The quest for understanding and improving human health has always been a fertile ground for technological advancement. Among the myriad of conditions that impact quality of life, sleep disorders, particularly sleep apnea, have emerged as significant areas of focus for innovation. While the medical diagnosis of sleep apnea has traditionally relied on established protocols, the underlying technology employed in modern testing is a testament to the strides made in Tech & Innovation. This article delves into the technological underpinnings of what constitutes a sleep apnea test, exploring the sensors, data processing, and advanced methodologies that are revolutionizing how this condition is identified and managed. We will move beyond the clinical definition to appreciate the sophisticated systems that gather and interpret the vital data points necessary for an accurate diagnosis.
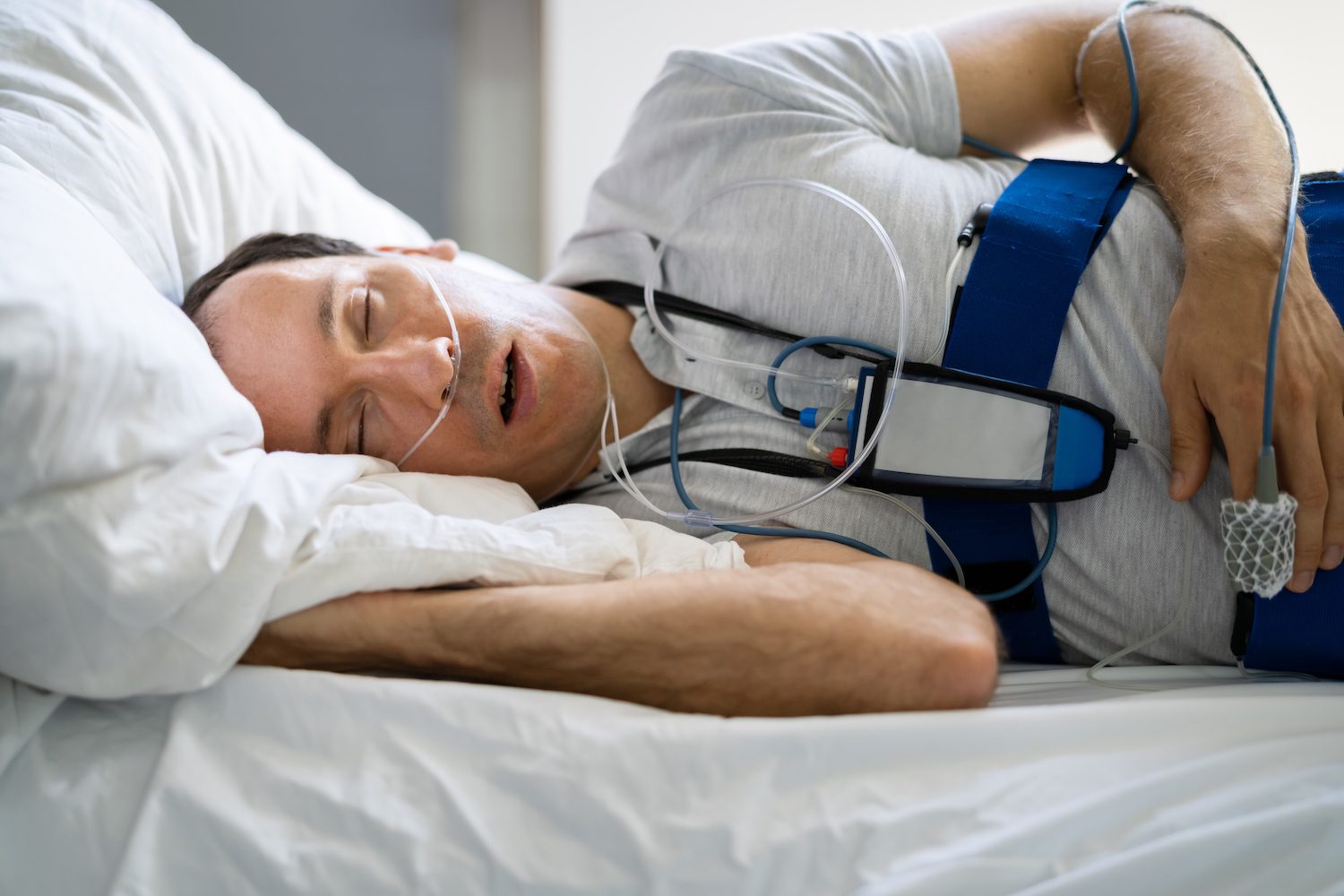
The Technological Core: Sensors and Data Acquisition
At the heart of any advanced sleep apnea test lies a suite of miniaturized, highly sensitive sensors designed to capture a comprehensive picture of physiological activity during sleep. These sensors are not merely passive collectors of information; they represent a confluence of engineering and biomedical science, meticulously crafted to withstand the rigors of overnight monitoring while providing precise, real-time data. The innovation in this space lies in the integration, miniaturization, and improved accuracy of these components, enabling more comfortable, convenient, and definitive testing.
Respiratory Monitoring Technologies
The defining characteristic of sleep apnea is the disruption of breathing. Therefore, respiratory monitoring forms the cornerstone of any sleep apnea test. Historically, this involved bulky equipment, but modern tests leverage advanced sensing technologies.
- Airflow Sensors: These devices, often integrated into nasal cannulas or masks, measure the subtle changes in airflow during breathing. Innovations include thermistor-based sensors that detect temperature differences between inhaled and exhaled air, and pressure transducers that can quantify the volume and rate of airflow. The precision of these sensors is crucial for identifying the characteristic cessation or reduction in airflow that defines apneic events. Newer designs are often wireless and unobtrusive, enhancing patient comfort and compliance.
- Thoracic and Abdominal Belts: These flexible belts, worn around the chest and abdomen, utilize strain gauges or inductive plethysmography to measure the effort and pattern of breathing. Strain gauges detect changes in belt circumference, indicating chest and abdominal expansion and contraction. Inductive plethysmography uses coils that change their electrical inductance as they expand or contract. The data from these belts helps differentiate between central sleep apnea (where breathing effort ceases) and obstructive sleep apnea (where breathing effort continues despite airway blockage). The innovation here is in the development of soft, comfortable, and highly responsive materials that ensure accurate readings without disturbing sleep.
- Oximetry: Blood oxygen saturation (SpO2) is a critical indicator of respiratory compromise. Pulse oximeters, typically a clip worn on a finger or earlobe, use light wavelengths to measure the amount of oxygen carried by hemoglobin in the blood. Advanced oximeters in sleep apnea testing are designed for continuous, high-fidelity readings, capable of detecting rapid drops in oxygen levels that can accompany apneic events. Innovations include improved algorithms to minimize artifact from movement and enhanced battery life for extended monitoring.
Physiological Parameter Sensors
Beyond direct respiratory monitoring, understanding the body’s overall response to disrupted breathing is vital. This involves capturing a range of physiological signals that can be correlated with sleep apnea events.
- Electrocardiogram (ECG) Leads: Small, adhesive electrodes placed on the skin record the electrical activity of the heart. This allows for monitoring heart rate, heart rate variability, and the detection of cardiac arrhythmias that can be exacerbated by sleep apnea. The technological leap here is in the development of dry electrodes that do not require skin preparation and offer superior signal quality with minimal discomfort, facilitating easier application and longer wear.
- Electroencephalogram (EEG) Sensors: While more common in in-lab polysomnography, simplified EEG sensors are increasingly integrated into home sleep apnea tests. These sensors, often embedded in headbands or caps, monitor brain wave activity to determine sleep stages. Accurate sleep staging is crucial because the severity and type of sleep apnea can vary significantly between different sleep stages. Innovations in wireless EEG technology and advanced signal processing algorithms have made these measurements more accessible for home use.
- Electromyogram (EMG) Sensors: EMG sensors, typically placed on the chin or legs, detect muscle activity. This helps identify leg movements that might disrupt sleep and indicate restless legs syndrome, a common co-occurring sleep disorder. Disposable, pre-gelled EMG electrodes have significantly improved user experience and data quality for home testing.
Data Processing and Analytical Innovations
The sheer volume of data collected by these sensors overnight would be overwhelming without sophisticated processing and analytical capabilities. This is where Tech & Innovation truly shines, transforming raw physiological signals into actionable diagnostic insights. The development of intelligent algorithms and powerful processing units has moved sleep apnea testing from a purely observational science to a data-driven diagnostic discipline.
Real-time Signal Processing and Artifact Rejection
Modern sleep apnea testing devices are equipped with on-board processors capable of performing complex signal processing in real-time. This is essential for several reasons:
- Noise Reduction: Physiological signals can be corrupted by noise from movement, environmental factors, or electrical interference. Advanced algorithms employ filtering techniques, spectral analysis, and adaptive filtering to isolate the true physiological signals from this noise.
- Event Detection Algorithms: Sophisticated algorithms are designed to automatically detect the hallmark events of sleep apnea, such as apneas (complete cessation of breathing), hypopneas (partial reduction in breathing), and respiratory effort related arousals. These algorithms analyze patterns in airflow, oxygen saturation, and respiratory effort data to identify these events with high accuracy.
- Artifact Management: Movement artifacts are a common challenge in sleep monitoring. Innovative techniques, including machine learning models trained on large datasets, are employed to identify and correct or flag data points contaminated by movement, ensuring the integrity of the diagnostic information. The ability to differentiate between true physiological events and artifacts is a key area of ongoing innovation.
Machine Learning and Artificial Intelligence in Diagnosis
The integration of Machine Learning (ML) and Artificial Intelligence (AI) is revolutionizing sleep apnea diagnostics, moving beyond simple rule-based event detection.
- Pattern Recognition: ML algorithms can be trained on vast datasets of polysomnography recordings to recognize complex patterns in physiological data that are indicative of sleep apnea, even those that might be missed by traditional scoring methods. This allows for a more nuanced and potentially earlier diagnosis.
- Personalized Risk Stratification: AI can analyze a patient’s complete data profile, including demographics, symptom questionnaires, and physiological readings, to provide a more personalized risk assessment for sleep apnea and its severity. This can help prioritize individuals for further testing and treatment.
- Automated Scoring and Reporting: While human scoring of sleep studies remains the gold standard, AI is increasingly being used to automate parts of the scoring process, flagging potential events for review by a sleep technician or physician. This can significantly reduce the time and cost associated with diagnosis. The ongoing development of AI models aims to improve accuracy and reduce the need for extensive manual review, making diagnosis more efficient and accessible.
Cloud-Based Data Management and Remote Analysis
The advent of cloud computing has transformed how sleep apnea test data is stored, accessed, and analyzed.

- Secure Data Transmission: Devices now routinely transmit encrypted data wirelessly to secure cloud platforms. This eliminates the need for physical data transfer and allows for immediate access by healthcare professionals.
- Remote Monitoring and Telemedicine: Cloud-based systems enable remote monitoring of patients, allowing healthcare providers to track progress and adjust treatment plans without requiring in-person visits. This is particularly beneficial for patients in remote areas or those with mobility issues.
- Big Data Analytics: The aggregated data from numerous sleep apnea tests stored in the cloud provides an invaluable resource for researchers. Big data analytics can identify new trends, risk factors, and potential therapeutic targets, driving further Tech & Innovation in the field.
The Evolution Towards Home Sleep Apnea Testing (HSAT)
One of the most significant technological advancements in sleep apnea testing has been the transition from hospital-based polysomnography (PSG) to Home Sleep Apnea Testing (HSAT). This shift has been driven by innovation in sensor miniaturization, wireless connectivity, user-friendly interfaces, and robust data processing.
Miniaturization and Wearable Technology
The drive towards HSAT has necessitated the development of smaller, more comfortable, and easier-to-use devices.
- Compact Devices: Modern HSAT devices are often pocket-sized, containing all the necessary sensors and processing units. They are designed to be worn comfortably throughout the night with minimal disruption to sleep.
- Integrated Sensors: Many HSAT devices integrate multiple sensors into a single unit, reducing the number of wires and attachments required. This often includes airflow, oxygen saturation, and sometimes even basic ECG and snoring microphones.
- Wireless Connectivity: Bluetooth and Wi-Fi capabilities allow devices to seamlessly transmit data to a patient’s smartphone or directly to a cloud server, simplifying the data collection process and eliminating the need for manual data downloads.
User Experience and Accessibility
Technological innovations have also focused on making sleep apnea testing more accessible and less intimidating for patients.
- Intuitive Interfaces: Many HSAT devices are designed with simple, user-friendly interfaces, often controlled via a companion smartphone app. This guides patients through the setup process and provides feedback on their data collection.
- Reduced Polysomnography Requirements: While full PSG is still the gold standard for complex cases, HSAT devices are increasingly capable of accurately diagnosing moderate to severe obstructive sleep apnea in uncomplicated patients, significantly increasing accessibility to diagnosis and treatment.
- Patient Education and Engagement: Apps and online platforms associated with HSAT devices can provide patients with educational resources about sleep apnea and their test results, fostering greater engagement in their own health management.
The Role of Smart Devices in Sleep Monitoring
The proliferation of consumer-grade smart devices has also contributed to the broader technological landscape of sleep monitoring. While not typically diagnostic sleep apnea tests themselves, these devices often incorporate sensors that can track sleep duration, movement, and sometimes even breathing patterns.
- Early Detection and Awareness: These consumer devices can act as an early warning system, alerting individuals to potential sleep disruptions that might warrant further investigation with a medical-grade sleep apnea test.
- Complementary Data: Data from smartwatches and fitness trackers can sometimes be used in conjunction with medical data, providing a more holistic view of a patient’s sleep habits and overall health.
- Driving Further Research: The widespread use of consumer sleep tracking technology has increased public awareness of sleep health and fueled demand for more accurate and accessible diagnostic tools, further spurring Tech & Innovation in the medical device sector.
The Future of Sleep Apnea Testing: Predictive and Proactive Technologies
The ongoing trajectory of Tech & Innovation in sleep apnea testing points towards a future where diagnosis is not only more accurate and accessible but also more predictive and proactive. The integration of advanced analytics, novel sensing modalities, and personalized medicine approaches promises to transform how sleep apnea is managed.
Predictive Analytics and Early Intervention
- AI-Powered Risk Prediction: Beyond diagnosing existing conditions, AI algorithms are being developed to predict an individual’s future risk of developing sleep apnea based on genetic predispositions, lifestyle factors, and early physiological markers. This could enable proactive interventions to mitigate risk.
- Continuous Monitoring and Trend Analysis: Future devices may offer continuous, unobtrusive monitoring of sleep patterns, allowing for the detection of subtle changes that might indicate the onset of sleep apnea long before symptoms become severe. This shifts the paradigm from reactive diagnosis to proactive health management.
Novel Sensing Modalities
- Non-Invasive Biosensors: Research is ongoing into non-invasive biosensors that can detect biochemical markers in sweat or exhaled breath related to sleep apnea, potentially offering an even simpler and more convenient diagnostic method.
- Advanced Wearable Integration: Further integration of sensors into everyday wearables, such as smart clothing or jewelry, could make sleep monitoring and even preliminary diagnosis a seamless part of daily life.

Personalized Treatment and Management
- Biomarker Identification: As our understanding of the complex interplay of factors contributing to sleep apnea grows, technological innovations will enable the identification of specific biomarkers that can predict an individual’s response to different treatment modalities, leading to more personalized and effective care.
- Closed-Loop Treatment Systems: The ultimate goal may involve closed-loop treatment systems where diagnostic devices are directly integrated with therapeutic devices, automatically adjusting treatment in real-time based on continuous physiological monitoring.
In conclusion, the “sleep apnea test” is far more than a simple medical procedure; it is a sophisticated integration of cutting-edge technology. From the intricate design of its sensors to the intelligent algorithms that process its data, every aspect of modern sleep apnea testing reflects significant advancements in Tech & Innovation. As these technologies continue to evolve, they promise to deliver more precise diagnoses, empower patients with better insights into their health, and ultimately pave the way for a future where sleep disorders are understood and managed with unprecedented efficacy.
