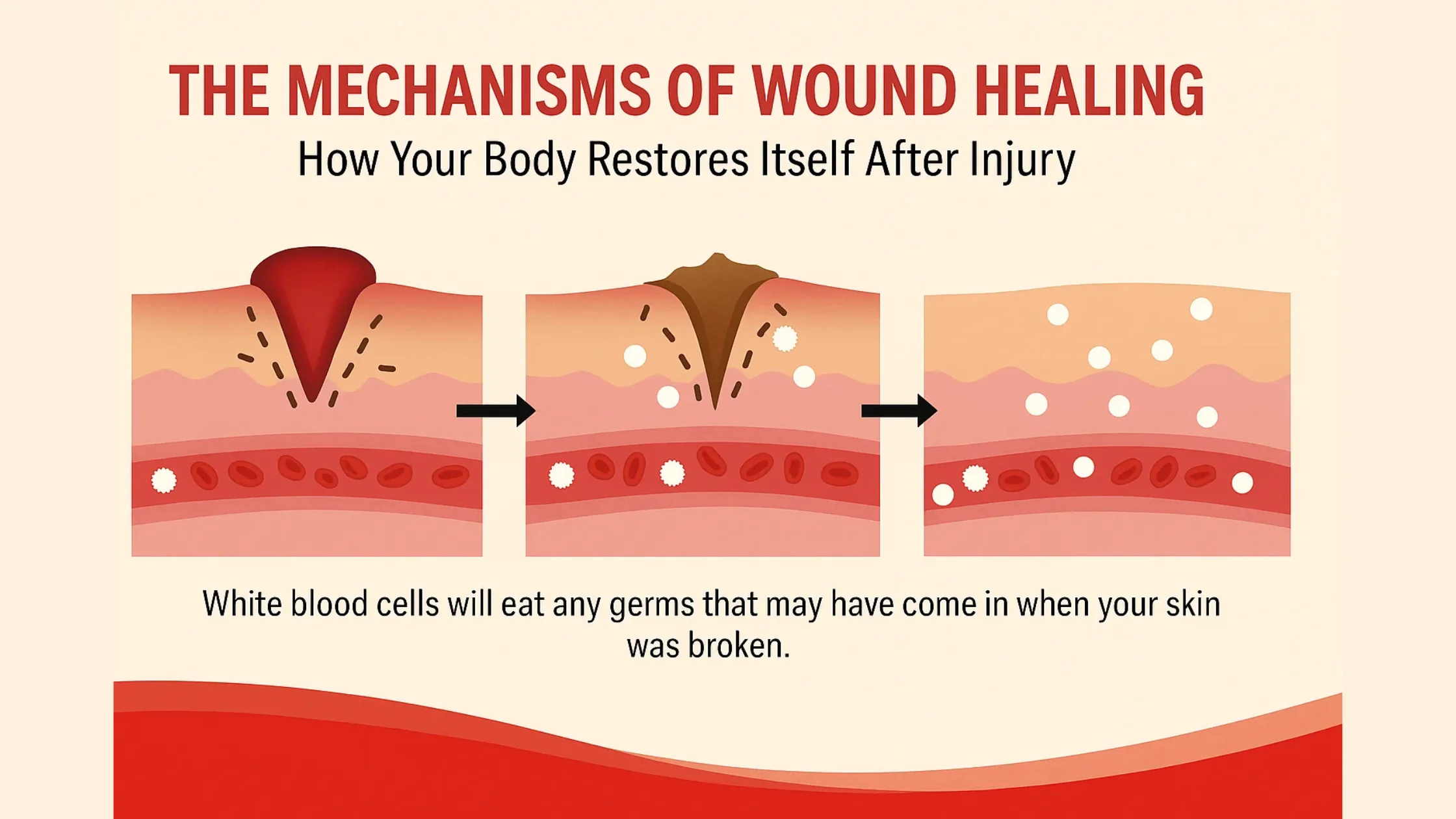
Factors Affecting Skin Healing
Similar to other tissues, skin healing is influenced by blood supply, nutrition, age, and the presence of underlying medical conditions like diabetes or circulatory problems. Infection is a major impediment to skin healing, dramatically slowing down the process and increasing the risk of complications. Chronic wounds, such as pressure ulcers or diabetic foot ulcers, often heal poorly due to a combination of impaired blood flow, increased inflammation, and altered cellular function. However, for acute injuries in healthy individuals, the skin’s ability to mend itself is a testament to its remarkable regenerative power.
