The buffy coat, a thin, whitish layer found above the red blood cell sediment after centrifugation of blood, is far more than just an incidental byproduct of hematological analysis. It represents a concentrated collection of critical cellular components that play pivotal roles in immune response, blood clotting, and tissue regeneration. Understanding the composition and function of the buffy coat is fundamental to fields ranging from diagnostic medicine and transfusion science to cutting-edge regenerative therapies. While seemingly simple in its appearance, this layer is a microcosm of the body’s sophisticated defense and repair mechanisms.
The Cellular Architecture of the Buffy Coat
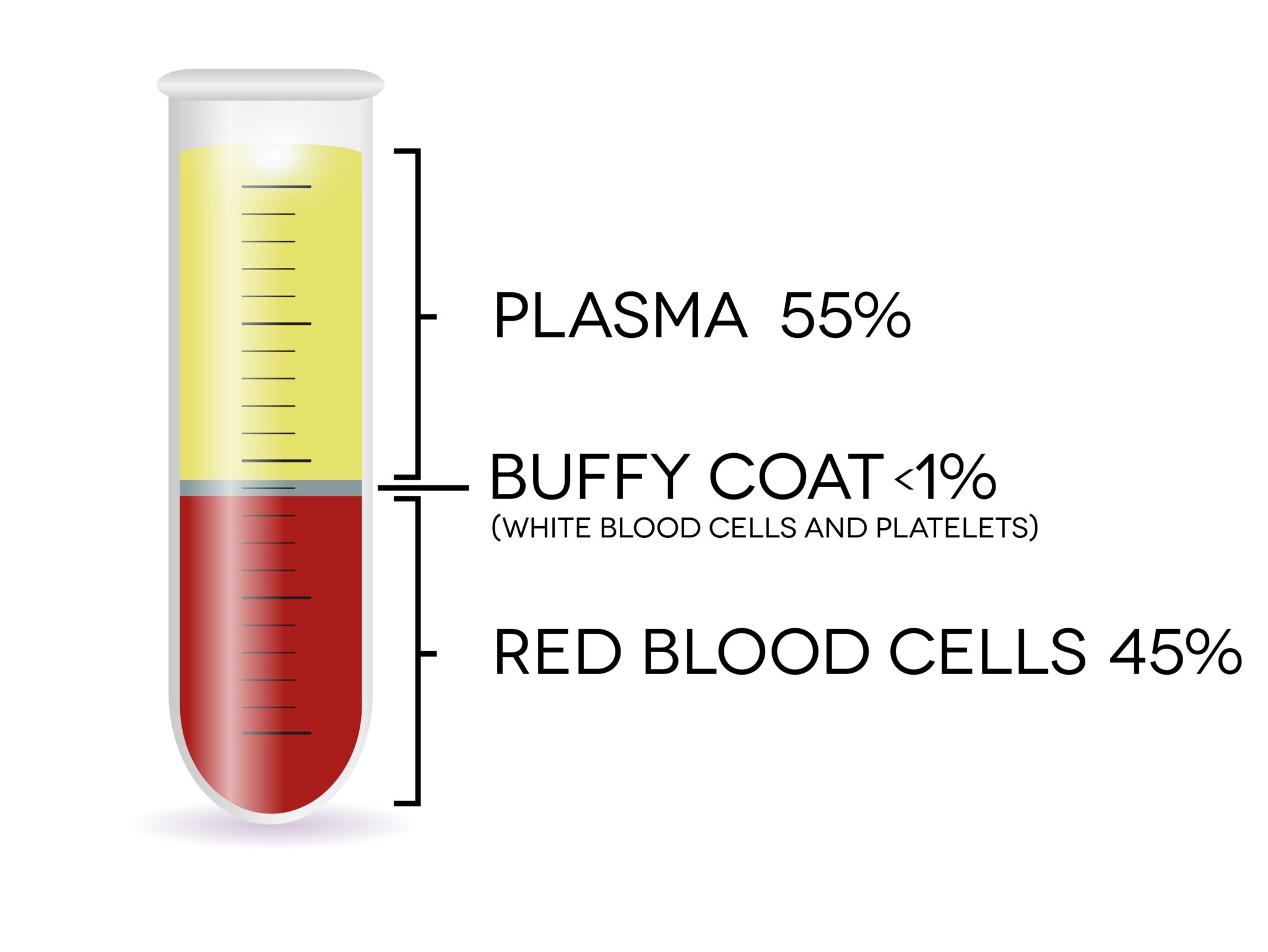
The buffy coat is primarily composed of leukocytes (white blood cells) and platelets (thrombocytes). The relative proportions of these cells can vary depending on an individual’s physiological state, such as the presence of infection or inflammation.
Leukocytes: The Body’s Immune Sentinels
White blood cells are the cornerstone of the immune system, responsible for defending the body against pathogens and foreign substances. The buffy coat provides a rich source of all major types of leukocytes:
Neutrophils
These are the most abundant type of white blood cell and are the first responders to sites of infection or injury. Neutrophils are phagocytic, meaning they engulf and digest bacteria, fungi, and cellular debris. Their characteristic segmented nucleus and granular cytoplasm are clearly visible in stained blood smears derived from the buffy coat. In cases of bacterial infection, the neutrophil count within the buffy coat can be significantly elevated, a phenomenon known as neutrophilia.
Lymphocytes
Lymphocytes are crucial for the adaptive immune response. They include T cells, B cells, and Natural Killer (NK) cells. T cells are involved in cell-mediated immunity, directly attacking infected cells or regulating the immune response. B cells produce antibodies, which are proteins that neutralize pathogens. NK cells provide rapid responses to virus-infected cells and tumor cells. The buffy coat allows for the isolation and study of these lymphocytes, which is essential for diagnosing viral infections, monitoring immune status, and in the development of immunotherapies.
Monocytes
These are the largest type of white blood cell and are precursors to macrophages. Once monocytes migrate from the bloodstream into tissues, they differentiate into macrophages, powerful phagocytic cells that engulf larger debris and pathogens. Monocytes also play a role in presenting antigens to lymphocytes, thereby initiating and shaping the adaptive immune response. Elevated monocyte counts (monocytosis) can indicate chronic infections or inflammatory conditions.
Eosinophils
Eosinophils are primarily involved in combating parasitic infections and play a role in allergic reactions. Their granules contain enzymes that can damage the cell membranes of parasites. In the buffy coat, increased eosinophil numbers (eosinophilia) are often indicative of helminthic infections or allergic diseases like asthma and eczema.
Basophils
Basophils are the least common type of white blood cell. Their granules contain histamine and heparin, which are released during allergic reactions and inflammation. Histamine is a potent vasodilator, increasing blood flow to the affected area, while heparin acts as an anticoagulant. The presence of basophils in the buffy coat, though sparse, contributes to the understanding of hypersensitivity reactions.
Platelets: The Hemostatic Powerhouses
Platelets, also known as thrombocytes, are small, anucleated cell fragments derived from megakaryocytes in the bone marrow. Their primary function is to prevent bleeding through hemostasis, the process of stopping blood loss.
Coagulation Cascade Initiation
When a blood vessel is damaged, platelets adhere to the site of injury, aggregate with one another, and form a platelet plug. This plug provides immediate hemostatic support. Furthermore, activated platelets release various factors that initiate and amplify the coagulation cascade, a complex series of enzymatic reactions that ultimately leads to the formation of fibrin. Fibrin strands then reinforce the platelet plug, forming a stable blood clot.
Growth Factors and Tissue Repair
Beyond their hemostatic role, platelets are rich sources of various growth factors, such as platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-β), and vascular endothelial growth factor (VEGF). These growth factors are critical for tissue repair and regeneration. They stimulate cell proliferation, migration, and differentiation, contributing to wound healing and the remodeling of damaged tissues. The buffy coat, therefore, represents a readily accessible source of these potent regenerative molecules.
Applications of Buffy Coat Research and Utilization
The rich cellular and molecular content of the buffy coat makes it an invaluable resource across various medical and scientific disciplines.
Diagnostic Hematology and Immunology
The buffy coat is a cornerstone in the diagnosis and monitoring of a wide array of hematological and immunological disorders.

Leukocyte Differential Count
Microscopic examination of a stained buffy coat smear allows for a differential count of white blood cells, providing crucial information about the types and numbers of each leukocyte present. Deviations from normal ranges can indicate infections, inflammatory diseases, leukemia, lymphoma, and other hematological malignancies.
Detection of Parasites and Microorganisms
In regions where parasitic infections are endemic, microscopic examination of the buffy coat can be an effective method for detecting blood-borne parasites such as Plasmodium species (causing malaria) and microfilariae (causing filariasis). Certain bacteria and fungi can also be visualized within the buffy coat.
Flow Cytometry and Immunophenotyping
For more sophisticated analyses, cells from the buffy coat can be used for flow cytometry. This technique allows for the precise quantification and characterization of different cell populations based on their surface markers. Immunophenotyping is essential for diagnosing leukemias and lymphomas, monitoring immune reconstitution after transplantation, and characterizing immune deficiencies.
Transfusion Medicine and Blood Banking
The buffy coat has significant implications in transfusion medicine, particularly in the context of blood component therapy.
Platelet-Rich Plasma (PRP) and Platelet Concentrates
While whole blood contains platelets, they are relatively fragile and have a short shelf life. For therapeutic purposes, platelets are typically concentrated from donated blood. The buffy coat, along with the plasma above it, is processed to yield platelet-rich plasma (PRP) and subsequently platelet concentrates. These are administered to patients with thrombocytopenia (low platelet counts) resulting from conditions like chemotherapy, bone marrow transplantation, or bleeding disorders, to prevent or manage hemorrhage.
Leukoreduction
In some blood products, the buffy coat, which is rich in leukocytes, is removed. This process, known as leukoreduction, is performed to minimize the risk of febrile non-hemolytic transfusion reactions, reduce the transmission of certain viruses, and prevent alloimmunization (the development of antibodies against foreign white blood cell antigens).
Regenerative Medicine and Cellular Therapies
The presence of progenitor cells and growth factors within the buffy coat positions it as a promising source for regenerative medicine applications.
Mesenchymal Stem Cells (MSCs)
While bone marrow and adipose tissue are more commonly recognized sources of mesenchymal stem cells, the buffy coat has also been identified as a site where MSCs can be isolated. These multipotent stem cells have the capacity to differentiate into various cell types, including bone, cartilage, and fat cells, making them attractive for tissue engineering and regenerative therapies for orthopedic injuries, osteoarthritis, and wound healing.
Autologous Blood Therapies
The growth factors and cytokines released by platelets in the buffy coat are harnessed in autologous blood therapies. Platelet-rich plasma (PRP) injections, derived from a patient’s own blood, are increasingly used in orthopedics, dentistry, and cosmetic procedures to accelerate healing, reduce inflammation, and promote tissue regeneration. The buffy coat serves as the source material for preparing these therapeutic preparations.
Wound Healing Accelerators
The wound-healing properties of platelets are well-established. Concentrated buffy coat preparations or PRP can be applied topically to chronic wounds, burns, and surgical sites to promote faster healing, reduce scarring, and improve the quality of tissue repair.
Challenges and Future Directions
Despite its immense value, the utilization of the buffy coat is not without its challenges, and ongoing research continues to refine and expand its applications.
Standardization of Isolation and Processing
The efficiency and efficacy of buffy coat-derived therapies can be influenced by the methods used for isolation and processing. Standardization of these protocols is crucial to ensure consistency and reproducibility of results, particularly in the context of clinical applications.
Cryopreservation and Storage
For long-term storage and future therapeutic use, effective cryopreservation techniques for buffy coat components, such as MSCs, are essential. Research is ongoing to optimize cryopreservation protocols to maintain cell viability and functional integrity.
Ex Vivo Expansion and Differentiation
To generate sufficient quantities of cells for certain therapeutic applications, ex vivo expansion and directed differentiation protocols for buffy coat-derived stem cells are being developed. This allows for the generation of specific cell lineages required for tissue repair or to reconstitute immune function.

Exploration of Novel Biomolecules
The buffy coat contains a complex milieu of biomolecules beyond growth factors. Ongoing research aims to identify and characterize novel cytokines, chemokines, and extracellular vesicles within the buffy coat that may have therapeutic potential for a range of diseases.
In conclusion, the buffy coat, often overlooked as a mere cellular layer, is a dynamic and invaluable component of blood. Its dense concentration of leukocytes and platelets underpins critical immunological defense, hemostatic functions, and regenerative processes. From its foundational role in diagnostics to its burgeoning potential in regenerative medicine, the buffy coat continues to be a focal point of scientific inquiry and clinical innovation, promising further advancements in the understanding and treatment of human health.
