Cytology testing, a cornerstone of modern diagnostic medicine, is a specialized branch of pathology that focuses on the microscopic examination of individual cells. Unlike histology, which examines intact tissues, cytology analyzes cells that have been shed from the body or collected through various sampling techniques. This fundamental difference allows for the early detection of a wide range of diseases, including cancers, precancerous conditions, and infectious agents, often with minimal invasiveness. The insights gleaned from cytology are crucial for guiding clinical decisions, monitoring treatment efficacy, and ultimately improving patient outcomes. Understanding the principles, applications, and techniques behind cytology testing provides a valuable perspective on its significance in healthcare.
The Fundamental Principles of Cytology
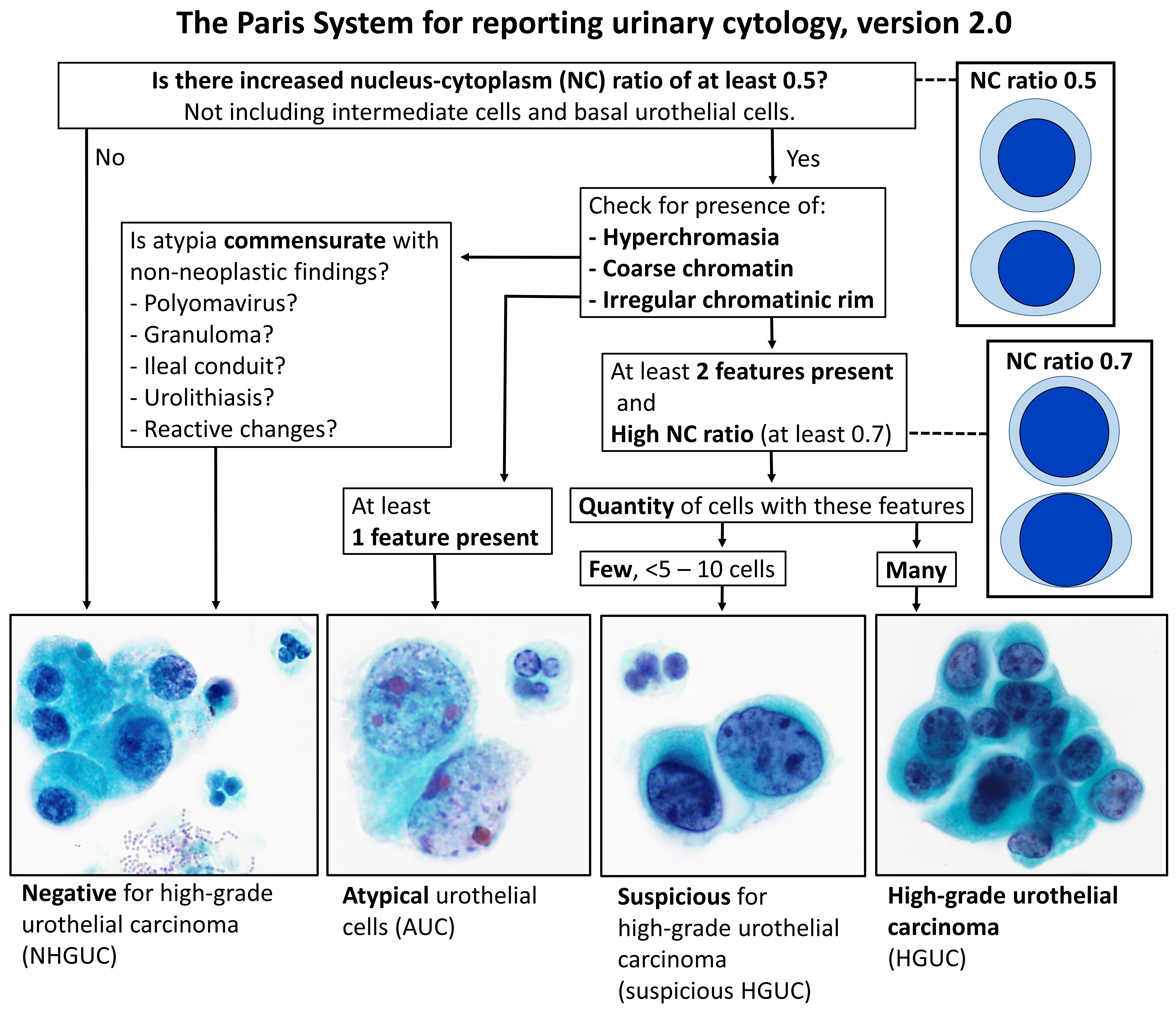
At its core, cytology is about cell morphology. Pathologists and cytotechnologists meticulously scrutinize the physical characteristics of individual cells to identify abnormalities. This involves examining various cellular features, including the size and shape of the cell, the characteristics of its nucleus (such as its size, chromatin pattern, and presence of nucleoli), and the appearance of the cytoplasm. Changes in these features can be indicative of disease processes. The process relies on specialized staining techniques that highlight cellular components, making subtle differences visible under high magnification.
Cellular Morphology: The Key to Diagnosis
The diagnostic power of cytology rests heavily on the interpretation of cellular morphology. Every cell possesses a unique set of characteristics that reflect its origin and function. When cells undergo pathological changes, these characteristics are altered in predictable ways. For instance, cancerous cells often exhibit nuclear enlargement, irregular nuclear contours, hyperchromasia (darkly stained chromatin), and prominent nucleoli. The cytoplasm may also show changes, such as increased vacuolation or abnormal inclusions. Cytologists are trained to recognize these subtle yet significant deviations from normal cellular appearance, which serve as critical clues in identifying disease.
Staining Techniques: Illuminating Cellular Details
To effectively visualize cellular structures and identify abnormalities, cytological specimens are typically stained. The most common and widely used staining method in diagnostic cytology is the Papanicolaou stain, often referred to as the “Pap stain.” This complex multi-step stain utilizes a combination of acidic and basic dyes to differentiate various cellular components, including the nucleus and cytoplasm, in shades of blue, pink, and green. Other stains, such as Hematoxylin and Eosin (H&E), Giemsa, and Papanicolaou’s stain variations, are also employed depending on the specimen type and the suspected pathology. These stains are not merely aesthetic; they are essential tools that enhance contrast and highlight specific cellular features, making them amenable to microscopic analysis.
Specimen Collection Methods: Obtaining the Cells
The success of cytology hinges on obtaining a representative sample of cells. Various methods are employed for specimen collection, each suited to different anatomical sites and suspected conditions. These methods are often minimally invasive, contributing to the appeal and widespread use of cytology.
Liquid-Based Cytology (LBC)
Liquid-based cytology has largely replaced conventional smear methods for many gynecological and non-gynecological specimens. In LBC, the cellular material collected is placed in a liquid preservative solution. This approach not only preserves the cells but also allows for processing that removes debris and blood, creating a cleaner, more uniform slide for examination. This often leads to improved sample quality and a reduction in unsatisfactory or borderline results.
Conventional Smears
In conventional smear techniques, cells are directly smeared onto a glass slide, which is then immediately fixed and stained. While still utilized for certain specimen types, this method can sometimes result in overlapping cells, obscuration by blood or inflammatory exudate, and a higher rate of unsatisfactory samples compared to LBC.
Fine Needle Aspiration (FNA)
Fine Needle Aspiration is a procedure where a thin needle is used to collect cells from a suspicious lump or mass, such as those found in the breast, thyroid, or lymph nodes. The aspirated material is then spread on slides for cytological examination. FNA is a highly valuable technique for distinguishing between benign and malignant lesions, often avoiding the need for more invasive surgical biopsies.
Exfoliative Cytology
Exfoliative cytology involves the examination of cells that are naturally shed from the body’s surfaces. Examples include:
- Gynecological Cytology (Pap Smear): The most well-known application, where cells are collected from the cervix to screen for cervical cancer and precancerous changes.
- Urine Cytology: Used to detect cancers of the urinary tract, such as bladder cancer, by examining cells shed into the urine.
- Sputum Cytology: Analysis of coughed-up material to identify lung cancer or other respiratory conditions.
- Serous Effusion Cytology: Examination of fluids collected from body cavities (e.g., pleural, peritoneal, pericardial) to detect cancers that have spread to these areas or to diagnose inflammatory conditions.
Applications of Cytology Testing
The versatility of cytology testing allows for its application across a broad spectrum of medical specialties and diagnostic scenarios. Its ability to provide rapid, cost-effective, and often minimally invasive diagnoses makes it an indispensable tool in modern healthcare.
Cancer Screening and Diagnosis
Cytology plays a pivotal role in the early detection and diagnosis of various cancers. For many malignancies, cytology offers a less invasive alternative to tissue biopsy, allowing for prompt identification of cancerous or precancerous cells.
Cervical Cancer Screening
The Pap smear, a cornerstone of gynecological health for decades, is a prime example of cytology’s impact. By examining cells from the cervix, it can detect precancerous changes (dysplasia) and early-stage cervical cancer, enabling timely intervention and significantly reducing mortality rates from this disease. The advent of human papillomavirus (HPV) testing, often performed in conjunction with cytology, has further revolutionized cervical cancer prevention.
Detection of Other Cancers
Beyond cervical cancer, cytology is vital for detecting other malignancies:
- Lung Cancer: Sputum cytology and bronchoalveolar lavage cytology can identify malignant cells shed from the lung.
- Bladder Cancer: Urine cytology is a key tool in the diagnosis and monitoring of bladder cancer.
- Thyroid Nodules: Fine Needle Aspiration (FNA) of thyroid nodules is crucial for determining whether a nodule is benign or malignant.
- Breast Masses: FNA of breast lumps can help differentiate between benign conditions and breast cancer.
- Gastrointestinal Cancers: Cytology via endoscopic brushing or FNA can aid in the diagnosis of cancers of the esophagus, stomach, and pancreas.
- Lymph Node Metastases: FNA of enlarged lymph nodes can detect the presence of metastatic cancer from primary sites elsewhere in the body.
Detection of Infectious Agents
Cytology is not limited to cancer detection; it is also highly effective in identifying various infectious organisms. By examining cellular changes and the presence of microorganisms, cytologists can help diagnose infections that might otherwise be difficult to pinpoint.
Viral Infections
Certain cellular changes are characteristic of viral infections. For example, the characteristic “owl eye” nuclear inclusions seen in cytomegalovirus (CMV) infection are readily identifiable on cytology. Viral cytopathic effects can also be observed in herpes simplex virus (HSV) infections.
Bacterial and Fungal Infections
While definitive diagnosis of many bacterial and fungal infections relies on culture, cytology can provide initial evidence. For instance, the presence of inflammatory cells and characteristic cellular debris in samples from infected sites can be suggestive of a bacterial infection. Special stains can highlight the presence of certain fungi, such as Candida or Aspergillus. In cases of tuberculosis, acid-fast bacilli might be identified within macrophages in sputum or other bodily fluids.
Parasitic Infections
Cytology can also be used to detect parasitic infections. For example, examination of stool samples can reveal the presence of intestinal parasites, and certain parasites may be identified in body fluids or tissue aspirates.
Non-Malignant Conditions and Inflammatory Processes
Cytology’s utility extends to the diagnosis and monitoring of a wide range of non-malignant conditions, including various inflammatory processes and benign lesions.
Inflammatory Diseases
Cytology can help identify the type and severity of inflammation. The presence and types of inflammatory cells (e.g., neutrophils, lymphocytes, eosinophils, macrophages) within a sample can provide crucial diagnostic clues. For example, a predominance of eosinophils might suggest an allergic reaction or parasitic infection, while neutrophils could indicate a bacterial infection.
Benign Lesions
Many benign growths and conditions present with characteristic cellular patterns that cytology can identify. For instance, benign thyroid nodules, fibrocystic changes in the breast, or reactive changes in the cervix can be distinguished from malignant counterparts through careful cytological examination.
Monitoring Treatment Response
In some cases, cytology can be used to monitor the effectiveness of treatment. For example, a decrease in abnormal cells in a Pap smear after treatment for cervical dysplasia, or the absence of malignant cells in effusions after chemotherapy for ovarian cancer, can indicate a positive response to therapy.
The Cytology Workflow and Quality Assurance
The accurate interpretation of cytological specimens requires a systematic approach and stringent quality control measures. From specimen collection to final reporting, each step is critical in ensuring reliable diagnostic outcomes.
The Role of the Cytotechnologist
Cytotechnologists are highly trained professionals who form the backbone of the cytology laboratory. They are responsible for preparing and screening cytological slides under microscopic examination. Their keen eye for detail and extensive knowledge of cellular morphology enable them to identify normal and abnormal cells, flagging suspicious findings for review by a pathologist. They play a crucial role in the initial triage of slides, ensuring that potentially significant abnormalities are not overlooked.
Pathologist Review and Final Diagnosis
While cytotechnologists perform the initial screening, the final diagnosis rests with a cytopathologist. The pathologist reviews slides identified as abnormal by the cytotechnologist, as well as a selection of normal slides for quality control. They correlate the cytological findings with clinical information, imaging studies, and sometimes, subsequent histological findings to render a definitive diagnosis. This collaborative approach ensures the highest level of accuracy and reliability in cytological diagnoses.
Quality Assurance and Proficiency Testing
Given the critical nature of cytological diagnoses, rigorous quality assurance (QA) programs are essential. These programs encompass a multi-faceted approach to ensure the consistent accuracy and reliability of the laboratory’s performance.
Internal Quality Control
Internal QA measures include regular inter-observer and intra-observer comparisons (where different cytotechnologists or the same cytotechnologist at different times review the same slides), detailed case reviews, and ongoing training for staff. Monitoring of turnaround times and rates of unsatisfactory specimens are also key components of internal QA.
External Proficiency Testing
External proficiency testing, often mandated by regulatory bodies, involves laboratories participating in blind slide studies administered by external agencies. Laboratories receive sets of slides and are evaluated on their ability to correctly identify abnormalities. Consistent performance in these tests is vital for accreditation and maintaining operational licenses. This external validation provides an objective measure of a laboratory’s diagnostic competence.
Bethesda System for Gynecologic Cytology
The development and widespread adoption of standardized reporting systems, such as the Bethesda System for Gynecologic Cytology, have significantly improved the clarity and consistency of diagnoses. This system provides specific terminology for describing cervical cytology findings, categorizing them into clear diagnostic groups (e.g., Negative for Intraepithelial Lesion or Malignancy (NILM), Atypical Squamous Cells of Undetermined Significance (ASC-US), Low-grade Squamous Intraepithelial Lesion (LSIL), High-grade Squamous Intraepithelial Lesion (HSIL), and Malignant). This standardization facilitates better communication between laboratories and clinicians and ensures that patients receive appropriate management based on well-defined diagnostic criteria. Similar standardized systems are being developed and implemented for non-gynecological cytology to further enhance diagnostic consistency across the field.
In conclusion, cytology testing is a dynamic and essential diagnostic discipline that leverages the microscopic examination of individual cells to detect a wide array of diseases. Its minimally invasive nature, cost-effectiveness, and broad applicability in screening, diagnosis, and monitoring underscore its profound importance in contemporary healthcare, contributing significantly to improved patient care and health outcomes.
