The term “MS Hug” in the context of multiple sclerosis (MS) is a colloquial and descriptive phrase used by individuals living with the condition to articulate a particular symptom they experience. It’s crucial to understand that this is not a medical diagnosis in itself, but rather a patient-reported phenomenon that describes a distinct physical sensation.
Understanding the Sensation of an “MS Hug”
At its core, an MS Hug refers to a constricting, tight, or squeezing sensation that can occur anywhere on the body. While it can manifest in various locations, it is most commonly felt around the torso, resembling the feeling of being tightly bound or embraced. This sensation can range in intensity from a mild discomfort to a severe and debilitating pain. The experience is subjective, meaning it is felt and interpreted by the individual experiencing it, and can vary significantly from one person to another, and even in the same person from day to day.
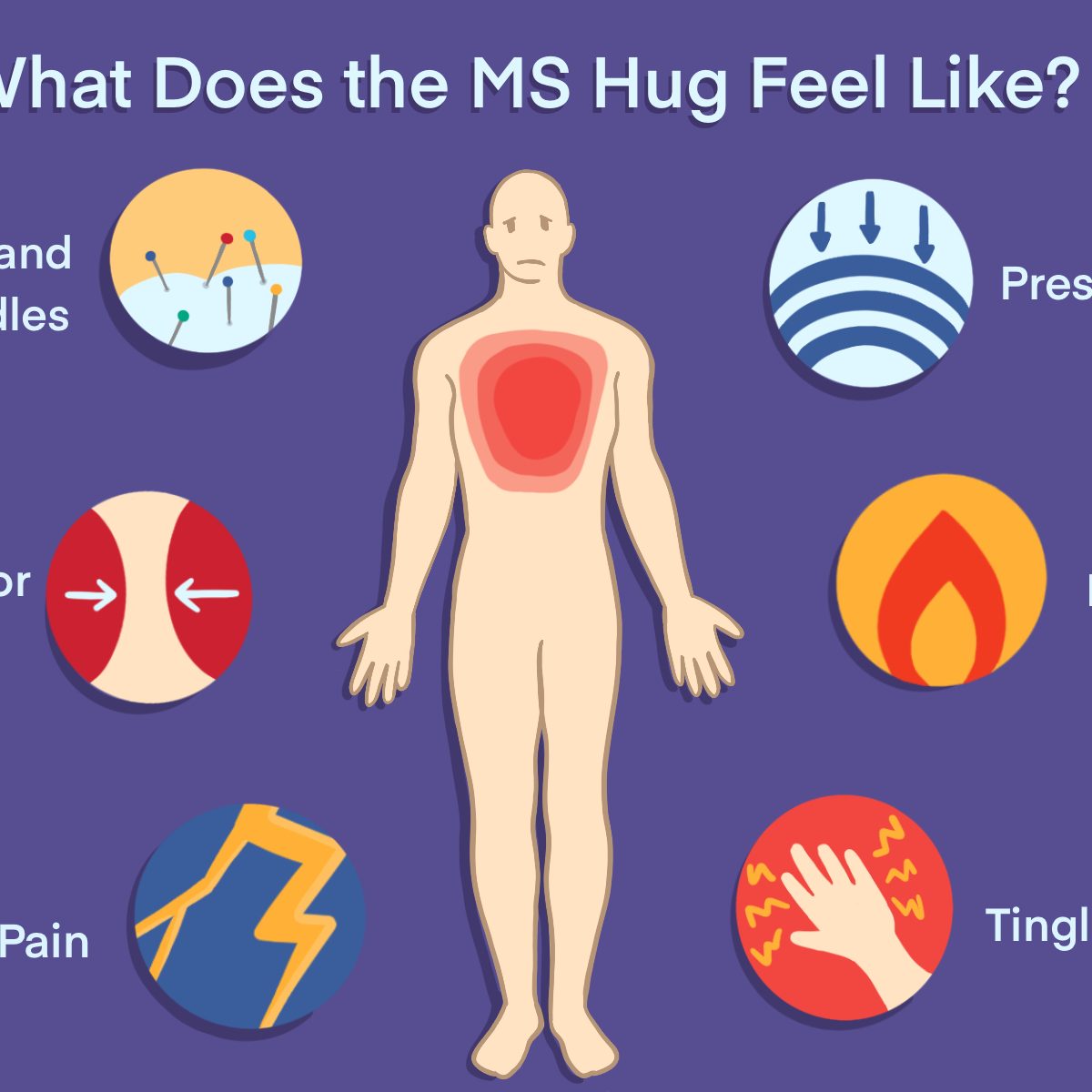
The underlying cause of this sensation is believed to be related to the damage to the myelin sheath, the protective covering around nerve fibers, which is a hallmark of MS. When this myelin is damaged, it disrupts the transmission of nerve signals, leading to a wide array of neurological symptoms. In the case of the MS Hug, the disrupted signals are interpreted by the brain as pressure, tightness, or pain. The nerves responsible for sensing touch, pressure, and pain are affected, leading to these unusual sensory disturbances.
The Neurological Basis of Sensory Symptoms in MS
Multiple sclerosis is an autoimmune disease where the body’s immune system mistakenly attacks the central nervous system, specifically the myelin sheath. This sheath acts as an insulator for nerve fibers, allowing for the rapid and efficient transmission of electrical signals. When myelin is damaged (a process called demyelination), these signals can be slowed down, distorted, or even completely blocked.
The sensory nervous system is particularly susceptible to these disruptions. Nerves responsible for transmitting information about touch, temperature, vibration, proprioception (sense of body position), and pain can all be affected. The MS Hug is thought to be a result of aberrant signaling within these sensory pathways. It can be likened to a faulty electrical wire where the insulation is compromised, leading to static or interference in the signal.
The specific areas of the central nervous system that are affected by MS lesions can dictate the type and location of sensory symptoms. Lesions in the spinal cord, brainstem, or even higher brain centers can all contribute to altered sensory perception. The complex network of nerves in the torso, for example, can be affected in a way that the brain interprets this neural misfiring as a physical constriction.
Differentiating the “MS Hug” from Other Sensations
It’s important for individuals experiencing such sensations to communicate them clearly to their healthcare providers. While “MS Hug” is a widely understood term within the MS community, medical professionals may use more precise terminology to describe the symptom and its underlying neurological cause. These sensations can be categorized as:
- Paresthesias: These are abnormal sensations such as tingling, prickling, or “pins and needles.” While not the primary characteristic of an MS Hug, they can sometimes co-occur or be a milder form of the sensory disturbance.
- Dysesthesias: These are unpleasant, abnormal sensations, which can include burning, aching, or sharp, shooting pains. An MS Hug can sometimes manifest as a form of dysesthesia, particularly when it involves significant discomfort or pain.
- Allodynia: This is pain caused by a stimulus that does not normally provoke pain, such as light touch. While less common as the sole description of an MS Hug, the heightened sensitivity associated with the sensation can make even light pressure feel uncomfortable.
- Hyperesthesia: This refers to increased sensitivity to touch. An MS Hug can involve an extreme form of hyperesthesia, where even normal bodily movements or contact with clothing can exacerbate the feeling of constriction.
The key differentiating factor of an MS Hug is the overwhelming sensation of tightness or squeezing, often without an obvious external trigger. It’s a feeling that originates internally due to the neurological changes brought about by MS.
Triggers and Variability of the MS Hug
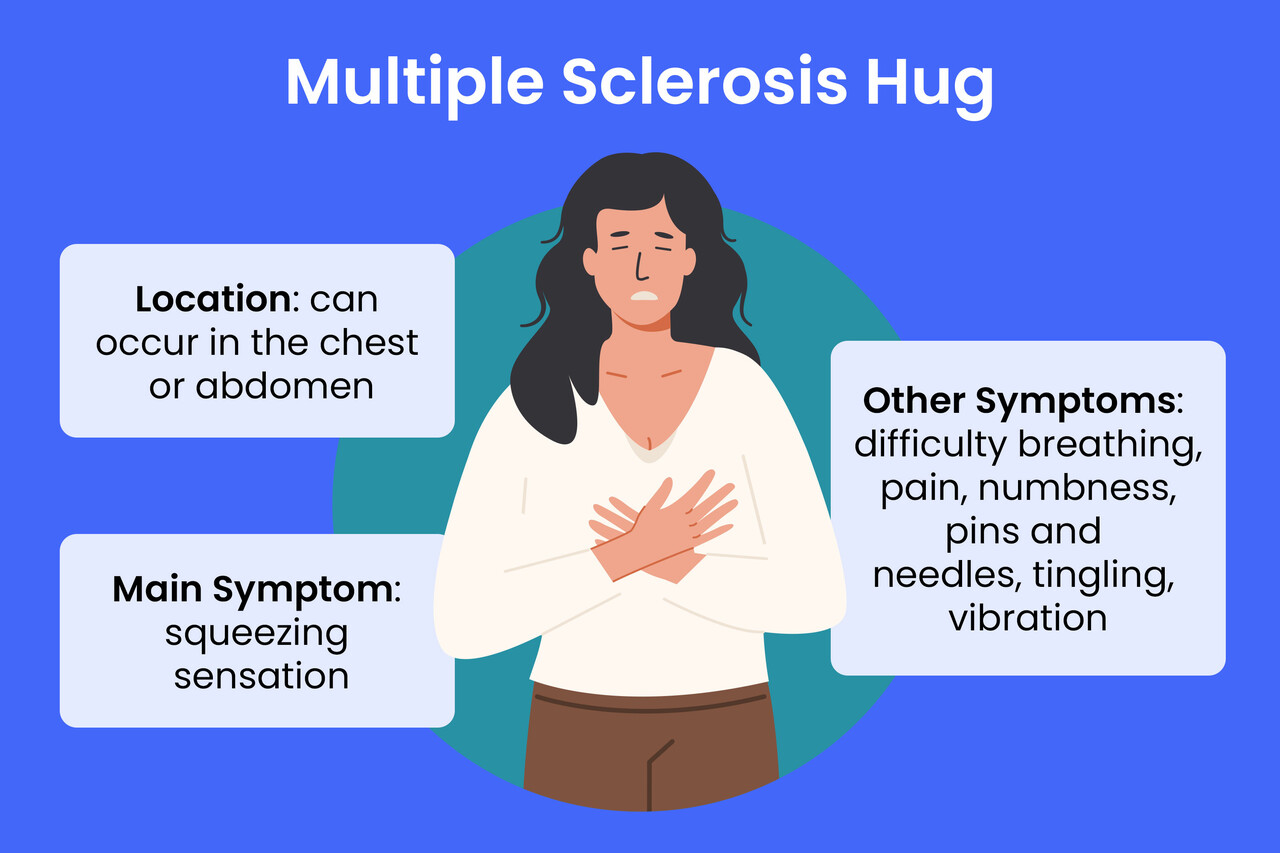
The MS Hug is not a constant symptom for most individuals. Its occurrence and intensity can fluctuate, and certain factors may act as triggers or exacerbate the sensation. Understanding these triggers can be helpful for individuals in managing their symptoms and improving their quality of life.
Common Triggers and Exacerbating Factors
- Fatigue: One of the most pervasive symptoms of MS is fatigue, and this can often worsen sensory disturbances, including the MS Hug. When fatigued, the body’s ability to manage and process sensory information may be compromised, leading to a more pronounced experience of the hug.
- Stress and Anxiety: Emotional and psychological stress can significantly impact the nervous system. For individuals with MS, stress can heighten nerve sensitivity and contribute to the onset or intensification of various symptoms, including the MS Hug. The perception of pain and discomfort is often amplified under stress.
- Heat: Temperature sensitivity is common in MS. Exposure to heat, whether through a warm environment, hot baths, or physical exertion, can worsen neurological symptoms. This can include an exacerbation of the MS Hug, as heat can temporarily impair nerve conduction in demyelinated areas.
- Overexertion: Physical exertion, especially beyond an individual’s current capacity, can lead to increased body temperature and fatigue, both of which can trigger or worsen the MS Hug.
- Bowel or Bladder Dysfunction: Issues with bowel or bladder function, which are common in MS, can sometimes contribute to or be associated with sensations in the pelvic and abdominal regions, potentially including or mimicking aspects of an MS Hug.
- Certain Movements or Positions: For some, specific body movements, prolonged sitting or standing, or even changes in posture can seem to trigger the sensation. This is likely due to the way these actions might affect nerve compression or irritation in already sensitive areas.
The variability of the MS Hug is a significant aspect of its experience. It can appear suddenly, last for minutes, hours, or even days, and then disappear just as abruptly. This unpredictability can be frustrating and challenging to manage.
Management and Treatment Strategies
While there is no single cure for the MS Hug, a variety of strategies can be employed to manage its symptoms and improve an individual’s comfort and well-being. These often involve a multi-faceted approach, combining lifestyle adjustments, therapeutic interventions, and sometimes pharmacological treatments.
Lifestyle Modifications and Self-Care
- Pacing Activities: Learning to pace one’s energy levels and avoid overexertion is crucial. This involves breaking down tasks, taking regular rest breaks, and listening to the body’s signals.
- Stress Management Techniques: Practicing mindfulness, meditation, deep breathing exercises, yoga, or engaging in enjoyable hobbies can help reduce stress and anxiety, thereby mitigating their impact on symptoms.
- Temperature Regulation: Avoiding extreme heat and keeping the body cool can be beneficial. This might involve staying in air-conditioned environments, using cooling wraps, or taking cool showers.
- Gentle Exercise: While overexertion should be avoided, regular, gentle exercise, as recommended by a healthcare professional, can help maintain overall health and potentially improve nerve function and resilience.
- Hydration and Nutrition: Maintaining adequate hydration and a balanced diet supports overall bodily functions, which can indirectly contribute to better symptom management.
Therapeutic Interventions
- Physical Therapy: A physical therapist can assess the specific nature of the MS Hug and recommend exercises or stretches to alleviate muscle tension or improve posture that might be contributing to the sensation. They can also provide strategies for pain management.
- Occupational Therapy: An occupational therapist can help individuals adapt their daily activities and environment to minimize triggers and manage symptoms. This might involve recommending adaptive equipment or strategies for dressing and personal care.
- Complementary Therapies: Some individuals find relief through complementary therapies such as acupuncture, massage therapy (gentle and applied appropriately), or biofeedback. It is essential to discuss these options with a healthcare provider to ensure they are safe and suitable.

Pharmacological Treatments
When lifestyle modifications and therapies are insufficient, healthcare providers may consider pharmacological interventions to manage the pain and discomfort associated with the MS Hug. The choice of medication will depend on the severity and nature of the sensation, as well as other individual factors.
- Pain Relievers: Over-the-counter pain relievers like acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs) may offer some relief for mild discomfort, though they are often not sufficient for more severe sensations.
- Anticonvulsant Medications: Medications typically used to treat epilepsy, such as gabapentin or pregabalin, are often effective in managing neuropathic pain and sensory disturbances like the MS Hug. They work by calming overactive nerve signals.
- Antidepressants: Certain types of antidepressants, particularly tricyclic antidepressants (TCAs) and serotonin-norepinephrine reuptake inhibitors (SNRIs), can also be effective in treating neuropathic pain, even in individuals who are not experiencing depression.
- Muscle Relaxants: In cases where muscle spasticity contributes to or exacerbates the feeling of tightness, muscle relaxants might be prescribed.
- Disease-Modifying Therapies (DMTs): While not directly treating the MS Hug, DMTs are crucial in managing the underlying disease progression of MS. By reducing inflammation and preventing new lesions, DMTs can potentially decrease the likelihood or severity of various MS symptoms, including sensory disturbances.
It is imperative for individuals experiencing the MS Hug to have an open and honest dialogue with their neurologist or MS care team. They can provide accurate diagnosis, monitor symptom progression, and tailor a management plan that best suits the individual’s needs, ultimately aiming to improve their quality of life and functional independence.
