The term “anoscope” might sound technical, but it refers to a straightforward and vital medical instrument. In its essence, an anoscope is a specialized tool used for examining the anal canal. This examination is a crucial part of diagnosing and managing a variety of conditions affecting this sensitive area. Understanding what an anoscope is, how it functions, and its applications provides valuable insight into common medical procedures and the importance of diagnostic tools in healthcare.
The Anatomy of an Anoscope
At its core, an anoscope is a short, rigid or flexible tube, typically made of plastic or metal. Its design is deliberately simple yet effective, prioritizing clear visualization of the anal canal. The most common type is the rigid anoscope, which is a hollow cylinder with a tapered or rounded end. This tapered end allows for gentle insertion into the anal opening. Many rigid anoscope designs also feature a light source or are designed to be used in conjunction with an external light source, such as an otoscope or a headlamp, to illuminate the canal.

Components and Variations
- The Tube: This is the main body of the anoscope. Its length is typically short, ranging from a few centimeters to about 10-15 centimeters, sufficient to visualize the anal canal and the lower rectum. The diameter also varies, designed to be comfortably inserted while providing a wide enough view.
- The Obturator (for rigid scopes): Many rigid anoscopes come with a removable obturator, a smooth, rounded tip that fits inside the tube. The obturator facilitates smooth and atraumatic insertion of the anoscope into the anal canal. Once the scope is in place, the obturator is withdrawn, leaving the hollow tube open for examination.
- Light Source: Some advanced anoscopes incorporate a built-in light source at the tip, powered by batteries or connected to an external power source. This eliminates the need for separate lighting, enhancing convenience and often improving the quality of illumination.
- Magnification: While not standard on all models, some anoscopes may include a magnifying lens to provide a closer, more detailed view of the tissue.
- Flexible Anoscopes: In contrast to rigid anoscopes, flexible versions exist. These are made of a more pliable material and may have a slightly different shape, often used when a more comfortable examination is desired or when navigating more tortuous anatomy. However, rigid anoscopes are generally preferred for their superior rigidity, which allows for better control and more direct visualization of the anal canal.
- Disposable vs. Reusable: Anoscopes come in both disposable (single-use) plastic models and reusable metal or autoclavable plastic models. Disposable scopes are increasingly popular due to their convenience, reduced risk of cross-contamination, and elimination of the need for sterilization. Reusable scopes require thorough cleaning and sterilization between uses.
The straightforward design of the anoscope belies its significant clinical utility. It is an indispensable tool for physicians, particularly gastroenterologists and colorectal surgeons, but also general practitioners, in performing essential diagnostic procedures.
The Procedure: How an Anoscope Is Used
The use of an anoscope is typically part of a proctoscopy or an anoscopy examination. The procedure is relatively brief and generally well-tolerated, though some discomfort may be experienced by the patient. It is usually performed in a clinical setting, such as a doctor’s office or examination room.
Preparing for the Examination
Before the anoscopy, the healthcare provider will explain the procedure to the patient and obtain their consent. The patient is typically asked to lie on their side in a fetal position (knees drawn up to the chest) or to stand and bend forward over the examination table. This positioning relaxes the anal sphincter muscles and provides optimal access to the anal canal. In some cases, a mild laxative or enema may be recommended beforehand to ensure the anal canal is empty, though this is not always necessary for a basic anoscopy.
The Examination Process
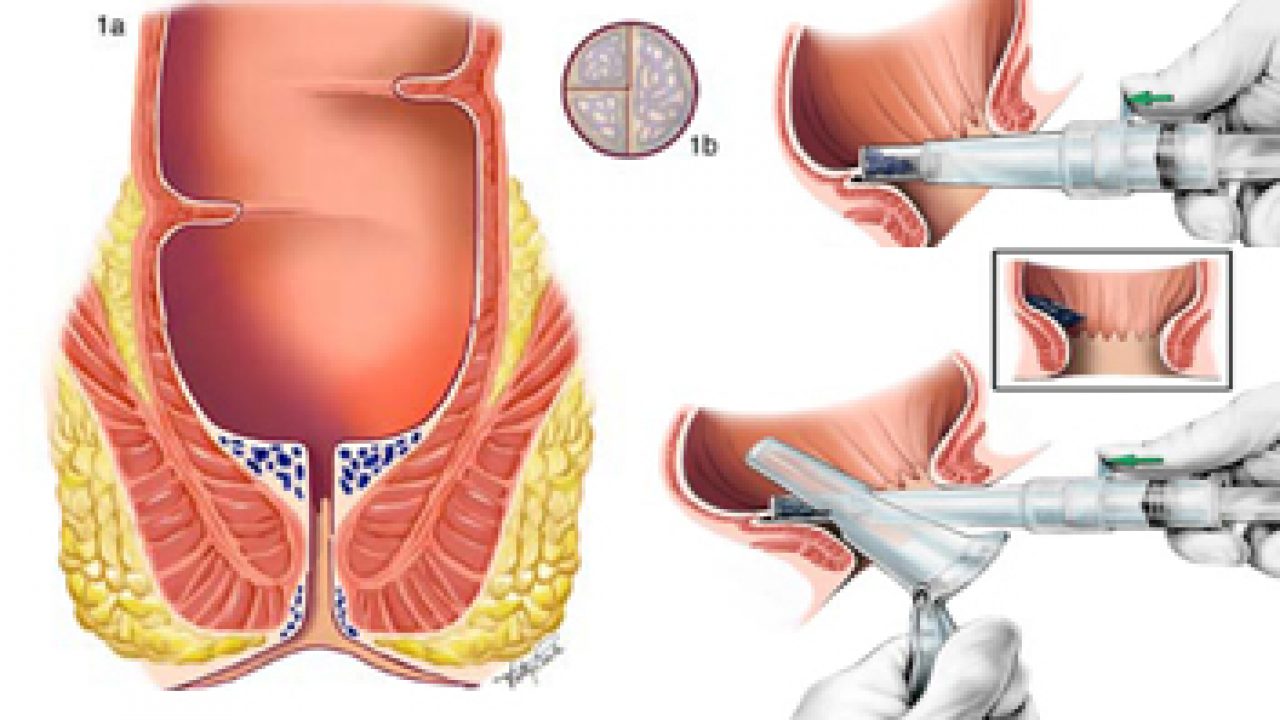
- Lubrication: The tip of the anoscope, especially if it’s a rigid model with an obturator, is generously lubricated with a water-based lubricant. This is crucial to ensure smooth and comfortable insertion.
- Insertion: The healthcare provider gently inserts the lubricated anoscope, often with the obturator in place for rigid scopes, into the anal opening. As the tapered end enters, the patient may feel a sensation of pressure or the urge to defecate. The provider will then withdraw the obturator, leaving the hollow tube in place.
- Visualization: With the anoscope in position, the healthcare provider looks through the opening of the anoscope to visualize the anal canal. If the anoscope doesn’t have a built-in light, an external light source will be used to illuminate the canal. The provider will systematically examine the lining of the anal canal, looking for any abnormalities.
- Inspection and Palpation (if applicable): The provider inspects the entire circumference of the anal canal, noting the presence of hemorrhoids, fissures, fistulas, polyps, tumors, or any signs of inflammation or infection. In some cases, the provider may gently rotate the anoscope or ask the patient to bear down slightly to get a better view of specific areas.
- Biopsy or Further Intervention: If any suspicious lesions are identified, the provider may use specialized instruments passed through the anoscope to take a biopsy for further laboratory analysis. In some instances, minor procedures like the removal of small polyps might be performed during the anoscopy.
- Withdrawal: Once the examination is complete, the anoscope is slowly and carefully withdrawn, again with lubrication to ensure comfort.
The entire procedure usually takes only a few minutes. While some patients may experience mild discomfort or cramping during the examination, it is generally not considered painful.
Clinical Applications: Why Is Anoscopy Performed?
The anoscope is a fundamental diagnostic tool used to identify and assess a wide range of conditions affecting the anal canal and lower rectum. Its primary function is to provide a direct, magnified view of the mucosal lining, which is often not adequately visualized during a routine external examination or digital rectal examination alone.
Common Reasons for Anoscopy
- Hemorrhoids: Anoscopy is the gold standard for diagnosing internal hemorrhoids, which are swollen veins in the anal canal. The anoscope allows for clear visualization of their size, location, and whether they are thrombosed (clotted) or prolapsed (extruding from the anus).
- Anal Fissures: These are small tears in the lining of the anal canal, often caused by passing hard stools. Anoscopy can help identify acute or chronic fissures, assess their depth, and look for associated conditions like skin tags.
- Anal Fistulas: A fistula is an abnormal tunnel that forms between the anal canal and the skin surface. Anoscopy can help identify the internal opening of the fistula within the anal canal, which is crucial for planning surgical treatment.
- Polyps and Tumors: While polyps in the anal canal are less common than those in the colon, anoscopy can detect them. More importantly, it plays a role in the staging and assessment of anal cancers and other rectal tumors that may involve the anal canal.
- Infections and Abscesses: The anoscope can help identify signs of infection, such as proctitis (inflammation of the rectal lining), or locate the internal opening of an anal abscess.
- Pain and Bleeding: Patients experiencing anal pain, itching, or bleeding often undergo an anoscopy to determine the cause. These symptoms can be indicative of various conditions, and the anoscope provides essential visual confirmation.
- Screening: In certain high-risk individuals, an anoscopy might be part of a screening protocol, although it is more commonly used for diagnostic purposes when symptoms are present.
The information gained from an anoscopy is vital for accurate diagnosis, appropriate treatment planning, and monitoring the effectiveness of therapies for anal and rectal conditions. It is a simple, low-risk procedure that offers significant diagnostic value.
The Significance of Direct Visualization
The power of the anoscope lies in its ability to provide direct, magnified visualization of the anal canal. While a digital rectal examination (DRE) can assess the tone of the sphincter muscles, detect some larger masses, and assess the prostate in men, it is limited in its ability to see the internal lining. The anal canal is approximately 3-4 cm long, and the junction between the skin of the external anus and the mucosal lining of the rectum (the dentate line) is a critical area for many pathologies. The anoscope allows clinicians to meticulously inspect this entire zone.

Beyond the Digital Touch
- Detail and Precision: Unlike the indirect assessment of a DRE, an anoscope offers a close-up view of mucosal texture, color, and any subtle lesions. This allows for earlier detection of subtle changes that might be missed otherwise.
- Targeted Biopsies: When abnormalities are found, the anoscope facilitates the precise collection of tissue samples (biopsies) from the specific area of concern. This is crucial for histopathological diagnosis, distinguishing between benign and malignant conditions.
- Assessment of Depth and Extent: The anoscope helps in determining the size, location, and potential depth of lesions, providing critical information for treatment decisions, especially for conditions like fistulas and tumors.
- Procedural Guidance: For minor interventions performed through the anoscope, such as banding of internal hemorrhoids or snare polypectomy of small anal polyps, the direct visualization is paramount for safety and efficacy.
In conclusion, the anoscope, despite its simple appearance, is an indispensable medical instrument. It empowers healthcare professionals with the ability to see and diagnose conditions within the anal canal that are otherwise hidden, playing a critical role in patient care and management. Its straightforward design, ease of use, and diagnostic power make it a cornerstone of examinations in gastroenterology and colorectal medicine.
