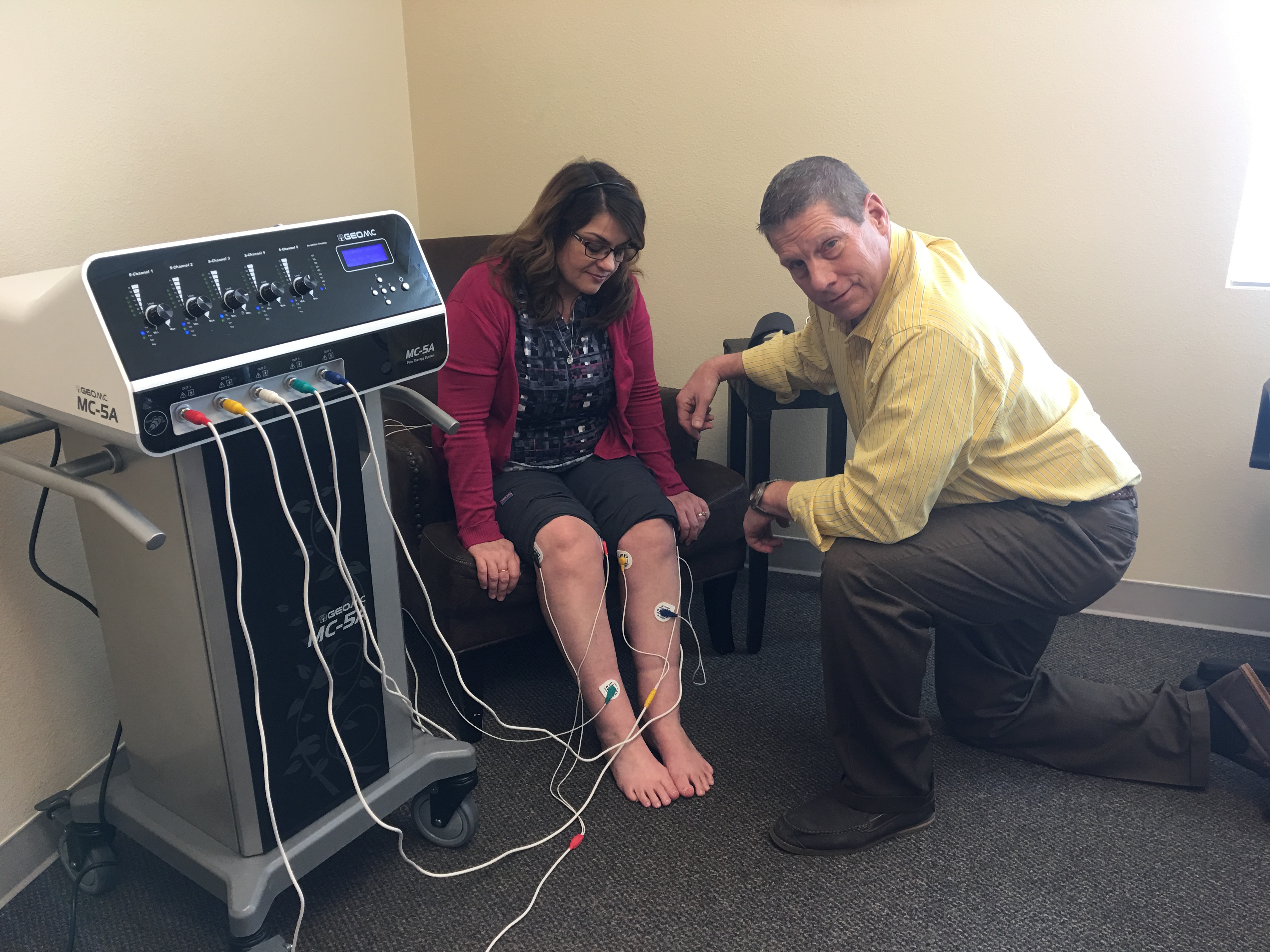
While the term “Scrambler Therapy” might evoke images of covert operations or sophisticated digital warfare, its true nature lies within the realm of cutting-edge medical technology, specifically in the field of non-invasive pain management. Scrambler Therapy represents a revolutionary approach to treating chronic pain by utilizing a sophisticated transcutaneous electrical nerve stimulation (TENS) device that essentially “scrambles” the pain signals being sent from the periphery to the brain. This innovative therapy offers a ray of hope for individuals who have found little relief from conventional pain treatments, providing a drug-free and highly targeted solution.
The development of Scrambler Therapy is rooted in a deeper understanding of how the nervous system processes and transmits pain signals. For decades, medical professionals have employed electrical stimulation to influence nerve activity and alleviate pain. However, Scrambler Therapy takes this concept to a new level of precision and effectiveness, distinguishing itself significantly from standard TENS devices. It leverages advanced neuromodulation principles to actively intervene in the pain pathway, offering a paradigm shift in chronic pain management.

The Neurological Basis of Pain and Scrambler Therapy
Understanding how Scrambler Therapy works necessitates a brief exploration of the underlying neurobiology of pain. Pain is a complex sensory and emotional experience that arises from the activation of nociceptors, specialized sensory receptors that detect potentially harmful stimuli. When these nociceptors are triggered, they generate electrical signals that travel along nerve fibers to the spinal cord and then up to the brain, where they are interpreted as pain. This intricate pathway can become dysfunctional in chronic pain conditions, leading to persistent and often debilitating sensations.
The Pain Signal Pathway
When a painful stimulus occurs, such as touching a hot surface, nociceptors in the skin are activated. These receptors release neurotransmitters that excite nerve endings of A-delta and C fibers, which are thinly myelinated and unmyelinated nerve fibers, respectively. These fibers are responsible for transmitting the initial pain signal. The signals then travel to the dorsal horn of the spinal cord, where they synapse with secondary neurons. These neurons then project to various brain regions, including the thalamus, somatosensory cortex, and limbic system, which are involved in processing the sensory, emotional, and cognitive aspects of pain.
In chronic pain conditions, this pathway can become sensitized or altered. This can happen due to various factors, including persistent inflammation, nerve damage, or changes in the central nervous system’s processing of pain signals. The result is that the brain may continue to perceive pain even in the absence of ongoing tissue damage, or the pain signals may be amplified, leading to hyperalgesia (increased sensitivity to pain) or allodynia (pain in response to stimuli that are not normally painful).
The Principle of Neuromodulation
Neuromodulation is a broad term that refers to the alteration of nerve activity through targeted delivery of a stimulus, such as electrical stimulation or pharmaceutical agents. In the context of pain management, neuromodulation aims to interrupt or modify the aberrant electrical signals that contribute to chronic pain. Traditional TENS devices, for example, work on the gate control theory of pain, where electrical stimulation is thought to activate non-pain fibers, thereby closing the “gate” in the spinal cord and preventing pain signals from reaching the brain. However, the effectiveness of standard TENS can be limited, and its mechanism is often based on sensory distraction rather than a direct intervention in the pain signal itself.
Scrambler Therapy goes beyond simple distraction. It is designed to directly interact with the malfunctioning pain pathways and “re-educate” the nervous system. By applying specific electrical waveforms and frequencies, Scrambler Therapy aims to deliver a signal that is indistinguishable from a “no-pain” signal to the brain. This effectively overrides or cancels out the erroneous pain signals, leading to a reduction or elimination of the perceived pain. This targeted approach offers a more sophisticated and potentially more effective method of neuromodulation compared to earlier forms of electrical stimulation.
How Scrambler Therapy Works: The “Scrambling” Mechanism
The core innovation of Scrambler Therapy lies in its unique method of delivering electrical stimulation. Unlike conventional TENS units that typically deliver a constant or patterned electrical current, Scrambler Therapy employs a sophisticated algorithm that generates a series of pulses. These pulses are designed to mimic “normal” sensory information, effectively tricking the brain into perceiving a lack of pain. The “scrambling” refers to the process by which the erroneous pain signals are intercepted and replaced with these non-painful signals.
The “No-Pain” Signal Analogy
Imagine the nervous system as a communication network. In chronic pain, this network is sending out a constant “error message” – the pain signal. Scrambler Therapy acts like a sophisticated network administrator that detects this error message and floods the system with a “normal signal.” The brain, receiving this new, “normal” signal, can no longer distinguish it from the original pain signal. It essentially prioritizes the new, non-painful information, leading to a reduction or cessation of the pain experience. This is akin to overwriting a corrupted file with a clean version. The therapy doesn’t necessarily eliminate the underlying cause of the pain but rather disrupts the brain’s perception of it.
The Role of the Scrambler Device and Electrode Placement
The Scrambler Therapy device itself is a specialized piece of medical equipment. It utilizes a series of electrodes that are strategically placed on the skin over the affected painful area or in specific dermatomes (areas of skin supplied by a single spinal nerve root). The precise placement is crucial for the therapy’s effectiveness, as it dictates which nerve pathways are being targeted. The device then generates a series of electrical pulses with specific amplitudes, frequencies, and pulse widths. These parameters are carefully calibrated and often adjusted throughout the treatment session based on the patient’s response.
The therapy is delivered in sessions, typically lasting around 30 to 60 minutes, and often involves a series of treatments over several days or weeks. The goal is to achieve a lasting change in how the nervous system processes pain signals. The initial treatments aim to “reset” the pain pathways, while subsequent sessions reinforce this change, leading to prolonged pain relief. The “scrambling” effect is believed to be a result of neuroplasticity – the brain’s ability to reorganize itself by forming new neural connections throughout life. By consistently delivering non-painful signals, the brain is encouraged to adapt and to prioritize these signals over the pain signals.
Applications and Effectiveness of Scrambler Therapy
Scrambler Therapy has demonstrated promising results in treating a wide array of chronic pain conditions, offering a valuable alternative for patients who have exhausted other treatment options. Its non-invasive nature, lack of significant side effects, and potential for sustained pain relief make it an attractive therapeutic modality for both patients and clinicians.
Conditions Treated by Scrambler Therapy
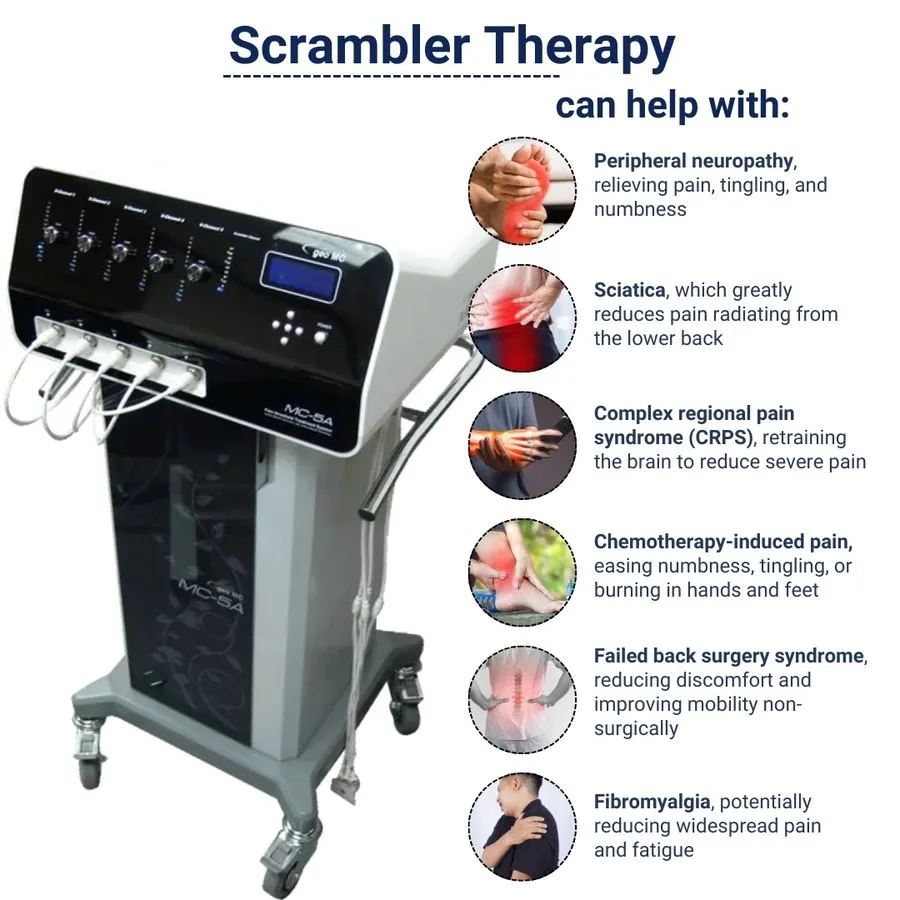
The versatility of Scrambler Therapy allows it to be applied to a broad spectrum of chronic pain syndromes. Some of the conditions that have shown significant improvement with this therapy include:
- Neuropathic Pain: This type of pain arises from damage to the nerves themselves. Conditions like diabetic neuropathy, post-herpetic neuralgia (shingles pain), trigeminal neuralgia, and phantom limb pain are often treated with Scrambler Therapy. The therapy can help to desensitize the overactive nerve fibers responsible for these conditions.
- Musculoskeletal Pain: While often managed with other therapies, chronic musculoskeletal pain, such as persistent back pain, neck pain, and joint pain, can also benefit from Scrambler Therapy, particularly when nerve involvement is suspected or contributing to the pain.
- Fibromyalgia: This complex condition characterized by widespread musculoskeletal pain, fatigue, and tenderness in specific points can be challenging to treat. Scrambler Therapy has shown efficacy in reducing pain and improving the quality of life for some individuals with fibromyalgia.
- Cancer Pain: For patients experiencing chronic pain related to cancer, Scrambler Therapy offers a non-pharmacological option to manage their discomfort, potentially reducing reliance on opioid medications.
- Post-Surgical Pain: Persistent pain following surgery, especially when nerve irritation or damage is a factor, can be a debilitating issue. Scrambler Therapy can be employed to address this type of chronic pain.
- Complex Regional Pain Syndrome (CRPS): This is a chronic pain condition characterized by severe pain, swelling, and changes in the skin and bones, often following an injury. Scrambler Therapy has shown particular promise in managing CRPS due to its ability to modulate nerve signaling.
Benefits and Limitations of Scrambler Therapy
The advantages of Scrambler Therapy are numerous, contributing to its growing popularity. The primary benefit is its non-invasive nature, meaning it does not require surgery or injections. This translates to a lack of significant side effects, unlike many pain medications which can cause drowsiness, addiction, or gastrointestinal issues. Patients often report a rapid onset of pain relief, with many experiencing noticeable improvement during or immediately after their first treatment session. Furthermore, the drug-free approach appeals to individuals seeking alternatives to long-term medication use. The potential for sustained pain relief after a course of treatment is another significant advantage, offering a chance for patients to regain functional capacity and improve their quality of life.
However, it’s important to acknowledge the limitations of Scrambler Therapy. While highly effective for many, it is not a universal cure for all types of pain. Its effectiveness can vary depending on the individual and the specific cause of their pain. The duration of relief can also vary, with some patients requiring maintenance sessions to sustain their pain reduction. The therapy also requires dedicated treatment sessions, meaning patients need to commit to a series of appointments, which can be time-consuming. Finally, access to trained practitioners and specialized equipment can be a limiting factor in some geographical areas.
The Future of Pain Management and Scrambler Therapy
Scrambler Therapy represents a significant advancement in the field of pain management, moving beyond symptom suppression to actively retraining the nervous system. As research continues to delve into the complexities of chronic pain and the potential of neuromodulation, therapies like Scrambler Therapy are likely to play an increasingly vital role in improving the lives of individuals suffering from debilitating pain.
Advancements and Research in Neuromodulation
The field of neuromodulation is continuously evolving, with ongoing research exploring new targets, stimulation techniques, and technological innovations. As our understanding of the brain and nervous system deepens, so too will our ability to precisely modulate nerve activity for therapeutic purposes. Future research on Scrambler Therapy may focus on refining the stimulation parameters, identifying optimal treatment protocols for specific conditions, and exploring its potential in combination with other therapeutic modalities. The development of more portable and user-friendly devices could also expand accessibility. Furthermore, advancements in neuroimaging and electrophysiology are providing deeper insights into the brain mechanisms underlying pain, which will undoubtedly inform the development of even more sophisticated neuromodulation techniques.
The Growing Importance of Non-Pharmacological Pain Treatments
In an era where the opioid crisis remains a significant public health concern, there is an undeniable shift towards seeking non-pharmacological alternatives for pain management. Scrambler Therapy aligns perfectly with this trend, offering a safe and effective option that avoids the risks associated with long-term opioid use. As more evidence emerges regarding the efficacy and safety of therapies like Scrambler Therapy, it is expected that they will become a more integrated part of multimodal pain management strategies. This approach emphasizes personalized care, combining various therapeutic interventions to address the multifaceted nature of chronic pain, thereby improving patient outcomes and reducing healthcare costs associated with chronic pain management. The growing emphasis on patient-centered care and the desire to minimize medication reliance positions Scrambler Therapy as a key player in the future of pain relief.