Pneumonia, an infection that inflames the air sacs in one or both lungs, is a condition that can range in severity from mild to life-threatening. When discussing pneumonia, two common terms emerge: “walking pneumonia” and “regular pneumonia.” While both refer to an infection of the lungs, the distinction lies primarily in the severity of symptoms and the causative agent. Understanding these differences is crucial for appropriate diagnosis, treatment, and patient care.
Understanding Pneumonia: The Basics
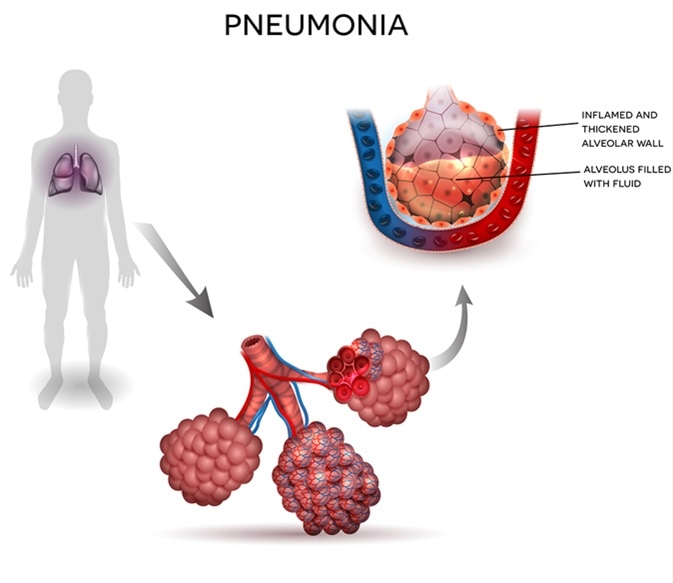
Pneumonia is an umbrella term for a lung infection. The air sacs in the lungs, called alveoli, typically fill with air when you breathe in. However, when someone has pneumonia, these alveoli may fill with fluid or pus. This inflammation and fluid accumulation make breathing difficult and can impair oxygen exchange in the lungs.

Causes of Pneumonia
Pneumonia can be caused by a variety of pathogens, including bacteria, viruses, and fungi.
Bacterial Pneumonia
Bacterial pneumonia is a common cause of the illness. Streptococcus pneumoniae is one of the most frequent bacterial culprits. Bacterial infections often lead to more severe symptoms and may require antibiotic treatment.
Viral Pneumonia
Viruses, such as influenza, respiratory syncytial virus (RSV), and coronaviruses (including SARS-CoV-2), can also cause pneumonia. Viral pneumonia can sometimes be less severe than bacterial pneumonia, but it can also lead to serious complications, especially in vulnerable populations like young children and the elderly.
Fungal Pneumonia
Fungal pneumonia is less common in healthy individuals and typically affects people with weakened immune systems, such as those with HIV/AIDS or undergoing chemotherapy.
How Pneumonia Affects the Lungs
The inflammatory response triggered by the infection leads to the alveoli filling with exudate – a mixture of fluid, inflammatory cells, and sometimes pus. This exudate obstructs the normal flow of air and reduces the surface area available for gas exchange. Consequently, the body receives less oxygen, leading to symptoms like shortness of breath and a lower oxygen saturation level in the blood.
Walking Pneumonia: A Milder Form
Walking pneumonia, also known as atypical pneumonia, is a colloquial term used to describe a milder form of pneumonia. The name “walking pneumonia” stems from the fact that individuals experiencing it may be able to continue with their daily activities, including walking, despite being infected. This is in contrast to more severe forms of pneumonia where rest and hospitalization might be necessary.
Characteristics of Walking Pneumonia
The hallmark of walking pneumonia is its less severe presentation. While symptoms are present, they are generally not debilitating enough to confine the individual to bed.
Mild Symptoms
Common symptoms of walking pneumonia can include:
- Cough: Often persistent and dry, though it may produce some mucus.
- Sore Throat: A common accompanying symptom.
- Headache: A dull or throbbing headache may be present.
- Fatigue: A general feeling of tiredness or lack of energy.
- Low-grade Fever: The fever, if present, is typically not very high.
- Chest Discomfort: A mild soreness or discomfort in the chest, often associated with coughing.
Atypical Pathogens
Walking pneumonia is often caused by pathogens that differ from those responsible for typical bacterial pneumonia. Mycoplasma pneumoniae is a very common cause of walking pneumonia. This bacterium lacks a cell wall, making it resistant to certain antibiotics that target cell walls. Other atypical pathogens include Chlamydophila pneumoniae and certain viruses.
Diagnosis and Treatment of Walking Pneumonia
Diagnosing walking pneumonia can sometimes be challenging due to its subtle symptoms, which can mimic other respiratory infections like the common cold or bronchitis.
Diagnostic Approaches
- Physical Examination: A doctor will listen to the lungs with a stethoscope. While crackles or diminished breath sounds might be present, they may be less pronounced than in severe pneumonia.
- Chest X-ray: A chest X-ray is often the most definitive diagnostic tool. In walking pneumonia, the infiltrates (areas of inflammation and fluid) seen on the X-ray are often more diffuse and less dense compared to those seen in lobar pneumonia (a more severe form affecting a whole lobe of the lung).
- Symptom Assessment: The patient’s history and reported symptoms play a crucial role in the diagnostic process.
Treatment Strategies
Treatment for walking pneumonia typically focuses on symptom relief and targeting the specific pathogen if identified.
- Antibiotics: If a bacterial cause like Mycoplasma pneumoniae is suspected or confirmed, antibiotics that are effective against these types of bacteria will be prescribed. It’s important to note that standard antibiotics for typical bacterial pneumonia might not be effective for walking pneumonia caused by atypical organisms.
- Rest and Hydration: Adequate rest and fluid intake are essential for recovery.
- Over-the-Counter Medications: Medications to alleviate cough and fever can be used as needed.
Regular Pneumonia: More Severe Presentations
The term “regular pneumonia” is often used to encompass more severe forms of pneumonia, typically those caused by more common bacterial pathogens or presenting with more pronounced symptoms requiring more intensive medical attention. While the lines can be blurred, regular pneumonia generally implies a greater degree of lung inflammation and a more significant impact on a person’s ability to function.
Manifestations of Regular Pneumonia
The symptoms of regular pneumonia are typically more intense and debilitating, directly impacting the respiratory system’s ability to function effectively.
Pronounced Symptoms
- High Fever: Often accompanied by chills and sweating.
- Severe Cough: May produce thick, discolored mucus (yellow, green, or even bloody).
- Shortness of Breath: Significant difficulty breathing, even at rest.
- Chest Pain: Sharp or stabbing pain in the chest, which may worsen with breathing or coughing.
- Fatigue and Weakness: Extreme exhaustion that limits daily activities.
- Confusion or Altered Mental State: Particularly in older adults.
- Nausea and Vomiting: May occur, especially in children.
Common Pathogens
While viruses can cause severe pneumonia, many cases of what is considered “regular pneumonia” are bacterial. Streptococcus pneumoniae remains a leading cause of bacterial pneumonia. Other common bacterial culprits include Haemophilus influenzae, Klebsiella pneumoniae, and Staphylococcus aureus.
Medical Management and Prognosis
The severity of symptoms in regular pneumonia often necessitates a more aggressive medical approach and can lead to a longer recovery period.
Diagnostic Rigor
- Medical History and Physical Exam: A thorough assessment is conducted, listening for characteristic lung sounds like crackles or bronchial breathing.
- Chest X-ray: In regular pneumonia, X-rays often reveal more extensive consolidations or infiltrates within the lung tissue, sometimes affecting entire lobes.
- Blood Tests: Complete blood count (CBC) and C-reactive protein (CRP) levels can indicate the presence and severity of infection.
- Sputum Culture: Analyzing mucus samples can help identify the specific bacterial pathogen and determine its sensitivity to various antibiotics, guiding treatment.
- Pulse Oximetry: This non-invasive test measures blood oxygen levels, which are often significantly lower in severe pneumonia.
Treatment and Recovery
Treatment for regular pneumonia is tailored to the identified pathogen and the patient’s overall health.
- Antibiotics: For bacterial pneumonia, a course of antibiotics is crucial. The type and duration of antibiotics will depend on the identified bacteria and its resistance patterns. Intravenous antibiotics may be necessary in severe cases.
- Antiviral or Antifungal Medications: If a viral or fungal cause is identified, specific antiviral or antifungal drugs will be prescribed.
- Hospitalization: Severe cases of pneumonia, particularly those with significant respiratory distress, low oxygen levels, or complications, may require hospitalization. This allows for close monitoring, administration of intravenous medications, and respiratory support (e.g., oxygen therapy, mechanical ventilation).
- Supportive Care: This includes managing fever, pain, and ensuring adequate hydration.
Key Distinctions and When to Seek Medical Advice
While both walking pneumonia and regular pneumonia are lung infections, the differences in their presentation and the potential for complications are significant. Early recognition and appropriate medical care are paramount for successful recovery.
Summarizing the Differences
The primary distinctions between walking pneumonia and regular pneumonia can be summarized as follows:
| Feature | Walking Pneumonia | Regular Pneumonia |
|---|---|---|
| Symptom Severity | Mild to moderate; individuals can often remain ambulatory. | Moderate to severe; symptoms often debilitating, requiring rest and potentially hospitalization. |
| Onset | Gradual and subtle. | Often more abrupt and pronounced. |
| Fever | Low-grade or absent. | High fever, often with chills. |
| Cough | Persistent, often dry, sometimes with minimal mucus. | Severe, often producing thick, discolored mucus. |
| Shortness of Breath | Mild, if present. | Significant, even at rest. |
| Chest Pain | Mild discomfort. | Sharp, stabbing pain, often worse with breathing. |
| Pathogens | Often atypical bacteria (e.g., Mycoplasma pneumoniae, Chlamydophila pneumoniae) or viruses. | Common bacteria (e.g., Streptococcus pneumoniae) or more virulent viruses. |
| X-ray Findings | Diffuse, less dense infiltrates. | Dense consolidations, potentially affecting entire lobes. |
| Prognosis | Generally good with appropriate treatment. | Can be more serious, with a higher risk of complications and longer recovery. |

The Importance of Professional Diagnosis
It is crucial to emphasize that self-diagnosis of pneumonia is not recommended. The symptoms of walking pneumonia can be easily mistaken for other, less serious respiratory illnesses. Similarly, downplaying symptoms of what might be regular pneumonia can lead to delayed treatment and potential complications.
When to Seek Medical Advice:
- Persistent Cough: Especially if it’s producing colored mucus or is accompanied by chest pain.
- Difficulty Breathing: Any significant shortness of breath requires immediate medical attention.
- High Fever: A fever of 102°F (39°C) or higher, or a fever that doesn’t respond to over-the-counter medication.
- Chest Pain: Particularly if it’s sharp or worsens with breathing.
- Confusion or Drowsiness: This can be a sign of a severe infection, especially in older adults.
- Worsening Symptoms: If your symptoms are not improving or are getting worse, consult a healthcare professional.
Healthcare providers are equipped with the tools and knowledge to accurately diagnose pneumonia, differentiate between its various forms, and initiate the most effective treatment plan. This ensures prompt recovery and minimizes the risk of potential complications.
