This article delves into the intricacies of uterine prolapse, a condition that affects many women. We will explore its causes, symptoms, diagnostic methods, and the various treatment options available. Understanding uterine prolapse is crucial for women to recognize the signs and seek appropriate medical attention, ultimately improving their quality of life.
Understanding Uterine Prolapse: A Foundation
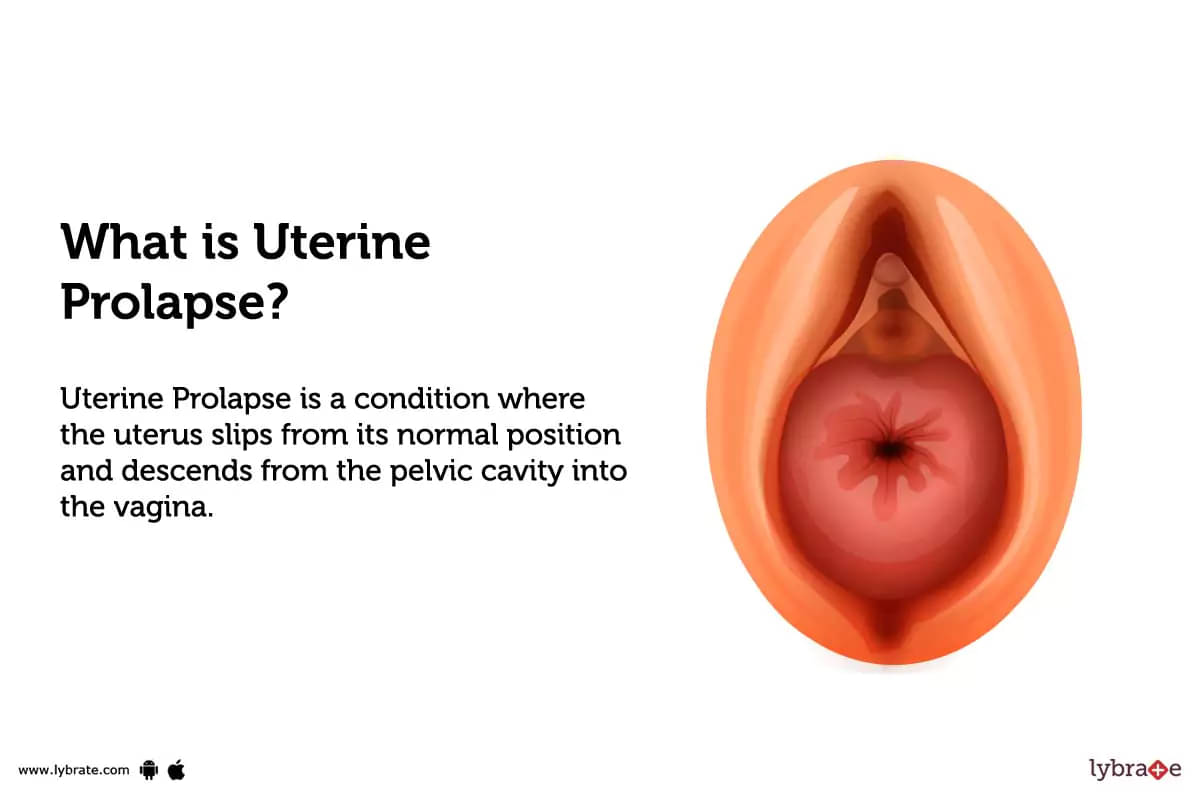
Uterine prolapse occurs when the pelvic floor muscles and ligaments that support the uterus become weakened or damaged. This loss of support allows the uterus to descend from its normal position in the pelvis and into or out of the vaginal canal. The severity of prolapse can range from mild, where the uterus only slightly drops, to severe, where it protrudes significantly from the vagina.

Anatomy of Pelvic Support
To comprehend uterine prolapse, it’s essential to understand the pelvic floor. This complex network of muscles, ligaments, and connective tissues forms a hammock-like structure at the base of the pelvis. It plays a vital role in supporting pelvic organs, including the uterus, bladder, and rectum, and is crucial for maintaining urinary and fecal continence. When these supportive structures are compromised, the organs can descend.
Contributing Factors to Pelvic Floor Weakness
Several factors can contribute to the weakening of the pelvic floor muscles and ligaments. One of the most common and significant is childbirth. Vaginal deliveries, especially those that are prolonged, involve large babies, or require assisted delivery techniques like forceps or vacuum extraction, can stretch and damage the pelvic floor. Multiple pregnancies also increase the risk.
Other significant contributors include:
- Aging and Menopause: As women age, estrogen levels decline, particularly after menopause. Estrogen plays a role in maintaining the strength and elasticity of pelvic tissues. A decrease in estrogen can lead to thinning and weakening of these structures, making them more susceptible to prolapse.
- Chronic Cough or Straining: Persistent conditions that lead to increased intra-abdominal pressure can put significant strain on the pelvic floor over time. This includes chronic bronchitis, emphysema, persistent constipation, and heavy lifting, especially in occupational settings.
- Obesity: Excess body weight increases the pressure on the pelvic floor. This constant pressure can weaken the muscles and ligaments, increasing the likelihood of prolapse.
- Genetics: Some women may have a genetic predisposition to weaker connective tissues, making them more vulnerable to developing pelvic organ prolapse.
- Previous Pelvic Surgery: Certain surgeries in the pelvic region, particularly hysterectomy (though this addresses prolapse of other organs when the uterus is removed), can sometimes affect the supporting structures.
Stages of Uterine Prolapse
Uterine prolapse is typically classified into four stages, based on the degree to which the uterus has descended:
- Stage 0 (Normal): The uterus is in its normal position.
- Stage I (Mild): The uterus descends into the upper vagina, but does not protrude outside the vaginal opening.
- Stage II (Moderate): The uterus descends to the level of the vaginal opening, and may begin to protrude during straining.
- Stage III (Severe): The uterus protrudes from the vaginal opening.
- Stage IV (Complete or Procidentia): The entire uterus has fallen out of the vagina.
Recognizing the Signs: Symptoms of Uterine Prolapse
The symptoms of uterine prolapse can vary widely depending on the severity of the condition. Many women with mild prolapse experience no noticeable symptoms and may only discover it during a routine pelvic examination. However, as the prolapse progresses, symptoms become more pronounced and can significantly impact a woman’s quality of life.
Common Symptoms
- A Feeling of Heaviness or Pressure in the Pelvis: This is often described as a dragging sensation or a feeling that something is falling out of the vagina. It may be worse at the end of the day or after standing for long periods.
- A Visible or Palpable Mass in the Vagina: In moderate to severe cases, women may feel or see a bulge or lump protruding from the vaginal opening. This sensation might be more noticeable when coughing, sneezing, or straining.
- Urinary Symptoms: As the uterus descends, it can put pressure on the bladder and urethra. This can lead to:
- Urinary Incontinence: Stress incontinence (leakage of urine during coughing, sneezing, or exercise) is common.
- Urgency: A sudden, strong urge to urinate.
- Frequency: Needing to urinate more often than usual.
- Difficulty Emptying the Bladder: In severe cases, the prolapse can kink the urethra, making it difficult to fully empty the bladder.
- Recurrent Urinary Tract Infections (UTIs): Incomplete bladder emptying can contribute to the development of UTIs.
- Bowel Symptoms: Pressure on the rectum can also lead to bowel-related issues:
- Constipation: Difficulty passing stools due to pressure or kinking of the rectum.
- Feeling of Incomplete Bowel Emptying: A sensation that the bowels have not been fully emptied after a bowel movement.
- Fecal Incontinence: Leakage of stool or gas, although this is less common than urinary incontinence.
- Sexual Dysfunction: The changes in vaginal anatomy due to prolapse can lead to discomfort or pain during sexual intercourse (dyspareunia). Some women may also experience a decreased libido.
- Low Back Pain: While not always directly caused by prolapse, the altered pelvic anatomy can sometimes lead to or exacerbate lower back pain.
When to Seek Medical Advice
It is important for women to consult a healthcare professional if they experience any of the symptoms mentioned above, especially if they are persistent or worsening. Early diagnosis and intervention can prevent the condition from progressing and improve treatment outcomes.
Diagnosis and Assessment
Diagnosing uterine prolapse typically involves a thorough medical history, a physical examination, and potentially further tests to assess the extent of the prolapse and rule out other conditions.
Medical History and Symptom Review
The initial step in diagnosis involves a detailed discussion with a healthcare provider about the patient’s medical history, including any previous pregnancies, births, surgeries, and chronic medical conditions. The provider will ask about the specific symptoms experienced, their onset, and their impact on daily life.
Pelvic Examination

A physical examination is the cornerstone of diagnosing uterine prolapse. The healthcare provider will perform a bimanual pelvic exam to assess the position of the pelvic organs. This involves:
- Visual Inspection: Examining the vulva and vaginal opening for any visible protrusion.
- Palpation: Gently inserting gloved fingers into the vagina to feel for the uterus and other pelvic organs. The provider may ask the patient to cough, bear down, or strain during the exam to assess how the prolapse changes with increased intra-abdominal pressure.
- Assessing Pelvic Floor Muscle Strength: The provider may also assess the strength of the pelvic floor muscles.
Imaging and Diagnostic Tests
In some cases, further tests may be recommended to confirm the diagnosis, determine the severity, and rule out other potential issues:
- Urodynamic Studies: These tests evaluate bladder function and are particularly useful if urinary incontinence is a significant symptom. They can help determine if the prolapse is contributing to bladder dysfunction.
- Pelvic Ultrasound: An ultrasound can provide images of the pelvic organs and assess their position and any associated abnormalities.
- Cystoscopy: This procedure involves inserting a thin, flexible tube with a light and camera into the bladder to visualize the bladder and urethra. It is used to investigate urinary symptoms and rule out other bladder conditions.
- Defecography: This imaging test assesses bowel function and can be helpful in identifying problems with bowel emptying that may be related to prolapse.
Treatment Options for Uterine Prolapse
The treatment approach for uterine prolapse is tailored to the individual patient, considering the severity of the prolapse, the presence and bothersomeness of symptoms, the patient’s age, overall health, and desire for future fertility. Treatment options range from conservative management to surgical interventions.
Conservative Management
For mild to moderate prolapse with minimal or no bothersome symptoms, conservative management may be sufficient. These approaches focus on strengthening pelvic floor muscles and reducing strain.
- Pelvic Floor Muscle Exercises (Kegels): These exercises involve consciously contracting and relaxing the pelvic floor muscles. Regular and correct execution of Kegel exercises can strengthen these muscles, providing better support for the pelvic organs. A physical therapist specializing in pelvic floor rehabilitation can provide guidance on proper technique.
- Lifestyle Modifications:
- Weight Management: Losing excess weight can significantly reduce pressure on the pelvic floor.
- Dietary Changes: Increasing fiber intake and ensuring adequate hydration can prevent constipation and reduce straining during bowel movements.
- Avoiding Heavy Lifting: Limiting activities that involve heavy lifting can decrease intra-abdominal pressure.
- Managing Chronic Cough: Seeking treatment for conditions that cause chronic coughing can reduce the strain on the pelvic floor.
- Pessaries: A pessary is a removable device inserted into the vagina to support the prolapsed organs. Pessaries come in various shapes and sizes and can be effective in alleviating symptoms for many women. They require regular cleaning and follow-up appointments with a healthcare provider to ensure proper fit and prevent complications like vaginal irritation or infection.
Surgical Interventions
When conservative measures are insufficient or when prolapse is severe and significantly impacting a woman’s quality of life, surgery may be recommended. Surgical options aim to repair the damaged pelvic floor support and restore the organs to their normal positions.
- Vaginal Surgery: This is the most common approach for uterine prolapse. The surgeon can repair the prolapse by:
- Uterine Suspension: Reattaching the uterus to stronger pelvic ligaments, pulling it back into its normal position.
- Colporrhaphy: This procedure repairs weakened vaginal walls. Anterior colporrhaphy addresses weakness in the front vaginal wall (often associated with bladder prolapse), while posterior colporrhaphy addresses weakness in the back vaginal wall (often associated with rectal prolapse).
- Abdominal Surgery: In some cases, particularly for more severe prolapse or when vaginal surgery is not feasible, abdominal surgery may be performed. This can involve:
- Sacrocolpopexy: The uterus is suspended to the sacrum (the triangular bone at the base of the spine) using surgical mesh. This procedure can be performed laparoscopically or abdominally.
- Hysterectomy: If a woman has completed childbearing and the prolapse is significant, a hysterectomy (surgical removal of the uterus) may be performed along with prolapse repair procedures. However, hysterectomy alone does not fix prolapse, as the vaginal vault can still prolapse.
- Minimally Invasive Surgery: Laparoscopic and robotic-assisted surgeries are becoming increasingly common. These techniques involve smaller incisions, potentially leading to less pain, shorter recovery times, and reduced scarring.
The choice between vaginal and abdominal surgery, and whether to perform a hysterectomy, depends on individual factors and the surgeon’s expertise. Post-operative recovery varies, but typically involves avoiding strenuous activity and sexual intercourse for several weeks. Long-term success rates for surgical repair are generally high, but there is a possibility of recurrence in some cases.
Living with and Preventing Uterine Prolapse
While uterine prolapse can be a distressing condition, it is manageable, and proactive steps can be taken to prevent its development or progression and to improve the quality of life for those affected.
Managing Symptoms and Long-Term Outlook
For women with uterine prolapse, ongoing management is key. This may involve:
- Regular Follow-Up Care: Attending scheduled appointments with healthcare providers is crucial to monitor the prolapse, assess the effectiveness of treatment, and address any new concerns.
- Continued Pelvic Floor Exercises: Even after successful treatment, maintaining strong pelvic floor muscles through regular exercises is vital for long-term support.
- Adhering to Lifestyle Recommendations: Continuing with healthy habits such as maintaining a healthy weight, a fiber-rich diet, and adequate hydration will continue to benefit pelvic health.
- Utilizing Pessaries: For women who opt for pessary use, consistent cleaning and regular check-ups are essential to prevent complications.
The long-term outlook for women with uterine prolapse is generally positive, especially with appropriate treatment. While the condition can recur, especially if contributing factors are not addressed, most women can achieve significant symptom relief and maintain a good quality of life.
Preventive Strategies
Preventing uterine prolapse involves strengthening and protecting the pelvic floor muscles throughout a woman’s life.
- Pelvic Floor Exercises: Starting Kegel exercises during pregnancy and continuing them postpartum can help maintain pelvic floor strength. These exercises are beneficial at any stage of life.
- Healthy Weight Maintenance: Maintaining a healthy body weight reduces the chronic strain on the pelvic floor.
- Preventing Constipation: A high-fiber diet, adequate fluid intake, and avoiding straining during bowel movements are critical.
- Proper Lifting Techniques: When lifting heavy objects, it’s important to use proper body mechanics to avoid putting excessive pressure on the abdomen and pelvis.
- Managing Chronic Cough: Seeking medical advice and treatment for persistent coughs is important to reduce sustained pressure on the pelvic floor.
- Avoiding Smoking: Smoking can weaken connective tissues throughout the body, potentially contributing to pelvic floor weakness.
Empowering Women’s Health
Understanding uterine prolapse and its implications is an essential part of women’s health education. Open communication with healthcare providers, proactive management of symptoms, and adherence to preventive strategies can empower women to take control of their pelvic health and live fulfilling lives. By raising awareness and encouraging timely medical consultation, the impact of uterine prolapse can be significantly mitigated.
