Nasal stuffiness, often referred to as a blocked or congested nose, is a common and frequently bothersome symptom characterized by the sensation of difficulty breathing through one’s nostrils. This feeling arises from swelling and inflammation of the nasal tissues, which leads to a reduction in the size of the nasal passages. While it can be an isolated symptom, it frequently accompanies other upper respiratory complaints such as a runny nose, sneezing, post-nasal drip, and facial pressure. Understanding the underlying causes and mechanisms of nasal stuffiness is crucial for effective management and relief.
The Anatomy and Physiology of Nasal Congestion
The nasal cavity is a complex structure designed for several critical functions: warming, humidifying, and filtering inhaled air before it reaches the lungs. This intricate process is facilitated by a delicate lining of mucous membranes, which are rich in blood vessels and mucus-producing cells. When these tissues are irritated or inflamed, they swell, and mucus production can increase, leading to obstruction.

Nasal Passages and Airflow
The nasal passages are lined with ciliated pseudostratified columnar epithelium. The cilia are tiny hair-like structures that beat rhythmically, propelling mucus and trapped particles, such as dust, pollen, and pathogens, towards the back of the throat to be swallowed or expelled. The turbinates, also known as conchae, are bony structures covered by this mucous membrane that project into the nasal cavity. They increase the surface area of the nasal lining, enhancing its ability to condition the air. The intricate folds and projections of the turbinates create turbulent airflow, allowing for more efficient contact between the inhaled air and the nasal mucosa. Any swelling of the turbinates or the surrounding mucosa can significantly impede this airflow, resulting in the sensation of stuffiness.
The Role of Blood Vessels and Mucus
The nasal mucosa is densely supplied with blood vessels. These vessels play a vital role in warming inhaled air and can engorge or dilate in response to various stimuli, such as cold air, irritants, or allergens. This engorgement contributes to the swelling of the nasal tissues and, consequently, to nasal congestion.
Mucus, produced by goblet cells and submucosal glands within the nasal lining, is another key player. Its primary functions include trapping foreign particles, lubricating the nasal passages, and providing a medium for the action of the cilia. Under normal conditions, mucus is thin and watery, allowing for easy passage of air. However, in response to inflammation or infection, mucus production can increase, and its consistency can change, becoming thicker and more abundant. This excess, often thickened, mucus can further block the nasal passages, exacerbating the feeling of stuffiness.
Common Causes of Nasal Stuffiness
Nasal stuffiness can stem from a wide array of causes, ranging from acute infections to chronic inflammatory conditions and environmental factors. Identifying the specific cause is paramount for targeted treatment.
Infectious Causes
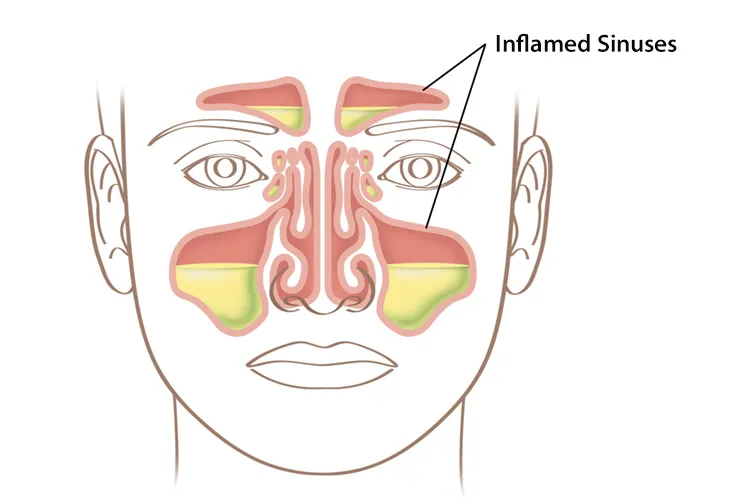
The most frequent culprits behind acute nasal stuffiness are viral infections, commonly known as the common cold. Rhinoviruses are the most prevalent cause, initiating an inflammatory response that leads to swollen nasal tissues and increased mucus production. Bacteria can also cause nasal infections, such as sinusitis, where the sinuses, air-filled cavities connected to the nasal passages, become inflamed and infected. This inflammation can extend to the nasal lining, contributing to severe congestion. Influenza, another viral illness, can also manifest with significant nasal stuffiness.
Allergic Rhinitis
Allergic rhinitis, commonly known as hay fever, is a chronic or intermittent inflammatory condition triggered by an immune system overreaction to airborne allergens. These allergens can include pollen, dust mites, mold spores, and pet dander. Upon exposure, the body releases histamine and other inflammatory mediators, causing the blood vessels in the nasal lining to dilate, the tissues to swell, and mucus production to increase. This results in characteristic symptoms of sneezing, itching, a runny nose, and, of course, nasal stuffiness.
Non-Allergic Rhinitis
Unlike allergic rhinitis, non-allergic rhinitis is not triggered by an immune response to allergens. Instead, it can be caused by a variety of irritants or environmental factors that trigger inflammation in the nasal passages. These can include changes in temperature or humidity, strong odors (perfumes, cleaning products), certain medications, hormonal changes, and even stress. Vasomotor rhinitis is a common form of non-allergic rhinitis where the blood vessels in the nose are overly sensitive to environmental stimuli, leading to swelling and congestion.
Structural Abnormalities
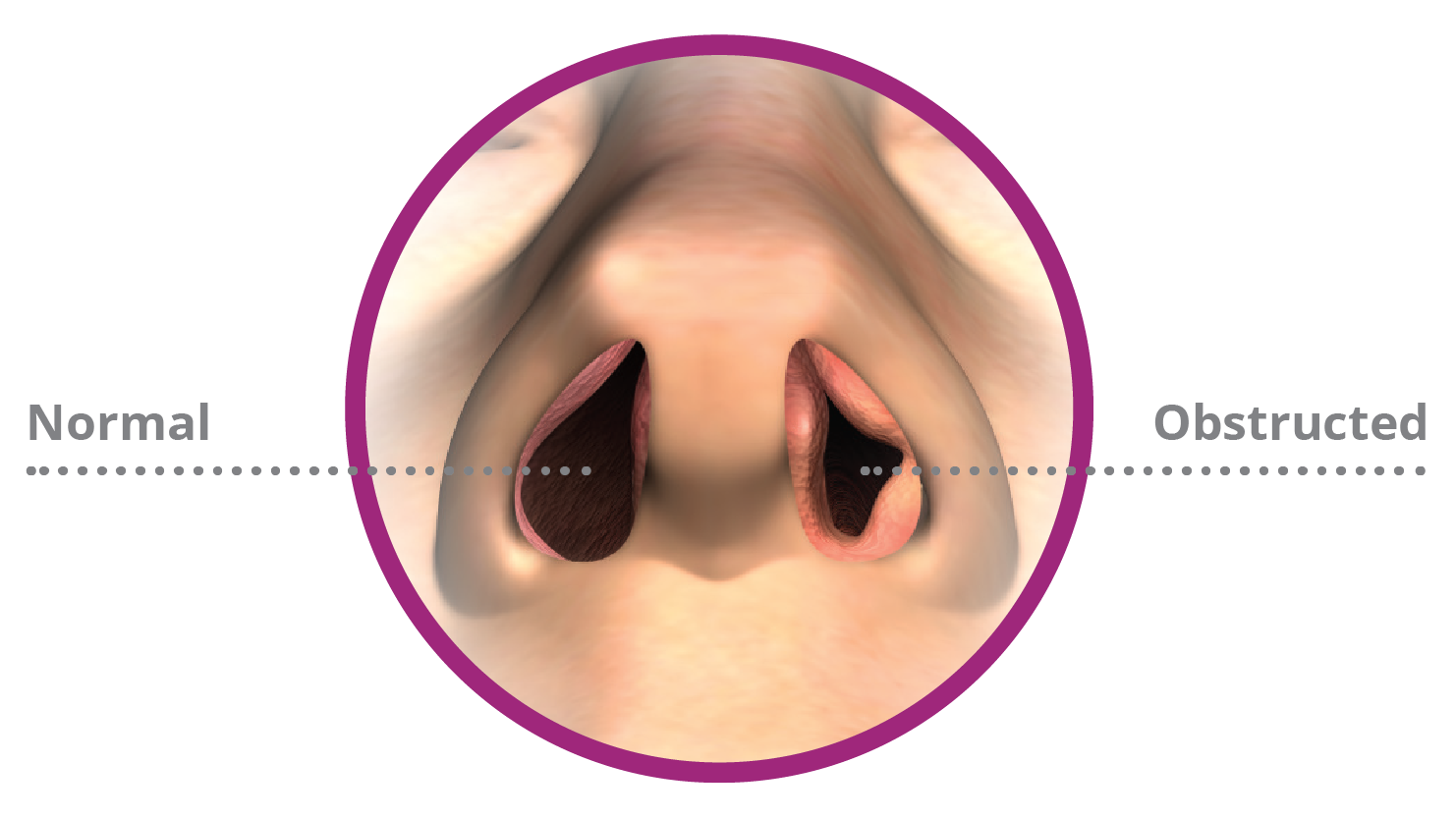
In some individuals, nasal stuffiness can be attributed to physical blockages within the nasal passages. A deviated septum, where the cartilage wall dividing the two nostrils is off-center or crooked, can narrow one nasal passage, leading to chronic congestion on that side. Nasal polyps, soft, non-cancerous growths that can develop in the lining of the nasal passages or sinuses, can also obstruct airflow and cause significant stuffiness, often accompanied by a loss of smell. Enlarged adenoids, particularly in children, can block the passage of air from the nose to the throat.
Other Contributing Factors
- Medications: Certain medications, such as some blood pressure medications, oral contraceptives, and even over-the-counter decongestant nasal sprays used excessively (rebound congestion), can contribute to nasal stuffiness.
- Hormonal Changes: Fluctuations in hormones, such as during pregnancy or menstruation, can lead to increased blood flow to the nasal mucosa, causing swelling and congestion.
- Environmental Irritants: Exposure to smoke, pollution, and dry air can irritate the nasal lining, leading to inflammation and stuffiness.
- Gastroesophageal Reflux Disease (GERD): In some cases, stomach acid refluxing into the esophagus can trigger a reflex in the upper airways, leading to nasal congestion.
The Impact of Nasal Stuffiness on Daily Life
Nasal stuffiness is more than just a physical discomfort; it can significantly impact an individual’s quality of life, affecting sleep, concentration, and overall well-being.
Sleep Disturbances
When the nasal passages are blocked, breathing through the nose becomes difficult, often forcing individuals to breathe through their mouth. This can lead to snoring, dry mouth, sore throat, and fragmented sleep. Chronic nasal congestion can contribute to or exacerbate conditions like sleep apnea, a disorder characterized by repeated interruptions in breathing during sleep. The resulting lack of restful sleep can lead to daytime fatigue, irritability, and decreased cognitive function.
Cognitive and Sensory Impairment
The reduced airflow through the nasal passages can impact the sense of smell, which is closely linked to the sense of taste. This diminished sensory experience can make eating less enjoyable and can even pose a safety risk if one cannot detect the smell of smoke or spoiled food. Furthermore, the discomfort and constant awareness of nasal congestion can make it difficult to concentrate on tasks, leading to reduced productivity at work or school.
Social and Emotional Well-being
The persistent discomfort, fatigue, and impaired sensory perception associated with nasal stuffiness can contribute to feelings of irritability, frustration, and even social withdrawal. The physical symptoms can also make one feel generally unwell and less inclined to participate in social activities.
Managing and Relieving Nasal Stuffiness
The approach to managing nasal stuffiness depends heavily on its underlying cause. A multifaceted strategy often involves home remedies, over-the-counter treatments, and, in some cases, prescription medications or medical interventions.
Home Remedies and Lifestyle Modifications
- Saline Nasal Rinses: Using a neti pot or saline spray can effectively clear mucus and allergens from the nasal passages, reducing inflammation and promoting drainage.
- Humidification: Using a humidifier, especially in dry environments or during winter, can help keep nasal passages moist and soothe irritated tissues. Taking steamy showers or inhaling steam from a bowl of hot water can also provide temporary relief.
- Hydration: Drinking plenty of fluids, such as water and herbal teas, helps thin mucus, making it easier to drain.
- Elevating the Head: Sleeping with the head elevated can help reduce congestion by promoting drainage.
- Avoiding Irritants: Identifying and avoiding triggers like smoke, strong perfumes, and known allergens is crucial for individuals with non-allergic or allergic rhinitis.
Over-the-Counter (OTC) Treatments
- Decongestants: Oral decongestants (e.g., pseudoephedrine, phenylephrine) work by constricting blood vessels in the nasal lining, reducing swelling. Nasal decongestant sprays (e.g., oxymetazoline) offer rapid relief but should be used for no more than three consecutive days to avoid rebound congestion.
- Antihistamines: For allergic rhinitis, antihistamines (e.g., loratadine, cetirizine) block the action of histamine, a key chemical released during allergic reactions, thereby reducing sneezing, itching, and runny nose. Some antihistamines also have mild decongestant properties.
- Corticosteroid Nasal Sprays: These sprays (e.g., fluticasone, budesonide) are highly effective for allergic and non-allergic rhinitis. They reduce inflammation directly in the nasal passages and are often recommended for daily use for long-term symptom control.
Medical Interventions
When home remedies and OTC treatments are insufficient, medical intervention may be necessary.
- Prescription Medications: Doctors may prescribe stronger corticosteroids, anticholinergic nasal sprays (to reduce mucus), or leukotriene modifiers for more severe or persistent cases. Antibiotics are prescribed only for bacterial infections.
- Immunotherapy (Allergy Shots): For individuals with severe allergies, immunotherapy can help desensitize the immune system to specific allergens over time.
- Surgery: In cases of significant structural abnormalities, such as a severely deviated septum or large nasal polyps, surgical correction may be recommended to improve airflow and alleviate chronic congestion. This can include septoplasty, rhinoplasty, or polypectomy.
Understanding the varied causes and mechanisms of nasal stuffiness empowers individuals to seek appropriate relief and improve their overall health and well-being. By addressing the root cause, one can effectively manage this common and often debilitating symptom.
