Knee ankylosis, a condition characterized by the stiffening and immobility of the knee joint, represents a significant challenge for individuals seeking to maintain an active and independent lifestyle. This fusion of bones within the joint, typically occurring due to severe injury, chronic inflammation, or other pathological processes, can profoundly impact daily activities, from walking and standing to more complex movements. Understanding the underlying causes, diagnostic approaches, and available management strategies for knee ankylosis is crucial for both patients and healthcare professionals.
Understanding the Pathophysiology of Knee Ankylosis
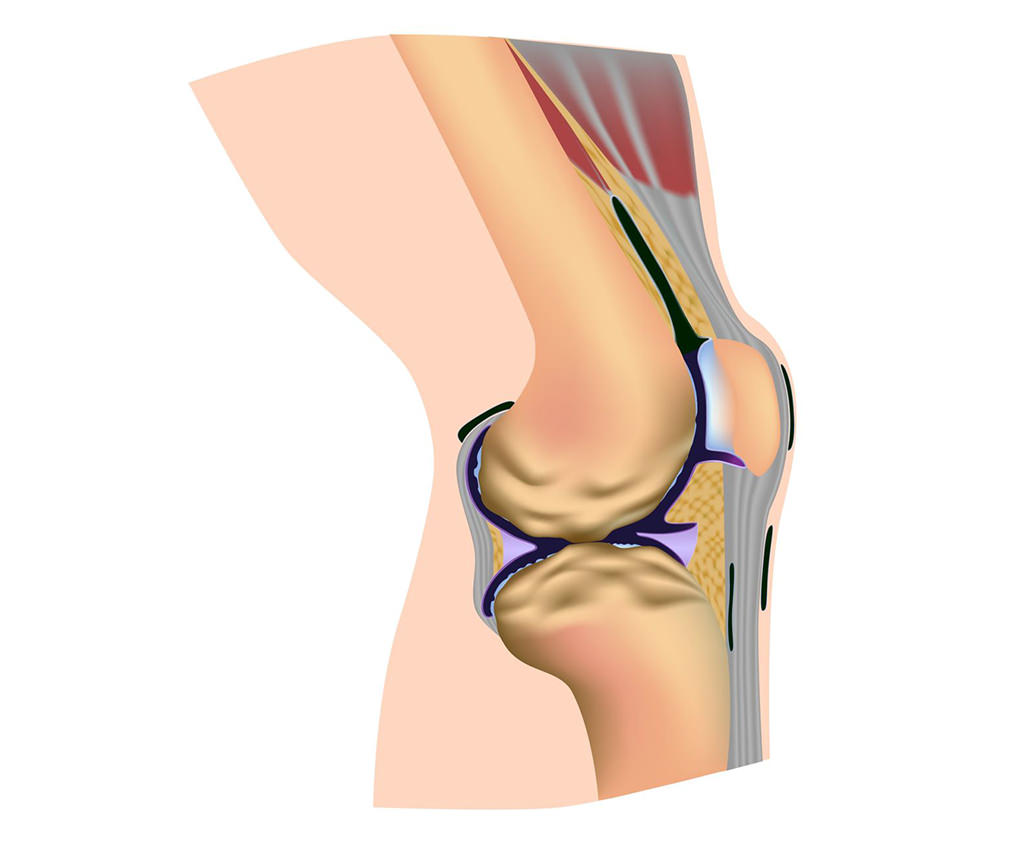
Knee ankylosis is fundamentally a process of joint fusion, where the normal articulation between the femur (thigh bone) and the tibia (shin bone) is replaced by solid bone or extensive scar tissue. This pathological fusion can occur in varying degrees, from partial stiffness to complete and irreversible loss of motion. The underlying mechanisms driving this fusion are typically inflammatory or degenerative in nature, leading to the breakdown of articular cartilage, formation of adhesions, and ultimately, osseous bridging.
Inflammatory Arthritis and Ankylosis
One of the most common drivers of knee ankylosis is inflammatory arthritis, a group of conditions where the immune system mistakenly attacks the joint tissues.
Rheumatoid Arthritis (RA)
Rheumatoid arthritis is a systemic autoimmune disease that primarily affects the joints. In the knee, RA causes chronic inflammation of the synovium, the lining of the joint capsule. This persistent inflammation leads to the erosion of articular cartilage, damage to the ligaments and menisci, and the formation of pannus – a destructive granulation tissue. If left untreated or if the disease is particularly aggressive, the inflammatory process can progress to fibrosis and eventually bony fusion, resulting in ankylosis. The symmetrical nature of RA often means that both knees can be affected, exacerbating the functional limitations.
Ankylosing Spondylitis (AS)
While ankylosing spondylitis is primarily known for affecting the spine, it can also involve the peripheral joints, including the knees. AS is a chronic inflammatory disease that causes inflammation of the entheses – the points where tendons and ligaments attach to bone. In the knee, this can lead to inflammation of the joint capsule and surrounding structures. Over time, this chronic inflammation can result in bony overgrowth and fusion, leading to ankylosis. The sacroiliac joints are typically the first to be affected in AS, and progression to other joints, including the knees, is common.
Other Inflammatory Conditions
Other forms of inflammatory arthritis, such as psoriatic arthritis and reactive arthritis, can also, in severe or long-standing cases, lead to knee ankylosis through similar mechanisms of chronic inflammation and subsequent bony fusion.
Traumatic Injuries and Ankylosis
Severe trauma to the knee joint is another significant cause of ankylosis. The nature of the injury and the subsequent healing process play a critical role.
Fractures
Intra-articular fractures, those that extend into the joint space, are particularly prone to causing ankylosis. If bone fragments are displaced within the joint, or if the fracture involves a large portion of the articular surface, the healing process can lead to significant irregularities and adhesions.
Direct Articular Surface Damage
When the smooth articular cartilage that covers the ends of the bones is directly damaged or destroyed by the fracture, the underlying bone is exposed. This can stimulate abnormal bone formation and the development of fibrous scar tissue that bridges the joint.
Post-Traumatic Arthritis
Following a significant knee injury, even if not a direct fracture into the joint, post-traumatic arthritis can develop. This condition involves the accelerated degeneration of articular cartilage due to the altered biomechanics and inflammatory responses triggered by the injury. Chronic inflammation and cartilage loss can, over time, lead to the development of bony spurs (osteophytes) and eventual fusion.
Severe Soft Tissue Damage and Infection
Extensive damage to the ligaments, tendons, and menisci can lead to joint instability and altered biomechanics. If these injuries are accompanied by significant bleeding within the joint (hemarthrosis) or if infection (septic arthritis) occurs, the inflammatory response and the body’s attempt to heal can result in extensive scar tissue formation and adhesions, potentially leading to ankylosis.
Other Causes of Knee Ankylosis
Beyond inflammatory and traumatic etiologies, several other factors can contribute to the development of knee ankylosis.
Osteomyelitis
Osteomyelitis is a serious bone infection. If it affects the femur, tibia, or the joint itself, the intense inflammatory response and the body’s attempt to wall off the infection can lead to significant fibrosis and bony changes that result in ankylosis.
Tumors
While less common, tumors within or around the knee joint can directly invade and damage joint structures, leading to inflammation, pain, and, in some cases, ankylosis as a consequence of the tumor’s growth and the subsequent treatment or inflammatory response.
Congenital Conditions
In rare instances, congenital conditions or developmental abnormalities can result in the incomplete formation or fusion of the knee joint from birth, leading to a form of congenital ankylosis.
Prolonged Immobilization
Extended periods of immobilization of the knee joint, whether due to casting, bracing, or prolonged bed rest, can contribute to stiffness. While this typically results in a less severe form of stiffness (arthrofibrosis) rather than true bony ankylosis, in extreme and prolonged cases, it can lead to significant functional loss and may progress towards fusion.
Diagnosing Knee Ankylosis: A Comprehensive Approach
The diagnosis of knee ankylosis involves a thorough evaluation of the patient’s medical history, a detailed physical examination, and the judicious use of imaging techniques. The goal is to confirm the presence of joint fusion, assess its severity, and identify the underlying cause.
Medical History and Physical Examination
The patient’s history is paramount. Questions about the onset of symptoms, any history of trauma, inflammatory conditions, infections, or prolonged immobilization provide crucial clues.
Patient Interview
Key details to elicit include:
- Onset and duration of symptoms: Was it sudden or gradual? How long has the stiffness been present?
- Pain characteristics: Is the pain constant or intermittent? What exacerbates or alleviates it?
- Mechanism of injury (if any): Details of any accidents or falls.
- Past medical history: Diagnosed inflammatory conditions (RA, AS), history of infections, previous surgeries on the knee.
- Functional limitations: How has the stiffness affected daily activities, work, and hobbies?
Physical Assessment

The physical examination focuses on assessing the knee joint’s range of motion, stability, and integrity.
- Range of Motion (ROM) Assessment: This is the cornerstone of diagnosing ankylosis. The examiner will attempt to passively move the knee through its full flexion and extension. A complete absence of passive motion, or extremely limited motion (e.g., less than 10 degrees), strongly suggests ankylosis. It’s important to distinguish between active ROM (what the patient can do) and passive ROM (what the examiner can do).
- Palpation: Feeling for bony irregularities, warmth (indicating inflammation), swelling, and tenderness.
- Gait Analysis: Observing how the patient walks can reveal compensatory mechanisms and the extent of functional impairment.
- Inspection: Looking for signs of atrophy (muscle wasting), scars, or deformities.
- Joint Stability Tests: While stability is often compromised in ankylosis, certain tests might still be performed to assess remaining ligamentous integrity, though their interpretation can be challenging with severe stiffness.
Imaging Modalities
Imaging plays a critical role in visualizing the extent of bony fusion and identifying underlying pathological changes.
X-rays
Standard X-rays are typically the first-line imaging modality. They are excellent for visualizing bone and can clearly demonstrate:
- Bony fusion: The presence of osseous bridging between the femur and tibia.
- Joint space narrowing: Indicative of cartilage loss.
- Osteophytes: Bony spurs that often form in arthritic conditions and can contribute to fusion.
- Deformity: Any angular or rotational deformities of the knee.
- Erosions: Characteristic of inflammatory arthritis.
Different views, including anteroposterior (AP), lateral, and skyline (patellofemoral) views, are essential for a comprehensive assessment.
Computed Tomography (CT) Scan
CT scans provide more detailed cross-sectional images of the knee. They are particularly useful for:
- Precise characterization of bony fusion: CT can better define the extent and density of the bony bridge, which is crucial for surgical planning if intervention is considered.
- Assessing complex fractures: If ankylosis is post-traumatic, CT can delineate the exact location and nature of any old fracture lines that may have contributed to the fusion.
- Identifying loose bodies: Fragments of bone or cartilage that may be within the joint.
Magnetic Resonance Imaging (MRI)
MRI is the gold standard for visualizing soft tissues. While it may not be the primary tool for diagnosing bony ankylosis itself, it is invaluable for:
- Evaluating the extent of underlying soft tissue damage: Such as ligament tears, meniscal damage, or cartilage loss that may have preceded or accompanied the development of ankylosis.
- Detecting active inflammation: MRI can highlight areas of synovitis, which is important if an inflammatory arthritis is suspected as the cause.
- Assessing for infection: MRI is sensitive in detecting osteomyelitis or fluid collections suggestive of infection.
- Differentiating between true bony ankylosis and severe fibrous adhesions or muscle contractures: Although bony fusion is the defining feature of ankylosis, MRI can sometimes help delineate the extent of fibrous tissue involved, which might be relevant for treatment planning.
Management and Treatment Strategies for Knee Ankylosis
The management of knee ankylosis is challenging, as complete reversal of bony fusion is often impossible. Treatment strategies aim to alleviate pain, improve function, and enhance quality of life. The approach is highly individualized, depending on the cause of ankylosis, the degree of fusion, the patient’s overall health, and their functional goals.
Conservative Management
For some individuals, particularly those with less severe stiffness or when surgery is not an option, conservative measures may offer some relief.
Pain Management
- Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and inflammation, particularly if an underlying inflammatory process is still active. Analgesics may be prescribed for pain relief.
- Thermotherapy/Cryotherapy: Heat or cold application can provide temporary symptom relief.
Physical Therapy and Rehabilitation
While extensive range of motion is not achievable with true ankylosis, a tailored physical therapy program can still be beneficial.
- Strengthening: Exercises to strengthen the muscles around the knee (quadriceps, hamstrings, glutes) can improve stability and support.
- Gait training: Working with a physical therapist to optimize walking patterns and use of assistive devices can improve mobility and reduce the risk of secondary injuries.
- Range of Motion Exercises (Limited): Gentle passive or active-assisted range of motion exercises may be employed within the limits of motion to prevent further stiffness in adjacent joints and maintain muscle length.
Assistive Devices
- Braces and Orthotics: Custom-designed braces can provide support and improve alignment during ambulation.
- Walking Aids: Canes, crutches, or walkers can reduce the load on the knee and improve stability.
Surgical Interventions
When conservative measures are insufficient and functional impairment is significant, surgical intervention may be considered. The type of surgery depends on the nature and extent of the ankylosis.
Arthroplasty (Total Knee Replacement)
Total knee arthroplasty (TKA) is a common surgical procedure for severe knee osteoarthritis, and it can also be a viable option for knee ankylosis, particularly when the ankylosis is not severe or when there is significant associated arthritis.
- Procedure: The damaged joint surfaces are removed and replaced with prosthetic components.
- Challenges in Ankylosis: Performing a TKA in a fused knee presents significant surgical challenges. The surgeon must meticulously release the bony fusion and remove extensive scar tissue to expose the joint surfaces for implantation of the prosthesis. This often requires prolonged and technically demanding dissection.
- Post-operative Rehabilitation: Intense and diligent post-operative physical therapy is crucial to achieve functional improvement and prevent re-fusion or implant complications.
Arthrodesis (Joint Fusion)
In some cases, particularly when the knee is severely damaged, infected, or when reconstructive surgery is not feasible, surgical fusion of the knee (arthrodesis) might be considered. This procedure aims to create a stable, solid connection between the femur and tibia, eliminating motion but providing a pain-free, stable limb.
- Purpose: To create a solid, non-moving limb, which can be more functional than a painful, unstable, or severely deformed limb with limited motion.
- Positioning: The knee is fused in a functional position, typically around 0-10 degrees of extension, allowing for weight-bearing and a more stable gait.
- Indications: Often reserved for severe post-traumatic arthritis with extensive bone loss, chronic infection, or when other reconstructive options have failed.
Arthroscopic Procedures
In cases of less severe ankylosis or if significant arthrofibrosis (scar tissue) is the primary issue rather than complete bony fusion, arthroscopic surgery may be an option.
- Debridement and Adhesiolysis: Using small incisions and specialized instruments, the surgeon can carefully remove scar tissue, adhesions, and any bony spurs that are restricting motion.
- Goals: To restore a greater range of motion and alleviate pain.
- Limitations: Arthroscopic techniques are generally not suitable for complete bony ankylosis but can be effective for more superficial fibrous restrictions.

Prognosis and Long-Term Outlook
The prognosis for knee ankylosis is variable and depends heavily on the underlying cause, the severity of the fusion, and the success of the chosen treatment.
- Functional Outcome: Even with successful surgical intervention, achieving a full, pain-free range of motion similar to a healthy knee is often not possible. The goal is to maximize functional capacity and improve the patient’s ability to perform daily activities.
- Risk of Recurrence: In cases treated with arthroscopic procedures or even after arthroplasty, there is a risk of scar tissue reforming, leading to a recurrence of stiffness. Diligent post-operative rehabilitation is critical to minimize this risk.
- Lifestyle Modifications: Patients may need to make long-term lifestyle adjustments, such as avoiding high-impact activities and using assistive devices as needed.
Knee ankylosis remains a complex orthopedic challenge. A multidisciplinary approach involving orthopedic surgeons, rheumatologists, physical therapists, and occupational therapists is often necessary to provide comprehensive care and optimize outcomes for individuals affected by this condition. Continued research into novel regenerative techniques and improved surgical methods holds promise for enhancing the future management of knee ankylosis.
