Cortical Visual Impairment (CVI), often referred to as Cerebral Visual Impairment, stands as a leading cause of visual impairment in children in developed countries. Unlike traditional forms of visual impairment that stem from issues within the eye itself, CVI originates in the brain. It is a neurological condition where the eyes are healthy and capable of sending clear images to the brain, but the brain struggles to interpret or process these visual signals effectively. This distinction is crucial, as it fundamentally alters how CVI is diagnosed, understood, and managed, requiring a multidisciplinary approach that blends neurology, ophthalmology, education, and innovative therapeutic strategies.
Understanding CVI involves delving into the intricate pathways of the brain responsible for vision. It’s not simply about “seeing,” but about “understanding what is seen.” This complex process involves multiple areas of the brain, including the occipital cortex where primary visual processing occurs, as well as higher-order areas responsible for interpreting spatial relationships, recognizing objects and faces, perceiving motion, and integrating vision with other senses. Damage or dysfunction in any of these areas can manifest as CVI, presenting a unique and often variable set of visual challenges for affected individuals.
The impact of CVI extends far beyond mere sight. It significantly affects an individual’s ability to navigate their environment, interact with others, learn new concepts, and develop essential life skills. Early identification and tailored interventions are paramount to optimizing visual function and promoting overall development. This article will explore the multifaceted nature of CVI, from its neurological underpinnings and diverse causes to its characteristic behaviors, diagnostic processes, and the innovative strategies employed to support those living with this brain-based visual impairment.
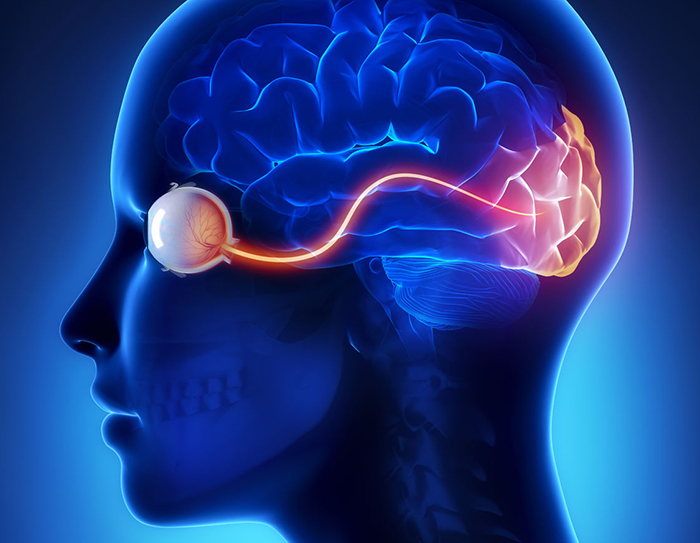
Understanding Cortical Visual Impairment (CVI)
At its core, CVI is a challenge of the brain’s ability to process visual information. While the eyes may be perfectly healthy and capable of registering light and images, the neural pathways and cortical areas responsible for interpreting these signals are compromised. This leads to a wide spectrum of visual difficulties that are often inconsistent and can fluctuate depending on various internal and external factors.
Defining CVI: A Brain-Based Visual Condition
CVI is defined as a decreased visual acuity or visual functioning due to a neurological disorder affecting the visual pathways and/or the visual cortex of the brain. The term “cortical” refers to the cerebral cortex, the outer layer of the brain where much of the complex processing occurs. Therefore, CVI is not an eye problem, but rather a brain problem. This critical distinction guides all aspects of diagnosis and intervention. Individuals with CVI can have perfect ocular health, including normal retinal function and clear lenses, yet still experience severe visual impairment because their brains cannot make sense of the visual input. It challenges the conventional understanding of blindness and low vision, shifting the focus from the organ of sight to the neural network responsible for perception.
Distinguishing CVI from Ocular Impairments
The primary difference between CVI and ocular visual impairment (OVI) lies in the anatomical location of the damage. OVI results from abnormalities in the eye itself – conditions like cataracts, glaucoma, retinal diseases, or optic nerve damage. For instance, a child with cataracts might have blurry vision because light cannot properly enter the eye. In contrast, a child with CVI might have perfectly clear images reaching their brain, but the brain struggles with tasks such as focusing on an object, recognizing a familiar face, or understanding spatial relationships.
This distinction has profound implications for treatment. While OVI often benefits from ophthalmic interventions like surgery, corrective lenses, or medication, CVI requires neurological and rehabilitative approaches. Management strategies for CVI focus on teaching the brain to interpret visual information more effectively, often by modifying the environment, using specific visual targets, and integrating other sensory inputs.
The Neurological Basis of Visual Processing
Vision is a complex neurological phenomenon involving more than just the eyes and the primary visual cortex. The process begins when light enters the eye, strikes the retina, and converts into electrical signals. These signals travel along the optic nerves to the thalamus, a relay station in the brain, and then to the primary visual cortex in the occipital lobe. However, this is just the beginning. From the primary visual cortex, information branches out into two main pathways: the dorsal stream (the “where” pathway) which processes spatial information, motion, and location, and the ventral stream (the “what” pathway) which is responsible for object recognition, face recognition, and color perception.
Damage to any part of this intricate network—from the optic radiations leading to the cortex, to the visual cortex itself, or the higher-order processing areas—can result in CVI. The specific location and extent of brain damage determine the unique characteristics and severity of CVI in each individual. Modern neuroimaging techniques, which represent a significant area of “Tech & Innovation” in medicine, play a crucial role in identifying these areas of damage or dysfunction, thereby aiding in diagnosis and personalized intervention planning.
Causes, Risk Factors, and Prevalence of CVI
CVI is a heterogeneous condition, meaning it can arise from a wide range of neurological events or conditions that affect the developing brain. Its prevalence is on the rise, partly due to advances in medical technology that allow for the survival of infants who might previously not have survived, but who may subsequently develop neurological damage.
Common Etiologies and Associated Conditions
The most common causes of CVI involve damage to the brain before, during, or shortly after birth. These etiologies include:
- Perinatal Hypoxia-Ischemia: A lack of oxygen and blood flow to the brain, often due to complications during birth or severe prematurity. This is a leading cause.
- Intraventricular Hemorrhage (IVH): Bleeding into the brain’s ventricles, particularly common in premature infants.
- Periventricular Leukomalacia (PVL): Damage to the white matter of the brain, especially around the ventricles, also common in prematurity.
- Central Nervous System Infections: Such as meningitis or encephalitis.
- Hydrocephalus: A buildup of cerebrospinal fluid in the brain.
- Traumatic Brain Injury (TBI): Resulting from accidents or abuse.
- Genetic and Metabolic Disorders: Certain rare genetic conditions or metabolic imbalances can also lead to brain abnormalities affecting vision.
- Brain Malformations: Abnormal development of brain structures during gestation.
Many children with CVI also present with other neurodevelopmental challenges, such as cerebral palsy, epilepsy, intellectual disabilities, and speech/language delays. This comorbidity underscores the widespread impact of neurological damage and necessitates a holistic approach to care and intervention.
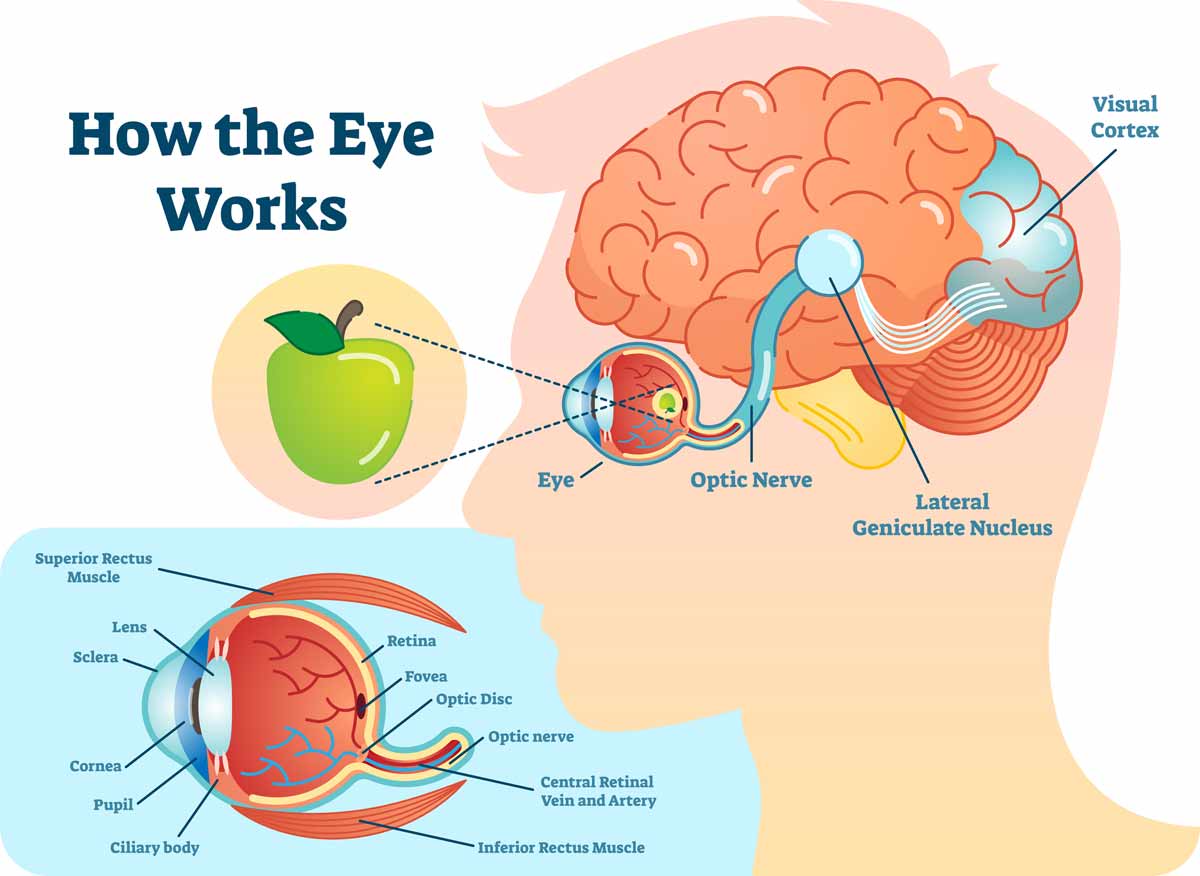
Early Identification and Developmental Impact
Early identification of CVI is critical, yet it can be challenging. Because the eyes appear healthy, CVI is often missed during routine eye exams. Pediatricians and parents may initially attribute a child’s lack of visual response or unusual visual behaviors to other developmental delays. Awareness among medical professionals, educators, and families is key to prompting timely referrals to specialists.
The developmental impact of CVI is profound. Vision is a primary driver of development, influencing motor skills, language acquisition, social interaction, and cognitive growth. A child who cannot effectively see their environment may struggle to reach for objects, follow moving targets, recognize facial expressions, or even orient themselves in space. This can lead to delays in gross and fine motor skills, communication difficulties, and challenges in forming social bonds. Early intervention aims to harness the brain’s plasticity, helping to establish new neural pathways or strengthen existing ones to improve visual processing.

Characteristics and Behaviors Associated with CVI
CVI is known for its wide spectrum of presentation. No two individuals with CVI are exactly alike, and their visual behaviors can change over time and in different environments. Recognizing these characteristic behaviors is crucial for accurate diagnosis and effective intervention.
Variability in Visual Functioning
A hallmark of CVI is the variability of visual response. An individual with CVI might perform a visual task perfectly one moment and struggle immensely with the same task moments later. This variability can be influenced by factors such as:
- Fatigue: Visual processing requires significant cognitive effort for individuals with CVI.
- Environmental Complexity: Busy backgrounds, clutter, or too many visual stimuli can overwhelm the visual system.
- Familiarity: Recognizing familiar objects or people is often easier than new ones.
- Emotional State: Stress, anxiety, or excitement can impact visual performance.
- Illumination: Specific lighting conditions might be beneficial or detrimental.
- Presentation Speed: Fast-moving objects or rapid changes in visual information can be difficult to process.
This inconsistency can be frustrating for both the individual and their caregivers, making it difficult to assess their true visual capabilities and plan consistent support.
Behavioral Indicators and Unique Visual Responses
Despite the variability, several common behavioral indicators are often observed in individuals with CVI:
- Preference for specific colors: Often red or yellow, as these colors tend to be highly salient and visually “pop.”
- Need for movement: Visual attention is often attracted by movement, even subtle wiggling of an object.
- Latency in visual response: It may take longer for an individual with CVI to look at, recognize, or respond to a visual stimulus.
- Visual field preferences: A tendency to look at objects from a specific angle or to use peripheral vision rather than direct gaze.
- Difficulty with complexity: Struggling with busy backgrounds, crowded environments, or objects with multiple features.
- Light gazing: Staring directly at light sources, seemingly fascinated by them.
- Difficulty with depth perception and spatial relationships: Leading to clumsiness or challenges navigating stairs or uneven surfaces.
- Atypical gaze: Not making eye contact or appearing to look “through” people or objects.
- Impact of sensory overload: Visual performance decreasing when other senses are highly stimulated (e.g., loud noises, strong smells).
These behaviors are not choices but rather manifestations of how the brain is processing visual information. Understanding these patterns is essential for creating an accessible and supportive environment.
Impact on Learning and Functional Vision
The challenges posed by CVI profoundly impact learning and the development of functional vision skills—the ability to use vision for daily tasks. In educational settings, children with CVI may struggle with reading, writing, recognizing symbols, and accessing visual information presented on blackboards or screens. Traditional teaching methods often rely heavily on visual input, making accommodations crucial.
Functional vision assessment for CVI is not about measuring acuity on an eye chart but about understanding how the child uses their vision in real-world contexts. It assesses their ability to find objects, navigate familiar and unfamiliar spaces, respond to visual cues, and interact visually with their environment. The goal is to maximize their useable vision and equip them with strategies to compensate for their visual processing difficulties, empowering them to participate fully in learning and daily life.
Diagnosis and Assessment of CVI
Diagnosing CVI is a complex process that requires expertise across multiple medical and educational disciplines. It involves ruling out ocular causes, identifying brain damage, and meticulously observing visual behaviors. Significant advancements in diagnostic technologies represent a key area of “Tech & Innovation” enabling more precise identification and understanding of CVI.
The Multidisciplinary Diagnostic Process
A comprehensive CVI diagnosis typically involves a team of specialists, including:
- Pediatric Ophthalmologist: To ensure the eyes are structurally healthy and rule out ocular causes of visual impairment.
- Pediatric Neurologist: To identify the underlying brain injury or condition causing the CVI. This specialist uses advanced imaging and neurological assessments.
- Developmental Pediatrician: To assess overall development and identify co-occurring conditions.
- Neuropsychologist: To evaluate cognitive functions related to visual perception and learning.
- Teacher of Students with Visual Impairments (TVI): Specializing in CVI, they conduct functional vision assessments and provide educational recommendations.
- Occupational Therapist: To address fine motor skills, sensory processing, and daily living activities.
This collaborative approach ensures that all aspects of the child’s visual and neurological health are considered, leading to a more accurate diagnosis and a holistic intervention plan.
Specialized Assessment Tools and Techniques
Traditional visual acuity tests are often insufficient for diagnosing or assessing CVI. Instead, specialists utilize specialized assessment tools and techniques that focus on functional vision and specific CVI characteristics. These might include:
- CVI Range Assessment: A structured observation tool that evaluates ten key visual characteristics associated with CVI, assigning a score that helps categorize the severity of CVI and guide intervention.
- Dynamic Visual Acuity Testing: Measuring vision while the head is moving, which can reveal specific difficulties.
- Visual Attention and Field Testing: Observing how a child responds to stimuli presented in different visual fields and under varying levels of complexity.
- Observation in Natural Environments: Assessing how the child uses their vision in familiar settings, such as home or school, where the visual demands are real-world.
These assessments are often qualitative and require experienced evaluators who can interpret subtle visual behaviors and preferences.
The Role of Medical Imaging
Medical imaging technologies are indispensable in the diagnosis of CVI. Technologies like Magnetic Resonance Imaging (MRI), particularly advanced sequences like Diffusion Tensor Imaging (DTI), provide detailed images of the brain structure and white matter pathways (like the optic radiations), which are often damaged in CVI.
- MRI: Can identify areas of brain damage, malformations, or previous injuries (e.g., strokes, hemorrhages, areas of oxygen deprivation).
- DTI: A specialized MRI technique that maps the diffusion of water molecules in the brain, allowing clinicians to visualize the integrity and connectivity of white matter tracts, including those crucial for visual processing. This offers insights into the neurological underpinnings of CVI that standard MRI might miss.
These “Tech & Innovation” advancements allow clinicians to pinpoint the neurological origin of CVI, helping to correlate specific brain damage with observed visual behaviors and guide prognosis.
Intervention Strategies and Supporting Individuals with CVI
Living with CVI requires ongoing support and tailored interventions designed to optimize an individual’s visual function and overall development. These strategies often blend educational approaches with assistive technologies and environmental modifications, reflecting a commitment to innovation in personalized care.
Tailored Educational and Therapeutic Approaches
Interventions for CVI are highly individualized and focus on leveraging an individual’s strengths while addressing their specific visual challenges. Key approaches include:
- Environmental Simplification: Reducing visual clutter, using plain backgrounds, and highlighting essential information to minimize visual overload.
- Use of Preferred Visual Characteristics: Incorporating specific colors (e.g., red or yellow), movement, and familiar objects into learning materials and daily routines.
- Structured Presentation: Presenting one item at a time, allowing for latency in response, and ensuring the child is ready to attend visually.
- Multi-sensory Learning: Integrating touch, sound, and smell with visual input to provide redundant cues and reinforce learning. For example, pairing a visual of an object with its tactile exploration and auditory label.
- Direct Instruction in Visual Skills: Explicitly teaching skills like visual scanning, tracking, and looking for specific features.
- Visual Schedule and Routines: Providing predictable visual and physical environments to reduce cognitive load and enhance participation.
These strategies are continuously refined through ongoing research and feedback, embodying an iterative approach to “Tech & Innovation” in special education.
Environmental Modifications and Assistive Technologies
Technology plays a vital role in empowering individuals with CVI. “Tech & Innovation” has yielded a range of assistive technologies and environmental modifications that can significantly enhance functional vision and independence:
- High-Contrast Materials: Using black-on-white or yellow-on-black for text and images to maximize visibility.
- Lighting Adjustments: Optimizing natural and artificial lighting to reduce glare or highlight important areas. Sometimes targeted lighting on a task is crucial.
- Assistive Software: Screen readers, text-to-speech programs, and magnification software on computers and tablets.
- Tactile and Auditory Cues: Incorporating raised line drawings, braille (for those with severe CVI), and auditory feedback devices.
- Augmentative and Alternative Communication (AAC) devices: For individuals with concurrent communication challenges, these devices often use simplified visual displays.
- Accessible Digital Content: Ensuring websites, apps, and educational materials are designed with CVI-friendly principles in mind (e.g., customizable colors, minimal animations, clear navigation).
- Specialized Toys and Learning Tools: Designed with specific CVI characteristics in mind, featuring high contrast, movement, and preferred colors.
These technological aids, developed through innovative engineering and design, are crucial for creating inclusive environments and fostering learning.
The Importance of Early and Ongoing Support
The journey with CVI is lifelong, and the need for support evolves with age. Early intervention services are critical for infants and toddlers, focusing on foundational visual skills and overall development. As children grow, support shifts to educational accommodations, vocational training, and independent living skills. For adults with CVI, emphasis may be on workplace adaptations, community mobility, and maintaining independence.
Ongoing research continues to deepen our understanding of CVI, exploring new diagnostic biomarkers, developing more effective therapies, and designing innovative assistive technologies. This continuous pursuit of knowledge and practical solutions underscores the dynamic nature of “Tech & Innovation” in addressing complex neurological conditions like CVI. By embracing this spirit of innovation, we can continue to improve the lives of individuals with Cortical Visual Impairment, empowering them to reach their full potential.
