The Shifting Landscape of Pathogens
The term “re-emerging disease” describes an infectious disease that has appeared again in the population after a period of decline or absence. This resurgence is not a simple return; it signifies a complex interplay of environmental, social, and biological factors that allow a once-contained pathogen to regain a foothold and spread. Understanding re-emerging diseases is crucial for public health preparedness and response, as these pathogens can pose significant challenges due to pre-existing immunity waning, altered host susceptibility, or changes in the pathogen’s own characteristics. Unlike novel diseases that emerge from unknown sources, re-emerging diseases are often familiar foes, their return catching us off guard and highlighting the dynamic nature of infectious disease epidemiology.

Defining Re-emergence: A Multifaceted Phenomenon
A disease can be classified as re-emerging based on several criteria, often occurring in combination. These include:
A Resurgence in Incidence or Geographic Spread
The most apparent sign of re-emergence is an increase in the number of cases of a disease in a specific region or a spread into areas where it was previously uncommon or eradicated. This can manifest as localized outbreaks or widespread epidemics. For instance, the resurgence of measles in communities with low vaccination rates exemplifies this aspect of re-emergence.
A Return After a Period of Control or Eradication
Diseases that were once effectively controlled through public health interventions like vaccination, vector control, or antimicrobial treatment can re-emerge if these measures falter. The polio virus, though on the brink of global eradication, has seen re-emergence in some regions due to disruptions in vaccination campaigns. Similarly, diseases like dengue fever have expanded their geographic reach and increased in incidence, making them a significant re-emerging threat in many tropical and subtropical areas.
Increased Severity or Virulence
In some instances, a re-emerging disease might not only increase in frequency but also exhibit a higher rate of severe illness or mortality. This could be due to genetic mutations in the pathogen, leading to increased virulence, or changes in the host population that make individuals more susceptible to severe outcomes.
Factors Driving Re-emergence
The return of familiar pathogens is rarely a random event. It is typically driven by a confluence of factors, often amplified by human activity and global changes.
Environmental Changes and Human Encroachment
- Climate Change: Alterations in temperature, rainfall patterns, and extreme weather events can create new ecological niches for disease vectors, such as mosquitoes and ticks, allowing them to expand their range and survival periods. This has been a major contributor to the re-emergence and spread of vector-borne diseases like West Nile virus and Lyme disease.
- Deforestation and Habitat Destruction: As human populations expand into previously untouched natural areas, there is increased contact between humans and wildlife, facilitating the spillover of zoonotic pathogens. This encroachment can also disrupt ecosystems, potentially altering the dynamics of existing disease cycles.
- Urbanization and Population Density: Rapid urbanization, often accompanied by inadequate sanitation and housing, can create conditions conducive to the rapid transmission of infectious agents. High population density in urban centers can facilitate the spread of respiratory and foodborne illnesses.
Societal and Behavioral Shifts
- Globalization and Travel: The unprecedented ease and volume of international travel mean that infectious diseases can spread across continents with remarkable speed. A localized outbreak in one corner of the world can become a global concern within days.
- Antimicrobial Resistance (AMR): The overuse and misuse of antibiotics have led to the evolution of drug-resistant bacteria, making once-treatable infections challenging to manage. This is a significant driver for the re-emergence of bacterial infections that were previously well-controlled.
- Changes in Public Health Infrastructure: Weakening of public health systems, reduced funding for disease surveillance, and declining vaccination rates can create vulnerabilities that pathogens exploit. The erosion of herd immunity, for example, leaves populations susceptible to vaccine-preventable diseases.
- War and Political Instability: Conflict and displacement can disrupt healthcare services, sanitation, and food security, leading to outbreaks of diseases like cholera, typhoid, and other infectious conditions.
Pathogen Evolution and Adaptation
- Genetic Mutation: Viruses and bacteria are constantly evolving. Genetic mutations can alter a pathogen’s ability to infect hosts, evade the immune system, or spread more efficiently. This can lead to increased virulence or a return to infectivity after periods of attenuation.
- Recombination and Reassortment: For some viruses, genetic material can be exchanged between different strains or viruses, creating new variants with novel characteristics that can contribute to re-emergence.
Examples of Re-emerging Diseases
The phenomenon of re-emerging diseases is not theoretical; it is a tangible reality reflected in the global health landscape. Numerous pathogens that were once considered under control or declining have demonstrated alarming resurgences.
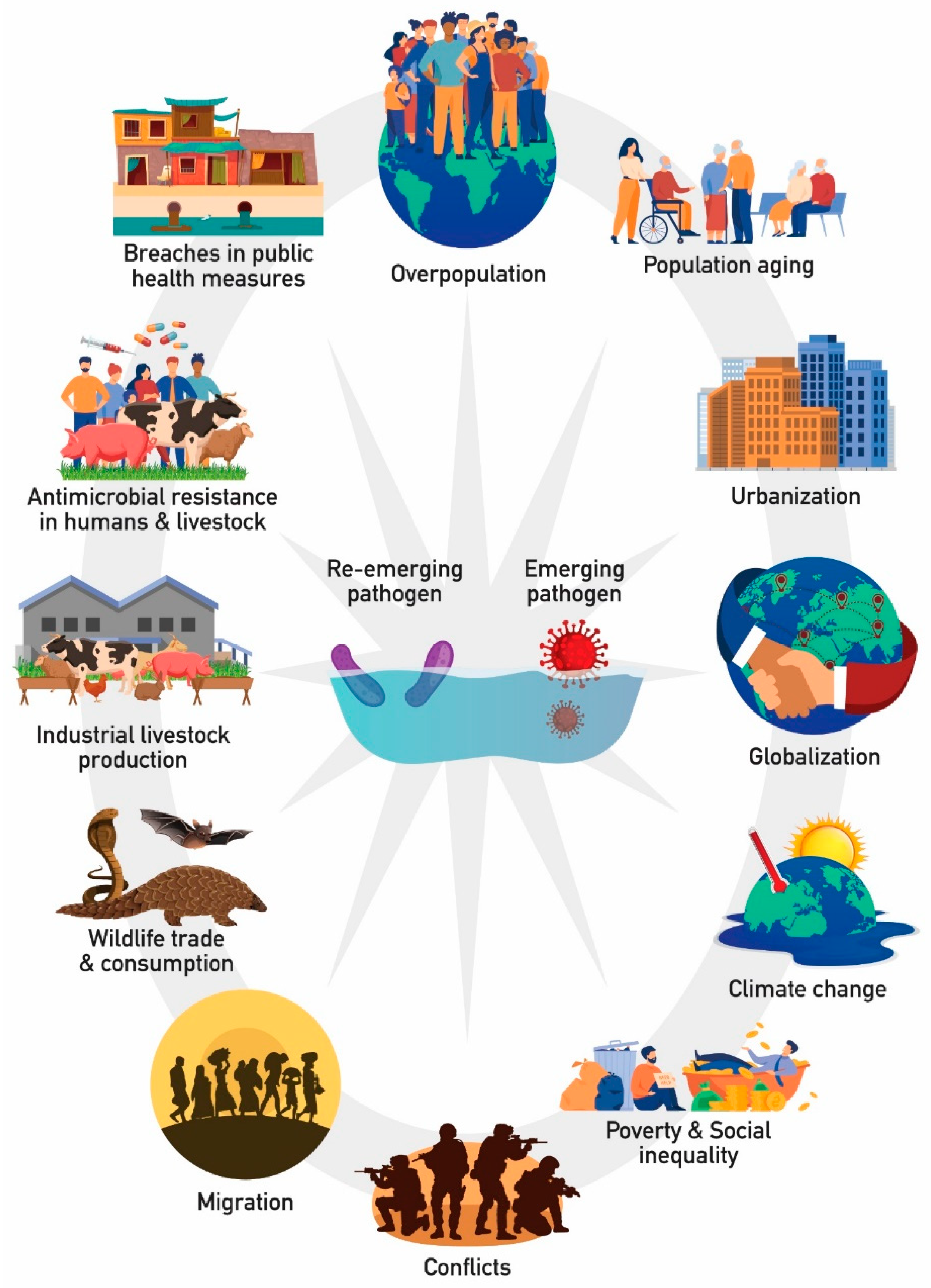
Vector-Borne Diseases: A Growing Concern
Vector-borne diseases, transmitted by arthropods like mosquitoes, ticks, and fleas, represent a significant and expanding category of re-emerging illnesses.
- Dengue Fever: Once confined to a few tropical regions, dengue has seen a dramatic increase in its global burden. It is now endemic in over 100 countries, affecting millions annually. Factors contributing to its re-emergence include increased urbanization, inadequate vector control, and changes in mosquito breeding patterns influenced by climate change. The emergence of all four dengue virus serotypes in many areas has also increased the risk of severe dengue.
- Zika Virus: While the 2015-2016 Zika outbreak in the Americas brought this virus to global attention, it had been circulating in Southeast Asia and Africa for decades. The rapid spread and association with microcephaly in newborns highlighted the potential for seemingly minor pathogens to cause significant public health crises when introduced into immunologically naive populations or under changing environmental conditions.
- Lyme Disease: The most common vector-borne disease in the Northern Hemisphere, Lyme disease, has seen its geographic range expand significantly in recent decades. This expansion is linked to reforestation, changes in deer populations (which carry ticks), and warmer winters that allow tick populations to thrive in new areas.
- Malaria: Despite decades of control efforts, malaria remains a major global health challenge, with some regions experiencing resurgence due to drug resistance in the parasite, insecticide resistance in mosquitoes, and disruption of control programs by conflict or natural disasters.
Zoonotic Diseases: The Human-Animal Interface
Zoonotic diseases, which originate in animals and transmit to humans, are a prime example of re-emerging threats, particularly as human activities bring us into closer contact with wildlife.
- Ebola Virus Disease: While Ebola outbreaks have historically been localized and rare, the 2014-2016 West African epidemic was unprecedented in scale and geographic reach. This outbreak highlighted the potential for zoonotic spillover events to escalate into widespread epidemics, driven by complex ecological factors and social conditions.
- Avian Influenza (Bird Flu): Various strains of avian influenza, such as H5N1 and H7N9, continue to circulate in bird populations and occasionally infect humans. While human-to-human transmission has historically been limited, the potential for these viruses to adapt and evolve into pandemic strains remains a significant public health concern, representing a constant re-emerging threat.
- Rabies: Though largely preventable with vaccination, rabies continues to re-emerge in certain populations, particularly in developing countries. The virus is maintained in domestic animal populations, and its re-emergence in humans is often linked to lapses in animal vaccination programs and inadequate access to post-exposure prophylaxis for humans.
Bacterial and Viral Diseases: Familiar Threats Resurfacing
Even diseases that were once thought to be well-managed can make a comeback.
- Tuberculosis (TB): Despite being a curable disease, TB remains a leading cause of death worldwide, and in some areas, it is re-emerging due to factors like HIV co-infection, drug resistance (MDR-TB and XDR-TB), and weakened public health systems.
- Cholera: This acute diarrheal disease, caused by Vibrio cholerae, thrives in conditions of poor sanitation and contaminated water. Outbreaks frequently re-emerge after natural disasters or in regions experiencing political instability, overwhelming already fragile healthcare infrastructures.
- Measles: Once on the path to elimination in many parts of the world, measles has seen significant resurgences in recent years. This is largely attributable to declining vaccination rates, often fueled by vaccine hesitancy and misinformation, which erode herd immunity and leave communities vulnerable to outbreaks.
Public Health Implications and Strategies
The re-emergence of diseases poses a continuous challenge to global public health. It necessitates a proactive and adaptable approach, moving beyond simply reacting to outbreaks to anticipating and mitigating future threats.
The Importance of Robust Surveillance and Early Warning Systems
Effective surveillance is the cornerstone of managing re-emerging diseases. This involves:
- Integrated Disease Surveillance: Establishing systems that monitor for a wide range of pathogens across different populations and environments. This includes human health, animal health, and environmental monitoring (a “One Health” approach).
- Genomic Surveillance: Utilizing advanced genetic sequencing technologies to track pathogen evolution, identify new variants, and understand transmission patterns in near real-time. This is crucial for detecting early signs of changes in virulence or transmissibility.
- Data Integration and Analysis: Developing sophisticated platforms for collecting, analyzing, and sharing surveillance data rapidly among different agencies and international bodies. This allows for quicker detection of anomalies and more informed decision-making.
Strengthening Public Health Infrastructure and Interventions
Re-emerging diseases highlight the need for sustained investment in public health:
- Vaccination Programs: Maintaining high vaccination coverage for established vaccines is critical to prevent the resurgence of vaccine-preventable diseases. Addressing vaccine hesitancy through education and community engagement is paramount.
- Vector Control: Implementing comprehensive and integrated vector control strategies, including environmental management, biological control, and targeted use of insecticides, is essential for managing vector-borne diseases.
- Antimicrobial Stewardship: Promoting responsible use of antibiotics in human and animal health, alongside research into new antimicrobial agents, is vital to combat the growing threat of AMR.
- Sanitation and Hygiene: Investing in and improving access to clean water and sanitation infrastructure is fundamental in preventing the spread of many infectious diseases, particularly in vulnerable communities.
- Emergency Preparedness and Response: Developing and regularly testing robust emergency response plans for infectious disease outbreaks, including surge capacity in healthcare systems and stockpiling of essential medical supplies.

Fostering Global Collaboration and Research
No single country can effectively combat re-emerging diseases alone. International cooperation is indispensable:
- Information Sharing: Open and timely sharing of epidemiological data, research findings, and best practices among nations.
- Joint Research Initiatives: Collaborating on research into pathogen biology, transmission dynamics, diagnostics, treatments, and vaccine development.
- Capacity Building: Supporting lower-income countries in strengthening their public health infrastructure, laboratory capabilities, and trained workforce to detect and respond to disease threats.
- Addressing the Root Causes: Recognizing and acting upon the underlying drivers of re-emergence, such as climate change mitigation, sustainable land use practices, and poverty reduction, is crucial for long-term prevention.
The battle against re-emerging diseases is an ongoing one, demanding vigilance, innovation, and a collective commitment to safeguarding global health. By understanding the complex factors that drive these resurgences and by implementing comprehensive, collaborative strategies, we can better protect ourselves from the familiar threats that continue to resurface.
