Understanding the Basics of Blood Borne Pathogens
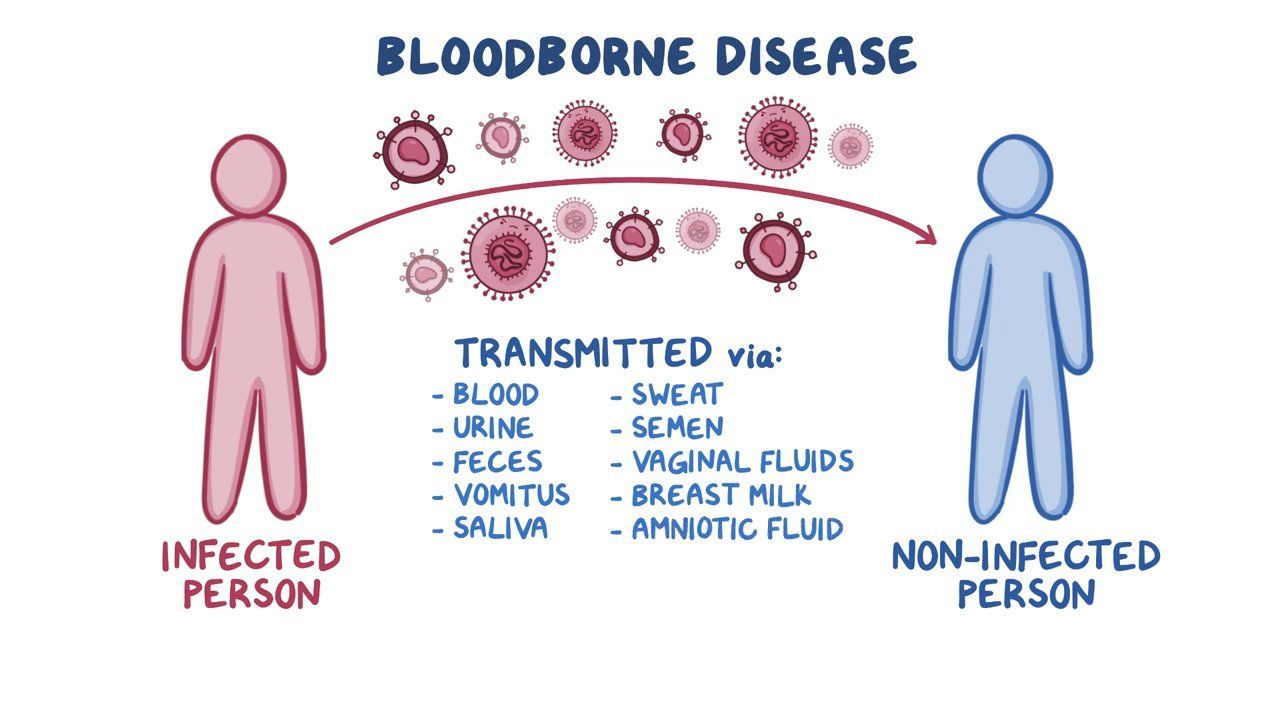
Bloodborne pathogens are microorganisms, such as viruses or bacteria, that can be present in the blood of infected individuals and can cause disease in humans. These pathogens are transmitted through direct contact with infected blood or other potentially infectious body fluids (OPIM). Understanding the routes of transmission and implementing appropriate preventive measures are crucial in healthcare settings and beyond to minimize the risk of infection.
Types of Bloodborne Pathogens
The most common and significant bloodborne pathogens of concern in healthcare and occupational settings include:
- Hepatitis B Virus (HBV): This virus targets the liver and can cause acute or chronic hepatitis. Chronic HBV infection can lead to serious complications like cirrhosis and liver cancer. HBV is highly prevalent and can survive for extended periods outside the body on surfaces.
- Hepatitis C Virus (HCV): Similar to HBV, HCV also attacks the liver, but it is more likely to cause chronic infection. Chronic HCV infection is a leading cause of liver transplantation and is associated with an increased risk of liver cancer.
- Human Immunodeficiency Virus (HIV): HIV is a retrovirus that attacks the body’s immune system, specifically targeting CD4 cells (T cells). Over time, if left untreated, HIV can lead to Acquired Immunodeficiency Syndrome (AIDS), a condition that severely weakens the immune system, making individuals susceptible to opportunistic infections and cancers.
While these three are the most prominent, other bloodborne pathogens can also pose a risk, including:
- Hepatitis D Virus (HDV): This virus requires the presence of HBV to replicate. Co-infection with HBV and HDV can lead to more severe liver disease.
- Syphilis: A bacterial infection that can be transmitted through direct contact with a syphilis sore, which may be present in the blood.
- Malaria: A parasitic disease transmitted through the bite of infected mosquitoes, but can also be transmitted through blood transfusions or needle-sharing.
Routes of Transmission
The primary routes of transmission for bloodborne pathogens involve direct contact with infected blood or OPIM. This can occur through:
- Percutaneous Injury: This is the most common route of occupational transmission and involves injuries caused by sharp objects contaminated with infected blood. Examples include needlestick injuries, cuts from broken glass, or punctures from surgical instruments.
- Mucous Membrane Exposure: Contact of infected blood or OPIM with mucous membranes, such as the eyes, nose, or mouth, can lead to transmission.
- Non-Intact Skin Exposure: Exposure of infected blood or OPIM to skin that is not intact, meaning it has cuts, abrasions, dermatitis, or other open sores, can also result in infection.
It is important to note that casual contact, such as hugging, kissing, or sharing utensils, does not typically transmit these pathogens. Transmission requires direct exposure to infected blood or certain body fluids.
Other Potentially Infectious Body Fluids (OPIM)
Beyond blood, other body fluids are considered potentially infectious if they contain blood or if there is a significant risk of transmission. These include:
- Cerebrospinal fluid (CSF): Fluid surrounding the brain and spinal cord.
- Pericardial fluid: Fluid surrounding the heart.
- Peritoneal fluid: Fluid within the abdominal cavity.
- Pleural fluid: Fluid surrounding the lungs.
- Amniotic fluid: Fluid surrounding a fetus during pregnancy.
- Seminal fluid: Including semen.
- Vaginal secretions:
- Synovial fluid: Fluid found in joints.
- Vomit: If it contains visible blood.
- Feces: If it contains visible blood.
- Urine: If it contains visible blood.
- Saliva: While generally considered low risk, saliva can transmit certain infections if blood is present.
Prevention and Control Measures
Preventing the transmission of bloodborne pathogens relies on a multi-faceted approach that includes engineering controls, administrative controls, and the use of personal protective equipment (PPE).
Engineering Controls
Engineering controls are designed to remove or reduce hazards at the source. In the context of bloodborne pathogens, these include:
- Needleless Systems: Devices that do not require needles for drawing fluids, administering medications, or other procedures, thereby reducing the risk of needlestick injuries.
- Sharps Disposal Containers: Puncture-resistant containers strategically placed in areas where sharps are used for safe disposal of contaminated needles, scalpels, and other sharp instruments.
- Biosafety Cabinets: Enclosed, ventilated workspaces that provide protection to laboratory personnel and prevent the release of infectious aerosols into the workplace.
Administrative Controls
Administrative controls involve establishing policies, procedures, and training programs to minimize exposure risk. These include:
- Exposure Control Plan: A comprehensive written plan that outlines procedures for identifying, evaluating, and controlling exposure to bloodborne pathogens. This plan should be regularly reviewed and updated.
- Training and Education: Providing regular training to employees who may be exposed to bloodborne pathogens. This training should cover routes of transmission, prevention strategies, safe work practices, and the proper use of PPE.
- Post-Exposure Evaluation and Follow-up: Establishing protocols for immediate medical evaluation and follow-up for individuals who have been exposed to bloodborne pathogens. This includes testing, prophylaxis, and counseling.
- Work Practice Controls: Implementing specific work practices designed to reduce the likelihood of exposure. Examples include prohibiting eating, drinking, smoking, or applying cosmetics in areas where bloodborne pathogens may be present.
Personal Protective Equipment (PPE)
PPE acts as a barrier between the individual and the potential hazard. Appropriate PPE for preventing bloodborne pathogen exposure includes:
- Gloves: Made of latex, nitrile, or neoprene, gloves are essential for preventing skin contact with blood and OPIM. They should be changed frequently and immediately if torn or contaminated.
- Gowns and Aprons: Fluid-resistant gowns or aprons should be worn when there is a potential for splashing or spraying of blood or OPIM.
- Masks and Eye Protection: Masks, eye protection (e.g., goggles or face shields), and nasal protection should be worn when there is a risk of splashes, sprays, or aerosols of blood or OPIM.
- Footwear Protection: Closed-toe shoes are generally recommended, and shoe covers may be necessary in certain high-risk situations.
The Importance of Universal Precautions
A cornerstone of bloodborne pathogen prevention is the adherence to Universal Precautions. This approach, developed by the Centers for Disease Control and Prevention (CDC), treats all human blood and certain body fluids as if they are known to be infectious for bloodborne pathogens. This means that appropriate precautions should be taken with every patient and in every situation where there is a potential for exposure, regardless of the patient’s known infection status.
The principles of Universal Precautions include:
- Using appropriate PPE.
- Practicing safe handling of sharps.
- Ensuring proper hand hygiene.
- Implementing safe work practices.
- Following established decontamination procedures.
Post-Exposure Prophylaxis (PEP)
For individuals who have experienced an occupational exposure to bloodborne pathogens, particularly HIV, Hepatitis B, and Hepatitis C, Post-Exposure Prophylaxis (PEP) may be recommended. PEP involves the administration of antiviral medications as soon as possible after exposure to reduce the risk of infection. The effectiveness of PEP is highly dependent on the timing of administration, with treatment initiated within hours of exposure yielding the best results. Medical professionals play a critical role in assessing the risk of exposure and prescribing the appropriate PEP regimen.

Conclusion
Bloodborne pathogens pose a significant health risk, particularly in occupational settings where exposure is possible. A thorough understanding of the types of pathogens, their routes of transmission, and the implementation of robust prevention and control measures, including engineering controls, administrative controls, appropriate PPE, and the diligent application of Universal Precautions, are paramount in safeguarding health and preventing infections. Continuous education, adherence to protocols, and prompt response to exposures are vital components of a comprehensive bloodborne pathogen safety program.
