Macrobid, a brand name for a specific formulation of nitrofurantoin, is a widely prescribed antibiotic primarily utilized to combat bacterial infections of the urinary tract. Its efficacy lies in its ability to target a broad spectrum of bacteria commonly responsible for these ailments, making it a cornerstone in the treatment of uncomplicated urinary tract infections (UTIs), particularly cystitis (bladder infections) and pyelonephritis (kidney infections). While its primary application is within the urinary system, understanding its mechanism, spectrum of activity, and clinical indications is crucial for healthcare professionals and patients alike.
Understanding Nitrofurantoin and its Mechanism of Action
Nitrofurantoin is a synthetic antimicrobial agent that has been in clinical use for decades. Its unique mechanism of action differentiates it from many other antibiotics, contributing to its effectiveness and its relatively low incidence of bacterial resistance. Unlike many bacteriostatic agents that inhibit bacterial growth, nitrofurantoin is primarily bactericidal, meaning it directly kills bacteria.
How Nitrofurantoin Works
Upon administration, nitrofurantoin is rapidly absorbed and undergoes reduction within bacterial cells by enzymes such as nitroreductases. This reduction process generates reactive intermediates that are toxic to bacterial cells. These intermediates interfere with multiple cellular processes, including:
- DNA Damage: The reactive metabolites can bind to bacterial DNA, causing breaks and strand interruptions, thereby inhibiting DNA replication and transcription.
- Ribosomal Inhibition: Nitrofurantoin can also interfere with protein synthesis by binding to bacterial ribosomes, preventing the formation of essential proteins.
- Metabolic Pathway Disruption: It is believed to disrupt various metabolic pathways within bacteria, further compromising their viability.
This multi-targeted approach makes it difficult for bacteria to develop resistance to nitrofurantoin. While resistance does occur, it is generally less prevalent compared to some other antibiotic classes. Furthermore, nitrofurantoin concentrates in the urine, reaching high therapeutic levels in the urinary tract, which is essential for effectively clearing the infection. Importantly, systemic concentrations of nitrofurantoin are typically low, which helps to minimize the risk of systemic side effects.
Spectrum of Activity
Nitrofurantoin exhibits activity against a wide range of common urinary pathogens. Its spectrum includes:
- Escherichia coli (E. coli): This is the most frequent cause of UTIs, accounting for a significant majority of cases. Nitrofurantoin is highly effective against most strains of E. coli.
- Staphylococcus saprophyticus: Another common pathogen, particularly in young women.
- Enterococcus faecalis: While nitrofurantoin has some activity against enterococci, it is generally not considered the first-line treatment for enterococcal UTIs, especially in complicated cases.
- Klebsiella pneumoniae: A common cause of both community-acquired and hospital-acquired UTIs.
- Proteus mirabilis: This bacterium can contribute to UTIs, particularly those associated with kidney stones. Nitrofurantoin’s efficacy against Proteus can be variable.
- Enterobacter species: Nitrofurantoin may have some activity against certain Enterobacter species, but susceptibility testing is often recommended.
It is important to note that nitrofurantoin has limited or no activity against certain bacteria, including Pseudomonas aeruginosa, Serratia marcescens, and Providencia species. Therefore, susceptibility testing is crucial in cases of recurrent infections, treatment failures, or infections caused by less common pathogens.
Primary Indications for Macrobid Use
Macrobid’s primary role in medicine is the treatment of uncomplicated urinary tract infections. The term “uncomplicated” refers to infections that occur in otherwise healthy, non-pregnant individuals with normal urinary tract anatomy and function. These infections are typically localized to the lower urinary tract (bladder and urethra) and do not involve the kidneys or prostate.
Treatment of Cystitis
Cystitis, or bladder infection, is the most common type of UTI. Symptoms typically include dysuria (painful urination), frequency (frequent urge to urinate), urgency (sudden, strong urge to urinate), and suprapubic pain (discomfort in the lower abdomen). Macrobid is a highly effective and well-tolerated treatment option for acute cystitis. It is often prescribed for a course of 5 to 7 days, depending on the specific clinical guidelines and the severity of symptoms.
Management of Pyelonephritis
While nitrofurantoin is primarily used for lower UTIs, it can also be considered for the treatment of mild to moderate uncomplicated pyelonephritis, an infection of the kidney. However, due to its lower systemic concentrations, it is generally not the preferred agent for severe pyelonephritis or in situations where rapid systemic absorption and high tissue penetration are paramount. In cases of suspected or confirmed pyelonephritis, oral nitrofurantoin may be part of a treatment regimen, often in conjunction with other agents or for a longer duration, but physicians will carefully weigh its use against other recommended antibiotics that achieve higher systemic levels. Close monitoring for treatment response and potential complications is essential when nitrofurantoin is used for pyelonephritis.
Prophylaxis and Suppression of Recurrent UTIs
In certain individuals who experience frequent, recurrent UTIs, low-dose nitrofurantoin may be prescribed for long-term prophylaxis or suppression. This strategy aims to prevent future infections by maintaining a low level of antimicrobial activity in the urinary tract. Prophylactic use is typically reserved for patients with a significant burden of recurrent infections that impact their quality of life and do not respond adequately to other preventive measures. The decision to initiate long-term nitrofurantoin prophylaxis is made on a case-by-case basis, considering the patient’s history, frequency of infections, and potential risks and benefits.

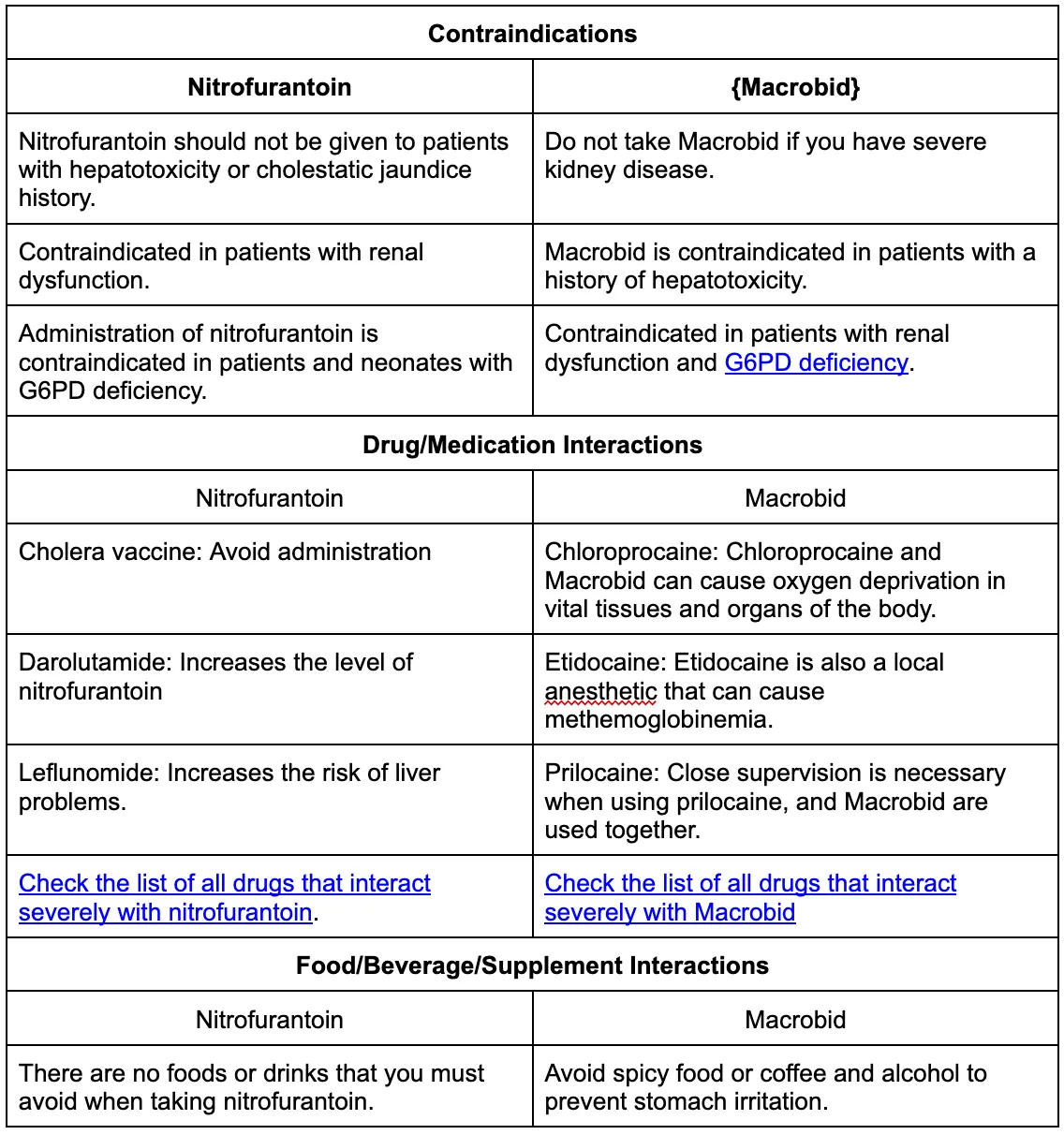
Contraindications and Precautions
Despite its broad utility, Macrobid is not suitable for all patients. Certain conditions and patient populations warrant caution or contraindicate its use.
Renal Impairment
Nitrofurantoin is primarily excreted by the kidneys. In patients with significant renal impairment, drug accumulation can occur, leading to an increased risk of toxicity. The effectiveness of nitrofurantoin is also diminished in the presence of impaired renal function, as adequate concentrations may not be achieved in the urine. Therefore, nitrofurantoin is generally contraindicated in patients with a creatinine clearance below 30-60 mL/min, depending on the specific guidelines and the formulation being used. Regular monitoring of renal function is crucial in patients with mild to moderate renal impairment who are receiving nitrofurantoin.
Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency
Individuals with G6PD deficiency are at an increased risk of developing hemolytic anemia when treated with nitrofurantoin. G6PD is an enzyme that helps protect red blood cells from oxidative damage. In susceptible individuals, nitrofurantoin can trigger oxidative stress, leading to the premature destruction of red blood cells. Screening for G6PD deficiency is not routinely recommended, but healthcare providers should be aware of this potential risk and exercise caution when prescribing nitrofurantoin to patients with a known history of G6PD deficiency.
Pulmonary and Hepatic Toxicity
While rare, nitrofurantoin can be associated with serious pulmonary and hepatic toxicity. Pulmonary reactions can range from acute, flu-like symptoms to chronic interstitial pneumonitis and pulmonary fibrosis, particularly with long-term use. Hepatic reactions, including hepatitis and jaundice, have also been reported. Patients experiencing symptoms suggestive of pulmonary or hepatic involvement, such as persistent cough, shortness of breath, fever, or jaundice, should discontinue nitrofurantoin and seek immediate medical attention.
Peripheral Neuropathy
Nitrofurantoin can also cause peripheral neuropathy, characterized by numbness, tingling, or burning sensations in the extremities. This is more common in patients with renal impairment or those on long-term therapy. If symptoms of peripheral neuropathy develop, nitrofurantoin should be discontinued.
Pregnancy and Lactation
The use of nitrofurantoin in pregnancy requires careful consideration. It is generally avoided in the third trimester (after 37 weeks of gestation) due to the theoretical risk of hemolytic anemia in the newborn. However, it can be used earlier in pregnancy for the treatment of UTIs when other options are not suitable. During lactation, nitrofurantoin is generally considered safe, as it is excreted in breast milk in low concentrations. However, caution is advised, and monitoring for any adverse effects in the infant is recommended.
Dosing and Administration
The standard dosing of Macrobid (nitrofurantoin monohydrate/macrocrystals) for the treatment of UTIs is typically 100 mg taken orally twice daily for 5 to 7 days. The macrocrystal formulation is designed for slower release and better gastrointestinal tolerance compared to older nitrofurantoin formulations.
Importance of Completing the Full Course
It is paramount for patients to complete the entire prescribed course of Macrobid, even if their symptoms improve before the medication is finished. Prematurely stopping the antibiotic can lead to the recurrence of the infection and may contribute to the development of antibiotic resistance.
Taking with Food
To enhance absorption and minimize gastrointestinal upset, Macrobid is often recommended to be taken with food. This helps to ensure that the medication is effectively absorbed into the bloodstream and reaches therapeutic concentrations in the urinary tract.
Monitoring and Follow-up
While Macrobid is generally well-tolerated, healthcare providers may recommend follow-up appointments or urine cultures to confirm the resolution of the infection, especially in cases of recurrent UTIs or when initial treatment response is suboptimal. Patients should be advised to report any new or worsening symptoms to their physician promptly.
In summary, Macrobid is a valuable antibiotic for treating uncomplicated urinary tract infections, offering a reliable and effective option for a common bacterial ailment. Its unique mechanism of action, broad spectrum of activity against key urinary pathogens, and established safety profile make it a cornerstone in the management of cystitis and a consideration for mild pyelonephritis. However, its use necessitates a thorough understanding of contraindications, precautions, and proper dosing to ensure optimal patient outcomes and minimize potential risks.
