In the intricate ecosystem of modern healthcare, the efficiency and effectiveness of patient care are paramount. While the terms “hospital unit” might conjure images of intensive care wards or surgical theaters, there exists a crucial, yet often less understood, operational component: the observation unit. This specialized area plays a vital role in bridging the gap between emergency department (ED) visits and definitive inpatient admission or discharge. It’s a space designed for patients who require more detailed assessment and monitoring than typically provided in the ED, but whose conditions do not necessarily warrant immediate, full inpatient bed assignment. Understanding the function and significance of an observation unit is key to appreciating the nuanced pathways of patient management within a hospital.

The Spectrum of Patient Care: Bridging the Gap
Observation units have emerged as a strategic response to the growing demands on hospital resources and the need for more refined patient triage. They address a specific patient population that falls into a grey area, often presenting with symptoms that are concerning but not immediately life-threatening or requiring the full diagnostic and treatment intensity of an inpatient stay.
The Intermediate Patient Pathway
Historically, patients presenting with symptoms like chest pain, abdominal discomfort, or mild respiratory issues, but who stabilized after initial ED interventions, faced a dilemma. They might be discharged home with follow-up instructions, potentially missing a subtle but progressing issue, or admitted to an inpatient bed, consuming resources that might be better allocated to sicker patients. The observation unit offers a middle ground, a dedicated space for a defined period of further evaluation. This period typically ranges from a few hours to 24-48 hours, during which a patient can undergo targeted diagnostic tests, receive specific treatments, and be closely monitored by a specialized team.
Defined Admission Criteria and Length of Stay
Unlike general inpatient units where patients are admitted indefinitely until medically cleared, observation units operate with distinct admission criteria and a predetermined, albeit flexible, length of stay. Patients are generally admitted with the intention of resolving their acute diagnostic question or stabilizing their condition within a defined timeframe. This contrasts with inpatient admissions, which are typically for more complex illnesses requiring extended management, or direct discharges from the ED, for patients whose conditions are deemed stable enough for home care with appropriate follow-up. The observation unit serves as a proactive measure to prevent unnecessary admissions and expedite the diagnostic process for select patients.
Function and Purpose: Optimized Assessment and Management
The primary function of an observation unit is to provide a focused environment for the comprehensive assessment and management of patients who are not acutely ill enough for full inpatient admission but require more than what the emergency department can offer. This involves a multidisciplinary approach and a structured workflow.
Diagnostic Stabilization and Workup
A core purpose of the observation unit is to facilitate a more thorough diagnostic workup than might be feasible in the bustling ED environment. Patients may undergo serial electrocardiograms (ECGs), cardiac enzyme monitoring, abdominal imaging, blood tests, or respiratory function assessments. The unit is equipped to administer specific treatments, such as intravenous fluids, pain medication, or bronchodilators, allowing clinicians to observe the patient’s response and further refine the diagnosis. This focused approach helps in making informed decisions about subsequent care, whether that be a safe discharge or a definitive inpatient admission.
Enhanced Monitoring and Timely Intervention
The observation unit provides a higher level of patient monitoring than a standard ED waiting area. Patients are typically in a dedicated bed or recliner, within visual or audible range of nursing staff. This allows for more frequent vital sign checks, symptom assessment, and prompt recognition of any deterioration or improvement. The proximity of diagnostic services and the availability of a specialized medical team enable rapid intervention if a patient’s condition changes unexpectedly. This proactive approach can prevent complications, reduce the need for more intensive care, and ultimately improve patient outcomes.
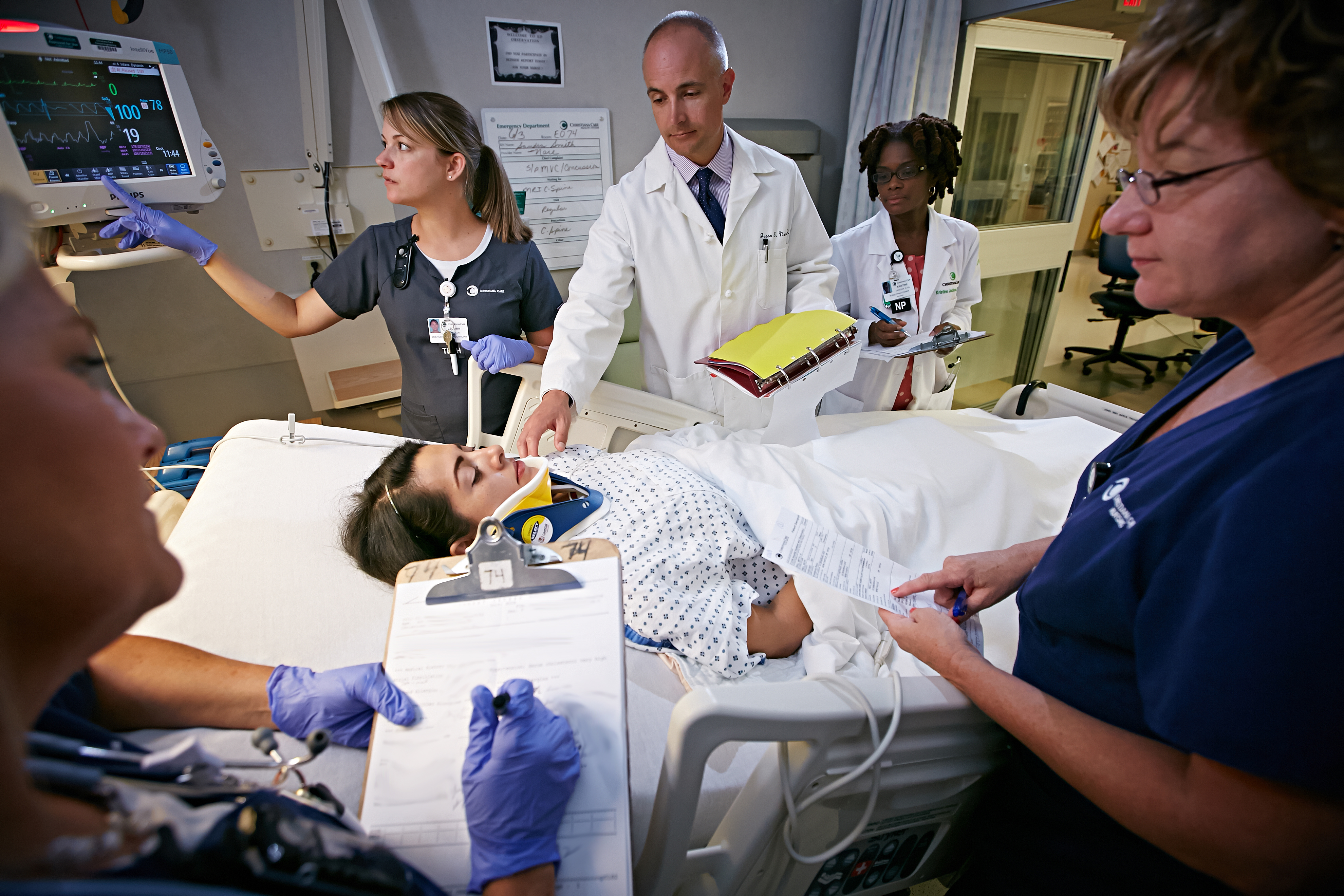
Operational Structure and Staffing Models
The success of an observation unit hinges on its specialized operational structure and the expertise of its dedicated staff. These units are designed for efficiency and rapid patient turnover, with a focus on clear communication and collaborative care.
Dedicated Medical and Nursing Teams
Observation units are typically staffed by a dedicated team of physicians, often hospitalists or ED physicians with a specific interest in observation medicine, and nurses who are trained in acute care assessment and monitoring. This specialized team develops expertise in managing the common conditions that present to observation, leading to more efficient and effective care. Pharmacists, respiratory therapists, and other ancillary services often have designated roles or easy access to the unit, further enhancing the collaborative nature of patient management.
Workflow and Throughput Efficiency
A key operational goal for observation units is to optimize patient flow and throughput. This often involves standardized protocols for patient admission, assessment, treatment, and discharge. The unit is designed to facilitate rapid turnaround of diagnostic tests and timely consultations with specialists. The goal is to resolve the diagnostic question or stabilize the patient as efficiently as possible, allowing for either a safe discharge with clear follow-up instructions or an expedited transfer to an appropriate inpatient service if admission becomes necessary. This focus on efficiency helps reduce ED boarding times and improves overall hospital capacity.
Benefits and Impact on Healthcare Delivery
The implementation of observation units has yielded significant benefits for patients, healthcare providers, and the hospital system as a whole. They represent an evolving model of care designed to meet the complex demands of modern healthcare.
Improved Patient Outcomes and Satisfaction
By providing a dedicated space for targeted assessment and monitoring, observation units can lead to more accurate diagnoses, timely interventions, and ultimately, better patient outcomes. Patients who might have been discharged prematurely from the ED with undiagnosed issues can receive the necessary evaluation. Similarly, those who might have occupied inpatient beds unnecessarily can be managed more efficiently, freeing up resources for critically ill patients. This focused care and reduced wait times can also contribute to higher patient satisfaction.
Enhanced Resource Utilization and Cost-Effectiveness
Observation units play a crucial role in optimizing hospital resources. By diverting patients who do not require full inpatient admission away from traditional inpatient beds, hospitals can increase bed availability for those who truly need it. The more efficient diagnostic and treatment pathways within the observation unit can also lead to shorter overall hospital stays and reduced healthcare costs. This model allows for a more judicious use of expensive inpatient resources, making healthcare delivery more sustainable and cost-effective.
Reduced Emergency Department Congestion
The ED is often the gateway to hospital admission, and overcrowding is a persistent challenge. Observation units act as a valuable buffer, absorbing patients who require extended evaluation but not necessarily a full inpatient admission. By managing these patients in a dedicated setting, observation units can significantly reduce the boarding of patients in the ED, improving the ED’s ability to care for critically ill patients and enhancing the overall efficiency of the hospital’s patient flow.
