Understanding Alanine Aminotransferase (ALT) in the Context of Liver Health
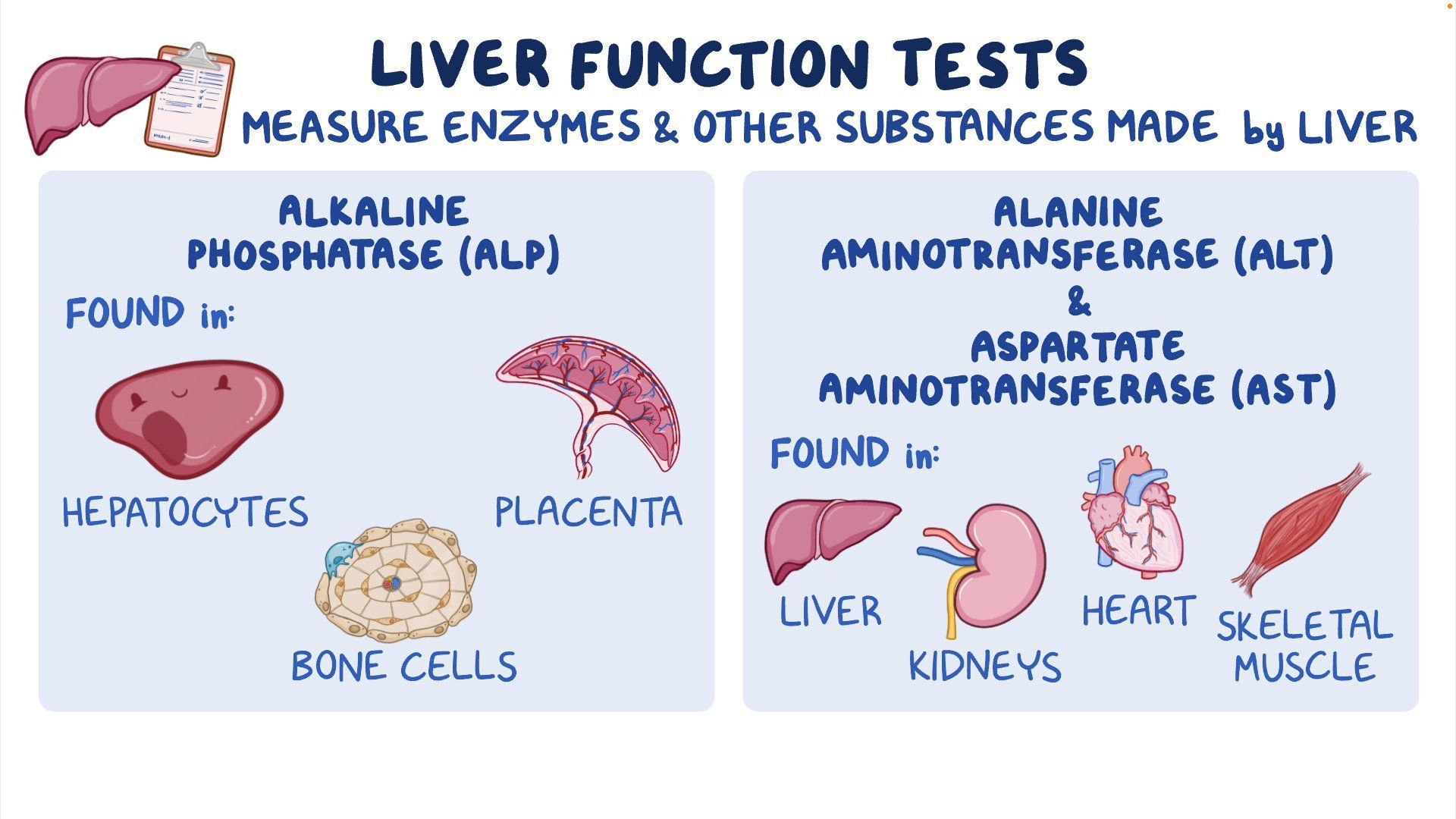
Alanine aminotransferase, commonly abbreviated as ALT, is an enzyme found predominantly in the liver. Its primary role in the body is to help metabolize proteins, specifically by converting alanine, an amino acid, into other substances that the body needs. While ALT is present in other tissues like the kidneys, heart, and muscles, it is most concentrated within liver cells (hepatocytes). This high concentration makes ALT an exceptionally sensitive indicator of liver damage. When liver cells are injured or inflamed, they release ALT into the bloodstream. Therefore, measuring ALT levels in the blood is a fundamental diagnostic tool used by healthcare professionals to assess liver function and detect potential liver diseases.

The Role of ALT in Cellular Metabolism
Within the intricate biochemical pathways of the human body, ALT plays a crucial role in amino acid metabolism. It facilitates the transfer of an amino group from alanine to alpha-ketoglutarate, a process known as transamination. This reaction results in the formation of pyruvate and glutamate. Pyruvate is a key intermediate in energy production, entering the citric acid cycle for ATP generation. Glutamate, on the other hand, is involved in various metabolic processes, including nitrogen transport and the synthesis of other amino acids. This continuous metabolic activity highlights ALT’s importance in maintaining cellular energy balance and protein turnover. The efficiency and regulation of this enzymatic reaction are vital for overall cellular health, and any disruption can signal underlying physiological issues.
ALT and Liver Injury: A Diagnostic Link
The diagnostic significance of ALT levels arises directly from its localization within hepatocytes. When the liver is subjected to stress, injury, or disease, the cell membranes of hepatocytes become compromised. This damage allows intracellular enzymes, including ALT, to leak out of the cells and enter the bloodstream. Consequently, elevated levels of ALT in a blood serum sample are a strong indicator that liver cells have been damaged. The degree of elevation often correlates with the extent of liver injury. While ALT is not the sole determinant of liver health, it serves as a critical early warning sign, prompting further investigation to identify the underlying cause of the liver dysfunction.
Interpreting ALT Blood Test Results
A standard blood test, often part of a comprehensive metabolic panel (CMP) or liver function test (LFT), measures ALT levels. The results are typically reported in units per liter (U/L). While specific normal ranges can vary slightly between laboratories due to differences in testing methods and equipment, generally, a normal ALT level for adults falls within a range of approximately 7 to 56 U/L. However, it’s crucial to understand that “normal” is a statistical average, and individual variations exist. Healthcare providers interpret ALT results in conjunction with other clinical findings, patient history, and other laboratory tests to form a comprehensive diagnosis.
Normal ALT Ranges and Variations
The accepted normal ranges for ALT are established through extensive population studies. These ranges represent the typical levels found in healthy individuals. However, factors such as age, sex, and even the time of day a blood sample is taken can influence ALT levels. For instance, some studies suggest slightly higher ALT levels in men compared to women. Understanding these potential variations is important for accurate interpretation, though significant deviations from the normal range are usually indicative of a problem regardless of these minor fluctuations.
What Do Elevated ALT Levels Mean?
Elevated ALT levels, medically termed alanine aminotransferase elevation, can signify a wide spectrum of liver conditions. Mild elevations, perhaps a few times the upper limit of normal, might be caused by less severe issues. However, significantly elevated ALT levels, especially those in the hundreds or thousands, often point to more acute or severe liver injury. Common causes include viral hepatitis (Hepatitis A, B, C), non-alcoholic fatty liver disease (NAFLD), alcoholic liver disease, drug-induced liver injury (DILI), and certain autoimmune conditions. It’s important to note that ALT can also be elevated by conditions unrelated to direct liver pathology, such as muscle injury or hemolytic anemia, though liver-related causes are the most frequent culprits.
Low ALT Levels: Significance and Implications
While elevated ALT levels are more commonly discussed due to their association with liver damage, very low ALT levels are generally not a cause for concern and are rarely clinically significant. In fact, persistently low ALT levels are sometimes observed in individuals with vitamin B6 deficiency, as vitamin B6 is a cofactor for the ALT enzyme. However, in the vast majority of cases, low ALT is simply a benign finding and does not require further investigation. The focus of clinical attention is overwhelmingly on elevated ALT as a marker of hepatic distress.
Common Causes of Elevated ALT
The liver is a resilient organ, but it is susceptible to damage from various sources. Understanding these causes is fundamental to diagnosing and managing liver health effectively. When ALT levels rise, a clinician will investigate a range of potential culprits, often starting with the most prevalent and easily identifiable issues.
Viral Hepatitis Infections
Viral hepatitis is a leading cause of acute and chronic liver inflammation, and consequently, significantly elevated ALT levels. Hepatitis A, B, and C are the most common types affecting the liver. Hepatitis A is typically an acute infection spread through contaminated food or water. Hepatitis B and C are more often transmitted through blood and body fluid contact and can lead to chronic liver disease, cirrhosis, and liver cancer if left untreated. During the active phase of these infections, liver cells are heavily damaged, leading to substantial ALT release into the bloodstream.
Non-Alcoholic Fatty Liver Disease (NAFLD)
NAFLD has become increasingly prevalent worldwide, closely linked to the rise in obesity, type 2 diabetes, and metabolic syndrome. It is characterized by the accumulation of fat in liver cells, which can progress to inflammation (non-alcoholic steatohepatitis or NASH) and eventually fibrosis and cirrhosis. Even in its earlier stages, NAFLD can cause mild to moderate elevations in ALT levels. Lifestyle modifications, including diet and exercise, are the cornerstone of managing NAFLD and can often lead to improvement in ALT levels.
Alcoholic Liver Disease
Excessive and prolonged alcohol consumption is a major contributor to liver damage. Alcohol is directly toxic to liver cells, leading to inflammation and fat accumulation. As the disease progresses, it can result in alcoholic hepatitis, fibrosis, and cirrhosis. ALT levels are typically elevated in alcoholic liver disease, though often AST (aspartate aminotransferase), another liver enzyme, may be elevated to a greater extent than ALT in alcoholic cases, sometimes referred to as an AST:ALT ratio greater than 2:1.
Drug-Induced Liver Injury (DILI)
Many medications, both prescription and over-the-counter, can cause liver damage as a side effect. This drug-induced liver injury (DILI) is a significant cause of acute liver failure. Common offenders include acetaminophen (paracetamol), certain antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), and some herbal supplements. The mechanism of injury can vary depending on the drug, but it often involves direct toxicity or an immune-mediated reaction within the liver. ALT elevation is a hallmark of DILI and often prompts a review and potential discontinuation of suspect medications.
Other Liver Conditions
Beyond the common causes, a multitude of other conditions can lead to elevated ALT levels. These include:
- Autoimmune Hepatitis: The body’s immune system mistakenly attacks liver cells, causing inflammation and damage.
- Hemochromatosis: A genetic disorder causing excessive iron absorption and storage, leading to organ damage, including the liver.
- Wilson’s Disease: A rare genetic disorder characterized by excessive copper accumulation in the body, particularly the liver and brain.
- Celiac Disease: An autoimmune disorder triggered by gluten, which can sometimes be associated with elevated liver enzymes.
- Ischemic Hepatitis: Also known as “shock liver,” this occurs when the liver doesn’t receive enough oxygenated blood, often due to severe illness or shock.
- Alpha-1 Antitrypsin Deficiency: A genetic disorder that can lead to lung and liver disease.
- Cirrhosis: Advanced scarring of the liver tissue, which can result from various chronic liver diseases. While cirrhosis itself is a severe condition, ALT levels may sometimes be normal or even low in end-stage liver disease due to a significant loss of functional liver cells.
Managing Liver Health and ALT Levels
Maintaining optimal liver health is paramount for overall well-being. Given the liver’s vital role in detoxification, metabolism, and synthesis of essential proteins, any signs of dysfunction, as indicated by elevated ALT, warrant attention. Proactive lifestyle choices and prompt medical intervention are key to safeguarding liver function and managing conditions that affect ALT levels.
Lifestyle Modifications for Liver Health
Several lifestyle adjustments can significantly benefit liver health and help normalize elevated ALT levels.
- Diet: A balanced diet rich in fruits, vegetables, and whole grains, while low in saturated fats, processed foods, and excessive sugar, is crucial. Limiting intake of high-fructose corn syrup can be particularly beneficial for those with NAFLD.
- Weight Management: Maintaining a healthy weight or achieving weight loss if overweight or obese is one of the most effective strategies for improving NAFLD and reducing liver inflammation.
- Alcohol Consumption: For individuals with elevated ALT or diagnosed liver conditions, limiting or abstaining from alcohol is essential. The recommended limit for moderate alcohol consumption is generally up to one drink per day for women and up to two drinks per day for men, but for those with liver issues, complete avoidance is often advised.
- Regular Exercise: Physical activity helps with weight management, improves insulin sensitivity, and can reduce liver fat. Aiming for at least 150 minutes of moderate-intensity aerobic exercise per week is recommended.
When to Seek Medical Attention
Any persistently elevated ALT levels, especially those that are significantly high or accompanied by symptoms such as jaundice (yellowing of the skin and eyes), abdominal pain, fatigue, nausea, or dark urine, should prompt a visit to a healthcare provider. It is also important to discuss all medications, including over-the-counter drugs and herbal supplements, with your doctor, as they could be contributing to liver stress. Regular health check-ups, including liver function tests, can help in early detection and management of liver conditions.

The Importance of Comprehensive Liver Function Testing
While ALT is a vital marker, it is rarely used in isolation. Healthcare providers typically order a panel of liver function tests to get a more complete picture of liver health. This panel often includes:
- AST (Aspartate Aminotransferase): Another enzyme found in the liver and other organs; useful in conjunction with ALT to assess liver damage.
- Bilirubin: A waste product of red blood cell breakdown, measured to assess the liver’s ability to process and excrete waste.
- Albumin: A protein produced by the liver, reflecting the liver’s synthetic function.
- Prothrombin Time (PT) and International Normalized Ratio (INR): Measures of blood clotting time, which can indicate the liver’s ability to produce clotting factors.
- Alkaline Phosphatase (ALP): An enzyme found in the liver, bile ducts, and bone; elevated levels can indicate bile duct obstruction or bone disease.
- GGT (Gamma-Glutamyl Transferase): Another enzyme that can indicate liver and bile duct problems, particularly related to alcohol or bile duct issues.
By examining these markers together, along with clinical symptoms and imaging studies, physicians can accurately diagnose the cause of elevated ALT and develop an appropriate treatment plan to protect liver function and improve overall health.
