The Critical Core of Hospital Care
The Intensive Care Unit (ICU), often referred to as the Intensive Therapy Unit (ITU) or Critical Care Unit (CCU), represents the pinnacle of hospital medical care. It’s a specialized department dedicated to patients facing life-threatening illnesses or injuries, requiring constant, intensive monitoring and treatment. Unlike general hospital wards, the ICU is equipped with advanced technology and staffed by highly trained medical professionals, all focused on stabilizing critically ill patients and providing them with the best possible chance of recovery.
The very nature of the conditions treated within an ICU demands a heightened level of vigilance. Patients here are typically those who have suffered severe trauma, undergone major surgery, experienced a heart attack or stroke, or are battling overwhelming infections like sepsis. Their physiological functions – breathing, heart rate, blood pressure, organ function – are often compromised, necessitating continuous oversight and immediate intervention. The ICU is designed to be a controlled environment where these vital signs can be meticulously tracked and managed, buffering the patient against further deterioration.
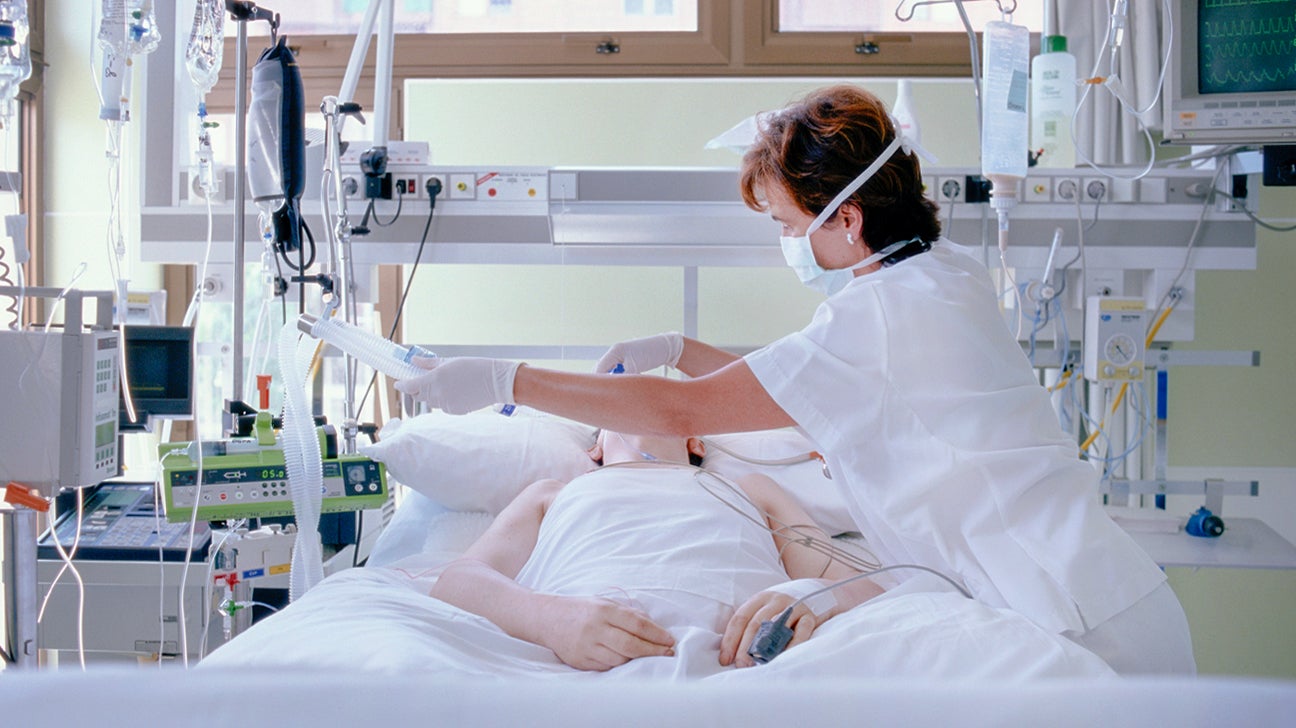
Who Needs ICU Care?
The decision to admit a patient to the ICU is never taken lightly. It is made by physicians based on a comprehensive assessment of the patient’s condition, prognosis, and the level of care required to sustain life. Common scenarios that necessitate ICU admission include:
- Severe Trauma: Patients with multiple serious injuries from accidents, falls, or violence, such as severe head injuries, internal bleeding, or extensive burns.
- Major Surgeries: Individuals undergoing complex or prolonged surgical procedures, especially those with pre-existing health conditions, may be transferred to the ICU for close post-operative monitoring.
- Cardiovascular Events: Patients experiencing heart attacks, severe arrhythmias, cardiac arrest, or requiring advanced cardiac support like intra-aortic balloon pumps or ventricular assist devices.
- Respiratory Failure: Individuals with conditions like acute respiratory distress syndrome (ARDS), severe pneumonia, or exacerbations of chronic lung diseases (like COPD or asthma) who require mechanical ventilation.
- Neurological Emergencies: Patients suffering from strokes, brain bleeds, seizures, or severe brain injuries that require continuous neurological monitoring and management.
- Sepsis and Septic Shock: Life-threatening responses to infection where organ function is severely impaired, often requiring vasopressors to maintain blood pressure and aggressive fluid resuscitation.
- Organ Failure: Patients with acute kidney injury, liver failure, or multi-organ dysfunction syndrome who require intensive support for failing organs.
- Post-Cardiac Arrest Resuscitation: Individuals who have had their heart stopped and successfully resuscitated, needing intensive monitoring and therapeutic measures to improve neurological outcomes.
The Environment of the ICU
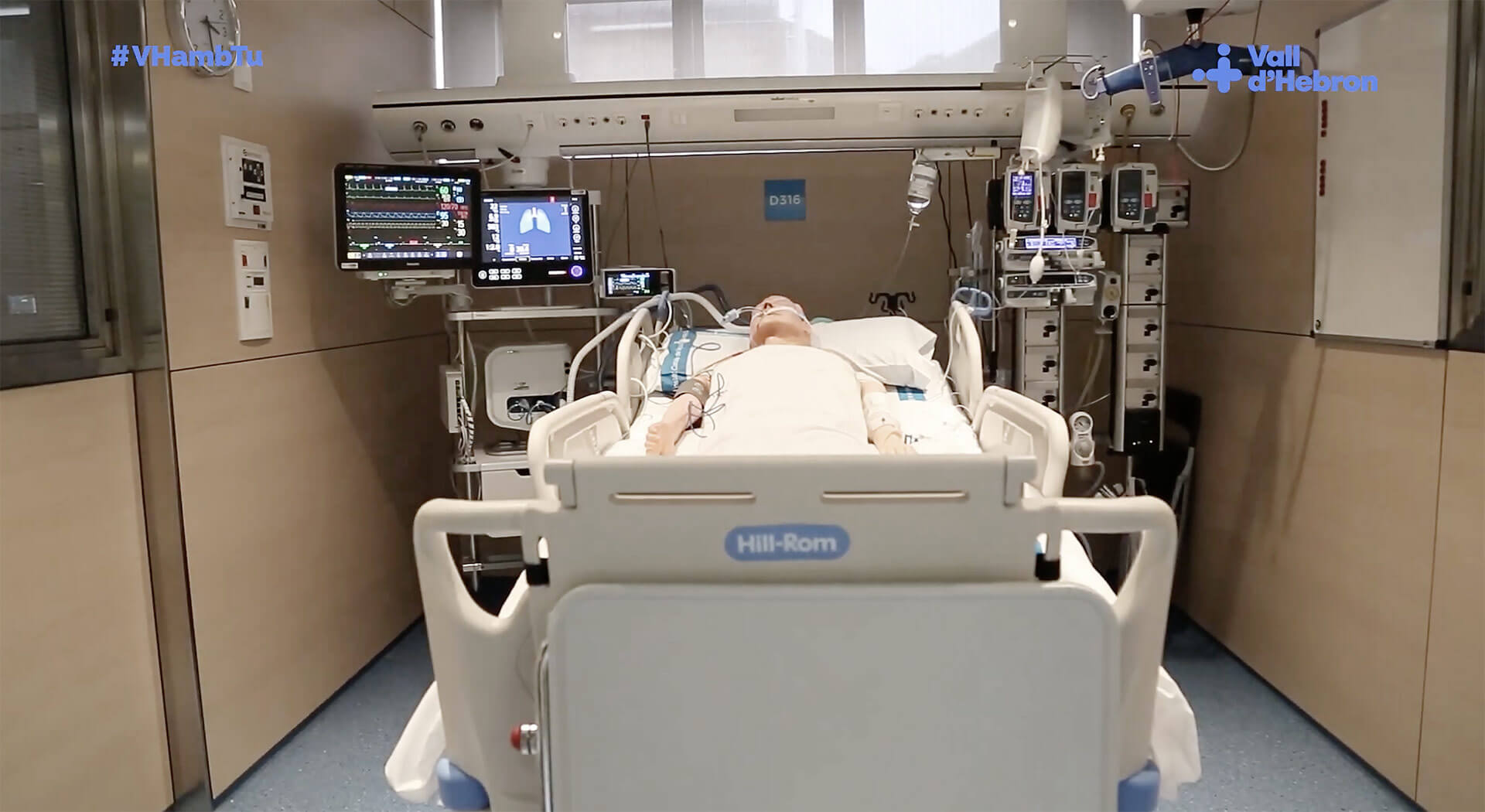
Stepping into an ICU is a stark contrast to a typical hospital floor. The atmosphere is one of quiet urgency, characterized by the rhythmic beeping of monitors and the hushed, focused movements of the medical team.
- Patient Rooms: ICU rooms are designed for optimal patient care and monitoring. They are typically private or semi-private to minimize infection risk and allow for closer observation. Each room is equipped with specialized medical equipment, including advanced patient monitoring systems, ventilators, and infusion pumps.
- Monitoring Technology: This is the cornerstone of ICU care. Sophisticated machines continuously track a multitude of vital signs:
- ECG (Electrocardiogram): Monitors heart rhythm and electrical activity.
- Blood Pressure: Continuous invasive (arterial line) or non-invasive monitoring.
- Oxygen Saturation (SpO2): Measures the oxygen levels in the blood.
- Respiration Rate: Tracks breathing patterns.
- Temperature: Core body temperature is closely monitored.
- Intracranial Pressure (ICP): In cases of head injury, this invasive monitoring helps detect dangerous pressure buildup in the skull.
- Hemodynamic Monitoring: Advanced techniques like pulmonary artery catheters can provide detailed information about the heart’s pumping function and fluid status.
- Ventilators: Mechanical ventilators are common in the ICU, assisting or completely taking over the breathing of patients who cannot do so adequately on their own. These machines deliver oxygen and help remove carbon dioxide from the lungs.
- Infusion Pumps: These precise devices deliver medications, fluids, and nutritional support intravenously at controlled rates, essential for managing complex drug regimens and maintaining fluid balance.
- Staffing: The ICU is staffed by a multidisciplinary team of highly specialized professionals. This includes:
- Intensivists: Physicians board-certified in critical care medicine, who lead the patient’s care team.
- Nurses: Critical care nurses possess specialized training in managing critically ill patients, operating complex equipment, and administering advanced therapies. They often have a lower patient-to-nurse ratio than in general wards.
- Respiratory Therapists: Manage ventilators, administer oxygen therapy, and assist with breathing treatments.
- Pharmacists: Ensure safe and effective medication management, often preparing complex intravenous drips.
- Physiotherapists: Help maintain muscle strength and mobility, crucial for preventing complications during prolonged immobility.
- Dietitians: Ensure appropriate nutritional support, which is vital for recovery.
- Technicians: Operate diagnostic equipment and assist with patient care.
- Family Presence: While historically restricted, many ICUs now recognize the importance of family involvement and have policies allowing for visitation, understanding that family support can be beneficial for patient recovery.
The Multidisciplinary Team in Action
The strength of the ICU lies in its integrated, team-based approach to patient care. The complex needs of critically ill patients require the expertise of various specialists working in concert.
Intensivists: The Captains of the Ship
Intensivists are the central figures in the ICU. They are medical doctors with specialized training in diagnosing and managing a wide range of critical conditions. Their responsibilities are extensive:
- Overall Medical Management: They oversee the patient’s entire treatment plan, making crucial decisions about diagnostics, therapies, and interventions.
- Coordination of Care: They orchestrate the efforts of the various specialists involved, ensuring seamless communication and a unified approach.
- Crisis Management: They are adept at rapidly assessing and responding to life-threatening emergencies that can arise in the ICU.
- Prognostication and Decision Making: They guide discussions with families regarding the patient’s prognosis and assist in complex end-of-life care decisions when necessary.
Critical Care Nurses: The Frontline Guardians
Critical care nurses are the eyes and ears of the ICU, providing continuous, hands-on care. Their role is demanding and multifaceted:
- Direct Patient Care: Administering medications, monitoring vital signs, assisting with hygiene, and providing emotional support.
- Equipment Management: Operating and troubleshooting complex machinery like ventilators, dialysis machines, and advanced monitoring systems.
- Early Recognition of Deterioration: Their keen observation skills allow them to detect subtle changes in a patient’s condition that might signal impending problems.
- Patient Advocacy: They act as advocates for their patients, ensuring their needs are met and their comfort is prioritized.
- Family Communication: They often serve as a liaison between the medical team and the patient’s family, providing updates and answering questions.
Allied Health Professionals: Essential Support
Beyond physicians and nurses, a range of allied health professionals play vital roles:
- Respiratory Therapists: Essential for patients requiring mechanical ventilation or breathing support. They manage the ventilators, monitor lung function, and perform other respiratory interventions.
- Pharmacists: Critical for managing the complex medication regimens in the ICU. They advise on drug selection, dosages, potential interactions, and monitor for adverse effects.
- Physiotherapists: Begin rehabilitation even when patients are critically ill, focusing on preventing muscle atrophy, contractures, and complications of immobility. They also assist with weaning patients from ventilators.
- Dietitians: Ensure that critically ill patients receive adequate nutrition, which is crucial for healing and recovery, often through specialized feeding tubes or intravenous methods.
- Technicians: Such as cardiovascular technicians or radiology technicians, who perform diagnostic tests and procedures necessary for patient management.
The constant collaboration and communication among these professionals are paramount. Regular multidisciplinary rounds, where the entire team discusses each patient’s progress and care plan, are a hallmark of effective ICU management.
Innovations and Challenges in Critical Care
The field of critical care medicine is dynamic, constantly evolving with technological advancements and new research findings. However, the ICU also faces significant challenges.
Technological Advancements
- Advanced Monitoring: Beyond basic vital signs, newer technologies allow for more sophisticated monitoring, including continuous cardiac output monitoring, cerebral oximetry (measuring oxygen levels in the brain), and advanced hemodynamic assessment tools.
- Minimally Invasive Techniques: The development of less invasive methods for procedures like central line insertion, arterial line placement, and even certain forms of organ support has reduced patient trauma and recovery times.
- Robotics and AI: While still in early stages for direct patient care, AI is being explored for predictive analytics to identify patients at risk of deterioration and for assisting with data analysis. Robotic assistance is also becoming more common in surgical procedures that may lead to ICU admission.
- Tele-ICU: Remote monitoring and consultation services are increasingly being implemented, allowing critical care specialists to oversee patients in ICUs at facilities that may lack on-site intensivists. This extends expertise to underserved areas.
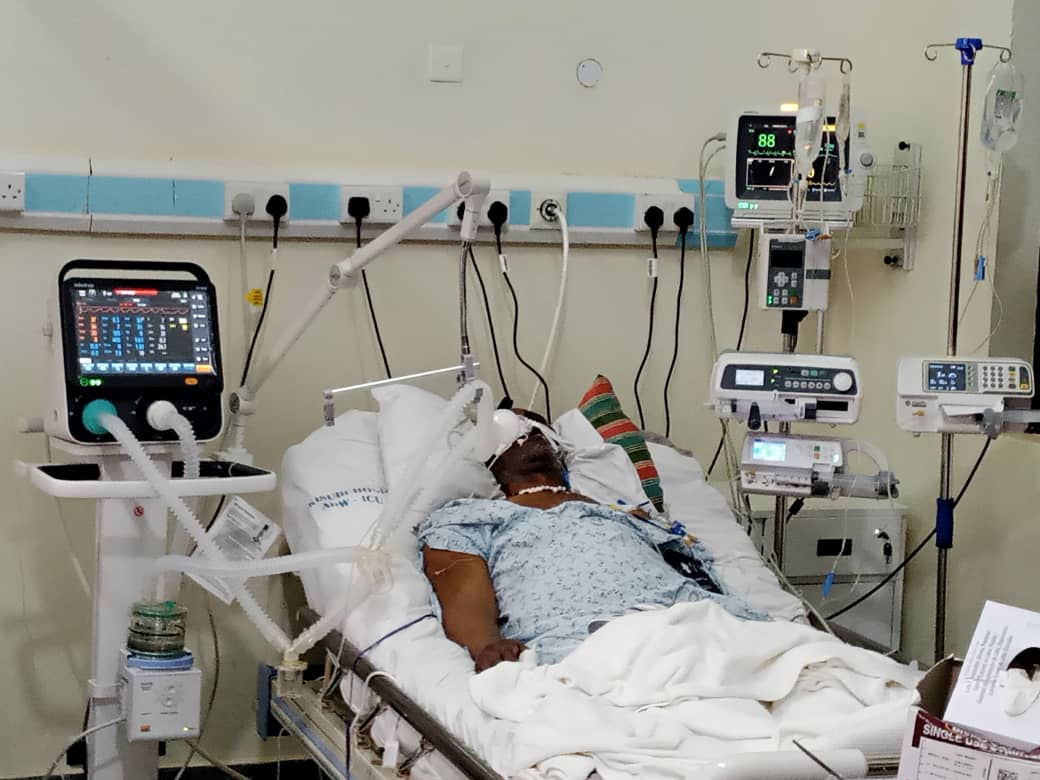
Challenges in Critical Care
- Resource Strain: ICUs are resource-intensive units, requiring significant investment in equipment, technology, and highly skilled personnel. This can lead to challenges with bed availability and staffing shortages.
- Patient Complexity: Patients admitted to the ICU often have multiple co-morbidities and complex conditions, making their management inherently challenging and prolonging recovery.
- Moral Distress and Burnout: The high-stakes environment, the constant battle against death, and the emotional toll of caring for critically ill patients can lead to significant moral distress and burnout among ICU staff.
- Cost of Care: ICU care is among the most expensive forms of healthcare due to the intensity of monitoring, specialized equipment, and the expertise required.
- Infection Control: Despite stringent protocols, the presence of invasive devices and immunocompromised patients makes the ICU a higher-risk environment for healthcare-associated infections.
Despite these challenges, the ICU remains an indispensable part of modern healthcare. It is a place where advanced medicine, cutting-edge technology, and dedicated human effort converge to offer a lifeline to those facing the most critical moments of their lives. The commitment of its multidisciplinary teams is what truly defines the Intensive Care Unit as a sanctuary of hope and healing.
