Airborne infection is a critical topic in public health and epidemiology, referring to the transmission of infectious diseases through the air. This mode of transmission is particularly concerning due to its rapid spread and the potential for widespread outbreaks. Understanding the mechanisms, implications, and preventative measures associated with airborne infections is paramount for both individual well-being and global health security.
Understanding the Fundamentals of Airborne Transmission
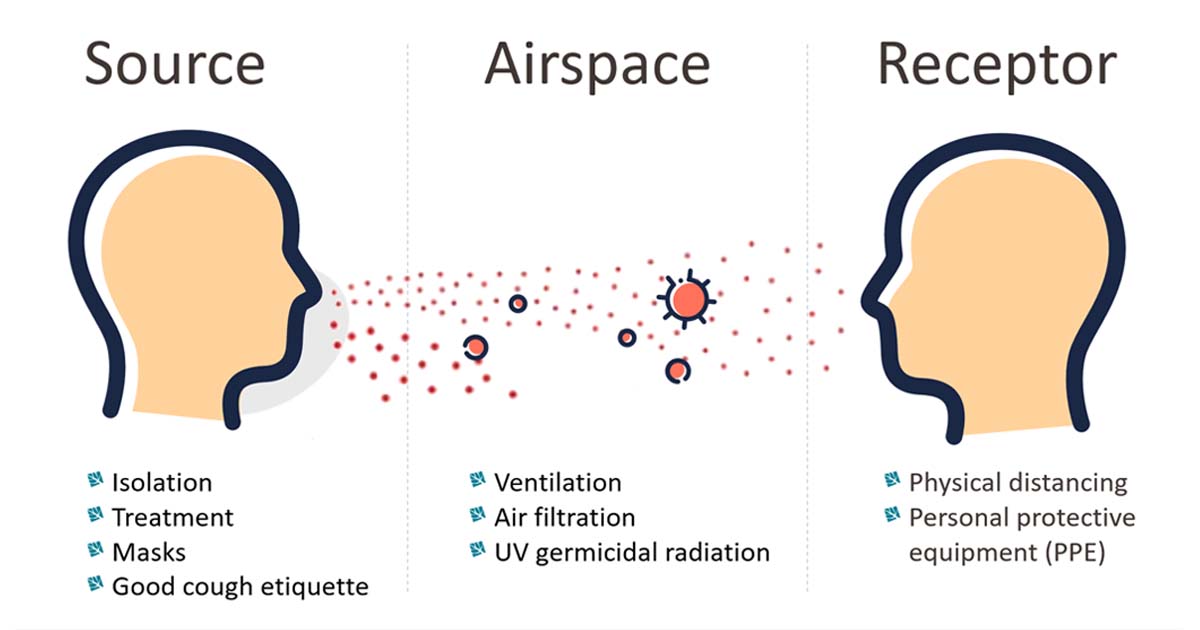
Airborne transmission occurs when infectious agents, such as bacteria, viruses, or fungi, are released into the air and subsequently inhaled by susceptible individuals. This process is fundamentally different from droplet transmission, which involves larger respiratory particles that typically travel shorter distances and settle more quickly. Airborne particles are significantly smaller, allowing them to remain suspended in the air for extended periods and travel further.
The Role of Respiratory Tracts
The primary source of airborne infectious agents is the respiratory tract of an infected individual. When a person coughs, sneezes, talks, or even breathes, they can expel tiny particles containing pathogens. The size and composition of these particles determine their fate in the environment and their potential for transmission.
Expiratory Events and Particle Sizes
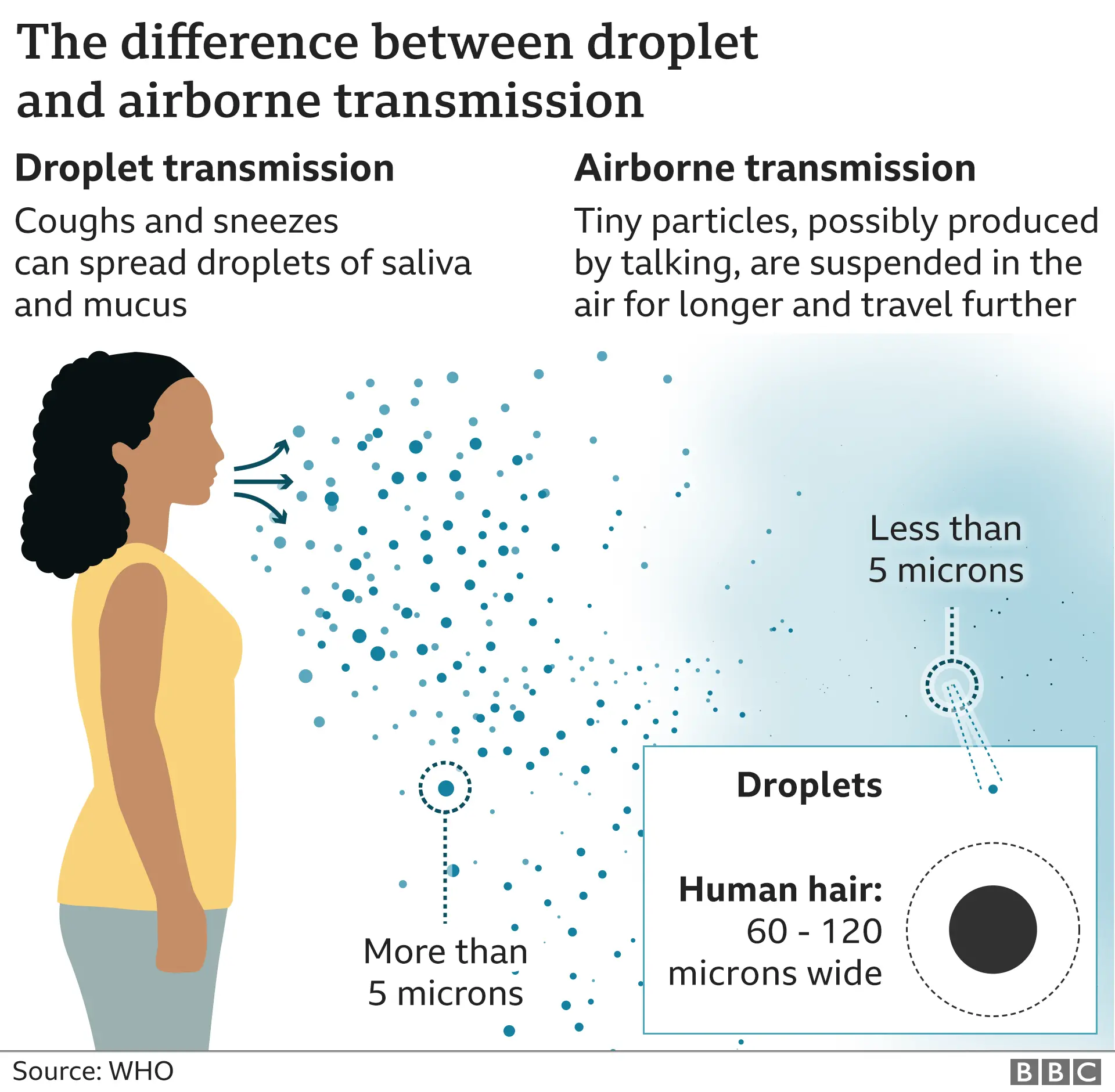
Coughing and sneezing are potent mechanisms for expelling a wide range of respiratory droplets. However, the most critical for airborne transmission are the aerosols – particles less than 5 micrometers in diameter. These aerosols are so small that they can evade the body’s initial defenses and remain suspended in the air, even in still environments. Larger droplets, typically greater than 5 micrometers, tend to fall to the ground within a few feet, posing more of a direct contact or short-range droplet transmission risk.
Viability and Persistence of Pathogens
The ability of a pathogen to survive and maintain its infectivity in the airborne state is a crucial factor in the success of airborne transmission. Factors such as humidity, temperature, ultraviolet (UV) radiation, and the presence of other airborne substances can influence the viability of these microorganisms. For instance, some viruses may become inactivated more rapidly in dry air, while others can persist for hours, or even days, in the right conditions.
Mechanisms of Inhalation and Deposition
Once airborne, infectious particles can travel considerable distances, especially within enclosed spaces with poor ventilation. The process of inhalation leads these particles into the respiratory system of a healthy individual. The location within the respiratory tract where these particles deposit depends on their size and the airflow patterns within the airways.
Upper vs. Lower Respiratory Tract Involvement
Larger aerosols may deposit in the upper respiratory tract, such as the nasal passages and pharynx, potentially leading to localized infections. However, smaller particles, capable of reaching the deeper parts of the lungs, can cause infections in the lower respiratory tract, such as bronchitis or pneumonia. The severity of the resulting illness is often linked to the site of deposition and the pathogen’s ability to replicate in specific tissues.
Factors Influencing Deposition
Several factors influence where inhaled particles deposit. Airflow dynamics within the respiratory system play a significant role; turbulent airflow in the larger airways can cause particles to deviate from the airflow and impact the airway walls. Smaller, more easily inhaled particles are more likely to reach the alveolar regions of the lungs. The individual’s breathing pattern also matters; faster, shallower breathing may result in deposition in the upper airways, while slower, deeper breathing can increase the likelihood of reaching the lower respiratory tract.
Common Airborne Infectious Diseases
Numerous diseases are known to spread through the air, posing significant public health challenges. Understanding which diseases are airborne is crucial for implementing targeted prevention and control strategies. The spectrum of airborne diseases ranges from common and relatively mild infections to severe and potentially fatal conditions.
Bacterial Airborne Infections
Certain bacteria are capable of airborne transmission, leading to a variety of illnesses. These bacteria often thrive in respiratory secretions and can be readily expelled into the environment.
Tuberculosis (TB)
Tuberculosis, caused by the bacterium Mycobacterium tuberculosis, is perhaps the most well-known airborne bacterial infection. TB primarily affects the lungs but can also impact other parts of the body. Inhalation of infectious aerosols from an infected individual is the primary route of transmission. The pathogen can remain dormant in the body for years before reactivating, especially in immunocompromised individuals.
Pertussis (Whooping Cough)
Pertussis, also known as whooping cough, is a highly contagious respiratory illness caused by the bacterium Bordetella pertussis. It spreads through respiratory droplets and aerosols produced during coughing fits. While vaccination has significantly reduced its incidence, outbreaks still occur, particularly in unvaccinated or under-vaccinated populations.
Viral Airborne Infections
Viruses are frequent culprits of airborne infections, and their rapid spread is often facilitated by this mode of transmission. Many common and severe viral illnesses rely on airborne routes for dissemination.
Influenza (Flu)
Influenza viruses are a prime example of airborne pathogens. Seasonal influenza epidemics are driven by the transmission of these viruses through respiratory droplets and aerosols. The virus infects the respiratory tract, causing symptoms ranging from mild to severe, including fever, cough, and body aches.
Measles
Measles is an extremely contagious viral disease that spreads through respiratory droplets and airborne particles. Infected individuals can transmit the virus for several days before the characteristic rash appears. Measles can lead to serious complications, including pneumonia and encephalitis, and its eradication relies heavily on widespread vaccination.
COVID-19
The recent global pandemic caused by the SARS-CoV-2 virus highlighted the significant threat of airborne viral transmission. While initial understanding focused on larger droplets, evidence has firmly established that SARS-CoV-2 can spread through aerosols, particularly in indoor and crowded settings. This understanding has reshaped public health recommendations for ventilation, masking, and social distancing.
Fungal Airborne Infections
While less common than bacterial or viral airborne infections, certain fungal pathogens can also spread through the air, posing risks, particularly to individuals with weakened immune systems.
Aspergillosis
Aspergillus species are ubiquitous fungi found in the environment. Inhalation of Aspergillus spores can lead to aspergillosis, a spectrum of diseases ranging from allergic reactions to invasive, life-threatening infections, especially in immunocompromised individuals. The spores can be present in dust and on decaying organic matter, becoming aerosolized and inhaled.
Factors Influencing Airborne Transmission Risk
Several environmental and behavioral factors significantly influence the risk of airborne infection transmission. Understanding these factors allows for the development of more effective control measures.
Ventilation and Air Exchange Rates
The effectiveness of ventilation in indoor spaces is a critical determinant of airborne transmission risk. Poorly ventilated areas allow airborne particles to accumulate, increasing the concentration of infectious agents and the likelihood of inhalation.
Indoor vs. Outdoor Environments
Outdoor environments generally have lower risks of airborne transmission due to the vastness of the space and constant air circulation, which dilutes any potential airborne pathogens. Indoor environments, especially those with limited airflow and high occupancy, present a significantly higher risk.
The Importance of Air Filtration and Purification
Implementing robust air filtration systems, such as HEPA filters, and air purification technologies can effectively remove airborne particles, including infectious agents, from the air. This is a crucial strategy for reducing transmission in high-risk settings.
Proximity and Duration of Exposure
The closer an individual is to an infected person and the longer the duration of exposure, the greater the risk of inhaling infectious particles. This principle underscores the importance of social distancing measures.
Close Contact and Aerosol Clouds
When an infected person coughs or sneezes, they generate an immediate cloud of respiratory droplets and aerosols. Being within this immediate vicinity increases the dose of inhaled pathogens.
Sustained Exposure in Shared Spaces
Spending prolonged periods in shared indoor spaces with an infected individual, even if not in direct close contact, can lead to cumulative exposure to airborne particles as they circulate within the environment.
Individual Susceptibility and Immunity
A person’s immune status plays a vital role in their susceptibility to airborne infections. Individuals with weakened immune systems are generally at a higher risk of contracting and developing severe illness from these diseases.
Immunocompromised Individuals
This includes individuals undergoing chemotherapy, organ transplant recipients, those with HIV/AIDS, and people with autoimmune diseases. Their compromised immune defenses make them more vulnerable to pathogens that might be easily cleared by a healthy immune system.
Vaccination Status
Vaccination is a cornerstone of preventing many airborne infections. Effective vaccines prime the immune system to recognize and fight off specific pathogens, significantly reducing the risk of infection or the severity of illness.
Strategies for Prevention and Control
Combating airborne infections requires a multi-faceted approach encompassing public health measures, personal protective behaviors, and environmental controls.
Public Health Interventions
Governmental and public health organizations play a crucial role in implementing large-scale interventions to control airborne diseases.
Vaccination Programs
Widespread vaccination campaigns are one of the most effective tools for preventing airborne infectious diseases. High vaccination rates create herd immunity, which protects even those who cannot be vaccinated.
Disease Surveillance and Outbreak Response
Robust surveillance systems are essential for detecting and monitoring the spread of airborne infections. Rapid outbreak investigation and response are critical to containing outbreaks and preventing wider dissemination.
Public Awareness and Education
Educating the public about airborne transmission, symptoms, and prevention methods is paramount. Clear and consistent communication from health authorities helps individuals make informed decisions to protect themselves and others.
Personal Protective Measures
Individual actions can significantly reduce the risk of airborne infection transmission.
Masking
Wearing masks, particularly in crowded indoor settings or when experiencing respiratory symptoms, is a highly effective method for reducing the expulsion and inhalation of airborne particles. The type of mask and its proper fit are important considerations.
Hand Hygiene
While primarily associated with direct contact transmission, thorough and frequent handwashing can prevent individuals from touching their face after contact with contaminated surfaces, thus indirectly reducing the risk of self-inoculation with airborne pathogens.
Respiratory Etiquette
Practicing good respiratory etiquette, such as covering coughs and sneezes with an elbow or tissue, helps minimize the release of infectious particles into the air.
Environmental Controls
Modifying the environment can significantly reduce the concentration of airborne pathogens.
Ventilation and Air Filtration
As previously discussed, improving indoor ventilation and employing effective air filtration systems are crucial for diluting and removing airborne infectious agents.
Social Distancing
Maintaining physical distance from others, especially in indoor settings, reduces the likelihood of inhaling infectious particles expelled by an infected individual.

Surface Cleaning and Disinfection
While airborne transmission is primarily through the air, regularly cleaning and disinfecting frequently touched surfaces can help reduce the overall pathogen load in an environment, indirectly contributing to a safer space.
In conclusion, airborne infection is a complex phenomenon driven by the release, suspension, and inhalation of infectious agents. A comprehensive understanding of the biological mechanisms, the range of diseases involved, and the influencing factors is essential. By implementing a combination of public health strategies, personal protective measures, and environmental controls, we can effectively mitigate the risks associated with airborne infections and safeguard public health.
