A jejunostomy tube, often abbreviated as a J-tube, is a specialized medical device that plays a critical role in providing nutrition and sometimes medication directly to the jejunum, the middle section of the small intestine. This method of feeding, known as jejunal feeding, bypasses the stomach and duodenum, offering a vital lifeline for individuals who cannot adequately receive nourishment through oral intake due to a variety of medical conditions. Understanding the intricacies of a jejunostomy tube involves delving into its purpose, the conditions it addresses, the insertion process, its care, and the potential benefits and considerations associated with its use.
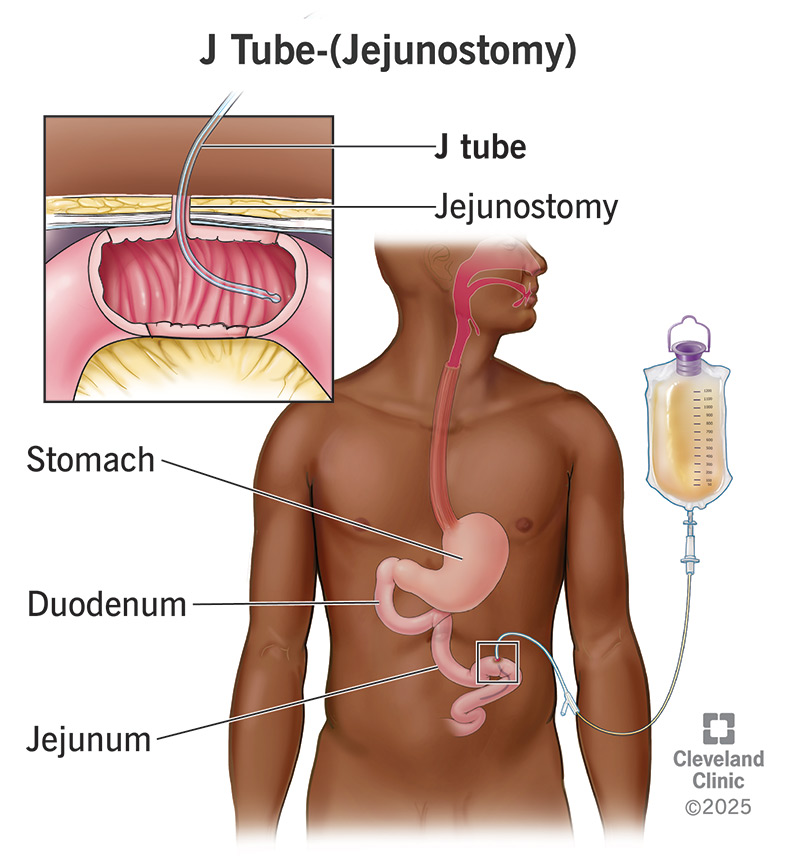
Understanding Jejunostomy Feeding
Jejunal feeding is a form of enteral nutrition, which means providing nutrition through the gastrointestinal tract. Unlike gastrostomy feeding, which delivers nutrients into the stomach, jejunal feeding directs them further down into the digestive system. This distinction is crucial for patients with specific medical challenges that make stomach feeding problematic or impossible.
The Role of the Jejunum
The jejunum is the primary site for the absorption of most nutrients, including carbohydrates, proteins, fats, vitamins, and minerals. By delivering feeding directly into this area, the body can efficiently absorb the essential components of a specialized liquid diet. This direct delivery system is particularly beneficial when the upper portions of the digestive tract are compromised.
When is Jejunostomy Feeding Necessary?
Several medical scenarios necessitate the use of a jejunostomy tube. These often involve conditions that impair swallowing, gastric emptying, or the ability to tolerate oral or gastric feeding.
Impaired Swallowing (Dysphagia)
Severe dysphagia, resulting from conditions like stroke, head and neck cancers, neurological disorders (e.g., amyotrophic lateral sclerosis – ALS, Parkinson’s disease), or severe trauma, can make oral ingestion of food dangerous or impossible. Aspiration, the inhalation of food or liquid into the lungs, is a significant risk with dysphagia and can lead to pneumonia and other serious complications. Jejunal feeding completely bypasses the swallowing mechanism, eliminating this risk.
Gastric Motility Disorders
Certain conditions affect the normal muscular contractions of the stomach that move food along the digestive tract. Gastroparesis, often associated with diabetes, can significantly delay gastric emptying, leading to nausea, vomiting, abdominal pain, and malnutrition. In such cases, feeding into the jejunum provides a way to deliver nutrition past the sluggish stomach.
Upper Gastrointestinal Obstructions or Malignancies
Blockages in the esophagus, stomach, or duodenum, caused by tumors, strictures (narrowing), or severe inflammation, can prevent food from passing through. A jejunostomy tube can circumvent these obstructions, allowing for nutritional support when oral or gastric routes are compromised.
Pancreatitis and Short Bowel Syndrome
In cases of severe pancreatitis, the digestive system needs to be rested to allow for healing. Jejunal feeding can provide the necessary nutrition without stimulating pancreatic enzyme production. Similarly, in patients with short bowel syndrome, where a significant portion of the small intestine has been removed, jejunal feeding can maximize nutrient absorption by delivering it to the remaining functional segments.
Pre- and Post-Surgical Nutritional Support
Jejunostomy tubes are sometimes used to provide nutritional support before or after certain surgeries, particularly those involving the gastrointestinal tract or head and neck. This can help improve the patient’s nutritional status, which is crucial for healing and recovery.
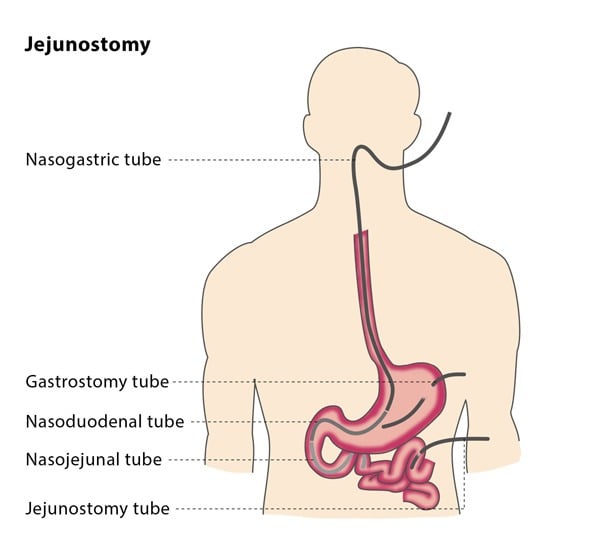
Types of Jejunostomy Tubes
Jejunostomy tubes come in various types, with the most common being percutaneous endoscopic gastrostomy with jejunal extension (PEG-J) tubes and surgically placed jejunostomy tubes.
PEG-J Tubes
A PEG-J tube is a dual-lumen tube. The larger lumen exits the abdomen at the stomach site and is used for gastric decompression or medication administration. The smaller, thinner lumen extends through the stomach and into the jejunum, serving as the feeding port. This type of tube is inserted endoscopically, often under sedation, making it a less invasive procedure compared to open surgery.
Surgically Placed Jejunostomy Tubes
These tubes are inserted during an open surgical procedure. While more invasive, surgical placement allows for greater flexibility in tube size and positioning, and may be preferred in certain complex cases or when other surgical interventions are being performed concurrently.
The Jejunostomy Tube Insertion Process
The insertion of a jejunostomy tube is a medical procedure performed by trained healthcare professionals, typically gastroenterologists or surgeons, depending on the method. The goal is to safely and effectively place the tube into the jejunum.
Percutaneous Endoscopic Gastrostomy with Jejunostomy Extension (PEG-J)
The PEG-J procedure is the most common method. It involves the following steps:
- Preparation: The patient is sedated, and the abdominal area is cleaned and prepped.
- Endoscopic Visualization: A flexible, lighted instrument called an endoscope is passed down the esophagus and into the stomach. This allows the physician to visualize the stomach and the point where the jejunal tube will be inserted.
- Tube Placement: A small incision is made in the abdominal wall. A guidewire is passed through the incision and then through the stomach and into the jejunum, guided by the endoscope. The feeding tube, often with a jejunal extension, is then threaded over the guidewire and into position.
- Securing the Tube: The external portion of the tube is secured to the abdominal wall with a fixation device to prevent dislodgement. An internal bumper or bolster holds the tube in place within the body.
- Confirmation: The position of the tube is confirmed using imaging techniques, such as an X-ray, to ensure it is correctly placed in the jejunum.
Surgical Jejunostomy
Surgical placement can be done laparoscopically or through an open incision.
- Laparoscopic Approach: This minimally invasive technique involves making several small incisions through which surgical instruments and a camera are inserted. The surgeon can then visualize the abdominal organs and place the jejunostomy tube.
- Open Surgical Approach: This involves a larger incision, allowing direct access to the abdominal cavity. This method might be chosen for patients with extensive adhesions, those undergoing other abdominal surgeries, or when laparoscopic access is not feasible.
Following insertion, regardless of the method, patients are closely monitored for any immediate complications.
Care and Maintenance of a Jejunostomy Tube
Proper care and maintenance of a jejunostomy tube are paramount to prevent complications, ensure effective feeding, and maintain the patient’s well-being. This involves regular cleaning, monitoring for signs of infection or dislodgement, and careful administration of feedings and medications.
Site Care
The skin around the stoma (the opening where the tube exits the body) needs regular cleaning to prevent infection and skin breakdown.
- Daily Cleaning: The stoma site should be gently cleaned daily with mild soap and water or a saline solution, as recommended by the healthcare provider.
- Drying: After cleaning, the area should be thoroughly dried to prevent moisture buildup, which can encourage bacterial growth.
- Dressing: A clean gauze pad or a specialized stoma dressing may be placed around the tube to absorb any drainage and protect the skin.
Tube Management
- Flushing: Before and after each feeding, and after administering medications, the tube must be flushed with water. This is crucial to prevent the tube from becoming clogged with formula or medications, which is a common issue. The amount of water used for flushing will be specified by the healthcare team.
- Checking for Placement: Periodically, and especially if the tube feels loose or has moved, its position should be checked. Signs of dislodgement include the tube moving further out of the stoma or leakage around the site.
- Securing the Tube: Ensuring the external part of the tube is securely anchored prevents accidental pulling or dislodgement.
Feeding and Medication Administration
- Formula: Specialized liquid formulas are used for jejunal feeding. These are designed to be nutritionally complete and easily digestible. The type and volume of formula, as well as the feeding schedule, are determined by a dietitian or physician based on the individual’s needs.
- Rate of Feeding: Feedings are typically administered slowly over a period of time to prevent gastrointestinal distress. This can be done via gravity or using a feeding pump.
- Medication Administration: Medications should be in liquid form or crushed into a fine powder and dissolved in water before administration. Large pills or capsules may clog the tube. Always flush the tube thoroughly before and after administering medications. Some medications may interact with feeding formulas, so it’s important to consult with the healthcare provider.
Monitoring for Complications
Regular monitoring by the patient, caregivers, and healthcare professionals is essential to detect potential complications early.
- Infection: Signs of infection at the stoma site include redness, swelling, increased pain, warmth, and pus-like drainage.
- Tube Blockage: Difficulty flushing or administering formula/medication indicates a possible blockage.
- Dislodgement: If the tube moves out of position or becomes loose, it needs to be addressed immediately.
- Skin Irritation/Breakdown: Redness, soreness, or breakdown of the skin around the stoma requires attention.
- Gastrointestinal Issues: Nausea, vomiting, diarrhea, or abdominal pain can be signs that the feeding regimen needs adjustment.
Benefits and Considerations of Jejunostomy Tubes
The implementation of a jejunostomy tube offers significant advantages for patients who cannot sustain adequate nutrition through oral intake. However, like any medical intervention, it also comes with considerations and potential challenges.
Benefits
- Improved Nutritional Status: The primary benefit is the ability to provide essential calories, protein, fluids, and micronutrients, preventing or correcting malnutrition. This can lead to improved energy levels, better immune function, and enhanced wound healing.
- Reduced Risk of Aspiration: For individuals with dysphagia, jejunal feeding completely bypasses the swallowing mechanism, eliminating the risk of aspiration pneumonia, a life-threatening complication.
- Enhanced Quality of Life: By addressing nutritional deficiencies and preventing complications, jejunal feeding can significantly improve a patient’s overall quality of life, allowing them to feel better and participate more actively in their care and daily activities.
- Bypassing Upper GI Issues: It provides a viable route for nutrition when the stomach or upper small intestine is not functioning properly due to disease, surgery, or obstruction.
- Medication Delivery: It offers a reliable way to administer medications, especially for individuals who have difficulty swallowing pills.
Potential Complications and Considerations
While generally safe and effective, jejunostomy tubes can be associated with certain risks and challenges.
- Infection: As with any indwelling device, there is a risk of infection at the stoma site.
- Tube Blockage: Inadequate flushing or certain types of medications can lead to tube obstruction, requiring intervention.
- Tube Dislodgement: Accidental pulling or shearing forces can lead to the tube being displaced from its intended position.
- Skin Irritation and Breakdown: The constant presence of the tube and any leakage can cause irritation or breakdown of the surrounding skin.
- Gastrointestinal Symptoms: Some individuals may experience nausea, vomiting, diarrhea, or abdominal cramping if the feeding rate or formula is not optimized.
- Gastroesophageal Reflux: While jejunal feeding bypasses the stomach, some patients may still experience reflux.
- Dehydration: If fluid intake is not adequately managed, dehydration can occur.
- Cost and Logistics: The cost of specialized formulas, supplies, and the need for ongoing medical support can be a significant consideration for patients and their families.

Living with a Jejunostomy Tube
Adapting to life with a jejunostomy tube requires a learning curve for both the patient and their caregivers. Comprehensive education from healthcare professionals, including nurses, dietitians, and physicians, is crucial. Support groups and online resources can also provide valuable information and emotional support. With proper training, diligent care, and regular medical follow-up, individuals can manage their jejunostomy tubes effectively, enabling them to receive the vital nutrition and hydration necessary for their health and well-being. The jejunostomy tube, though a medical intervention, represents a significant advancement in providing essential care and improving outcomes for a diverse range of patients.
