Bursitis in the foot, while perhaps not as widely discussed as ailments affecting larger joints, can be a significant source of pain and mobility issues for many individuals. Understanding this condition, its causes, symptoms, and management strategies is crucial for maintaining an active and pain-free lifestyle. This article delves into the specifics of foot bursitis, exploring the various types, contributing factors, and effective approaches to diagnosis and treatment.
Understanding Bursae and Bursitis
At the heart of bursitis lies the bursa itself. Bursae are small, fluid-filled sacs that act as cushions between bones, tendons, muscles, and ligaments. Their primary function is to reduce friction and allow for smooth, gliding movements of these structures over one another. Think of them as tiny shock absorbers strategically placed throughout the body, particularly in areas that experience repetitive motion or pressure.
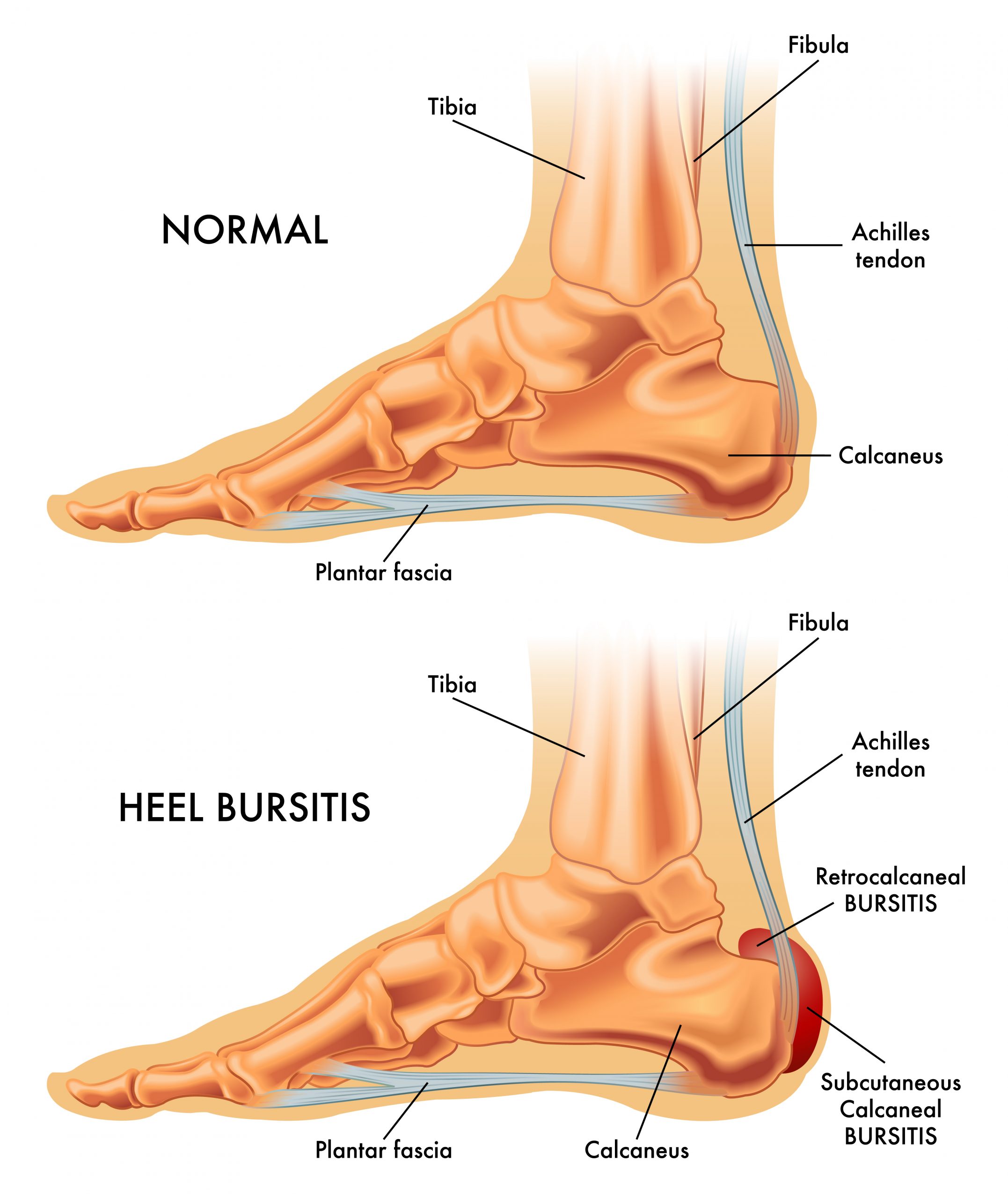
Anatomy of Foot Bursae
The foot, with its complex structure and constant demands, contains several bursae. While less numerous than in larger joints like the knee or elbow, their presence is vital for foot function. Some of the key bursae found in the foot include:
- Retrocalcaneal Bursa: Located between the heel bone (calcaneus) and the Achilles tendon. Inflammation here is common, especially with activities that involve a lot of ankle movement.
- Subcalcaneal Bursa: Situated beneath the heel bone, this bursa can become irritated by pressure from footwear or activities that involve prolonged standing or impact.
- Adventitious Bursae: These are bursae that can develop in unusual locations, often in response to chronic friction or pressure from ill-fitting shoes or bony prominences.
- Bursae around the Malleoli: Bursae can also be found around the bony prominences on either side of the ankle joint (the malleoli).
The Inflammatory Process
Bursitis, in its simplest definition, is the inflammation of one or more of these bursae. This inflammation typically occurs when a bursa is overused, overstretched, or subjected to excessive pressure or direct trauma. The body’s response to this irritation is to increase the production of synovial fluid within the bursa, leading to swelling. This swollen bursa then exerts pressure on surrounding nerves and tissues, resulting in pain, tenderness, and restricted movement.
Common Causes and Risk Factors of Foot Bursitis
The development of bursitis in the foot is rarely a spontaneous event. It is usually the result of a combination of factors, with repetitive stress and improper biomechanics being prominent culprits. Identifying these underlying causes is the first step towards effective prevention and treatment.
Overuse and Repetitive Stress
Activities that involve prolonged walking, running, jumping, or standing can place significant repetitive stress on the bursae in the foot. Athletes, dancers, postal workers, and individuals whose jobs require them to be on their feet for extended periods are at a higher risk. This constant friction and pressure can gradually irritate and inflame the bursae.
Improper Footwear
The role of footwear in foot health cannot be overstated. Ill-fitting shoes are a major contributor to bursitis. Shoes that are too tight, too narrow, or that rub in specific areas can create excessive friction and pressure points. High heels, for instance, can alter foot mechanics and place undue stress on the heel and forefoot bursae. Conversely, shoes that offer inadequate support can lead to poor biomechanics, indirectly contributing to bursal irritation.
Biomechanical Issues
The way a person walks, runs, or stands (their biomechanics) plays a critical role in how forces are distributed throughout their feet. Conditions such as:
- Flat Feet (Pes Planus): When the arch of the foot collapses, it can alter the normal weight-bearing distribution, leading to increased pressure on certain areas and potential bursal irritation.
- High Arches (Pes Cavus): Conversely, very high arches can also lead to abnormal pressure points and reduced shock absorption.
- Gait Abnormalities: Any unusual pattern of walking or running can put abnormal stress on specific joints and bursae.
Direct Trauma and Injury
While less common than overuse, a direct blow or injury to the foot can also cause bursitis. A fall, a stubbed toe, or a direct impact can bruise the bursa and trigger an inflammatory response.
Other Contributing Factors
Several other factors can increase an individual’s susceptibility to foot bursitis:
- Age: As we age, tendons and ligaments can become less flexible, and the protective fatty pads in the foot may diminish, making bursae more vulnerable to irritation.
- Arthritis: Conditions like osteoarthritis or rheumatoid arthritis can cause inflammation in and around the joints, which can extend to nearby bursae.
- Gout: This form of inflammatory arthritis can lead to crystal deposits in the joints and surrounding tissues, potentially irritating bursae.
- Obesity: Excess body weight places additional stress on the feet, increasing the likelihood of bursal inflammation.
- Bone Spurs (Osteophytes): The development of bony outgrowths can rub against adjacent bursae, causing chronic irritation.
Recognizing the Symptoms of Foot Bursitis
The hallmark symptom of bursitis is pain, but the presentation can vary depending on the location and severity of the inflammation. Early recognition of these symptoms is key to prompt treatment and preventing the condition from becoming chronic.
Pain and Tenderness
The primary complaint is usually localized pain in the area of the affected bursa. This pain can range from a dull ache to a sharp, stabbing sensation. It often worsens with activity, pressure, or direct touch. For instance, retrocalcaneal bursitis will typically cause pain at the back of the heel, especially when walking or wearing shoes. Subcalcaneal bursitis pain is felt on the bottom of the heel.
Swelling and Redness
Inflammation of the bursa leads to an accumulation of fluid, causing visible swelling. The affected area may appear puffy or enlarged. In some cases, particularly if the inflammation is severe or has become infected, the skin over the bursa may become red and warm to the touch.
Stiffness and Limited Range of Motion
The pain and swelling associated with bursitis can make it difficult to move the foot and ankle freely. This can result in stiffness, particularly in the morning or after periods of rest. The limited range of motion can impact gait and make simple activities like walking or climbing stairs challenging.
Aching Sensation
Some individuals describe a persistent aching sensation in the affected area, which may be more noticeable when at rest or during cooler weather.
Formation of a Lump (Less Common)
In chronic cases, or with certain types of bursitis, a small, firm lump may form over the inflamed bursa. This is essentially the thickened wall of the bursa or a collection of fluid.
Diagnosis and Treatment Approaches
Diagnosing foot bursitis involves a comprehensive evaluation by a healthcare professional, followed by a tailored treatment plan aimed at reducing inflammation, alleviating pain, and addressing the underlying causes.
Medical Evaluation
The diagnostic process typically begins with a thorough medical history and physical examination. The healthcare provider will inquire about your symptoms, activities, footwear, and any previous injuries. During the physical exam, they will:
- Palpate the affected area: To pinpoint the location of tenderness and swelling.
- Assess range of motion: To evaluate any limitations in ankle and foot movement.
- Observe gait: To identify any biomechanical abnormalities.
Imaging Studies
In some instances, imaging studies may be used to confirm the diagnosis, rule out other conditions, or assess the extent of the inflammation:
- X-rays: While X-rays cannot directly visualize bursae, they can help identify underlying bone spurs, arthritis, or other structural abnormalities that may be contributing to the bursitis.
- Ultrasound: This is often a valuable tool for visualizing soft tissues, including bursae. Ultrasound can detect inflammation, fluid accumulation, and thickening of the bursa.
- MRI (Magnetic Resonance Imaging): MRI provides detailed cross-sectional images of both bone and soft tissues and is useful for assessing the extent of bursal inflammation, as well as identifying any associated tendon or ligament injuries.
Fluid Aspiration
If there is significant swelling and concern about infection, a healthcare provider may perform a fluid aspiration. This involves using a needle to withdraw fluid from the bursa. The fluid can then be sent to a laboratory for analysis to check for signs of infection (bacterial) or crystal deposits (gout).
Treatment Strategies
The goal of treatment is to reduce inflammation, relieve pain, and prevent recurrence. Treatment approaches can be broadly categorized into conservative and, in rarer cases, surgical interventions.
Conservative Management
The majority of foot bursitis cases respond well to conservative treatments:
- Rest: Avoiding activities that aggravate the pain is paramount. This may involve modifying exercise routines or taking time off from strenuous activities.
- Ice Application: Applying ice packs to the affected area for 15-20 minutes several times a day can help reduce swelling and pain.
- Medications:
- Over-the-counter pain relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can help reduce pain and inflammation.
- Prescription NSAIDs: In more severe cases, a doctor may prescribe stronger NSAIDs.
- Corticosteroid Injections: Injections of corticosteroids directly into the bursa can provide rapid and potent relief from inflammation and pain. However, these are typically used judiciously due to potential side effects with repeated use.
- Padding and Support:
- Orthotics: Custom or over-the-counter orthotic inserts can help correct biomechanical issues and redistribute pressure more evenly across the foot.
- Heel Cups and Pads: These can provide cushioning and support to the heel area, relieving pressure on inflamed bursae.
- Physical Therapy: A physical therapist can guide you through a tailored exercise program to:
- Improve flexibility: Stretching exercises for the calf muscles and Achilles tendon can relieve tension.
- Strengthen foot and ankle muscles: To improve support and stability.
- Address biomechanical issues: Through specific exercises and gait retraining.
- Footwear Modification: Wearing well-fitting shoes with ample cushioning and support is crucial. Avoiding high heels and shoes that cause friction is recommended.
Surgical Intervention
Surgery is rarely necessary for foot bursitis and is typically reserved for cases that are severe, chronic, unresponsive to conservative treatment, or complicated by other issues like persistent infection or significant structural deformities. Surgical options may include:
- Bursae Removal (Excision): The inflamed bursa can be surgically removed, especially if it is causing significant pain or is prone to recurrent inflammation.
- Debridement: If bone spurs are contributing to the bursitis, they may be surgically removed.
Prevention and Long-Term Foot Health
Preventing the recurrence of foot bursitis involves a proactive approach to foot care and lifestyle choices. By understanding the contributing factors, individuals can take steps to protect their feet and maintain optimal mobility.
Choose Appropriate Footwear
This is arguably the most critical preventative measure. Opt for shoes that:
- Fit well: Ensure there is adequate room in the toe box and no rubbing.
- Provide good cushioning: Especially for high-impact activities.
- Offer adequate support: Particularly for the arch of the foot.
- Are suited to the activity: Running shoes for running, walking shoes for walking, etc.
- Avoid high heels and pointed-toe shoes for prolonged wear.
Maintain a Healthy Weight
Reducing excess body weight significantly lessens the load and stress on the feet, thereby decreasing the risk of bursal inflammation.
Gradual Increase in Activity Levels
When embarking on new or more intense physical activities, gradually increase the duration and intensity to allow your body, including your bursae, to adapt. Avoid sudden increases in mileage for runners or prolonged standing without breaks.
Incorporate Stretching and Strengthening Exercises
Regularly stretching the calf muscles, Achilles tendon, and foot muscles can improve flexibility and reduce tension. Strengthening exercises for the intrinsic muscles of the foot and the ankle can enhance stability and support.
Listen to Your Body
Pay attention to early warning signs of discomfort or pain in your feet. Do not push through pain, as this can exacerbate inflammation and lead to more significant problems. Seek professional advice if you experience persistent foot pain.
Regular Foot Care
Keep your feet clean and dry. Inspect your feet regularly for any signs of irritation, blisters, or changes in skin. Promptly address any issues with ingrown toenails or calluses, as these can contribute to abnormal pressure.
By understanding the nuances of bursitis in the foot, from its underlying causes to effective management and prevention strategies, individuals can take a proactive role in safeguarding their foot health and enjoying a life free from debilitating pain.
