Tirzepatide, a groundbreaking dual GIP and GLP-1 receptor agonist, has emerged as a significant advancement in the management of type 2 diabetes and chronic weight management. While initial treatment phases often focus on escalating doses to achieve therapeutic targets, understanding and implementing a “maintenance dose” is crucial for long-term efficacy, safety, and patient adherence. This concept differentiates from the titration schedule, representing a steady, sustained level of the medication designed for ongoing benefit after the initial dose escalation period.
Understanding Tirzepatide Dosing Regimens
Tirzepatide is administered via subcutaneous injection, typically once weekly. The dosing strategy is carefully designed to allow the body to adapt to the medication’s effects while maximizing its therapeutic potential. This typically involves an initial titration phase, where the dose is gradually increased over several weeks. This phased approach helps to minimize potential gastrointestinal side effects, which are common with incretin-based therapies.
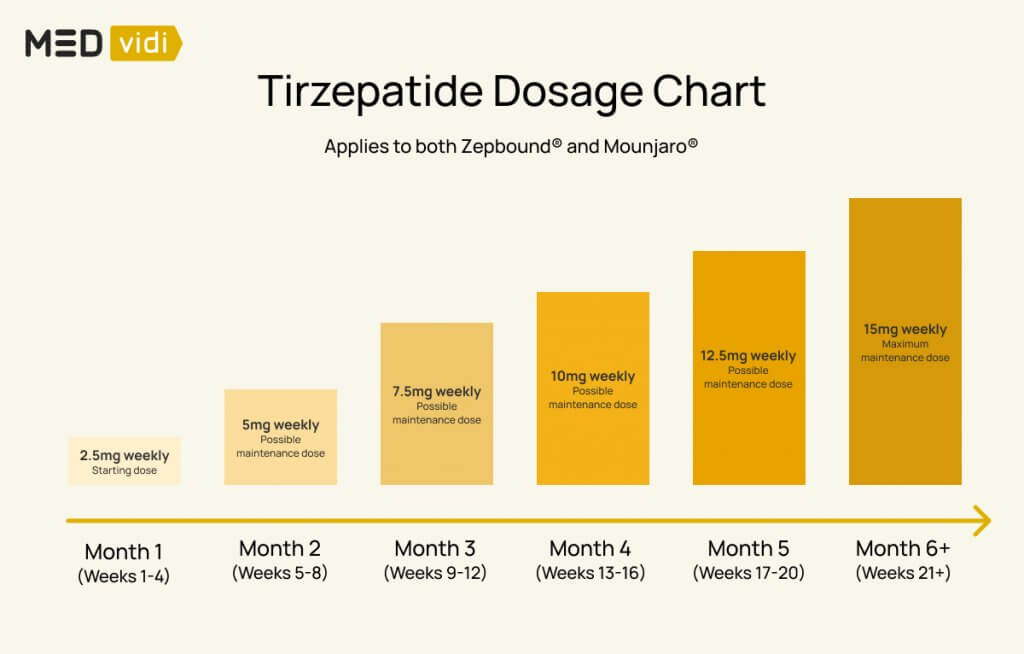
Initial Titration Phase
The standard titration schedule for tirzepatide usually begins with a low dose, often 2.5 mg once weekly. This dose is maintained for a defined period, typically four weeks, to assess tolerability. Following this initial period, the dose is progressively increased. Common subsequent doses include 5 mg, 10 mg, and potentially higher, depending on the individual’s response, tolerability, and therapeutic goals. This escalation is critical for achieving the desired glycemic control in type 2 diabetes or significant weight reduction.
The Transition to Maintenance
The concept of a “maintenance dose” in the context of tirzepatide refers to the dose that an individual will continue to receive long-term, after the titration phase is complete. This is not a formally defined, universally fixed dose that applies to all patients. Instead, it is an individualized dose determined by the treating physician based on a comprehensive assessment of the patient’s clinical response, including:
- Glycemic Control (for Type 2 Diabetes): For patients with type 2 diabetes, the maintenance dose is the level that consistently achieves target HbA1c levels, fasting blood glucose, and postprandial glucose readings, as defined by established clinical guidelines. It ensures sustained improvements in blood sugar regulation.
- Weight Management (for Chronic Weight Management): For individuals using tirzepatide for weight management, the maintenance dose is the level that facilitates and sustains a significant and clinically meaningful percentage of body weight loss. This also includes achieving and maintaining target weight-related health metrics.
- Tolerability and Side Effect Profile: A crucial aspect of determining the maintenance dose is ensuring the patient can tolerate the medication long-term with minimal or manageable side effects. If a higher dose during titration leads to persistent or bothersome adverse events, the physician may opt to maintain a lower, more tolerable dose, even if it means slightly less optimal glycemic control or weight loss. The goal is to find a balance between efficacy and patient well-being.
- Individual Patient Factors: Age, kidney function, liver function, other co-existing medical conditions, and concomitant medications all play a role in determining the optimal maintenance dose. A physician will consider these factors holistically.
Essentially, the maintenance dose is the highest effective dose that can be safely and comfortably tolerated by the patient for an extended period, achieving the desired therapeutic outcomes.
Differentiating Maintenance Dose from Maximum Recommended Dose
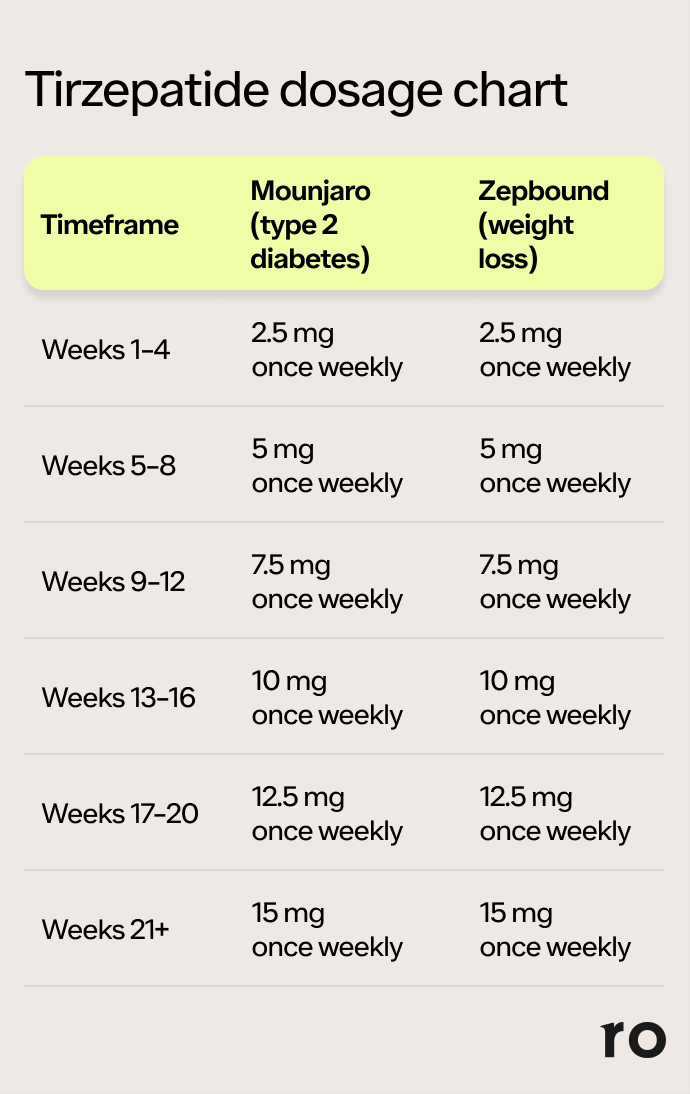
It is important to distinguish between a “maintenance dose” and the “maximum recommended dose” of tirzepatide. The maximum recommended dose, as established by regulatory bodies and reflected in clinical trial data, represents the upper limit of what has been demonstrated to be safe and effective in large patient populations. For tirzepatide, this is typically 15 mg once weekly for type 2 diabetes and chronic weight management.
However, not all individuals will reach or require the maximum recommended dose to achieve their therapeutic goals. Some patients may find that a lower dose, such as 5 mg or 10 mg weekly, provides sufficient glycemic control or weight loss while being exceptionally well-tolerated. In such cases, this lower, well-tolerated dose becomes their effective maintenance dose.
Conversely, some patients may tolerate and benefit from the maximum recommended dose of 15 mg weekly, and this would then constitute their maintenance dose. The decision to continue at the maximum dose hinges on continued benefit and acceptable tolerability.
The maintenance dose is thus a personalized target, distinct from a rigid maximum. It signifies the dose at which the benefits of tirzepatide are sustained with an acceptable risk profile for that specific individual.
Long-Term Benefits and Adherence
The establishment of an appropriate maintenance dose is fundamental to the long-term success of tirzepatide therapy. Once a stable and effective dose is identified, patients can continue to reap the benefits of improved metabolic health and/or sustained weight management.
Sustained Glycemic Control
For individuals with type 2 diabetes, a consistent maintenance dose helps to prevent the “rollercoaster” effect of fluctuating blood sugar levels. This sustained control is vital in mitigating the risk of long-term diabetes complications, such as cardiovascular disease, nephropathy, retinopathy, and neuropathy. By keeping glucose levels within a target range, the maintenance dose contributes to a healthier metabolic environment.
Sustainable Weight Management
In the context of chronic weight management, the maintenance dose plays a critical role in preventing weight regain. Significant weight loss achieved during the titration phase can be consolidated and maintained when the patient continues on an effective maintenance dose. This ongoing support for weight management is essential for long-term health benefits, including improved blood pressure, cholesterol levels, and reduced risk of obesity-related comorbidities like sleep apnea and osteoarthritis.
Impact on Adherence and Quality of Life
Identifying a tolerable maintenance dose significantly impacts patient adherence. When a medication is well-tolerated and provides tangible benefits, patients are more likely to continue taking it as prescribed. This adherence is paramount for achieving and sustaining the desired health outcomes. Furthermore, the positive effects on health metrics, coupled with a manageable side effect profile, can lead to a substantial improvement in a patient’s overall quality of life, enabling them to engage more fully in daily activities and pursue personal goals without the burden of uncontrolled diabetes or excess weight.
Monitoring and Adjustments of Maintenance Dose
While the term “maintenance dose” implies stability, it does not mean that the dose is entirely static or that monitoring ceases. Healthcare providers will continue to monitor patients receiving tirzepatide, even after a maintenance dose has been established.
Ongoing Clinical Assessment
Regular follow-up appointments are essential. During these visits, the physician will assess:
- Efficacy: Are the therapeutic goals (e.g., HbA1c targets, weight loss percentage) still being met?
- Tolerability: Are there any new or persistent side effects? Has the patient’s ability to tolerate the current dose changed?
- Overall Health Status: Are there any changes in kidney function, liver function, or other relevant health markers?
- Patient Lifestyle Factors: Changes in diet, exercise, stress levels, or other life circumstances can influence metabolic health and potentially necessitate dose adjustments.

Potential for Dose Adjustments
Although the goal of a maintenance dose is stability, adjustments may still be warranted. For instance:
- Worsening Glycemic Control: If a patient’s HbA1c starts to drift upwards despite consistent adherence, the physician might consider increasing the dose, if the maximum recommended dose has not yet been reached and if the patient can tolerate it.
- Significant Weight Regain: In weight management scenarios, if a patient begins to regain weight despite being on a maintenance dose, a dose adjustment might be considered, or a reassessment of lifestyle factors would be undertaken.
- Development of Intolerances: Conversely, if a patient who was previously tolerating a dose well starts experiencing new or worsening side effects, a dose reduction might be necessary.
- Emergence of Comorbidities or Changes in Organ Function: The development of new health conditions or changes in the function of organs like the kidneys can necessitate adjustments to medication doses.
The concept of a maintenance dose for tirzepatide, therefore, represents a personalized, long-term therapeutic target that is continually evaluated. It is the dose that provides sustained benefits with optimal tolerability, contributing significantly to the improved health and quality of life for individuals managing type 2 diabetes or chronic weight. This individualized approach underscores the precision medicine paradigm in modern pharmacotherapy.
