Understanding the Anatomy and Physiology of the Cecum
The cecum, a small pouch located at the beginning of the large intestine, plays a crucial yet often overlooked role in the digestive process. It is the initial segment of the colon, where the small intestine, specifically the ileum, empties its contents. Attached to the cecum is the appendix, a small, finger-like appendage whose exact function remains a subject of ongoing research, though it is often associated with immune system activity and the gut microbiome.
The cecum’s primary function is to act as a reservoir for digested material, allowing for further absorption of water and electrolytes before the waste progresses through the colon. Its muscular walls churn the contents, aiding in the mixing and breakdown of food particles. The ileocecal valve, situated at the junction of the ileum and the cecum, is a critical sphincter that controls the flow of chyme from the small intestine into the large intestine, preventing backflow and maintaining the directional movement of digested material.
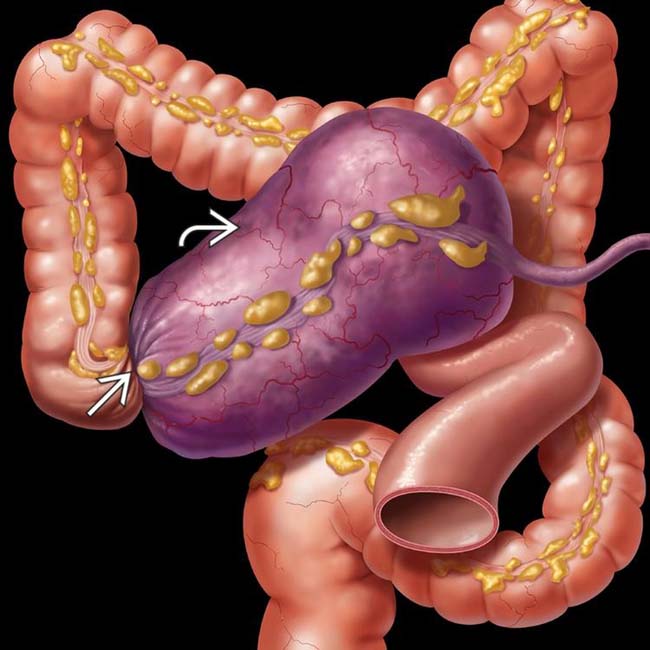
The anatomy of the cecum is characterized by its location in the right lower quadrant of the abdomen. It is typically anchored by the peritoneum, a serous membrane lining the abdominal cavity, but its mobility can vary significantly among individuals. This inherent mobility, coupled with its anatomical connections, sets the stage for potential complications such as volvulus. The surrounding structures, including loops of the small intestine, the ascending colon, and other abdominal organs, contribute to the complex environment within which the cecum resides. Understanding this intricate anatomical relationship is paramount to comprehending the mechanics and consequences of cecal volvulus.
The physiological processes occurring within the cecum are integral to overall digestive health. The slow transit time within the cecum allows for efficient reabsorption of water, which solidifies the fecal matter. The microbial population within the cecum, part of the gut microbiome, also plays a vital role in further breaking down undigested material and synthesizing certain vitamins. Disruptions to this delicate balance, whether due to anatomical abnormalities or external factors, can have significant implications for digestive function and overall well-being.
Defining Cecal Volvulus: A Twist of Fate
Cecal volvulus is a surgical emergency characterized by the twisting of the cecum around its mesentery, the fold of tissue that attaches the intestine to the abdominal wall. This torsion obstructs the passage of intestinal contents and compromises the blood supply to the affected segment of the bowel, potentially leading to ischemia and necrosis. It represents a specific type of intestinal obstruction, distinct from other colonic volvuluses like sigmoid volvulus, due to the unique anatomical position and mobility of the cecum.
The mechanism of cecal volvulus typically involves a mobile cecum, often due to incomplete fixation to the posterior abdominal wall during embryonic development. This lack of fixation allows the cecum to possess a long mesentery, creating a pedicle around which twisting can occur. Various factors can precipitate the twist, including increased colonic distension due to a high-fiber diet, rapid transit of stool, or even changes in intra-abdominal pressure. The twisting action can be clockwise or counterclockwise, leading to occlusion of the lumen and venous and arterial compromise.
The consequences of this torsion are severe. The luminal obstruction prevents the normal passage of stool and gas, leading to abdominal distension and pain. More critically, the compromised blood supply can rapidly lead to strangulation of the bowel. If left untreated, this can result in bowel infarction (tissue death), perforation, and subsequent peritonitis, a life-threatening infection of the abdominal cavity. The speed at which these complications develop underscores the urgent nature of cecal volvulus as a medical condition.
Etiology and Risk Factors: Why Does it Happen?
The development of cecal volvulus is multifactorial, with a combination of anatomical predisposition and triggering events contributing to its occurrence. While the exact cause can vary, several key factors are consistently identified in the medical literature.
Anatomical Predisposition
The most significant predisposing factor is an abnormally mobile cecum. During fetal development, the cecum normally becomes fixed to the retroperitoneum (the space behind the peritoneum) as the colon ascends. However, in some individuals, this fixation is incomplete, leaving the cecum with a long, mobile mesentery. This elongated mesentery acts like a hinge, allowing the cecum to twist upon itself. Conditions contributing to this malfixation include:
- Incomplete Retroperitoneal Fixation: This is the most common anatomical anomaly associated with cecal volvulus. The ascending colon and cecum may remain largely intraperitoneal, allowing for greater range of motion.
- Long and Mobille Cecal Mesentery: The mesentery supporting the cecum can be unusually long and narrow, creating a potential axis for rotation.
- Absence of Fixation Bands: In some cases, the normal peritoneal folds that anchor the cecum to the abdominal wall may be absent or underdeveloped.
Triggering Factors
While anatomical predisposition creates the potential for volvulus, certain factors can precipitate the twisting event:
- Sudden Increase in Cecal Volume: Rapid distension of the cecum can increase its mobility and the likelihood of torsion. This can be caused by:
- High-Fiber Diet: A sudden increase in dietary fiber can lead to a large volume of undigested material in the colon, particularly in the cecum.
- Constipation: Prolonged constipation can lead to accumulation of stool in the cecum, increasing its bulk.
- Ileus or Gastroparesis: Conditions that slow down the movement of contents through the digestive tract can lead to distension.
- Changes in Intra-abdominal Pressure: Significant and sudden increases in abdominal pressure can displace the cecum and initiate torsion. Examples include:
- Pregnancy: The growing uterus can exert pressure.
- Obesity: Increased intra-abdominal fat can alter organ positioning.
- Heavy Lifting or Straining: These activities can cause acute pressure changes.
- Postoperative Factors: Following abdominal surgery, particularly procedures involving the colon or small bowel, adhesions can form. In some rare instances, these adhesions might restrict normal bowel movement and contribute to abnormal positioning, potentially leading to volvulus.
- Congenital Abnormalities: While less common, other congenital anomalies of the intestinal tract can predispose individuals to cecal volvulus.

It is important to note that in many cases, a clear precipitating event may not be identifiable, with the volvulus occurring spontaneously in individuals with the underlying anatomical vulnerability.
Clinical Manifestations and Diagnosis: Recognizing the Symptoms
The presentation of cecal volvulus can be varied, ranging from mild, intermittent discomfort to severe, acute abdominal pain. Prompt recognition of these symptoms is crucial for timely diagnosis and intervention.
Symptoms and Signs
The hallmark symptom of cecal volvulus is abdominal pain, typically located in the right lower quadrant or epigastric region. The pain is often sudden in onset and can be colicky, meaning it comes in waves. Other common symptoms include:
- Nausea and Vomiting: These are frequently present due to the obstruction of the intestinal tract. The vomitus may initially be bilious (containing bile) and can become feculent (smelling of stool) in cases of complete obstruction and prolonged duration.
- Abdominal Distension: As gas and fluid accumulate proximal to the obstruction, the abdomen becomes noticeably distended, particularly in the right lower quadrant.
- Constipation: While some patients may have had a normal bowel movement prior to the onset of symptoms, constipation is a common feature as the volvulus progresses and the obstruction becomes complete.
- Lack of Flatus: The inability to pass gas is a significant indicator of intestinal obstruction.
- Tenderness: Palpation of the abdomen often reveals tenderness, particularly in the right iliac fossa. This tenderness can become more generalized if peritonitis develops.
- Rebound Tenderness and Guarding: These signs suggest peritoneal irritation, indicating a more severe complication such as bowel ischemia or perforation.
- Fever: Fever may develop, especially if there is bowel ischemia, necrosis, or perforation.
Diagnostic Modalities
The diagnosis of cecal volvulus relies on a combination of clinical suspicion, physical examination findings, and advanced imaging techniques.
- Abdominal Radiography (X-ray): Initial plain abdominal X-rays can be suggestive but are often not definitive. Findings may include:
- Dilated Cecum: A characteristic “coffee bean” or inverse “U” shaped loop of dilated bowel in the right upper or mid-abdomen, representing the twisted cecum.
- Air-Fluid Levels: Distended loops of small and large bowel with air-fluid levels can be seen.
- Lack of Distal Colonic Gas: Absence of gas in the distal colon and rectum is a strong indicator of obstruction.
- Computed Tomography (CT) Scan: CT scan is the most valuable imaging modality for diagnosing cecal volvulus. It provides detailed cross-sectional images of the abdomen and pelvis and can:
- Confirm Cecal Volvulus: Clearly visualize the twisted cecum and mesentery, often demonstrating a “whirlpool sign” or “bird’s beak” appearance of the mesentery at the point of torsion.
- Assess for Complications: Identify signs of bowel ischemia, necrosis, perforation, and the presence of free air or fluid.
- Differentiate from Other Causes of Obstruction: Help distinguish cecal volvulus from other conditions that cause similar symptoms.
- Barium Enema: While less commonly used now due to the advent of CT, a barium enema can sometimes reveal a characteristic “bird’s beak” deformity at the site of obstruction. However, it carries a risk of perforation if bowel ischemia is present.
- Ultrasound: Ultrasound may be used as an initial assessment tool, but its diagnostic yield for cecal volvulus is generally lower compared to CT scans.
A thorough history and physical examination, combined with appropriate imaging, are essential for making an accurate and timely diagnosis, paving the way for prompt surgical management.
Management and Surgical Intervention: Addressing the Twist
The management of cecal volvulus is primarily surgical, as conservative measures are rarely successful and carries a high risk of serious complications. The goal of surgery is to detorse the twisted bowel, assess its viability, and restore normal intestinal continuity.
Surgical Approaches
The surgical approach depends on the patient’s condition, the presence of complications, and the surgeon’s preference.
- Laparoscopic Detorsion and Cecopexy: For uncomplicated cases with viable bowel, a minimally invasive laparoscopic approach may be attempted. This involves detorsing the cecum and then securing it to the abdominal wall (cecopexy) to prevent recurrence. However, the success rate of cecopexy alone in preventing recurrence can be variable, and it may not be suitable for all patients.
- Laparotomy with Detorsion and Resection: If the bowel is ischemic or necrotic, or if the patient’s condition is unstable, an open laparotomy (abdominal incision) is typically performed. The surgeon will then detorse the cecum. If the bowel is viable, a cecopexy or cecostomy (creating an opening into the cecum) might be considered. However, if there is evidence of irreversible ischemia or perforation, a segmental resection of the cecum and ascending colon is necessary.
- Right Hemicolectomy: This is the most common definitive surgical procedure for cecal volvulus, especially when there is significant bowel compromise. It involves the surgical removal of the cecum, appendix, and a portion of the ascending colon. The remaining small intestine (ileum) is then reconnected to the remaining colon (transverse colon) in an end-to-end or end-to-side anastomosis to restore intestinal continuity.

Postoperative Care and Recurrence
Postoperative care focuses on managing pain, preventing infection, and ensuring adequate hydration and nutrition. Patients are typically monitored closely for signs of complications such as anastomotic leak, ileus, or wound infection.
Recurrence of cecal volvulus, while not as common as with some other types of volvulus, is a possibility, particularly if the underlying anatomical predisposition is not fully addressed. Factors influencing recurrence include the extent of fixation performed, the underlying cause of the mobile cecum, and individual patient anatomy. In cases where a cecopexy or cecostomy is performed and the bowel is viable, close follow-up is essential to monitor for any signs of recurrent torsion.
The decision regarding the specific surgical intervention is made on a case-by-case basis, balancing the risks and benefits of each approach to achieve the best possible outcome for the patient. Early diagnosis and prompt surgical intervention are critical to improving prognosis and reducing morbidity and mortality associated with cecal volvulus.
